Microbiologic Investigations Into Chronic Lyme Disease
There is very little microbiologic evidence that supports persistent B burgdorferi infection in patients who lack objective manifestations of Lyme disease, such as erythema migrans, arthritis, meningitis, and neuropathies. Advocates for CLD contend that our ability to detect B burgdorferi is hampered by current technology and an incomplete scientific understanding of B burgdorferi, and that conventional diagnostic testing misses patients with CLD.55,56 Naturally, this raises the question of why we should assume that chronic B burgdorferi infection exists at all if we are so ill-equipped to detect it. Even when chronically symptomatic patients have a well-documented history of treated Lyme disease, investigators have been unable to document persistent infection.5759 A recent study in which ticks were allowed to feed on persistently symptomatic posttreatment patients yielded molecular evidence of B burgdorferi in 1 of 16 patients and no patient had cultivatable organisms.60
Because validated testing methods fail to support the connection between B burgdorferi and clinically diagnosed CLD, physicians who specialize in CLD often turn to alternative tests. This has included the use of novel culture techniques, detection of B burgdorferi DNA in urine specimens, and enumeration of CD57-positive lymphocytes.6165 Independent investigations, however, have repudiated the validity of these tests.6670
The Chronic Lyme Disease Controversy
Chronic Lyme disease is a poorly defined term that describes the attribution of various atypical syndromes to protracted Borrelia burgdorferi infection. These syndromes are atypical for Lyme disease in their lack of the objective clinical abnormalities that are well-recognized in Lyme disease and, in many cases, the absence of serologic evidence of Lyme disease as well as the absence of plausible exposure to the infection. The syndromes usually diagnosed as CLD include chronic pain, fatigue, neurocognitive, and behavioral symptoms, as well as various alternative medical diagnosesmost commonly neurologic and rheumatologic diseases. Perhaps the most recognized and contentious facet of this debate is whether it is effective, appropriate, or even acceptable to treat patients with protracted antibiotic courses based on a clinical diagnosis of CLD.
Chronic Lyme Disease Vs Post
Patients typically use the term chronic Lyme disease to describe the cluster of symptoms that started after getting Lyme disease and that persist despite having received a course of antibiotic treatment which has been deemed curative by the Infectious Diseases Society of America. Patients say, “I’m not cured. I have symptoms now that I never had before Lyme disease. I’m fatigued 90% of the day. My muscles ache. My brain is in a fog. I can’t think clearly any more. I’m super sensitive to light and sound. What is going on? Chronic Lyme disease does exist – I’m a living example of it!”
Whatever one calls it, the experience is the same. Most often these patients experience profound fatigue, pain, and/or cognitive impairment. Mild to moderate levels of depression and anxiety may also accompany these symptoms, as the functional limitations can lead to social isolation, inability to work, and loss of sense of one’s identity as a provider, caretaker, or friend. Sometimes patients find themselves identifying with Job – the just and good man in the Bible whose life was wrecked by illness, death of loved ones, and economic disaster he felt tormented by God.
Read Also: Lyme Disease Is Caused By
If It Isnt Chronic Lyme What Is It
One day two summers ago, I woke up with a headache behind my right eye and muscle pain in my legs and back. By the end of the day, everything hurt. My skin felt so sensitive I tried not to rest my arm on the table. I was 32 and had always been healthy. I assumed Id get better in a week.
A month went by, and now I had a low-grade fever in addition to daily back and muscle pain. The fever returned at the same time every afternoon, escorted by a host of other strange symptoms: the bridge of my nose burned and swelled , one knee and my jaw seemed to want to unhinge themselves, and I could suddenly, disconcertingly feel my urethraa part of the body that is truly not meant to be felt, in my opinion, but which was now painfully swollen. My right hand sometimes hurt too much to use, and a deep ache radiated through my butt cheeks.
After five months of daily fever and flu symptoms, I was so weak I struggled with stairs. I started spending a significant part of each day in bed. I still wasnt sure what was wrong with me, but I knew it had to be something terrible. So why did test after test continue to come back negative? My primary doctor kept sending me to specialists, but, to my surprise, most of them seemed not to recognize my symptoms as indicating a specific condition.
Extremely general, they said.
Nebulous.
Systemic.
They seemed rushed. They didnt seem to have the time to investigate further.
Take Advil, I was told by several doctors in a row.
