Antimicrobial Treatments For Lyme Disease
The conventional medical approach to Lyme disease treatment in adults is a ten to 21-day course of the antibiotic doxycycline.1 However, a growing body of research shows that this treatment is insufficient, if not completely ineffective, for cases of chronic Lyme disease. Functional medicine offers a far more comprehensive approach to the antimicrobial treatment of Lyme disease. Read on to learn about the types of antimicrobial treatment options available, and how they can be combined for optimal effect.
Can Lyme Disease Completely Be Cured
Yes, Lyme disease can be cured completely with our CUREplus Homeopathy treatment.
Unfortunately, Lyme disease is not completely curable in conventional allopathic treatment. If you choose allopathic doctor, it can be treated and symptoms reduced and in some cases eliminated with early diagnosis and prompt treatment.
What Is The Outlook For Someone With Lyme Disease
Most of the people who get Lyme disease and treated early will be fine.
Post-Lyme Syndrome
Even after proper treatment, some patients may experience lingering fatigue, achiness or headaches. This does not signify ongoing infection and will not respond to additional antibiotics. The majority of people in this group will have symptoms resolve over the next 1-6 months.
Chronic Lyme Syndrome
Chronic Lyme syndrome is a term used by some that includes the symptoms of Post-Lyme syndrome outlined above. This is a controversial topic with no accepted etiology and no proven cause or association.
Also Check: Hydrogen Peroxide Treatment For Lyme Disease
How Can Lyme Disease Be Prevented
In areas where ticks are found, people should know about the risk of Lyme disease and should take precautions to protect themselves. Be aware of the signs and symptoms of Lyme disease so it can be detected and treated promptly. PHAC states that removing ticks within 24 to 36 hours after the tick bite usually prevents infection.
PHAC has also prepared a Lyme disease tool kit which provides material to raise awareness and educate.
Alternative & Holistic Treatment For Lyme Disease:

Alternative and holistic treatment for Lyme disease may include any of the natural treatment protocols and therapies as listed above. As mentioned previously, the conventional way of treating Acute or Early-Stage Lyme Disease is through antibiotics. However, some people cant use pharmaceutical antibiotics, chose not to use antibiotics or find them ineffective.
Herbs for lyme disease treatment include herbal antimicrobials such as teasel root and cats claw which have long been used in Chinese Medicine for their multiple health benefits. Teasel root is often used as an antimicrobial to strengthen kidney and liver function and cats claw has powerful ant-inflammatory and antioxidant properties. The Cowden Herbal Protocol and Buhner Protocol use medicinal herbs to treat Lyme disease holistically.
Homeopathic treatment for Lyme disease include Hypericum Perforatum which is used in the treatment of nerve pain, depression and as a natural antibiotic, and Arsenicum Album which is often used in treating digestive disorders including mucosal inflammation.
For further information on Alternative, Holistic and the Natural Treatment of Lyme Disease, please read our page HERE: https://www.lymediseaseadvice.com/natural-treatment-for-lyme-disease/
Dietary and nutritional changes are also effective in the treatment of Lyme disease and we have prepared a Lyme Disease Diet to get you stared HERE:
Read Also: Can Lyme Disease Cause Dizziness
Phylogenetic Diversity And Human Disease Taxonomy And Disease
B. burgdorferi was thought to be the sole genospecies in the United States until 1995 when Marconi and associates isolated B. andersonii from cottontail rabbits and I. dentatus ticks. Subsequently, it became evident that enzootic cycles exist involving non-sensu stricto species and specialist ixodid ticks with strong, selective host preferences and little or no proclivity to bite humans. Perhaps the best characterized of these is B. bissettii , transmitted by I. pacificus, I. affinis and I. spinipalpis and recovered and/or detected by PCR throughout the United States in ticks and a variety of vertebrates and, in rare instances, humans . Molecular evidence for infection of humans by B. americana and B. andersonii, particularly in Southern states, also has been reported . Moreover, B. mayonii was recently isolated from a few human specimens in upper midwestern U.S. . However, in the United States, B. burgdorferi remains the primary agent of disease.
Cdc Supports The Development Of New Tests
New tests may be developed as alternatives to one or both steps of the two-step process. Before CDC will recommend new tests, they must be cleared by the Food and Drug Administration . For more details, see: Recommendations for Test Performance and Interpretation from the Second National Conference on Serologic Diagnosis of Lyme Disease.
