Columbia Researchers Lead Placebo
NEW YORK Researchers at Columbia University Medical Center have added to the body of literature on Lyme disease with the publication of a study entitled, A Randomized, Placebo-Controlled Trial of Repeated IV Antibiotic Therapy for Lyme Encephalopathy, in the Oct. 10 online edition of Neurology.
The study, led by principal investigator Brian Fallon, M.D., M.P.H., director of the recently established Lyme and Tick-borne Disease Research Center at Columbia University Medical Center, involved screening 3,368 patients for potential inclusion. Strict selection criteria included memory impairment and a positive IgG Western blot for Lyme disease at study entry, as well as previous antibiotic treatment for Lyme disease completed at least 4 months before study entry. The research was funded by the National Institute of Neurological Disorders and Stroke .
Dr. Fallon and his research team identified patients with cognitive problems that developed after diagnosis with Lyme disease and that persisted or relapsed despite prior treatment. The goal was to determine whether patients who have already received the standard course of antibiotic treatment , would benefit from an additional 10 weeks of antibiotic therapy. They also set out to determine whether patients would relapse when taken off antibiotics or whether the alleviation of symptoms is sustained or enhanced with time.
– ### –
What Were The Major Findings
The majority of participants with PTLDS reported symptoms of cognitive difculty to some degree. Objective evidence of cognitive decline was identified in 26% of participants, with the most robust findings in verbal memory and processing speed. A subset also showed objective evidence of cognitive impairment compared to population-level performance. Despite subjective symptoms, 50% of the sample showed no statistically or clinically signicant objective decline in cognitive function using standardized neuropsychological measures. The remaining 24% of the sample were found to have sub-optimal engagement on testing measures, which may be due to the impact of fatigue, pain, prior negative clinical experiences, or other unknown factors.
Reports From The Literature
The literature search by using stringent diagnostic criteria disclosed only seven additional patients with dementia as a leading symptom of definitive LNB. These cases were reported in detail, so they can serve for the description of characteristic features. The data of all 10 patients are summarized in Table and .
You May Like: Old Lyme Cottages For Sale
What Helps Improve Cognitive Function For Lyme Patients
byJennifer Crystalon June 2, 2021
- Pharmaceutical treatment: Lyme is a bacterial infection, and you cant improve cognitive function without killing the bacteria thats causing it. Sometimes symptoms can get worse as bacteria die off faster than your body can eliminate them , but in my experience, the payoff is worth the temporary increase in discomfort and decrease in capabilities. Your doctor may want you to pulse antibiotics in order to give your body time to recover. There are particular antibiotics that work best to penetrate the blood-brain barrier and improve cognitive symptoms. Because every single case of tick-borne illness is unique, there is no set protocol, but your Lyme Literate Medical Doctor can tailor one to your needs.
- Supplements: Certain supplements can help reduce inflammation and neurotoxins. Glutathione and Essential Fatty Acids are two that are commonly used . Im wary of doctors who sell supplements themselves . Though supplements may seem good because theyre natural, they can have side effects and contraindications, so dont always assume that natural is better. For me, Ive needed a combination of both pharmaceutical treatment and supplements to improve all of my symptoms of Lyme disease, babesiosis, and ehrlichiosis.
Keeping It In Perspective
Its relatively uncommon for Lyme disease to cause brain effects. When Lyme disease does result in or problems with thinking and emotions, there are treatments that can help. Its also important to remember that only a very small portion of cognitive or psychiatric conditions are due to Lyme disease. In any case, talk with your doctor about identifying the cause of your problems and the treatment thats right for you.
Don’t Miss: What Does Lyme Disease Do To Your Body
Brain Inflammation And Lyme Disease
According to another study from Johns Hopkins, a PET scan of the brains of those with PTLDS as compared to other brains showed higher levels of inflammation. The scans searched for a protein in different sections of the brain associated with inflammation. That found it at significantly higher levels in eight regions of the brain.
While researchers expected to find some inflammation, they instead found it widespread throughout the brain. Brain inflammation can cause the symptoms patients say they experience, including brain fog and difficulty in remembering. The results suggest that drugs designed to curb neuroinflammation may be able to treat PTLDS, the Johns Hopkins researchers wrote.
Hyperbaric oxygen treatment also can reduce brain inflammation and may hold promise in treating those who suffer cognitive impairment after getting Lyme disease. Those who have had Lyme disease can also benefit from knowing which foods can reduce the risk of brain inflammation.
