The Role Of Lyme Disease Tests
The purpose of the most common type of Lyme disease testing is to determine whether you have developed antibodies as a result of past exposure to the Borrelia bacteria that cause Lyme disease. Antibodies are proteins created by the immune system that target specific threats like bacteria and viruses.
Blood testing alone cannot determine whether you have Lyme disease. Instead, testing can provide helpful information that your doctor can consider along with other factors, such as any symptoms youve had and whether youve been exposed to ticks that can carry Borrelia, to determine if a diagnosis of Lyme disease is appropriate.
Beyond blood testing, it is possible to analyze fluid from the central nervous system for signs of the Borrelia bacteria.
Does The Time Of Year Matter In The Diagnosis Of Lyme Disease
Since Lyme disease is a tick-borne infection, the seasonality of the disease is linked tightly to the life cycle and behavior of ticks. May, June, July, and early August are the biggest risk months for acquiring first stage Lyme disease in the US. This is the feeding time for nymph and adolescent ticks which are difficult to see. A viral-like illness in those early summer months might be Lyme disease. There is also some transmission of Lyme disease via adult ticks in the fall and winter and throughout the year anytime the temperature is above 40 degrees, but to a lesser degree.
The risk of acute Lyme disease is more of a year-round risk in more temperate regions such as northern California and the pacific northwest. Later stage Lyme disease, however, can manifest at any time.
What Is Lyme Disease How Does My Dog Get Infected
Lyme disease is an infectious disease caused by bacteria called Borrelia. The bacteria are most commonly carried by the deer tick . Infection occurs when a dog is bitten by an infected tick. It appears that the disease is not transmitted until the tick has fed for approximately 12 hours. The tick itself becomes infected by feeding on infected mice, birds, deer, and other animals.
Recommended Reading: Doxycycline Dosage For Lyme Disease
How Do They Test For Lyme Disease
Lyme disease is best tested using two different blood testing methods. These are:
- The Enzyme-linked Immunosorbent Assay test: In a nutshell, this test will look for signs that your body is trying to fight off Lyme disease by producing antibodies. However, the ELISA test may come back negative even when a person is infected by the Borrelia burgdorferi bacteria. False-negatives can occur during the early stages of the disease, where the infected persons body has not produced enough antibodies to fight off the B. burgdorferi bacteria. For this reason, reliable diagnosis is not usually based only on the ELISA test results.
- Western Blot test: Heres a simple way to explain the western blot test without getting into all the nitty-gritty details of what it does and how it does it. Put simply, it separates the blood proteins and detects antibodies to the bacteria causing the Lyme disease. Usually, when an ELISA test comes back positive, a western blot test is performed to confirm the diagnosis.
Ideally, the CDC recommends standard two-tier testing to confirm the veracity of the Lyme disease test accuracy. Together, the ELISA and western blot tests are 99.9% accurate.
What Happens During Lyme Disease Testing
Lyme disease testing is usually done with your blood or cerebrospinal fluid.
For a Lyme disease blood test:
- A health care professional will take a blood sample from a vein in your arm, using a small needle. After the needle is inserted, a small amount of blood will be collected into a test tube or vial. You may feel a little sting when the needle goes in or out. This usually takes less than five minutes.
If you have symptoms of Lyme disease affecting your nervous system, such as neck stiffness and numbness in hands or feet, you may need a test of cerebrospinal fluid . CSF is a clear liquid found in your brain and spinal cord. During this test, your CSF will be collected through a procedure called a lumbar puncture, also known as a spinal tap. During the procedure:
You May Like: Houses For Sale In Lyme Ct
Best For Dna Test: Selfdecode
Self Decode
-
Tests for chronic conditions related to Lyme disease like PTLDS
-
Results in 6-8 weeks
SelfDecode searches for more than Lyme disease. When you take an at-home test through this company, you’ll receive an entire mock-up of your DNA. You will know if you ever had Lyme disease in the past, as well as if you are susceptible to PTLDS, a chronic condition triggered by Lyme Disease.
The test involves taking a simple cheek swab, after which the test is mailed back to the company’s lab. After six to eight weeks, you will receive your results via email, and you will be contacted by a medical professional to see what the next steps are.
This is a subscription service that costs just under roughly $100 a year, so you will be able to check yourself for Lyme disease regularly when the test is shipped out. This service is great for those who enjoy the outdoors and are exposed to ticks a lot.
SelfDecode’s test is not covered by insurance, but most primary care physicians will accept these results.
Current Research On New Approaches
NIAID actively supports research on Lyme disease diagnostics. Small businesses and public/private partnerships often submit applications for new research projects. NIAID grantees also work directly with CDC scientists to evaluate and compare the effectiveness of currently used diagnostic methods.
