What Are The Risks Of A Lumbar Puncture
Risks that exist and about which the patient must be informed include:
- bleeding and bruising
- Circulatory and consciousness disorders
- Temporary nerve failures with numbness or paralysis
In patients suffering from seizure disorders such as epilepsy or migraines , a lumbar puncture can trigger a seizure.
Another risk is the so-called CSF low pressure syndrome, in which the patient suffers from headaches, stiff neck, ringing in the ears , nausea and sensitivity to light. It can occur after a CSF puncture when the patient sits up or stands up from a lying position. The symptoms can be alleviated by the administration of certain medications such as theophylline or an autologous blood injection into the epidural gap . The use of the thinnest possible puncture needle and a correct insertion angle reduces the risk of developing a CSF hypotension syndrome.
Risk Factors For Lyme Disease
Several factors increase the risk of acquiring and the spread of Lyme disease. These include
- Age and sex. Men between the ages of 15 to 60 are most likely to play outside and go on outdoor activities such as camping, hunting, and hiking.
- Socioeconomic factors. Those people who live and work outdoors, in construction, landscaping, near the farm, park, wildlife, or forest.
- Geographic location. Ticks that carry Lyme disease are widespread but are mostly found in the northeast, upper midwest, and mid-Atlantic states and south-central and southeast Canada.
- Weather conditions. Tick bites are common during summer when people spend more time outdoors but it is also possible during early fall and late winter with extremes of temperatures.
- Environmental factors. Spending time in moorland and woodland areas with deep or overgrown plants with animals to feed the ticks and an increase in deer population where the ticks thrive.
- Pet. Taking care of a pet, especially a dog, increase the risk for Lyme disease.
Signs And Symptoms Of Lyme Disease
Lyme disease can produce a wide range of symptoms if left untreated. The symptoms depend on the stage of infection, such as:
- Stage 1. This stage is called early localized disease, which happens within 3 to 30 days after a tick bite. It starts with a single-circle rash that spreads around the site with a clear center which is not painful or itchy but warm to the touch also called erythema migrans . Other symptoms include fever, headache, fatigue, muscle pains, joint stiffness, nausea, upper respiratory problems, and swollen lymph nodes.
- Stage 2. This stage is called early disseminated disease, with more serious and widespread symptoms often showing within 3 to 10 weeks after a tick bite. Symptoms include rashes on different parts of the body, severe headache, neck pain or stiffness, facial muscle weakness, Bannwarth syndrome, dysrhythmias, fainting, shortness of breath, paresthesia, back pain radiating to the hips and legs, eye pain, swelling, or vision loss.
- Stage 3. This stage is called late disseminated disease and usually begins 2 to 12 months after a tick bite. Symptoms include long-lasting pain and swelling, arthritis in large joints, peripheral neuropathy, acrodermatitis chronic atrophicans, heart problems, insomnia, memory or concentration problems, and swelling/discoloration of the hands, feet, elbows, and knees.
Recommended Reading: Can Lyme Disease Cause Seizures In Dogs
How Do You Check For A Vacuum Leak With Soapy Water
If you suspect that you have a vacuum leak in a specific area, you can use soapy water in a spray bottle to see if there is a problem. Spray soapy water on the suspect area while the car is running. If the cars idle levels out after you spray the soapy water, then it is likely that it has temporarily blocked the leak.
What Is A Lumbar Puncture
During a lumbar puncture, nerve fluid is removed. To do this, the doctor uses a thin puncture needle, which he inserts into the spinal cord canal at the level of the lumbar spine . From this, the nerve fluid drips into a sample container. During the CSF examination, the doctor examines the cerebrospinal fluid for the presence of various cells, such as blood or inflammatory cells.
Don’t Miss: How Do I Know If I Have Lyme Disease
Lyme Disease Nursing Care Plan 5
Nursing Diagnosis: Self-care Deficit related to musculoskeletal impairment secondary to Lyme disease as evidenced by poor personal hygiene.
Desired Outcomes:
- The patient will be able to perform personal hygiene measures within their level of ability.
- The patient will be able to demonstrate independence in completing personal needs through the appropriate use of adaptive equipment.
Lyme Disease Nursing Care Plan 4
Nursing Diagnosis: Acute Pain related to peripheral neuropathy secondary to Lyme disease as evidenced by verbalization of tingling sensations and numbness.
