Intrathecal Antibody Synthesis Borrelia
3.4.1 Overview
In most patients with Lyme neuroborreliosis the suspected clinical diagnosis can be confirmed by detecting Borrelia-specific intrathecal antibody synthesis related to inflammatory changes in their cerebrospinal fluid , , , . The production of specific intrathecal antibodies is detected by determining the Borrelia-specific CSF/serum antibody index , , .
3.4.2 Determination method
Methods used to determine the AI should take into account the blood/CSF barrier function, as otherwise false negative results may be produced . The determination of the antibody index according to Reiber is a proven method that is recommended , , , . The following formula is used to calculate the Borrelia-specific AI : Antibody index =
If intrathecal immunoglobulin synthesis is present in the Reiber diagram , the total IgG ratio must be replaced by the Q-Lim ratio . In this case: Antibody index =
A value of =1.5 is recommended as the cut-off for a positive AI, unless otherwise evaluated , , , previously recommended higher limit values of 2.0 are considered less sensitive when a reliable test performance can be ensured . Quantitative measuring methods are usually used to determine the AI and are implemented in commercial, EDP-supported systems .
It is important to note that there can be considerable fluctuations in the determination of AI . Hence antibody testing and AI determination should be conducted in accredited microbiology laboratories.
Summary
Getting A Correct Diagnosis
Diagnosing Lyme is often a complicated process, most physicians are not adequately qualified to identify Lyme disease and the common tests used to confirm a Lyme diagnosis can report incorrect results 50% of the time . To make matters more complex, Lyme patients with neurological symptoms are often misdiagnosed with neurological diseases like Multiple Sclerosis, Lupus, Parkinson’s disease, or even worse, their symptoms are dismissed altogether. The symptoms that they are experiencing are frustrating and maddening, especially when they are being told it’s all in your head. The struggle to find the right diagnosis is extremely draining for patients who are already facing depression, brain fog, memory loss, tremors, and other crippling symptoms.
At Envita our doctors and staff are highly trained in identifying Lyme disease our physicians utilize a proprietary PCR diagnosis protocol which allows them to not only accurately diagnose Lyme disease, but be able to monitor the Lyme infection and co-infection levels in the body throughout treatment. While this technology is still in research-and-development and is currently only available at Envita, it is proving to be a vitally important diagnostic tool for our Lyme patients. Correctly diagnosing the disease is always the first step in reaching a solution and at Envita we understand the importance of quickly and accurately diagnosing our patients.
Borrelia Releasing Neurotoxins in the Brain
Understanding Neurologic Lyme Disease
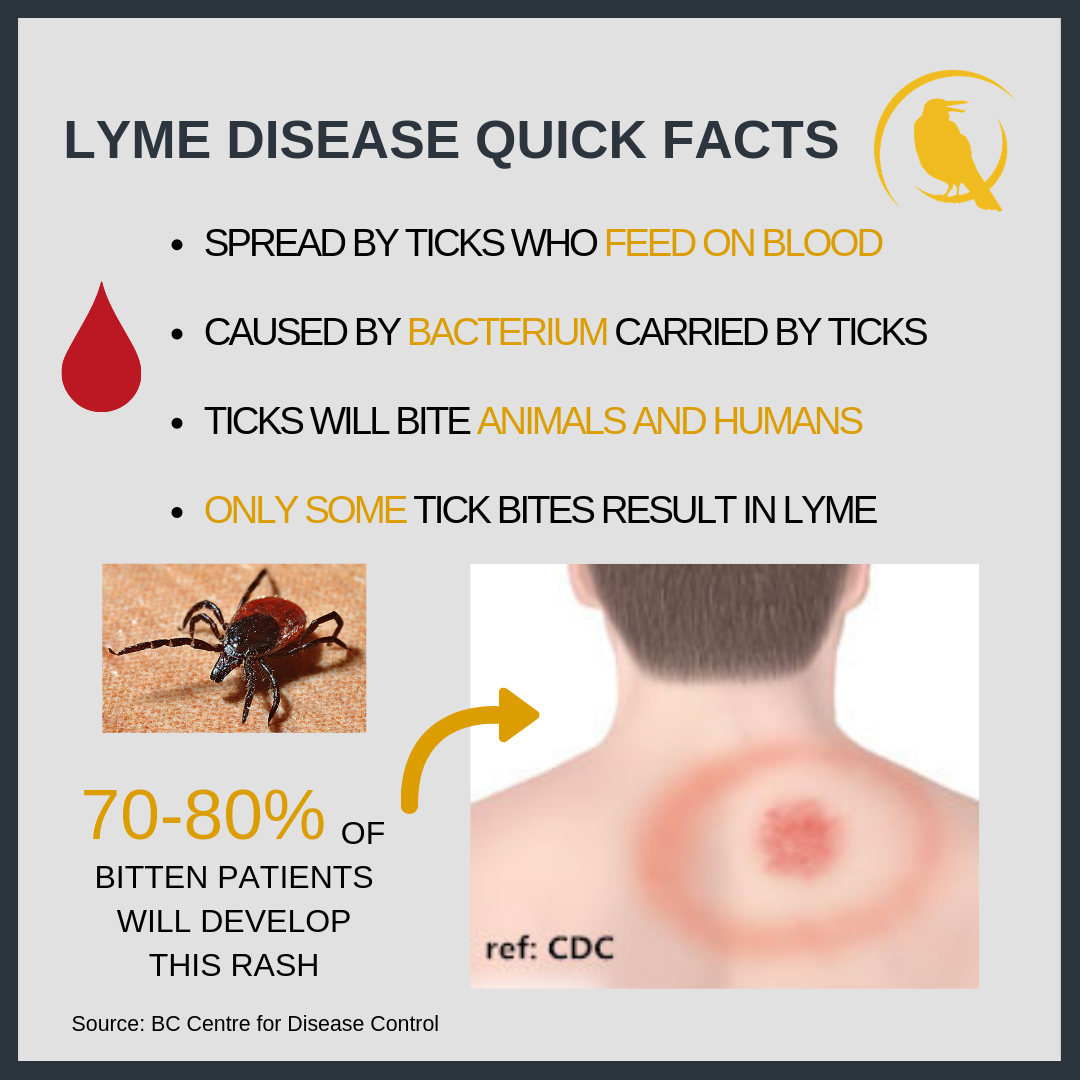