Yes, 20.
She did.
A Reasonable Approach To Post
If you are being treated for PTLD, there is no magic bullet to treat this problem, but here are some important steps to consider:
- Choose a doctor you trust and who can work closely with you.
- If your doctor agrees to start antibiotics for several months, make sure you talk about the risks and cost, as this can be dangerous and expensive.
- Make sure not to rely solely on antibiotics. The evidence for a benefit from antibiotics is weak, and we rely mostly on physicians clinical experience and interest in the disease to design a personalized therapeutic plan. For some, a more holistic approach may be the way to go.
- If you try supplements, ask about their source and purity, as they are not FDA-regulated.
- Consider looking for services in medical school hospitals or clinics where they may have programs with ongoing research on how to diagnose and treat Lyme.
About the Author
You May Like: Can Lyme Disease Cause Vertigo
Is Chronic Lyme Disease Real
- Post author:Dr. John Dempster, ND
- Post published:October 12, 2021
As long as we wish to be surrounded by nature and trees, we have to accept the possibility of tick bites and tickborne diseases. And even though many are harmless and cause no noticeable symptoms, there are bacteria, like Borrelia burgdorferi that transmit serious diseases like Lyme disease.
Lyme disease the most commonly transmitted tick-borne infection in North America wasnt recognized as a medical condition until very recently, just some 40-45 years ago! This is even more surprising considering that the bacteria causing Lyme disease has been lurking around for thousands of years. Excavation of a 5,300 year-old mummy, called an Iceman, confirmed that our ancestors also suffered from B. burgdorferi and possibly even Lyme disease.
But it wasnt until the 1960-70s when Lyme disease gained public attention after children in Lyme, Connecticut started having unexplainable symptoms like fatigue, skin rashes, fever, arthritis, etc. If it wasnt for two persistent mothers who pushed the Connecticut State Department of Health to look into this outbreak, we might have still been oblivious to this serious medical condition.
How Is Lyme Disease Treated
For early Lyme disease, a short course of oral antibiotics such as doxycycline or amoxicillin is curative in the majority of the cases. In more complicated cases, Lyme disease can usually be successfully treated with three to four weeks of antibiotic therapy.
In patients who have non-specific symptoms after being treated for Lyme disease and who have no evidence of active infection , studies have shown that more antibiotic therapy is not helpful and can be dangerous.
Read Also: Lyme Disease And Swollen Lymph Nodes
Has Niaid Looked At Whether Infection Persists After Antibiotic Therapy
Several recent studies suggest that B. burgdorferi may persist in animals after antibiotic therapy. In one study, NIAID-supported scientists found that remnants of B. burgdorferi remained in mice after antibiotic treatment. Another team of NIAID-supported investigators found that intact B. burgdorferi persist in nonhuman primates after antibiotic treatment. It was not possible to culture these bacteria and it is not clear whether they are infectious. More recent work by Hodzic et al. replicated the earlier finding of persisting DNA but non-cultivatable B. burgdorferi after antibiotic treatment using a mouse model. In 2017, scientists at the Tulane National Primate Research Centers, funded in part by an NIH research resources grant, reported evidence of persistent and metabolically active B. burgdorferi after antibiotic treatment in rhesus macaques.
In a first-of-its-kind study for Lyme disease, NIAID-supported researchers have used live, disease-free ticks to see if Lyme disease bacteria can be detected in people who continue to experience symptoms such as fatigue or arthritis after completing antibiotic therapy). This study remains underway.
Understanding The Road Forward
A common refrain: Chronic Lyme disease is an easy answer to a seemingly-impossible-to-solve problem. The dialogue over CLD provokes strong feelings, and has been more acrimonious than any other aspect of Lyme disease, Paul M. Lantos, MD, of Duke University, writes in a 2016 paper in the Infectious Disease Clinics of North America. What is clear is that patients are in very real pain, no matter if the cause is Lyme or not, he says. That is something both sides agree on.
But patients are caught in the middle, the medical community is failing them, and theyre suffering for it. Its difficult to be your own advocate when you lack the energy to champion your health. The problem is that patients arent getting taken care of, says Dr. Green.
We wouldnt do this in any other disease. Wed investigate whats going on.