Why Was This Study Done
Patients with post-treatment Lyme disease syndrome commonly complain of cognitive symptoms, however prior studies assessing neuropsychological functioning in this population have varied. This study was done to systematically examine and measure cognitive functioning of patients with PTLDS, using standardized testing instruments.
Don’t Miss: Over The Counter Treatment For Lyme Disease
How Was This Study Done
213 participants with PTLD were tested and results compared with controls. Visual CS was measured using a PelliRobson chart with forced-choice procedures, in which participants had to identify two of the three letters in each triplet to proceed with testing. The total number of letters read was recorded for each eye. CS impairment was defined for age < 60 years as logCS of 1.80 and for those age 60 years as logCS of 1.65 . Visual acuity testing was done using the Early Treatment for Diabetic Retinopathy Study charts and protocols. Participants self-administered a questionnaire to assess presence of eye and vision symptoms and also underwent a neurologic exam and battery of neurocognitive tests
Does Lyme Disease Lead To Cognitive Impairment
- 3 minute read
One of the little-understood ramifications of Lyme disease is its impact on cognitive function. Many people who have the disease, including those in post-treatment, report lingering brain-related issues. Scientists in the last few years are trying to find objective results that support these subjective claims.
Research has shown that in some patients, Lyme disease leads to cognitive impairment, especially in verbal memory and processing speed. Another showed an increase in chemical markers that lead to brain inflammation, which has been associated with dementia and other neurodegenerative disorders.
Some also have found an association between Lyme disease and mental health, including increased risk of depression.
Also Check: Cutter Lyme Disease Tick Test
Detecting Borrelia Spirochetes: A Case Study With Validation Among Autopsy Specimens
- 1Division of Immunology, Tulane National Primate Research Center, Tulane University Health Sciences, Covington, LA, United States
- 2Department of Psychiatry, Columbia University, New York, NY, United States
- 3Division of Molecular Imaging and Neuropathology, New York State Psychiatric Institute, New York, NY, United States
- 4Macedonian Academy of Sciences and Arts, Skopje, Macedonia
- 5Department of Pathology and Cell Biology, Columbia University, New York, NY, United States
Losing The Ability To Retain Information
| Nothing sunk in and it became very frustrating. I find my self looking at my notebook and clearly reading what I had written but not being able to make sense of the words because I didn’t retain what was taught earlier. In order to somewhat retain the information I had to read a sentence almost ten times to accomplish what a normal person could retain with a couple glances. I could look up a word, look at the meaning and understand it but when I’d close the dictionary, I was right back where I was before I even opened the dictionary. Clueless. |
Also Check: What Do I Do If My Dog Has Lyme Disease
Lyme Disease May Be Linked To Mental Disorders
People with the tick-borne infectious disease Lyme borreliosis, or Lyme disease, showed higher rates of a variety of mental disorders and higher rates of suicide attempts compared with those without the disease, according to authors of a population-based retrospective cohort study published in the American Journal of Psychiatry.
Small studies have shown associations between Lyme disease and depression, suicidal thoughts, obsessive-compulsive disorder, mania, and cognitive impairment. These mental disorders have been reported in people with acute cases of Lyme disease, as well those who have undergone antibiotic treatment for the disease.
In the current study, investigators used Denmarks National Patient Register and the Psychiatric Central Research Register to compare the rate of new-onset mental disorders among people diagnosed with Lyme disease against the rate reported in people without Lyme disease. The study included all persons living in Denmark from 1994 through 2016 nearly 7 million individuals aged 3 to 104 years. A total of 12,616 people in the study population had received a hospital-based diagnosis of Lyme disease.
The results of this study may not be generalizable to people with less severe cases of Lyme disease as the study only included hospital-based diagnoses. The same limitation applies to the various psychological conditions reported.
Reference
Rnascope Is A Sensitive Technique For Finding Viable Pathogen But Requires Freshly Prepared Tissue
Figure 8. Validation of RNA integrity on Fresh frozen NHP frontal cortex brain tissue using RNAscope assay. NHP tissue was stained with a 3-plex positive control probe POLR2A targeting DNA-directed RNA polymerase II RPB1, PPIB targeting cyclophilin B, and UBC that targets Ubiquitin C. In terms of relative expression levels, UBC is highest, PPIB is considered a moderate-high, POLR2A is moderate-to low expressor target. Successful staining has 49 dots per cell of PPIB/POLR2A and UBC of 1015 dots per cell. PPIB is considered a standard to determine the RNA quality of brain samples. Represents red fluorescence, indicating the specificity of PPIB, whereas, displays a far-red puncta targeting UBC gene. Absence of POLR2A signal in represents, quality of RNA being partially compromised. A merge image of all the channels can be seen in . White arrows were pointing toward the fluorescence puncta and orange arrows toward autofluorescence of the tissue.