Working with CDC, NIAID plays a major role in encouraging the development of new approaches to improve Lyme disease diagnosis in people with tick-borne co-infections such as anaplasmosis or babesiosis. New diagnostic tests are also needed to distinguish between people with B. burgdorferi infection and those whose immune responses stemming solely from past Lyme disease vaccination. Although Lyme disease vaccines for humans are no longer available in the United States, the discontinued LYMErix vaccine used between 1998 and 2002 was based on a specific part of B. burgdorferi called outer surface protein A . In response to the vaccines, immunized individuals developed antibodies for OspA. Because the conventional ELISA measures OspA antibodies to determine if someone has Lyme disease, the test does not provide accurate results for immunized individuals. People who received the vaccination will test positive whether or not they are actually infected with B. burgdorferi.
NIAID is supporting research on a variety of approaches to improve the diagnosis of Lyme disease:
You May Like: Lyme Disease Immune System Weakened
Early Vs Later Diagnosis
Lyme disease has been diagnosed long enough, and the infectious bacteria that causes it is easy enough to identify, that most patients with early Lyme disease are able to find a healthcare provider who can accurately diagnose it. Even those patients who are originally told by a healthcare provider that their symptoms are all in their head are often able to find another practitioner to help them get the accurate diagnosis.
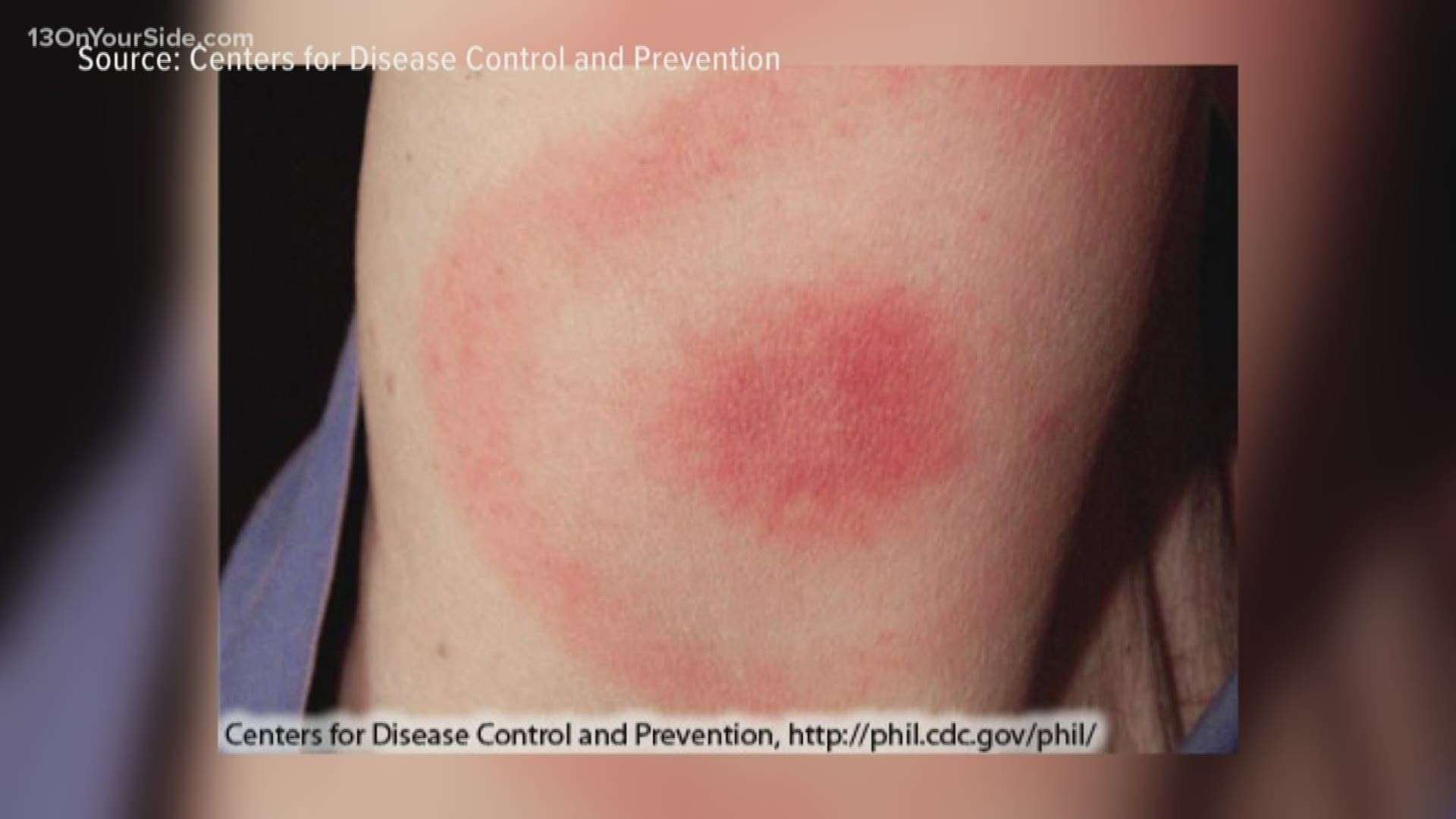
But in some cases, patients find great difficulty in getting a Lyme disease diagnosis. And that’s because there is a controversy that surrounds such a diagnosis for patients who don’t suffer symptoms until long after they were possibly bitten by a tick. While some people exhibit symptoms, including the classic “bull’s eye” rash, early after a tick bite, it’s possible that symptoms won’t show up for months or years after being infected.