She herself doesnt use the term chronic Lyme, rather she calls it late Lyme, which refers to Lyme disease that was missed or treated ineffectively. causing a lot of illness and morbidity, loss of productive hours, and quality of life, she says.
We wouldnt do this in any other disease, says Dr. Green. Wed change our treatment course or investigate whats going onnot say oh its all in your head.
Recommended Reading: When Is It Too Late To Treat Lyme Disease
Has Niaid Looked At The Potential Benefits Of Long
Yes. NIAID has funded three placebo-controlled clinical trials on the efficacy of prolonged antibiotic therapy for treating PTLDS. The published results were subjected to rigorous statistical, editorial, and scientific peer review.
These trials were designed to ensure that several key parameters were addressed:
- The susceptibility of B.burgdorferi to the antibiotics used
- The ability of the antibiotics to both cross the blood-brain barrier and access the central nervous system and to persist at effective levels throughout the course of therapy
- The ability of the antibiotics to kill bacteria living both outside and inside mammalian cells
- The safety and welfare of patients enrolled in the trials
The first clinical trial, which included two multicenter studies, provided no evidence that extended antibiotic treatment is beneficial. In those studies, physicians examined long-term antibiotic therapy in patients with a well-documented history of previous Lyme disease but who reported persistent pain, fatigue, impaired cognitive function, or unexplained numbness. Those symptoms are common among people reporting PTLDS. Patients were treated with 30 days of an intravenous antibiotic followed by 60 days of an oral antibiotic.
In 2016, a clinical trial conducted in the Netherlands also concluded that in patients with persistent symptoms attributed to Lyme disease, longer term treatment with antibiotics did not provide additional benefits compared with shorter term regimens.
Legal Mandates To Cover Unproven Treatments
The state of Connecticut, meanwhile, enacted a law on June 18, 2009, “to allow a licensed physician to prescribe, administer or dispense long-term antibiotics for a therapeutic purpose to a patient clinically diagnosed with Lyme disease.” The states of Rhode Island, California, Massachusetts, New Hampshire, Vermont, New York, Maine, and Iowa have similar laws.
Massachusetts and Rhode Island have laws mandating insurance coverage for long-term antibiotic therapy for Lyme disease when deemed medically necessary by a physician. In 1999 Connecticut had passed a similar, though somewhat more restrictive law.
Don’t Miss: How Do You Feel When You Have Lyme Disease
Chronic Lyme Dos And Don’ts
Chronic Lyme disease is an ongoing Borrelia burgdorferi infection that can involve any body system or tissue. The infection produces a wide range of symptoms and signs, which can be debilitating for some patients. Common symptoms include severe fatigue, migratory musculoskeletal pain, headaches, and impaired memory. Unfortunately, chronic Lyme disease is complex and often misunderstood, which means that many patients will struggle to obtain the care they need to regain their health. Every patient concerned about Lyme disease and tick-borne illness should know the following.
How You Get Lyme Disease
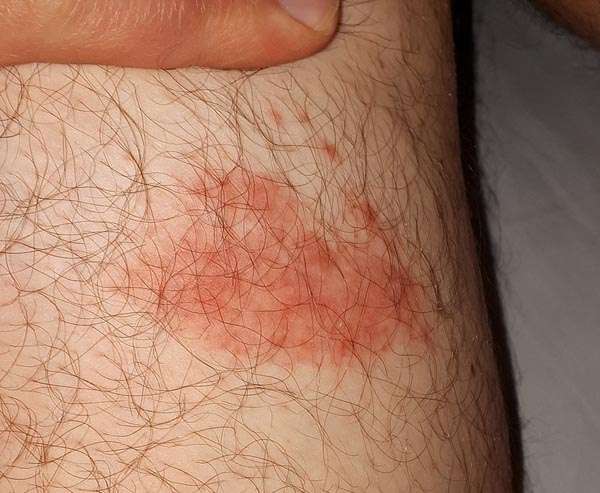
If a tick bites an animal carrying the bacteria that cause Lyme disease, the tick can become infected. The tick can then transfer the bacteria to a human by biting them.
Ticks don’t jump or fly. They climb on to your clothes or skin if you brush against something they’re on. They then bite into the skin and start to feed on your blood.
Generally, you’re more likely to become infected if the tick is attached to your skin for more than 24 hours. Ticks are very small and their bites are not painful, so you may not realise you have one attached to your skin.