The Patient Harbored Borrelia in the Amygdala and Spinal Cord
Tissue slices adjacent to the autopsy tissue specimens that were positive for DNA were stained for the presence of persisters. For this, slides were stained with the primary rabbit polyclonal antiB. burgdorferi antibody and a goat anti-rabbit IgG-Alexa Fluor 488 secondary antibody. An intact Borrelia spirochete with the expected morphology was identified within fixed tissue of the spinal cord . The spirochete appeared to be adjacent to vasculature.
Don’t Miss: Can Bed Bugs Cause Lyme Disease
The Experience Of Lyme Disease
In our book, Conquering Lyme Disease: Science Bridges the Great Divide, we review several of the key features of Lyme disease that can make the experience of this illness so challenging, including:
- The politically charged climate
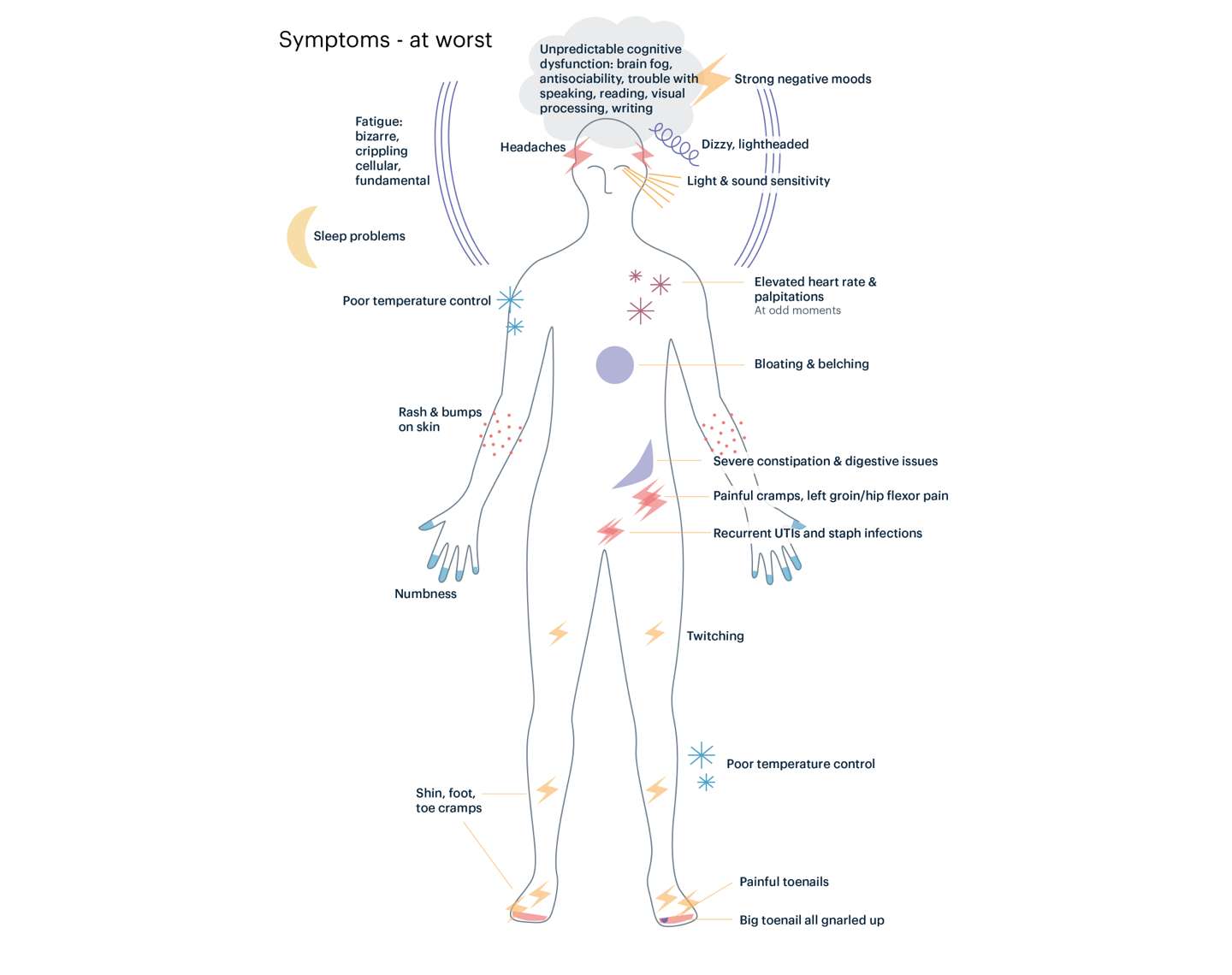
- The protean nature of manifestations of the illness
- The waxing and waning course of symptoms
- The psychological ramifications of having an “invisible” chronic illness and the experience of invalidation
- The challenge of having a disease that affects the brain and sensory system
- The impact of uncertainty surrounding diagnosis, treatment, and prognosis
Lyme Disease And Cognitive Impairment
For decades, those who have had Lyme disease frequently complain of cognitive impairment, even after treatment with antibiotics is concluded. How frequently? A study led by researchers from Johns Hopkins University School of Medicine reported that 92 percent of Lyme disease patients in the study reported experiencing cognitive issues.
