What Is Lyme Disease
Lyme disease is a bacterial infection caused by the bacteria Borrelia burgdorferi, affecting an estimated 329,000 individuals in the United States each year. It is spread through the bites of infected blacklegged ticks, commonly known as deer ticks.
Lyme disease can cause fatigue, fever, and joint and muscle pain. When treated with antibiotics in the early stages, most people make a quick and complete recovery. If left untreated, Lyme disease can lead to serious joint and nervous system complications.
Mitochondria Dysfunction And Chronic Pain
Mitochondria are the energy factories found in every cell. By some estimates there are 300 to 400 mitochondria in a cell. Chronic infection can damage the mitochondria. There is a growing body of science showing damaged mitochondria leads to chronic pain.
Lyme Disease Pain Strategy
It is possible to repair mitochondria. See How to Fix Mitochondria & Get Energy in Lyme Disease for steps to repair the injured mitochondria.
One other strategy is to eat low inflammatory foods which support mitochondria. See The Best Brain, Inflammation, Pain, Energy, and Detox Diet Ever for more information about an effective paleo diet.
Early Detection Is Key
Lyme disease is easiest to treat at the early or acute stage, within the first 30 days of exposure. This is why its so important to take precautions to prevent tick bites, both during and outside of tick season. Protect yourself when near potential tick habitats, always perform tick checks after outdoor activity , and dont delay seeking medical attention if you notice any symptoms that might be related to tick-borne illness. Its important to get tested as soon as possible for the best chances of recovery.
Read Also: Beach Houses For Sale In Old Lyme Ct
Lyme Disease And Leaky Gut Syndrome
Small intestine inflammation more commonly known as leaky gut syndrome is a condition where the spaces between the cells that line the small intestine become enlarged. This allows bacteria and food particles to enter the bloodstream triggering the immune system to respond by releasing inflammatory cytokines. The outer layer of bacteria that enters the bloodstream contains fat and a carbohydrate called lipopolysaccharide that causes the immune system to react. Food allergies, alcoholism, stress, infections , toxicants, certain medications, and mast cell activation syndrome are some of the causes of increased intestinal permeability. Paradoxically, leaky gut syndrome also leads to an increase in food allergies since food proteins pass through the inflamed small intestine into the bloodstream creating an antibody response.
Leaky gut syndrome can lead to systemic inflammation which contributes to fatigue, headaches, joint pain, ADHD, and brain fog. Research has demonstrated leaky gut syndrome can contribute to autoimmune conditions. Since many of the symptoms related to Lyme disease are caused by inflammation, successfully treating leaky gut syndrome is crucial to reducing the systemic inflammatory burden.
Imaging For Lyme Arthritis
X-rays are a helpful diagnostic tool to identify the cause of arthritis and pain. Joint space narrowing is the hallmark finding on X-ray in osteoarthritis, and not seen in other causes of joint pain. Lyme disease rarely causes changes of the bones on X-ray.
Soft tissue swelling will be seen with Lyme disease and trauma, not in other conditions.
An MRI of a joint is useful at differentiating Lyme arthritis from septic arthritis or structural damage. In Lyme disease, an MRI will demonstrate joint effusion, synovitis, and muscle edema .
Recommended Reading: Signs And Symptoms Of Lyme Disease In Child
Read Also: Lyme Disease In Dogs Prognosis
The Sneaky Explanation Behind Increased Painful Lyme Disease Symptoms
While Lyme disease is often associated with painful symptoms, inflammation in the peripheral and central nervous systems can increase the discomfort.
While Lyme disease is often associated with painful symptoms, inflammation in the peripheral and central nervous systems can increase the discomfort.
Caused by a bite from a tick with spirochete Borrelia burgdorferi , Lyme disease has the potential to leave patients in debilitating situations. The illness can lead to arthritis and carditis, and when the nervous system is involved, called Lyme neuroborreliosis , it can cause muscle weakness, sensory loss, facial nerve palsy, and limb and neurogenic pain in the back, legs, and feet.
Researchers from the Tulane National Primate Research Center and Louisiana State University Health Sciences Center explored how inflammation levels in the central nervous system, spinal nerves, and dorsal root ganglia played a role in symptom intensity.
These results suggest that inflammation has a causal role in the pathogenesis of acute Lyme neuroborreliosis, one of the authors Mario T. Philipp, PhD, said in a news release.
All of the infected animals except for the group treated with dexamethasone had increased cell counts, mostly made up of white blood cells, along with more of the inflammatory mediators, interleukin.