Desired Outcomes:
- The patient will be able to adapt skills to manage the sensory disturbances with the long-term treatment of Lyme disease.
- The patient will be able to resume activities of daily living with minimal supervision and assistance.
Also Check: Natural Treatment For Dog Lyme Disease
Lumbar Puncture As A Diagnostic Tool
The cerebrospinal fluid puncture is used to prove or rule out various diseases:
- Brain and spinal cord tumors
- Cancer of the meninges , for example in lymphomas
- inflammatory diseases of the brain or the meninges
- Infectious diseases
- subarachnoid hemorrhage
- multiple sclerosis
In addition, the doctor can measure the pressure inside the skull as part of the CSF diagnostics in order to determine an expansion of the so-called CSF spaces .
Are There Any Risks To Lyme Disease Tests
There is very little risk to having a blood test or a lumbar puncture.
With a blood test, you may have slight pain or bruising at the spot where the needle was put in, but most symptoms go away quickly.
With a CSF test, you may feel a little pinch or pressure when the needle is inserted. After the test, you may feel some pain or tenderness in your back where the needle was inserted.
You may also have some bleeding at the site or get a headache. The headache may last for several hours or up to a week or more, but your provider may suggest treatment to help relieve the pain.
Read Also: Best Diet For Lyme Disease Patients
Is There Anything Else I Need To Know About Lyme Disease Tests
At-home test kits for Lyme disease are available. To do these tests, you usually collect a drop of blood from your finger and send it to a lab for testing. If you want to do an at-home test, it’s important to talk with your provider first. Some at-home tests may use lab methods that aren’t proven to work, so your results may not be accurate.
What Are The Indications For Lumbar Puncture In Patients With Lyme Disease
Log in to MyKarger to check if you already have access to this content.
Buy a Karger Article Bundle and profit from a discount!
If you would like to redeem your KAB credit, please log in.
Save over 20%
- Immediate access to all parts of this book
- Cover-to-cover formats may be available
- Unlimited re-access via MyKarger
The final prices may differ from the prices shown due to specifics of VAT rules.
You May Like: How Long For Lyme Disease Symptoms To Appear
What Do I Have To Consider After A Lumbar Puncture
After the lumbar puncture, you should lie on your stomach for about half an hour to prevent the cerebrospinal fluid from flowing back. In the first few hours after the puncture, you should remain in bed as much as possible. However, they are allowed to go to the toilet independently or sit up at meals.
Lyme Disease Nursing Care Plan 1

Nursing Diagnosis: Risk for Impaired Skin Integrity related to impaired sensation secondary to Lyme disease
Desired Outcomes:
- The patient will be able to verbalize awareness of the risk of loss of sensation with Lyme disease.
- The patient will collaborate with the nurse in planning care to maintain uncompromised skin and tissue integrity.
- The patient will be able to prevent the development of the condition from complications.
Recommended Reading: What Tests Are Done For Lyme Disease
What Do The Results Mean
Lyme disease is difficult to diagnose. The symptoms are common to many conditions, and test results alone can’t diagnose the disease. To make a diagnosis, your provider will consider your test results along with your medical history, exposure, and symptoms. You may also need other tests.
A negative blood test result means that antibodies to fight the Lyme disease bacteria were not found in your blood. If you had symptoms for longer than 30 days before your test, you probably don’t have Lyme disease.
But if you had symptoms for less than 30 days before you gave your blood sample, you may need to have another Lyme disease test. That’s because it may take a few weeks for your body to make enough antibodies to show up on a test. If your test was done too soon, you could be infected even though your test was negative. This is called a “false negative.”
A positive blood test result means that antibodies to fight the Lyme disease bacteria were found in your blood. In this case, the Centers for Disease Control and Prevention recommends a second blood test on the same blood sample. If the second test is positive and you have symptoms of infection, you probably have Lyme disease.
But positive test results don’t always mean that Lyme disease is causing your symptoms. You could have antibodies from a past case of Lyme disease that your body successfully fought off months or even years ago.
Learn more about laboratory tests, reference ranges, and understanding results.
Lumbar Puncture Not All That Helpful For Diagnosing Lyme Neuroborreliosis
Welcome to another Inside Lyme Podcast with your host Dr. Daniel Cameron. In this episode, Dr. Cameron will be discussing a case which examines the diagnostic value of a lumbar puncture in Lyme neuroborreliosis.