Read Also: Beach Houses For Sale In Old Lyme Ct
Chronic Lyme Disease And Post
Almost 30 years ago, clinicians began to report that some Lyme disease patients have persistent nonspecific symptoms after receiving an adequate course of therapy . In its 2006 guidelines, the Infectious Diseases Society of America created a working definition for this entity, now called post-treatment Lyme disease syndrome or PTLDS: clinical symptoms persisting at least six months after treatment for Lyme disease in persons who lack objective evidence of treatment failure, reinfection, or relapse . PTLDS differs from CLD in one particularly important respect patients with PTLDS have unequivocal documentation for appropriately treated Lyme disease. PTLDS occurs in only a small percentage of treated patients. As noted by Lantos in an excellent review , only 222 of 5846 patients screened to participate in clinical trials for PTLDS had credible evidence for past Lyme disease, while less than 10% of patients in ten prospective studies of EM and early disseminated Lyme disease described persistent symptoms such as myalgias or fatigue 9 or more months following treatment. Fortunately, multiple longitudinal studies in the U.S. and Europe report that functional impairment by PTLDS diminishes over time .
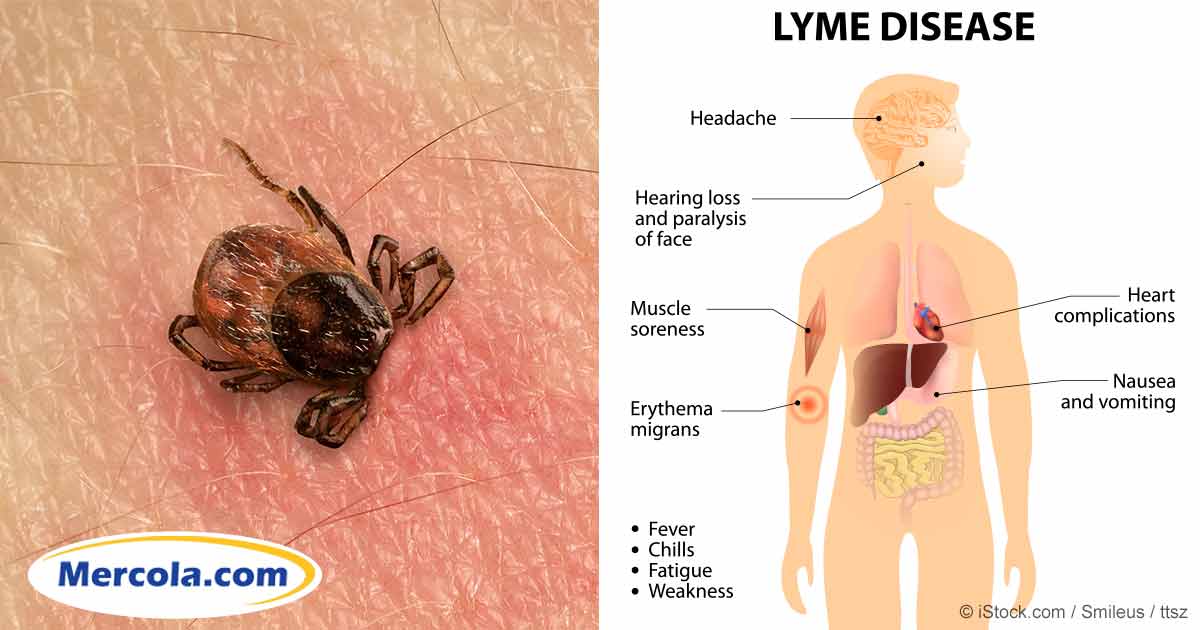
What Are The Signs And Symptoms Of Lyme Disease
Tick bites are usually painless and most people do not know they have been bitten. Signs and symptoms of Lyme disease vary greatly from person to person, and may appear anywhere between 3 to 30 days after a person has been bitten.
Symptoms often include:
- Swollen lymph nodes.
- Skin rash.
One sign of infection can be an expanding rash, sometimes referred to as a “bull’s eye” rash because it may have rings spreading from the bite site ). It is important to note that rashes without the bull’s eye may occur, and that rashes do not appear in every case of Lyme disease infection.
The PHAC states that if left untreated, more severe symptoms may occur and can last from months to years. Severe symptoms may include:
- Severe headaches
- Additional EM skin rashes..
- Neurological disorders
- Nervous system disorders, including facial paralysis or Bell’s palsy .
- Intermittent muscle, joint, tendon, and bone aches
- Arthritis with severe joint pain and swelling, particularly the knees and less commonly in other joints such as the ankle, elbow, and wrists.
If untreated, a condition called late disseminated Lyme disease may occur. PHAC reports symptoms include recurring arthritis , nervous system and/or neurological problems. Symptoms can also include numbness and/or paralysis . Deaths from Lyme disease are rare but may occur.
PHAC provides more information on Lyme Disease.