All 124 patients had experienced either physical or mental post-treatment Lyme disease syndrome . Evidence from 26 percent of the patients showed significant cognitive decline in the areas of memory and cognitive processing speed.
The gap between the number of people reporting brain fog and the number of issues subjectively proven in tests led some researchers to think perhaps the issue was psychosomatic and related to depression or anxiety. Certainly, depression is an issue with Lyme disease, with as high as 45 percent of patients reporting feelings of depression in some studies, according to the Global Mental Health Program at Columbia University.
But new research shows that something else may be involved: brain inflammation.
You May Like: Does Lyme Disease Cause Headaches
Lyme Disease Neurocognitive & Neuropsychiatric Symptoms Dr Capanna
Neurocognitive and neuropsychiatric symptoms associated with tick-borne disease.
Gabriella: Dr. Roseann, thank you for joining ASPIRE to talk about neurocognitive and neuropsychiatric symptoms associated with tick-borne disease.
Many of our families are dealing with PANS, Lyme, and other tick-borne infections whether or not a tick-borne infection triggered the first PANS symptoms. Some patients initial PANS symptoms were triggered by infections like strep, upper respiratory infections, flu, etc. and are also dealing with tick-borne infections while some patients symptoms were triggered by tick-borne infections. So no matter which infection triggered initial symptoms or subsequent flares, many patients treating multiple infections at once. Lyme Symptoms
Dr. Roseann: Absolutely. Many patients have both PANS and tick-borne illness diagnosis. It is very taxing on the body to fight so many infections at once, which can make it more difficult to heal. I rarely see someone with just one infection. Once one infection takes hold, and the immune system weakens, then others creep in, which of course, further weakens the immune system. See more about Treatment.
Three Complementary Modes of PANS/PANDAS Intervention
- Remove source of inflammation
- Treat dysregulated immune system and lower inflammation
- Treat the symptoms.
Gabriella: What are the neurological symptoms of tick-borne diseases and which ones overlap with PANS Symptoms?
Dr. Roseann:
For more on Lyme Symptoms:
Can Lyme Disease Cause Cognitive Dysfunction Or Dementia
The question of whether Lyme disease could cause dementia was addressed by Wormser and colleagues in an article entitled Lack of Convincing Evidence That Borrelia burgdorferi Infection Causes Either Alzheimer Disease or Lewy Body Dementia, published in the journal Clinical Infectious Diseases.¹
The authors reviewed a paper by Gadila et al.² which concluded that a Lyme disease infection might cause Lewy body dementia. The case described a 69-year-old woman who died 15 years after her initial infection with Lyme disease with a clinical diagnosis of Lewy body dementia.
The woman had initially presented with an erythema migrans rash, headache, joint pain, and fever. Her symptoms resolved with 10 days of doxycycline.
Over time, she developed a sleep behavior disorder, cognitive problems , photophobia, paresthesias, fasciculations, and myoclonic jerks. She initially improved with IV followed by oral antibiotics. But her condition later worsened.
The extensive workup at that time led to the diagnoses of both a REM behavioral disorder with verbalizations and movements and a neurodegenerative dementia characterized by expressive aphasia, visual agnosia, anomia, deficits in executive function and calculation, and mild memory problems.
She passed away 15 years after the onset of her illness.²
An autopsy revealed the presence of Borrelia burgdorferi in the brain and spinal cord tissue of the patient.