Lyme disease is a condition that is carried by infected black-legged deer ticks. These ticks are usually found in wooded areas with tall grass. Ticks intended targets are deer and other woodland animals, but will just as easily attach themselves to hikers, hunters, and unsuspecting adventurers. Lyme disease cases are consistently on the rise and the CDC estimates that the current numbers, around 300,000 cases every year, are dramatically underreported.
Dr. Joseph Schneider, DC, DACNB head neurologist at the Hope Brain and Body Recovery Center utilizes state-of-the-art treatment methods and expertise to help patients suffering from Neurologic Lyme Disease. Our team understands how much of a burden Lyme Disease can be and want to help you manage your symptoms and restore your quality of life.
Don’t Miss: Can Late Stage Lyme Disease Be Cured
Neurological Lyme Disease Treatment
Neuroborreliosis is a severe disease of the nervous system and treatment is with long-term antibiotic therapy. People with this type of Lyme disease need to reckon with taking several antibiotics at once over a long period of time. ILADS doctors use antibiotics such as doxycycline, tetracycline, penicillin, cephalosporins, and others. According to the ILADS organization, treatment of any version of Lyme disease should continue until symptoms resolve plus 1-2 months after symptoms disappear. Unfortunately, it is not uncommon for symptoms to come back. It is important to continue to lead a healthy lifestyle, eat healthily, and strengthen your immunity after successfully completing antibiotic therapy.
Of course, in addition to antibiotics, there are several alternative methods that can help cure Lyme disease. These include herbs , bioresonance, and stem cell treatment. Unfortunately, none of these methods have any research-confirmed activity against borrelia bacteria.
Recently, a lot has been said about the breakthrough in the treatment of Lyme disease, as it turned out that Disulfiram, a drug used to treat alcoholism, copes well with Lyme disease. Unfortunately, the topic is still in its infancy and we will wait a little longer before we find out what the pros and cons of such treatment are.
Administering Effective Lyme Treatments
Conventional medicine views Lyme disease treatment as an easy and straightforward proposition, a dose of antibiotics and youre cured. Though this may work in the earliest stage of the disease, it is when Lyme goes undiagnosed or mistreated and allowed to get to a chronic state when treatment becomes more difficult.
Lyme disease will often be accompanied by co-infections which work in synergy with borrelia to exacerbate symptoms making the disease difficult to treat. Lyme disease also has the unique ability to bypass the bodys blood-brain barrier, a barrier which typically prevents foreign invaders from affecting the brain, allowing the disease to enter the nervous system accounting for Lymes many complex neurological symptoms. Antibiotic treatment protocols alone do not account for this invasion of the bodys nervous system through the blood-brain barrier and therefore are not likely to have lasting results. To effectively treat chronic Lyme disease, antibiotics need to also move past the blood-brain barrier .