Recommended Reading: Where Can You Get A Lyme Disease Test
What Do You Do If There’s A Tick Under Your Skin
Use a pair of fine-tipped tweezers to remove it as soon as possible. Pull upward with steady pressure. If parts of the tick are still in your skin, try to get those with the tweezers, too. After everything is out, clean the bite area with rubbing alcohol or soap and water.
You probably wonât get infected if you remove the tick within 36 to 48 hours.
How do you throw away a tick?
Put it in soapy water or alcohol, stick it to a piece of tape, or flush it down the toilet.
Treatment For Erythema Migrans
People treated with appropriate antibiotics in the early stages of Lyme disease usually recover rapidly and completely. Early diagnosis and proper antibiotic treatment of Lyme disease can help prevent late Lyme disease.
Treatment regimens listed in the following table are for the erythema migrans rash, the most common manifestation of early Lyme disease. These regimens may need to be adjusted depending on a persons age, medical history, underlying health conditions, pregnancy status, or allergies. Consult an infectious disease specialist regarding individual patient treatment decisions.
| Age Category | |
|---|---|
| 100 mg, twice per day orally | N/A |
| 500 mg, three times per day orally | N/A |
| 500 mg, twice per day orally | N/A |
| 4.4 mg/kg per day orally, divided into 2 doses | 100 mg per dose |
| 50 mg/kg per day orally, divided into 3 doses | 500 mg per dose |
| 30 mg/kg per day orally, divided into 2 doses | 500 mg per dose |
*When different durations of antibiotics are shown to be effective for the treatment of Lyme disease, the shorter duration is preferred to minimize unnecessary antibiotics that might result in adverse effects, including infectious diarrhea and antimicrobial resistance.
NOTE: For people intolerant of amoxicillin, doxycycline, and cefuroxime, the macrolide azithromycin may be used, although it is less effective. People treated with azithromycin should be closely monitored to ensure that symptoms resolve.
Also Check: Does Lyme Disease Cause Constipation
Lyme Disease Treatment: 2 Herbal Compounds May Beat Antibiotics
Lyme disease transmitted via tick bite affects thousands of people in the United States and around the world. Currently, doctors use antibiotics to treat it, but could plant-based remedies be more effective?
Lyme disease is an infectious disease caused by the bacterium Borrelia burgdorferi .
The disease spreads to humans through the bite of a tick that carries the bacterium, and it affects an estimated each year in the U.S. alone.
Currently, healthcare professionals choose between three antibiotics in the treatment of Lyme disease. These are doxycycline, cefuroxime, and amoxicillin.
Sometimes, however, antibiotics are not effective in eradicating all traces of B. burgdorferi from the system, which means that the disease can persist.
When this happens, bacterial cells that have developed antibiotic resistance can continue to proliferate. These are known as persister cells .
Because of this, researchers have been looking into alternative modes of fighting the bacterium, and their first line of inquiry has focused on natural remedies.
In 2018, an in vitro study suggested that 10 plant-derived essential oils could help fight off B. burgdorferi.
Now, researchers from the Johns Hopkins Bloomberg School of Public Health in Baltimore, MD, and from the California Center for Functional Medicine and Focus Health in Berkeley, have conducted a new study that has led them to believe that two specific plants may lead to more effective therapies against Lyme disease.
Stage : Early Localized Disease
Symptoms of Lyme disease usually start 1 to 2 weeks after the tick bite. One of the earliest signs of the disease is a bulls-eye rash.
The rash occurs at the site of the tick bite, usually, but not always, as a central red spot surrounded by a clear spot with an area of redness at the edge. It may be warm to the touch, but it isnt painful and doesnt itch. This rash will gradually fade in most people.
The formal name for this rash is erythema migrans. Erythema migrans is said to be characteristic of Lyme disease. However, many people dont have this symptom.
Some people have a rash thats solid red, while people with dark complexions may have a rash that resembles a bruise.
The rash can occur with or without systemic viral or flu-like symptoms.
Other symptoms commonly seen in this stage of Lyme disease include:
Read Also: How Can You Tell If A Tick Has Lyme Disease
Risk Factors For Post
Youre at a greater risk for post-treatment Lyme disease syndrome if youre infected by the bite of a diseased tick. If the infection progresses to the chronic stage, your symptoms might continue for weeks, months, or even years after the initial tick bite.
You may also be at a higher risk for these long-term symptoms if youre not treated with the recommended antibiotics. However, even people who receive antibiotic therapy are at risk. Because the cause of post-treatment Lyme disease syndrome is unknown, theres no way to determine whether it will progress to the chronic stage.
Typically, the symptoms of post-treatment Lyme disease syndrome resemble those that occur in earlier stages. People with persistent symptoms often experience lingering episodes of:
- fatigue
What Are The Complications Of Lyme Disease
Lyme disease affects people differently. Relapse and incomplete treatment responses happen. Relapse and incomplete treatment responses happen. Complications of untreated early-stage disease include:
-
Joint disease
-
Frequent hospitalizations to manage the disease
Some of these complications result in chronic, debilitating conditions.