Related Content:
Lyme Disease: A Short Primer For Pain Practitioners
Gudin J. Lyme Disease: A Short Primer for Pain Practitioners. Pract Pain Manag. 2014 14.
Recently, the Centers for Disease Control and Prevention dramatically increased the estimate of the annual number of new cases of Lyme Disease in the United States from 30,000 to 300,000, with 14 states accounting for over 96% of cases reported.¹ In the United States, Lyme disease is most common in northeastern states, from Virginia to Maine Upper Midwest states, mostly Wisconsin and Minnesota and the West Coast, mainly in the northwest.
The number of new LD cases each year certainly qualifies this infection as an epidemic or at least a highly endemic disease. Consequently, pain practitioners must familiarize themselves with the signs and symptoms of LD. This article is a short primer on LD to give the pain practitioner some basic information and guidance. Given the magnitude of LD, Practical Pain Management will seek to expand on LD research in future issues.
Read Also: Coldwell Banker Old Lyme Ct
How Is Lyme Disease Diagnosed
As the symptoms and signs of Lyme disease are similar to those found in other conditions and are nonspecific, diagnosis is not easy. In addition to this, the ticks that spread the disease can also transmit other diseases at the same time.
Diagnosis is easier when your doctor can see that you have the characteristic bulls eye rash. However, if you dont, your doctor will ask you about your medical history, whether youve been outdoors in summertime, where you have been outdoors and will give you a medical examination.
Lab tests enable bacteria antibodies to be detected in order to confirm a diagnosis. They are most reliable when youve had the infection for a few weeks, as your body will then have had the time to develop the antibodies.
Tests for Lyme disease include:
- Enzyme-linked immunosorbent assay test. This is the test most commonly used to diagnose Lyme disease, and it detects antibodies to Borrelia burgdorferi bacteria. Sometimes the test brings up a false-positive so its not typically used as the sole test for diagnosis.
Although the test may not show as a positive result during the first stage of Lyme disease, often the accompanying rash is distinctive enough to make the diagnosis, especially if youve been in an area where Lyme disease-transmitting ticks are common.
- Western blot test. If the initial ELISA test comes back positive, the Western blot test will confirm your diagnosis.
Back Pain In Child Caused By Lyme Disease: A Case Report
Science Direct has just published a case report of a child in Massachusetts that was diagnosed and treated in the ER with isolated Lyme radiculoneuritis . The childs symptoms included fever and allodynia of the upper back. Though isolated radiculoneuritis is considered to be a rare presentation of early disseminated Lyme disease, authors state that this syndrome is likely underrecognized.
Laboratory results for the patient showed elevated inflammatory markers as well as a positive test for Borrelia. Additionally, nerve root enhancement was observed in C5-C6 and C6-C7 of the spine through MRI exam with contrast. The child was treated with oral doxycycline and symptoms resolved.
Access to the full text article can be found here
Read additional LDA articles on Lyme symptoms in children here
LDA May Lyme Awareness Blogs Begin May 1
Topics of Guest Blogs:Guest Blog Page of the website.
Pat Smith: Milestones in 47-year History of Lyme Disease & Her Story
Presented by PA Lyme Resources Impact SeriesMay 2022
The HHS Tick-Borne Disease Working Group, Washington, DC, created by legislation including patient/advocate representation, presents recommendations to Congress on Lyme & TBD every two years. Read More
Upcoming Events
There are no upcoming events at this time.
Support LDA, no cost to you: Shop Amazon or iGive
Lyme Disease Association, Inc.
Save this Information for Your Records:
LDA does not accept or reply to any comments on:
Don’t Miss: Treatment Plan For Lyme Disease
The Chance Of Getting Lyme Disease
Not all ticks in England carry the bacteria that causes Lyme disease.
But it’s still important to be aware of ticks and to safely remove them as soon as possible, just in case.
Ticks that may cause Lyme disease are found all over the UK, but high-risk places include grassy and wooded areas in southern and northern England and the Scottish Highlands.
Ticks are tiny spider-like creatures that live in woods, areas with long grass, and sometimes in urban parks and gardens. They’re found all over the UK.
Ticks do not jump or fly. They attach to the skin of animals or humans that brush past them.
Once a tick bites into the skin, it feeds on blood for a few days before dropping off.
Managing Chronic Pain For Lyme Disease Patients
Lyme disease is a debilitating condition that can, unfortunately, produce symptoms even after the illness has been treated. As we had mentioned in our blog overview, a rash in the form of a bulls-eye pattern is generally the first indication of an infected tick bite . Following the rash, flu-like symptoms typically develop such as fatigue, fever, chills, body aches, and headache.