Recommended Reading: When To Test For Lyme Disease
Study Shows Evidence Of Severe And Lingering Symptoms In Some After Treatment For Lyme Disease
In a study of 61 people treated for the bacteria that causes Lyme disease, Johns Hopkins researchers conclude that fatigue…
In a study of 61 people treated for the bacteria that causes Lyme disease, Johns Hopkins researchers conclude that fatigue, pain, insomnia and depression do indeed persist over long periods of time for some people, despite largely normal physical exams and clinical laboratory testing.
Post-treatment Lyme disease syndrome is a real disorder that causes severe symptoms in the absence of clinically detectable infection, says John N. Aucott, M.D., associate professor of medicine at the Johns Hopkins University School of Medicine and director of the Johns Hopkins Lyme Disease Clinical Research Center.
The findings, published in the December issue of Frontiers in Medicine, could spur further investigation into the cause of persistent symptoms, a source of medical controversy. As Lyme disease rates have steadily climbed in the United States since it was first recognized in the mid-1970s, so have reports of a collection of symptoms that patients commonly refer to as chronic Lyme disease. Experts in the field have questioned the validity of this term because of the lack of direct evidence in this group of patients of ongoing infection with Borrelia burgdorferi, the bacterium that causes Lyme disease.
Other Johns Hopkins researchers who participated in this study include Alison W. Rebman, Ting Yang, Erica A. Mihm, Mark J. Soloski and Cheryl Novak.
Defining Patient Subgroups: Post
Patients with persistent symptoms related to Lyme disease likely represent a heterogeneous population, which includes previously untreated patients, as well as those treated patients who remain symptomatic. As a result, some will manifest primarily patient-reported symptoms while others will present with symptoms in conjunction with objective, physical findings. This heterogeneity is further complicated by variation in terminology and the definitions used by different groups in the field.
Figure 3. A schematic of clinical- and research-defined patient subgroups among those with persistent symptoms associated with Lyme disease . The size of each patient subgroup is not meant to represent actual population frequency, as prevalence data is extremely limited. IDSA, Infectious Diseases Society of America ILADS, International Lyme and Associated Diseases Society CLD-PT, Chronic Lyme Disease-Previously Treated CLD-U, Chronic Lyme Disease-Untreated IgG, Immunoglobulin G CFS, Chronic Fatigue Syndrome FM, Fibromyalgia.
Also Check: Lyme Nephritis Symptoms In Dogs
The Problem With Cld Symptoms
Its that theyre common: Musculoskeletal pain, fatigue, headache, poor sleep, or low moodall things that are ascribed to CLDthese are symptoms that CDC studies show a fair amount of the adult population complains about, says Paul Auwaerter, MD, clinical director in the division of infectious diseases at Johns Hopkins Medicine and an expert on tick-borne diseases.
Kovacs spent years bouncing from specialist to specialist to try to tackle each problem as it camethe cardiologist after spells of dizziness and fainting, the GI doc for digestive problems. Because of that, it was so easy to fall through the cracks, she says. Her symptoms spanned everything from low blood pressure to joint pain to dizziness and confusion to clumsiness and migraines.
The Ashland, KY resident, who now runs the blog Lady of Lyme, wouldnt be told she has chronic Lyme disease until September 2011, more than five years after falling ill. She never found a tick bite, but says she had spent time in the woods and never checked her body after.
This is where things get complicated: If you didnt find an attached tick on your body, didnt see a rash, or didnt test positive for the bacteria, how can doctors be sure that youre feeling run down, foggy, and achy because of Lyme? What if you live in a state where Lyme isnt rampant?
What Is Chronic Lyme Disease
Lyme disease is an infection caused by the bacterium Borrelia burgdorferi. In the majority of cases, it is successfully treated with oral antibiotics. In some patients, symptoms, such as fatigue, pain and joint and muscle aches, persist even after treatment, a condition termed Post Treatment Lyme Disease Syndrome .
The term chronic Lyme disease has been used to describe people with different illnesses. While the term is sometimes used to describe illness in patients with Lyme disease, it has also been used to describe symptoms in people who have no clinical or diagnostic evidence of a current or past infection with B. burgdorferi . Because of the confusion in how the term CLD is employed, and the lack of a clearly defined clinical definition, many experts in this field do not support its use.
Recommended Reading: Common Symptoms Of Lyme Disease