The case was first described by Portales-Castillo and colleagues in the journal Cureus in a paper entitled To Lumbar Puncture or Not to Lumbar Puncture. The authors presented a case of early disseminated Lyme neuroborreliosis with manifestations of facial palsy and painful radiculoneuritis as determined by clinical and serological criteria.¹
A 61-year-old woman was admitted to the hospital with an inability to close her left eye and an odd sensation on part of her face. She presented with erythematous raised circled rash and swelling on the base of the index finger of her right hand.
She thought she might have been bitten by a spider two days prior and was therefore treated with cephalexin for a presumed cellulitis.
Three weeks later, she started to develop posterior dull neck pain, along with bilateral arm pain and arm weakness. Her symptoms progressed to the point where she could no longer comb her hair.
The pain later became associated with progressive arm weakness, which continued to progress over the following three weeks up to the point where she could not comb her hair, the authors wrote.
The woman then developed Bells palsy. A Lyme disease IgM Western blot test was positive, consistent with acute Lyme disease.
References:
Also Check: Lyme Disease Specialist Hudson Valley Ny
Why Do I Need A Lyme Disease Test
You may need a test if you have symptoms of infection and were exposed or possibly exposed to ticks that carry the bacteria that causes Lyme disease. The first symptoms of Lyme disease usually show up between 3 and 30 days after the tick bite.
Early signs and symptoms may include:
- A reddish round skin rash that slowly gets bigger over several days. It usually doesn’t itch or hurt, but it may be warm. As it gets better, it may look like a bull’s-eye , but not always.
- Muscle and joint aches
- Swollen lymph nodes
Later signs and symptoms of Lyme disease usually affect your joints and nervous system. They include:
- Severe headaches and neck stiffness
- Rashes on other parts of your body
- Arthritis with severe joint pain and swelling, especially in the knees
- Pain that comes and goes in your muscles, joints, bones, and tendons
- Shooting pains, numbness, or tingling in your hands or feet
Lyme Disease Nursing Care Plan 2
Nursing Diagnosis: Hyperthermia related to infectious process secondary to Lyme disease as evidenced by a temperature of 102.4 degrees Fahrenheit, weakness, and dehydration.
Desired Outcomes:
- The patient will be able to maintain a normal body temperature between 97.8 to 98.6 degrees Fahrenheit within 24 hours.
- The patient will display an increase in energy as evidenced by active participation in activities of daily living.
- The patient will display adequate tissue perfusion as evidenced by normal skin turgor.
Don’t Miss: Is There A Cure For Chronic Lyme Disease
Early Disseminated Lyme Neuroborreliosis
The classic triad of this stage, also known as meningoradiculoneuropathy, includes aseptic meningitis, cranial neuropathy, and painful radiculoneuritis which may occur alone or in combination. Acute encephalomyelitis is seen less frequently. Neurologic signs and symptoms develop from weeks to months after inoculation. The onset is acute or subacute. Accompanying erythema migrans and systemic signs and symptoms characteristic of early disseminated Lyme neuroborreliosis, may be present in up to two-thirds of cases. Neurologic involvement can occur without erythema migrans, however, and can be the first manifestation of the disease. Only 40% of patients recall tick bite. The absence of a history of travel to or residence in an endemic area tends to warn the clinician against the diagnosis of Lyme neuroborreliosis.
About two-thirds of patients with early disseminated Lyme neuroborreliosis have cranial neuropathies which can occur without other neurologic or systemic features and without preceding erythema migrans. The facial nerve is involved most commonly, although any of the cranial nerves may be involved. Remarkably, bilateral facial palsy is seen in approximately one-third of such cases. The differential diagnosis of bilateral facial palsy includes Guillain-Barre syndrome, acquired immunodeficiency syndrome , various other causes of meningitis, and Tangier’s disease.
How A Lumbar Puncture Can Help Diagnose Ms
The fluid that is drawn off in a lumbar puncture is analysed to look for a number of different things.
- White blood cells. If you have multiple sclerosis, then the number of white cells in your cerebrospinal fluid is usually up to seven times higher than normal. If the count is even higher than this, it is probably due to an infection of some sort, such as Lyme disease, and not MS.