Furthermore, some patients are treated early with antibiotics, but those antibiotics don’t completely destroy the Lyme Borrelia bacteria, or other symptoms occur even when no sign of any lingering infection remains.
“Chronic” Lyme Disease Diagnosis Controversy
Although no one denies that some people treated appropriately for Lyme disease go on to have persistent symptoms, there is a huge controversy over what it’s called, what causes it, and how it’s best treated. It has been called “chronic Lyme disease” the Centers for Disease Control and Prevention calls it post-treatment Lyme disease syndrome .
How Much Do At
Generally, at-home Lyme disease tests cost around $100, while others may cost closer to $500. The difference comes down to how many pathogens you are hoping to test for. On average, the test will look for two or three, but more expensive tests may screen for 10 to 15.
Depending on your insurance and which test you select, it may be covered. Another option is to pay for the Lyme disease test with your HSA/FSA, since some companies will accept that as a payment form.
Read Also: How To Treat Dogs For Lyme Disease
What Are The Symptoms Of Lyme Disease
Lyme Disease is a bacterial infection that results from a tick bite. The symptoms vary, and you can feel sick for months because of it. Some of the most common symptoms of Lyme disease are flu-like symptoms such as fever, chills, and headache. A rash can also occur in 70 to 80 percent of infections. If left untreated, the symptoms can worsen into facial palsy, dizziness, heart palpitations, and more.
How To Remove A Tick
Removing a tick is the same for humans and animals. Its important you do not crush or damage the tick because it could cause Lyme bacteria to pass from the tick into your bloodstream.
How to remove a tick.
Recommended Reading: What Happens When You Have Lyme Disease
How Can Lyme Disease Be Prevented
Tick control and prevention methods significantly reduce the likelihood of infection. Maintaining antibodies against B. burgdorferi through vaccination can further protect your animal. Antibody amounts and duration of vaccine antibodies can vary in individuals. Verifying your animals antibody response to vaccination helps to assure durable protection.
If My Dog Tests Positive Does He Need To Be Treated

The decision to treat Lyme disease is somewhat controversial since many infected dogs show no signs of illness. Factors that would support treatment include:
a moderate to high value of QC6 signs of illness compatible with Lyme disease at the time of testing a history of illness compatible with Lyme disease within the past year the presence of abnormal levels of protein in the urine.
Read Also: Full Recovery From Lyme Disease
Ongoing Symptoms Of Lyme Disease
A few people who are diagnosed and treated for Lyme disease continue to have symptoms, like tiredness, aches and loss of energy, that can last for years.
These symptoms are often compared to fibromyalgia and chronic fatigue syndrome.
It’s not clear why this happens to some people and not others. This means there’s also no agreed treatment.
Speak to a doctor if your symptoms come back, or do not improve, after treatment with antibiotics.
The doctor may be able to offer you further support if needed, such as:
- referral for a care needs assessment
- telling your employer, school or higher education institution that you require a gradual return to activities
- communicating with children and families’ social care
Page last reviewed: 05 July 2021 Next review due: 05 July 2024
Serological Testing Of Csf For The Diagnosis Of Neurological Lyme Disease
Serological testing for neurological Lyme disease is based on demonstrating intrathecal synthesis of Borrelia-specific antibodies in CSF. For laboratory testing for neurological Lyme disease, separate IgG and IgM ViraChip® serology assays are performed on CSF and paired serum and the results compared.
CSF samples must be tested in parallel with a contemporaneous serum sample and protein and immunoglobulin levels compared between the two sample types to produce a meaningful result.
For necessary sample types and volumes see Sample types for Lyme disease testing
Recommended Reading: What Antibiotic Is Used For Lyme Disease
Where Is Lyme Disease Found
In the United States, Lyme disease has been reported in every state, but over 95% of cases are from the Northeastern, Mid-Atlantic, and upper Midwestern states, with a small number of cases reported along the West Coast, especially Northern California. In Canada, Lyme-positive dogs are found mostly in southern Ontario and southern Manitoba, with a small number of cases in southern Quebec and the Maritime provinces.