If the illness is left untreated, chronic joint pain and neurological problems like meningitis, Bells palsy, numbness or weakness in the limbs, and impaired muscle movement may also occur. In these cases, a pain management program is often beneficial to mitigate symptoms.
At Tulsa Pain, managing chronic pain in Lyme disease patients often requires a multidisciplinary treatment approach. Pain medication, although effective, is not the only method for controlling pain and discomfort, which is why its imperative patients see a pain specialist for care. Patients should see their primary physician for antibiotics to control of their infection and a pain management specialist at Tulsa Pain to establish a positive patient experience and continuum of care.
Treatment for chronic pain in Lyme disease patients may include a combination of the following:
- Electrical stimulation
Also Check: What Do Ticks That Carry Lyme Disease Look Like
Is Lyme Disease Contagious
There is no evidence that Lyme disease is contagious. You can’t get infected from touching, kissing, or having sex with a person who has Lyme disease, or from receiving a transfusion of their blood. Untreated Lyme disease during pregnancy can lead to infection of the placenta, but new mothers cannot transmit the disease to their baby through breast milk.
When Should You See A Doctor If You Think You Have Lyme
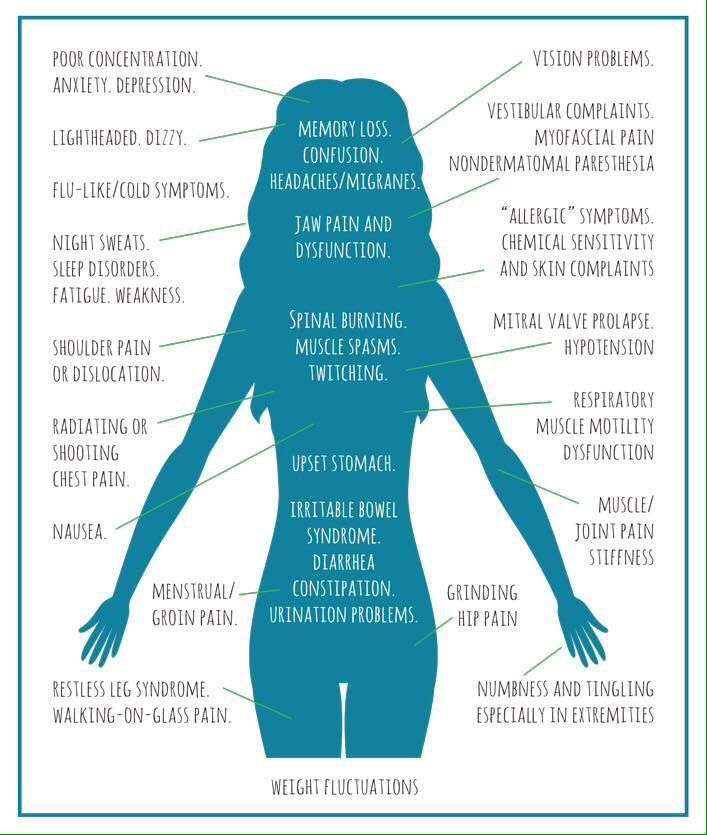
The rash is a pretty good indication that you may have been bitten. Take a photo of the rash and see your doctor. At this stage, treatment with antibiotics will probably work.
If you don’t have the rash but have symptoms like fatigue, fever, and headache but no respiratory symptoms like a cough, you may want to talk to your doctor.
Recommended Reading: Natural Treatment For Lyme Disease In Humans
Strategies For Managing Nerve Pain
1. Reduce Your Microbial Burden
When youre dealing with Lyme disease and co-infections, its not always easy to pinpoint which stealth pathogen is affecting your nervous system. In fact, its most reasonable to recognize that all sneaky microbes are capable of disrupting immune function and causing it to go awry.
When your bodys microbial burden becomes too great, your microbiome becomes imbalanced, driving inflammation and aggravating neuropathy. Thus, at the top of the priority list is decreasing the infectious load to normalize and calm the immune system.
When youre looking for natural solutions to lessen the impact of stealth pathogens, herbal therapy can play a critical role. Not only do herbs have antimicrobial properties, but they are anti-inflammatory and contain antioxidants as well.
Moreover, herbs dont disrupt the delicate balance of the microbiome like synthetics medications do. Some of my favorite herbs with antimicrobial and immunomodulating properties to keep in mind include:
2. Use Medications Cautiously
When it comes to neuropathy, the reality is that sometimes you need some extra support to get your pain levels to a tolerable level. There are a variety of over-the-counter and prescription medications that may be useful from time to time.