Borrelia Attacking Neurons in the Brain
You May Like: Best Cbd Oil For Lyme
Symptoms Of Early Stage Lyme Disease
According to the Centers for Disease Control and Prevention , early-stage Lyme disease symptoms crop up within 3 to 30 days after exposure and can include but are not limited to:
- Joint pain and swelling
- Swelling of the lymph nodes
- Erythema migrans , a bulls-eye-shaped rash that appears at the site of the tick bite
Early Lyme disease does not always appear the same in all patients. For example, up to 30% of patients dont remember experiencing a bulls eye rash.
Regression And Other Symptoms In Children
Children are the largest population of Lyme patients.
The CDC study of reported Lyme cases from 19922006 found that the incidence of new cases was highest among 5- to 14-year-olds . About one quarter of reported Lyme cases in the United States involve children under 14 years old .
Children can have all the signs and symptoms of Lyme that adults have, but they may have trouble telling you exactly what they feel or where it hurts.
You may notice a decline in school performance, or your childs mood swings may become problematic.
Your childs social and speech skills or motor coordination may regress. Or your child may lose their appetite.
Children are more likely than adults to have arthritis as an initial symptom 01267-2/fulltext#sec0040â³ rel=ânofollowâ> 25).
In a 2012 Nova Scotian study of children with Lyme, 65 percent developed Lyme arthritis . The knee was the most commonly affected joint.
Summary:
Read Also: Yolanda Hadid Lyme Disease Treatment
What Is Late Lyme Disease
Lyme disease, also known as Lyme borreliosis, is caused by an infection with the bacteria Borrelia burgdorferi. This bacteria is disseminated through tick bites. Infected ticks usually bite small mammals, who do not develop any kind of infection from the bacteria. When humans are exposed to B. Burgdorferi from a tick bite, however, they can develop Lyme disease.
People who work outside or spend time in woodland areas, where there is greater potential for exposure to tick bites, are most at risk of infection.
Lyme disease is a condition which progresses in stages:
The Numbers On Chronic Lyme
Because Lyme disease is commonly missed or misdiagnosed, statistics vary on how many Lyme patients go on to experience chronic symptoms. The following research nonetheless paints a basic picture of the problem.
- An estimated 5-20% of patients may have chronic symptoms after getting Lyme disease, according to the Columbia University Irving Medical Center.
- The treatment failure rate for chronic Lyme disease patients was estimated at 26-50% in 2004, compared to 16-39% for early Lyme patients, according to Lymedisease.org.
- Up to 15-40% of late-stage Lyme patients develop neurological disorders, which are responsible for many common symptoms of chronic Lyme disease.
Experts dont know for sure why some people experience persistent symptoms, even with treatment. However, some believe the Lyme infection may trigger an auto-immune response that manifests in the chronic symptoms detailed below.
Recommended Reading: Lyme Disease Blood Test Cost
Chronic Lyme Disease Symptoms
Chronic symptoms of Lyme disease arent always clear cut and manifest similarly to other conditions, which can lead to misdiagnosis. Chronic Lyme disease is often used to describe a range of physical, cognitive, and emotional symptoms that crop up after getting Lyme disease and persist for months to years after infection, Shah says. Common persistent symptoms include:
- Long-lasting, severe fatigue
- Neurological symptoms such as brain fog, cognitive impairment, or facial palsy
- Sensory sensitivity, particularly to lights and sounds
- Anxiety or depression
- Gastrointestinal issues, such as abdominal pain, nausea, blood in the stool, or chronic diarrhea
Many tick-borne infections go misdiagnosed for months because these nonspecific symptoms mirror other illnesses, Shah explains, adding that these symptoms can mimic chronic fatigue syndrome, fibromyalgia, ALS, Alzheimers disease, depression, insomnia, and autoimmune disorders such as rheumatoid arthritis and multiple sclerosis .
Chronic Lyme can also trigger an auto-immune response or make a person more susceptible to other infections, systemic inflammations, and imbalances in the gut microbiome, according to Dr. Kellman.
If you suspect you have chronic Lyme, your first step should be to a primary care provider you trust who can help you diagnose by eliminating other potential illnesses.