What If Lyme Disease Goes Untreated
If Lyme disease goes untreated, it can affect other systems in the body. According to the , common symptoms of later stage Lyme disease include:
- severe headaches and neck stiffness
- additional erythema migrans rashes on other areas of the body
- facial palsy, which is a loss of muscle tone or droop on one or both sides of the face
- arthritis with severe joint pain and swelling, particularly in the knees and other large joints
- intermittent pain in tendons, muscles, joints, and bones
- heart palpitations or an irregular heartbeat
- episodes of dizziness or shortness of breath
- inflammation of the brain and spinal cord
- nerve pain
- shooting pains, numbness, or tingling in the hands or feet
Don’t Miss: Diagnostic Procedures For Lyme Disease
Lyme Disease And Your Brain
Ticks transmit the disease by way of blood. The longer the tick is attached to you, the more chance you have of contracting the disease, assuming the tick is infected.
| Related: How the Lone Star Tick Is Making People Allergic to Meat |
Once in your system, the bacteria adapt so as to survive immune system attacks. They decrease the number of surface proteins that will trigger an inflammatory response. In addition to this, another surface protein is created that protects the bacteria from the host immune system.
The overly protected bacteria use the blood to travel and reach organs throughout your body. The ability to cross the blood-brain barrier allows the bacteria to get to your brain. By slipping through the endothelial cells, bacteria get into your brain, which triggers the nervous system changes associated with the disease.
Having previously avoided inflammatory attacks, the bacteria now draws in a larger response which complicates the impacts on your brain. The intense inflammation of the brain is what causes swelling and nervous system damage. It can, however, take years before these symptoms are noticed.
| Related: Why Curcumin Is Linked to Improved Brain Function |
With the symptoms occurring so long after the bite, many people do not link the two events, which lead to misdiagnosis of the disease. Memory problems are the first signs of brain infection and inflammation but additional neurological symptoms can also occur.
Symptoms Of Post Treatment Lyme Disease
- Include severe fatigue, musculoskeletal pain, & cognitive problems
- Can significantly impact patients health and quality of life
- Can be debilitating and prolonged
Our research indicates the chronic symptom burden related to PTLD is significant. Although often invisible to others, the negative impact on quality of life and daily functioning is substantial for PTLD sufferers.
The chronic symptom burden related to Lyme disease is considerable, as shown on the left side of the graph above, and statistically significantly greater than the aches and pains of daily living experienced by the control group, on the right.
Also Check: Northeast Medical Group East Lyme
How A Mom Got Adh To Confirm Lyme Disease
On May 26, 2016, Alarie and Josh Bowerman of Springdale dropped their three daughters off for a Girl Scout camp out for the weekend. Little were they to know how that would change their lives forever as all three girls came down with Lyme disease and other tick-borne diseases from a total of 23 tick bites among them. But since at that time the Arkansas Department of Health denied that Lyme disease was found in Arkansas, it was difficult getting their daughters the correct treatment in time to prevent permanent disabilities.
After their youngest daughter, Emory, has a positive blood test for Lyme, the Bowermans took the two older girls in to be tested, as well.
That is when things got really weird, really fast, Alarie Bowerman said. The on-call pediatrician said he just got off phone with an infectious disease specialist at Arkansas Childrens Hospital who informed him that Emorys test results were a false positive and that we shouldnt give her the antibiotic his colleague prescribed the night before, as it would cause teeth staining.
All three girls had babesiosis and cat scratch fever in addition to Lyme. The oldest, Anais, had Raynauds disease, as well.
Bowerman learned co infections are common. It is almost a given, she said. If you see one, you see others, too. The other co-infections are bad, as well.
But the pediatric clinic didnt want to treat them for a disease that ADH said didnt occur in Arkansas.
Are There Any Risks To Lyme Disease Tests

There is very little risk to having a blood test or a lumbar puncture. If you had a blood test, you may have slight pain or bruising at the spot where the needle was put in, but most symptoms go away quickly. If you had a lumbar puncture, you may have pain or tenderness in your back where the needle was inserted. You may also get a headache after the procedure.
You May Like: Ozone Therapy For Chronic Lyme
What Are The Risk Factors For Post Treatment Lyme Disease
Risk factors for Post Treatment Lyme Disease include:
- Delay in diagnosis
- Increased severity of initial illness
- Presence of neurologic symptoms
Increased severity of initial illness, the presence of neurologic symptoms, and initial misdiagnosis increase the risk of Post Treatment Lyme Disease. PTLD is especially common in people that have had neurologic involvement. The rates of Post Treatment Lyme Disease after neurologic involvement may be as high as 20% or even higher. Other risk factors being investigated are genetic predispositions and immunologic variables.
In addition to Borrelia burgdorferi, the bacteria that causes Lyme disease, there are several other tick-borne co-infections that may also contribute to more prolonged and complicated illness.