However, the value of medications is limited to short term management of symptoms because of cumulative side effects. The list of medications commonly recommended by healthcare providers includes:
Risk Factors For Acquiring Lyme Disease
Where you vacation or live, as well as what outdoor activities you participate in, affects your likelihood of being exposed to Lyme disease. Common factors that put you at risk of contracting Lyme disease include:
- Spending time in grassy or wooded areas. Deer ticks are very prevalent in the Central PA area due to its heavily wooded countryside. Deer ticks thrive in these types of places. Children here are particularly at risk as well as adults who work outdoors.
- Having exposed skin. Ticks find it easy to attach themselves to exposed skin, so if youre in an area thats known for ticks, always wear long sleeves and long pants and never allow your pets to run through long grasses.
- Removing ticks incorrectly or not quickly enough. As you already know, bacteria from a tick bite has the potential to enter your bloodstream if the tick has been attached to you for between 36 to 48 hours or longer. If you spot and correctly remove the tick within 48 hours, your risk of acquiring Lyme disease is low, so always check your skin after being outdoors.
The Centers for Disease Control and Prevention notes that older adults and children are most susceptible to the disease, along with others, like park rangers and firefighters, who spend time outside. Its estimated that 300,000 people nationwide are diagnosed with Lyme disease each year.
You May Like: Arizona Lyme Disease Treatment Center
Lyme Disease Vs Rheumatoid Arthritis
Lyme disease can sometimes be confused for other conditions, and its not uncommon for patients presenting with Lyme disease-related joint pain to be misdiagnosed with . Both Lyme and RA cause joint pain and can be debilitating when left untreated, but there are differences.
-
Lyme arthritis tends to manifest in larger joints , on one side of the body. Lyme joint pain tends to come and go.
-
Rheumatoid arthritis occurs more often in the hands, feet, fingers, and toes, and shows up on both sides of the body. RA joint pain and stiffness occurs every day, and is usually chronic.
-
Lyme disease usually goes away when treated, and most patients make a full recovery.
-
can manage symptoms and show the progression of the disease, but there is no cure.
Lyme pain can often migrate throughout the body, and patients may have pain in their knee one week, and in their wrists the following week, says Chicago-based integrative medicine specialist Casey Kelley, MD. With rheumatoid arthritis, the pain often stays where it begins and does not migrate.
Getting Lyme puts you at greater risk for later developing RA and other types of inflammatory arthritis. One study found that nearly one-third of participants who had Lyme-arthritis later developed an inflammatory arthritis.
Why Do My Hips Acheday And Night
HI..I am 52 yr old female. I sit at a desk all day but walk 3 miles a day for the past 2 years. I am not overweight. Both hips aches in the day AND The night. More so on my right side. I bought a new mattress, that didnt help. I get up and take breaks from my desk and also change positions..no help. I bought an ergonomic chair..no help. I have no leg or back, neck issues at all. This hurts every day, sometimes I get body aches when damp out. Pls note that I had active Lyme disease Fall 2009- April 2010 before diagnoses and antibiotics. July 2010 diagnosed with Epstein-Barr..mono. Fall 2010 I was told I have Chronic Fatigue Syndrome but I feel its all related to the Lyme and mono as I never had ANY of these isues before. I still get sever bouts of fatigue and chills and lose 4 days a month of my life over this. My hips started hurting while I had active Lyme and it never went away.Used to have pain in shoulder blades but after a year that is finally gone.Not sure if Hip pain is related or not but it aches daily and doesnt feel better with movement..stays the same. Thanks for any replies..
Also Check: What Happens When You Have Lyme Disease
Read Also: What Percentage Of Deer Ticks Carry Lyme Disease
Ongoing Symptoms Of Lyme Disease
A few people who are diagnosed and treated for Lyme disease continue to have symptoms, like tiredness, aches and loss of energy, that can last for years.
These symptoms are often compared to fibromyalgia and chronic fatigue syndrome.
It’s not clear why this happens to some people and not others. This means there’s also no agreed treatment.
Speak to a doctor if your symptoms come back, or do not improve, after treatment with antibiotics.
The doctor may be able to offer you further support if needed, such as:
- referral for a care needs assessment
- telling your employer, school or higher education institution that you require a gradual return to activities
- communicating with children and families’ social care
Page last reviewed: 05 July 2021 Next review due: 05 July 2024