Some people may develop post-Lyme disease syndrome . A condition also known as chronic Lyme disease includes PLDS, but also other syndromes. Usually, these are characterized by persistent musculoskeletal and peripheral nerve pain, fatigue, and memory impairment.
Also Check: What Happens If You Have Lyme Disease
Key Points To Remember
- Most Lyme disease tests are designed to detect antibodies made by the body in response to infection.
- Antibodies can take several weeks to develop, so patients may test negative if infected only recently.
- Antibodies normally persist in the blood for months or even years after the infection is gone therefore, the test cannot be used to determine cure.
- Infection with other diseases, including some tickborne diseases, or some viral, bacterial, or autoimmune diseases, can result in false positive test results.
- Some tests give results for two types of antibody, IgM and IgG. Positive IgM results should be disregarded if the patient has been ill for more than 30 days.
What Is The Best Antibiotic For Lyme Disease
The best anitbiotic for Lyme disease is Doxycycline. Doxycycline was the first to be found, and it works on both ticks and Lymecycline in ring form. Doxycycline combined with amoxicillin has proved to provide an even better results. The only downside of doxycyclines is that people under age 35 have higher chances of developing acne. And while others are being studied, so far there has not been a magic bullet against the bacterial family of Borrelia burgdorferi, which causes Lyme disease after an incubation period ranging from 3 days to months before any associated symptoms are experienced . It can take anywhere from 2-6 weeks for antibiotics or other treatments to kill all of the bacteria.
Doxycycline is an antibiotic used to treat infections such as Lyme disease and other tick-borne diseases, acne , rosacea, chlamydia , and others.
Don’t Miss: Getting A Tick Tested For Lyme Disease
Scientists Find Promising New Treatment For Lyme Disease
A new study gives hope that an effective treatment for Lyme disease may be available in the future. The new treatment involves the drugs cefotaxime and azlocillin.
The new paper appears in the Nature journal Scientific Reports .
Lyme disease affects nearly 300,000 people a year in the United States and around 230,000 people a year in Europe, according to an article in the Journal of Public Health .
Bacteria belonging to the group Borrelia burgdorferi cause Lyme disease. Most people develop it after being bitten by a tick that carries the bacteria.
Approximately 6080% of people with Lyme disease develop a circular red skin rash called erythema migrans around the infected tick bite, and some also develop flu-like symptoms.
Most people develop the rash within 4 weeks of being bitten, but it can appear up to 3 months afterward.
of people with the disease later develop symptoms of fatigue, pain in their muscles, joints or nerves, and cognitive impairment.
These symptoms can continue for months or even years after their initial infection.
Researchers have suggested that this may because of drug-tolerant persisters, a group of bacterial cells that survive the initial dose of antibiotics.
Others believe its an immune disorder caused by bacteria during the first exposure, which causes a perpetual inflammation condition. Whatever the cause, the pain for patients is still very real.
When Should I Call The Doctor
If a tick bites you, call your doctor. Other conditions can cause similar symptoms, so it’s always a good idea to discuss them with your doctor. That way you can get checked and treated, if needed. Call right away if you get a red-ringed rash, lasting flu-like symptoms, joint pain or a swollen joint, or facial paralysis.
You May Like: How Do You Catch Lyme Disease
Healthy Vs Weak Cells
How all this plays out is a function of the health of cells as much as the aggressiveness of the bacteria: Cells that are weak from being chronically stressed are more vulnerable to invasion by bacteria.
A healthy person with healthy cells who is bitten by a tick may not have much in the way of acute symptoms and may never develop chronic symptoms. It doesnt mean, however, that the bacteria have been eradicated from the body. They can stay dormant in tissues for a lifetime.
All it takes is a shift in the health of cells for dormant bacteria to surface and invade more cells. The immune system scrambles to keep a lid on things as bacteria erupt and infect other cells. Dead cells break apart and create debris. Macrophages secrete acid and free radicals to break down debris. Reinforcements are called in. More acid. More free radicals. More collateral damage. More debris. Flow of nutrients and oxygen is obstructed and cells are weakened even further.
The invasion intensifies as more cells are infected. Along with inflicting injury to cells in tissues, bacteria infect and kill WBCs. In addition, bacteria throw the immune system off balance by disrupting the cytokines the immune system uses to coordinate the resistance. As the process spirals out of control, the immune system loses the capacity to keep microbes in check.
Before long, tissues throughout the body start to look like a war zone. Cells suffer. Symptoms result. It becomes a never-ending cycle of misery.