Biological Explanations For Chronic Lyme Disease
Several arguments have been made to support the biological plausibility of CLD and to justify its treatment with lengthy courses of antibiotics. One is that B burgdorferilocalizes intracellularly in the infected host, and that the antibiotics typically chosen to treat it do not penetrate cells effectively. Aside from the fact that B burgdorferi predominantly occupies the extracellular matrix, the antibiotics currently recommended to treat Lyme disease are well-established to treat a variety of intracellular infections. For example, doxycycline and azithromycin are first-line drugs for the treatment of Mycoplasma, Chlamydia, and Legionella, and doxycycline is the drug of choice for Rickettsia and related species. Ceftriaxone is effective against Salmonella and Neisseria, both of which are predominantly intracellular amoxicillin is effective against Listeria.
Another commonly voiced argument is that B burgdorferi assumes a round morphology, variously described as cyst forms,spheroplasts,L-forms, and round bodies. These variants are said to be resistant to antibiotic treatment and require alternative antibiotics and dosing strategies. On close review of the literature there is little evidence that these variants arise in vivo in humans, let alone that they are associated with CLD-like symptom complexes or that they require treatment.
Read Also: What Medication Is Used For Lyme Disease
You May Like: Lyme Disease Specialist Long Island New York
The Path To Healing Chronic Neurological Lyme Disease
I spent countless hours searching for answers before I was finally diagnosed with Chronic Lyme Disease.
Since Lyme Disease is such a complicated illness, I knew that I could not get better on my own.
I knew I needed to find a doctor who had success in treating Lyme Disease.
Once I found a Lyme Literate MD, I knew my future then depended on one person.
That person was me.
My doctor was responsible for creating a treatment plan, but it was my responsibility to follow the plan. I knew it was ultimately up to me to be the driving force behind my healing.
Below are the steps I took to heal Chronic Neurological Lyme Disease, mold toxicity, and radiation exposure.
While I am still on my healing journey, these are the things that have made major improvements in my health.
Before I tell you the steps I took there is one critical thing to remember.
We are always on a journey. Life is the journey. There is no endpoint just an infinite amount of small goals and big wins along the way!
This is something helpful to remember when dealing with a chronic illness since there can be many ups and downs.
With that being said, here are my top ten tips to healing Chronic Neurological Lyme Disease:
Reports From The Literature
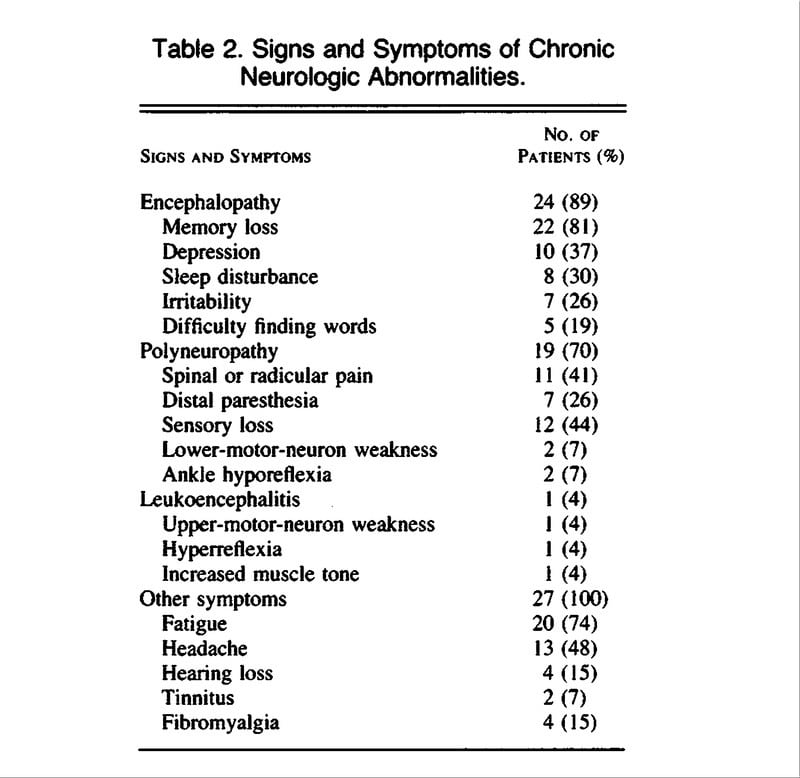
The literature search by using stringent diagnostic criteria disclosed only seven additional patients with dementia as a leading symptom of definitive LNB. These cases were reported in detail, so they can serve for the description of characteristic features. The data of all 10 patients are summarized in Table and .
Read Also: Are Lyme Disease Tests Reliable
Also Check: Dr Mark Hyman Lyme Disease
Neurological Manifestations In Adults
Garin-Bujadoux-Bannwarth syndrome is the most common manifestation of acute Lyme borreliosis in adults in Europe after erythema migrans , , .
In Europe, isolated meningitis is mainly observed in children , , , , .