- Neurofilaments. These are fragments of the structural support that normally surrounds your nerve axons. If neurofilaments are found in the CSF, then this is evidence that your myelin is under attack. If you have a subsequent lumbar puncture and fewer neurofilaments are found than before, this could be evidence that your disease-modifying drugs are effectively protecting the nerves.
- Oligoclonal bands. The immune system produces antibodies to fight infection. In MS, antibodies cross the blood-brain barrier and attack the myelin surrounding nerves. As a result, the level of antibodies in the cerebrospinal fluid of someone with MS is higher than it should be. It will also be higher than the level in the blood, so a blood sample will usually be analysed at the same time for comparison.
The test that shows the presence of antibodies is called electrophoresis. A sample of fluid is placed on a gel and voltage is applied. This causes antibodies of the same size to bunch together, forming visible ‘bands’.
Recommended Reading: Chances Of Getting Lyme Disease From A Tick
Lyme Disease Nursing Care Plan 3
Nursing Diagnosis: Fatigue related to prolonged infection secondary to Lyme disease as evidenced by general body discomfort and muscle weakness.
Desired Outcomes:
- The patient will verbalize improvements in fatigue after 72 hours of nursing interventions.
- The patient will be actively engaged with the daily activities independently.
Treatment For Lyme Disease

The chance of recovery from Lyme disease increases with early detection and treatment. This includes
- Medications. Used to relieve signs and symptoms and the infection associated with Lyme disease.
- NSAIDs.This is given for persistent pain associated with Lyme disease.
- Antibiotics. Early-stage Lyme disease usually follows a course of 10 to 14 days of oral antibiotic treatment. For severe or late disseminated infections intravenous antibiotic administration is recommended. The second round of antibiotic treatment is given if the swelling persists or recurs. Prolonged antibiotic treatment is recommended only for up to 28 days. Lyme arthritis or diseases affecting the heart and nervous system also requires an IV antibiotic treatment.
- Removing ticks. Use tweezers by applying them near the head or mouth of the tick while gently pulling it, making sure that all the tick parts have been removed. Wash hands and the site of the tick bite with soap and water then clean with rubbing alcohol.
- Physical therapy. This is recommended following the resolution of Lyme arthritis in adult patients.
- Pacemaker. Heart conduction abnormalities for patients with Lyme disease usually resolve within 6 weeks but some may end up with a permanent pacemaker or persistent heart block.
- DMARDs or synovectomy. It can accelerate recovery in patients with Lyme arthritis.
Also Check: Hydrogen Peroxide Treatment For Lyme Disease
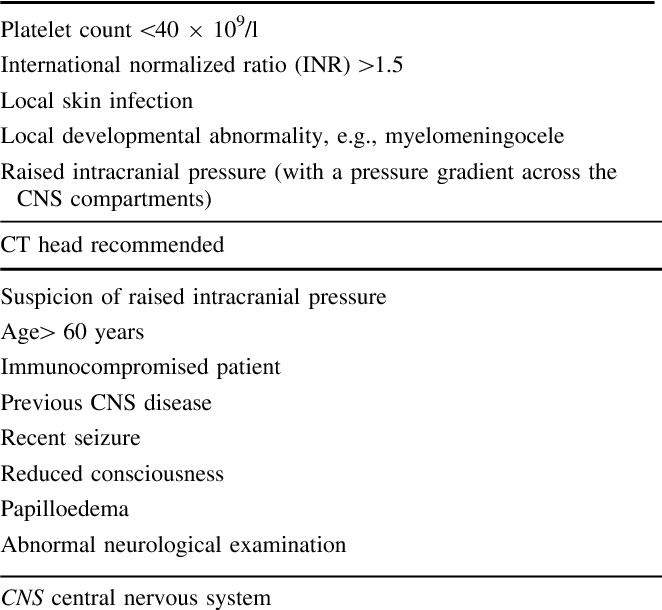
Key Points For Healthcare Providers
Lumbar Puncture For Therapy
Drugs can be introduced into the spinal canal through the puncture needle. These include, for example, local anesthetics or chemotherapeutic agents. If a patient has normal pressure hydrocephalus, i.e. an expansion of the liquor spaces without an increase in pressure, the fluid spaces can be relieved by means of a lumbar puncture by draining cerebrospinal fluid.
You May Like: Early Signs Of Lyme Disease In Adults