Can Lyme disease cause dementia?
Inside Lyme Podcast Series
References:
Also Check: Lyme Disease Essential Oil Bomb
Controlled Study Of Cognitive Deficits
Although neurologic Lyme disease is known to cause cognitive dysfunction in adults, little is known about its long-term sequelae in children.
A Controlled Study of Cognitive Decits in Children With Chronic Lyme Disease* Felice A. Tager, Ph.D., Brian A. Fallon, M.D., John Keilp, Ph.D., Marian Rissenberg, Ph.D., Charles Ray Jones, M.D., Michael R. Liebowitz, M.D
Received August 7, 2000 revised January 3, 2001 accepted January 10, 2001. From the Columbia University Department of Psychiatry, Division of Behavioral Medicine, New York, New York. Address cor- respondence to Dr. Tager, Columbia Presbyterian Medical Center, 622 West 168th Street, Box 427, New York, NY 10032. E-mail:
Copyright 2001 American Psychiatric Publishing, Inc.
J Neuropsychiatry Clin Neurosci 13:4, Fall 2001
* LDA has received permission to post this article in its entirety
to view the entire pdf of this article
ABSTRACT
Lyme disease is a multisystemic illness caused by the tick-borne spirochete Borrelia burgdorferi . LYD, the most common tick-borne illness in the United States, may manifest in a variety of ways: dermatologic, arthritic, ophthalmologic, cardiac, and neuropsychiat- ric. The incidence and spread of the disease increased during the 1980s, stabilizing somewhat in the late 1990s. Children below the age of 9 are at a high risk for Bb infection, with many new cases of Lyme occurring among persons younger than 14 years.
METHODS
Cognitive Evaluation
What Are The Signs And Symptoms Of Stage 3 Lyme Disease
Late or chronic Lyme disease refers to manifestations that occur months to years after the initial infection, sometimes after a period of latency. Signs and symptoms of chronic Lyme disease are primarily rheumatologic and neurologic. Acrodermatitis chronica atrophicans, the cutaneous feature of late-stage Lyme disease, is found almost exclusively in European patients.
Most patients presenting with late disease do not have a history of erythema migrans, because the rash typically leads to earlier treatment, which prevents the development of late disease. However, other manifestations of the disease may coexist or may have occurred in the past. Thus, a history of Bell palsy, aseptic meningitis, arthritis, acral paresthesias or dysesthesias , or cognitive dysfunction may be diagnostically useful.
Maladaptive host responses can lead to a variety of syndromes in stage 3, as follows :
- Postinfectious Lyme arthritis Massive inflammatory synovial proliferation, usually in a knee
- Posttreatment Lyme disease syndrome Pain, neurocognitive impairment, fatigue
- Autoimmune joint disease Rheumatoid arthritis, psoriatic arthritis, or peripheral spondyloarthropathy
- Autoimmune neurologic disease Chronic idiopathic demyelinating polyneuropathy
Lyme arthritis is the hallmark of stage 3 Lyme disease. It tends to involve large joints . Arthritis must be differentiated from arthralgia, which is common in early disease.
References
Don’t Miss: How You Get Lyme Disease
Lyme Disease Memory Loss Treatment
by lyme2440 | Sep 10, 2018 | Articles
Lyme Disease, caused by the bite of a bacteria-infected tick with Borrelia burgdorferi, mayonii, afzelii or garinii , not only attacks the patients organs and joints, but causes significant changes in their neurological state, sometimes called Lyme brain.
This serious and debilitating illness affects an estimated 365,000 individuals each year and numbers are rising.
For those who suffer from the cognitive impairments of Lyme, such as short-term memory loss, difficulty with speech and word recollection, loss of motor skills, depression, anxiety, hallucinations and other symptoms that may closely resemble Alzheimers disease or schizophrenia, finding a way to fight back is an absolute must.
Fortunately, the cognitive impairments often associated with Lyme Disease are well documented, and there are doctors, specialists and treatment centers who focus primarily on this kind of therapy.
Strategies can include everything from brain-training activities, such as biofeedback, to more internal treatments such as administering antibiotics intravenously to help correct memory recall issues by reducing inflammation of the brain if the infection is caught early on.
Treatment may take the form of a pharmaceutical approach, tackling the blood-brain barrier that causes symptoms of Lyme brain, aiming to penetrate this barrier, reduce inflammation, and stabilizing neurological function.
Choosing the Right Approach
Recent Posts
Categories