The symptoms of radiculitis develop on average 46 weeks after the tick bite or after the erythema migrans , . Segmental pain occurs first, which intensifies at night and whose localisation can change. Often the pain is initially localised in the extremity where the tick bite or erythema migrans was first observed , . The patient experiences pain that is burning, nagging, stabbing or tearing in nature and responds only slightly to conventional analgesics. It often peaks within a few hours or days. Three-quarters of patients develop neurological deficits after 14 weeks, and pareses are more frequent than sensory disorders , .
About 60% of patients with Bannwarths syndrome have cranial nerve deficits.
Involvement of the central nervous system is rare and occurs in only around 4% of Lyme neuroborreliosis cases , . Its onset is gradual and it is frequently chronic. The most common manifestation is myelitis with spastic atactic gait disturbance and bladder dysfunction , . Symptoms can develop over days or several months. Some patients suffer from severe tetra- or paraparesis. Approximately 60% of patients with myelitis have additional signs of encephalitis and around 40% have cranial nerve involvement. Encephalitis has no clinical properties specific to the pathogen.
When Does Lyme Disease Affect The Brain
The symptoms of Lyme Disease typically present in three stages:
Neurological Lyme Disease symptoms tend to start during the second stage which can occur weeks or months after the initial infection.
If left untreated the patient can enter the late disseminated stage months or even years after infection, and Acute Neurological Lyme Disease can turn into to Chronic Neurological Lyme Disease.
Recommended Reading: How Long Does A Lyme Blood Test Take
Invite More Calm Into Your Life
Since stress is a powerful immune system disruptor, finding more calm is key to restoring immune health and resolving symptoms of neurological Lyme. One of the best tools to fight stress is getting optimal sleep. Without it, your immune system becomes compromised and stalls healing.
Sleep is especially important for recovery from neuroinflammatory illnesses. Studies have shown that even one night of compromised sleep in healthy people is associated with accumulation of beta amyloid in the brain, a hallmark of Alzheimers disease.
Your goal: At least 8 hours of good sleep a night, including 4 hours of deep sleep. Practicing good sleep hygiene can help you hit the mark that includes keeping a regular bedtime, and limiting light, computer screens, and stimulation in the evening.
What happens during the day is also key to drifting off at night. Finding additional ways to de-stress, getting regular low-intensity exercise, and practicing meditation a couple of times during the day promotes good sleep onset and better quality sleep at night.
Melatonin, an important antioxidant in the brain that initiates sleep, is reduced in neuroinflammation. Supplemental melatonin at bedtime can help rebalance disrupted sleep pathways. Tart cherry juice is an excellent natural source of melatonin, as is Chinese skullcap, an herb providing both antimicrobial properties and immune-balancing properties.
The Experience Of Lyme Disease
In our book, Conquering Lyme Disease: Science Bridges the Great Divide, we review several of the key features of Lyme disease that can make the experience of this illness so challenging, including:
- The politically charged climate
- The protean nature of manifestations of the illness
- The waxing and waning course of symptoms
- The psychological ramifications of having an invisible chronic illness and the experience of invalidation
- The challenge of having a disease that affects the brain and sensory system
- The impact of uncertainty surrounding diagnosis, treatment, and prognosis
Read Also: Can Lyme Disease Cause Immune Deficiency
Making Connections To Clarify Diagnosis
Chronic Lyme disease shares many symptoms with other chronic illnesses. This is especially true of LNB and chronic neuroinflammatory illnesses such as multiple sclerosis, Alzheimers disease, amyotrophic lateral sclerosis , Parkinsons disease, and traumatic brain injury .
Not surprisingly, new sophisticated methods of microbial detection are showing potential links between these neuroinflammatory illnesses and many of the microbes associated with chronic Lyme disease.
For instance, both Mycoplasma and Chlamydia have been closely linked to multiple sclerosis. Mycoplasma, Borrelia, and Chlamydia have been associated with demyelination. Parkinsons and ALS have been linked to Borrelia and other microbes commonly associated with Lyme disease. Borrelia and other stealth pathogens have been found in the brains of patients who died of Alzheimers disease.
But the connections go well beyond Lyme disease microbes. Two studies shed some light on how closely disruptions in the microbiome are linked to neuroinflammation. One, published in Frontiers of Aging Neuroscience, evaluated the presence of microbes in the autopsied brains of deceased Alzheimers patients. The other, published in Scientific Reports, evaluated the presence of microbes in the autopsied brains of people who had died of multiple sclerosis.
Ultimately, the type of illness a person might end up with depends on three key things: