How To Diagnose Neuropathy
For most people, a diagnosis of neuropathy may be based upon a persons medical history, physical exam, lab work, and neurologic evaluation. The following tests can be useful to identify the condition, as well as rule out potential causes and contributing factors.
- Neurologic Exam: During a neurologic exam, your doctorusually a neurologistassesses reflexes ability to feel sensations like hot, cold, and pain coordination balance muscle strength and muscle tone.
- Blood Tests: Blood tests are run to assess nutritional deficiencies, organ function, toxins, and the presence of an atypical immune response.
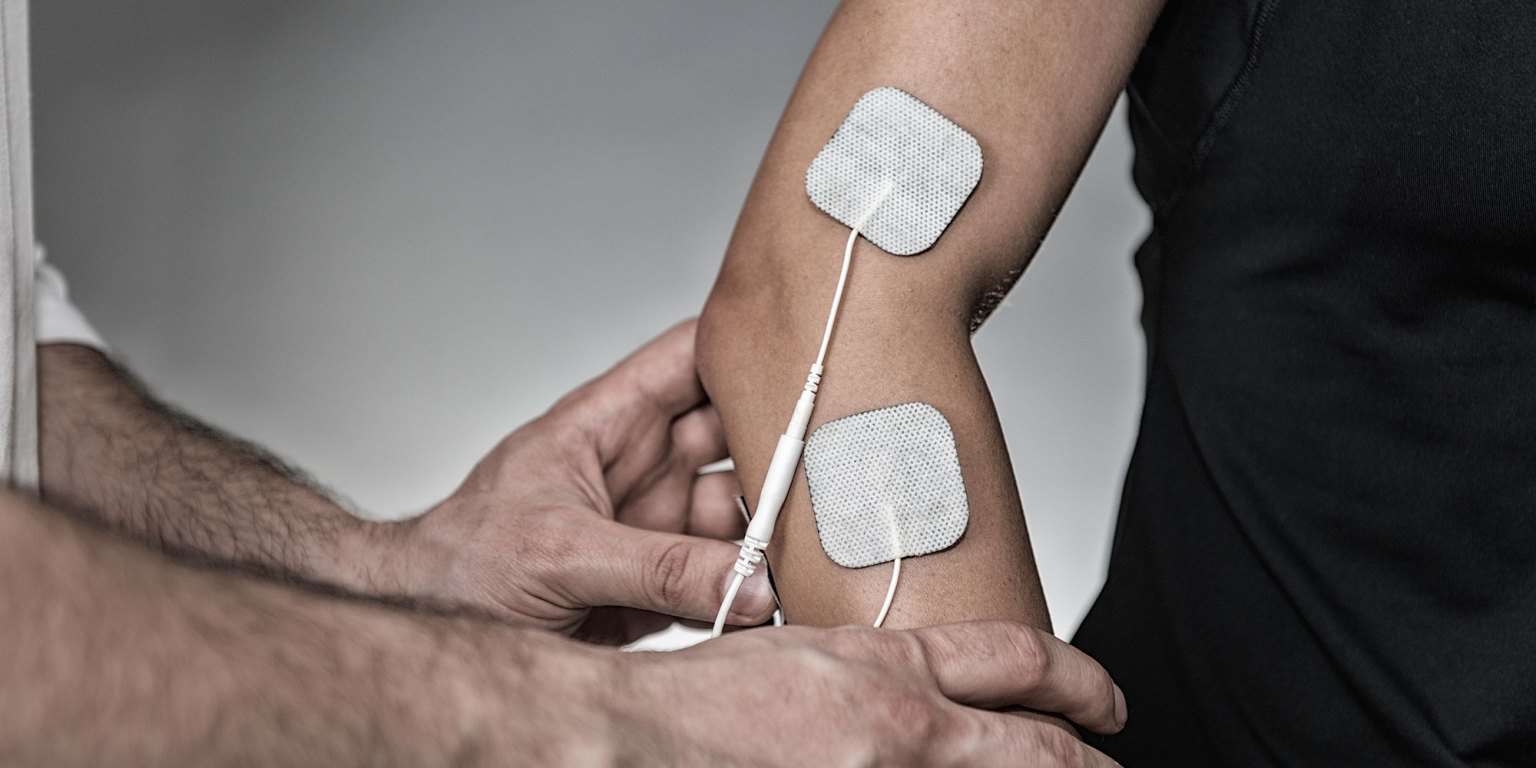
- Electrodiagnostic Tests : EDX testing checks how well the muscles and nerves are functioning by measuring their electrical activity, which assists in determining the extent of nerve damage. Two commonly used procedures are electromyography and nerve conduction velocity . During an EMG, small needle electrodes are inserted through the skin into the muscle to measure the electrical activity while the muscle is at rest, during a mild contraction, and during a powerful contraction. Frequently, the NVC will be completed at the same time as the EMG, which helps further assess the amount and speed with which an electrical impulse moves through a nerve.
- Other Tests: The need for other testing will depend on the severity of your symptoms and could include specialized sensory testing, genetic testing, or a biopsy with tissue samples from a nerve, muscle, or skin.
Diagnosing Neurological Lyme Disease
The first step in the diagnosis of Lyme disease and associated infections is to order blood tests through a Lyme specific laboratory. It is well-established the traditional two-tiered test has low sensitivity for diagnosing Lyme disease.
The diagnosis of acute central nervous system involvement of Lyme disease requires a lumbar puncture to analyze cerebral spinal fluid . The analysis of the CSF should include IgM and IgG antibodies to Borrelia bacteria and a test looking for the bacteria DNA . If either of these markers is elevated, it is diagnostic of Lyme neuroborreliosis.
An increased level of white blood cells in the CSF known as pleocytosis also aids in the diagnosis. However, some people with neuroborreliosis do not have elevated antibodies in the CSF, and since pleocytosis can be present in other central nervous system infections, Lyme disease may not be considered.
The chemical attractant something known to call the immune system to fight an infection CXCL13 in the CSF has become an important marker to help diagnose Lyme neuroborreliosis. In a 2018 study of Lyme neuroborreliosis patients with elevated white blood cells but no detectable Lyme antibodies in their CSF, 73% had raised levels of CXCL13. The authors of the study have proposed a CXCL13 result greater than 160 pg/mL is consistent with Lyme neuroborreliosis.
Visualization Of Ccl2 Il
The DRG tissue explants stimulated ex vivo with spirochetes in the presence of brefeldin A showed localization of CCL-2 in sensory neurons . CCL-2, which is stained green in this tissue, is localized inside the neurons giving a yellow signal due to the co-localization of red and green within the neurons. CCL-2 is also seen in areas occupied by satellite glial cells and dorsal root in the DRG. CCL-2 in green is seen co-localizing with the satellite glial cell marker GFAP . Both satellite glial cells and sensory neurons in the DRG that are known to stain positive for S-100 , seen in red, show the presence of CCL-2 . CCL-2 is also seen to co-localize with Schwann cells in the dorsal root, staining positive with p75NTR, seen in red , while remaining unstained nerve tissue is seen as gray. The spirochetes appear blue in Figure A-D.
Figure 1
Don’t Miss: How Long For Lyme Disease Test Results
How Is It Treated
Facial palsy is treated with oral antibiotics and Lyme meningitis/radiculoneuritis can either be treated with oral or intravenous antibiotics, depending on severity . Most people with Lyme disease respond well to antibiotics and fully recover. Varying degrees of permanent nervous system damage may develop in people who do not receive treatment in the early stages of illness and who develop late-stage Lyme disease.
How Does Lyme Affect The Nervous System
Borrelia, the spirochete that causes Lyme disease, can invade the nervous system, creating a condition called Lyme neuroborreliosis.
In the central nervous system, the infection can cause meningitis , and damage various nerves in the brain or brainstem. In the peripheral nervous system, the infection can result in pain that radiates along sensory nerves.
The exact reasons why some patients get better with treatment and other patients remain ill is unclear. The potential mechanisms may include permanent damage from infection, neuroinflammation, autoimmune reactions, or persistent infection.
As Professor Holly Ahern explains, the main problem with research into so-called PTLDS is the absence of an accurate blood test or biomarker. Researchers have no way to determine if persisting infection is the cause of the continuing symptoms.
Dr. Novak and his team set out to find objective measures. We know these patients are suffering. The next question is how do we treat them? says Novak.
The most valuable studies are those that give us a biomarker, something we can measure, so that when we treat them, we can look objectively to see if they get better or not.
Also Check: Rheumatologist Specializing In Lyme Disease
Can You Reverse Nerve Damage Caused By Lyme Disease
Only one tick bite can cause a debilitating disorder named Lyme disease.
Lyme affects the entire body and causes problems with your immune system and brain function. What is even more concerning is that the bacteria can lay dormant and still affect a patient long after being treated. This is the main reason why Lyme disease causes nerve damage.
Which Neurologic Findings Suggest Lyme Disease
Approximately 5-10% of untreated patients with Lyme disease have signs of cranial neuropathies, and up to 60% of patients with early neuroborreliosis develop cranial neuritis. Seventh nerve palsy is by far the most common. Bilateral facial palsy can be seen in 35% of patients and is a unique characteristic that is useful for distinguishing it from idiopathic Bell palsy and other disorders.
Typical associated findings depend on the nerve affected and can include visual or auditory disturbances, facial paresthesia, and/or vertigo. Other neurologic manifestations include diffuse or focal mononeuropathy multiplex , plexopathy, and/or radiculoneuropathy . Less common presentations include myositis, pseudotumor cerebri, and cerebellitis.
Lyme meningitis is relatively common, occurring in as many as 15% of untreated patients bitten by the Ixodes tick and in 30% of Lyme disease cases, and does not manifest as the usual signs of bacterial meningitis . Meningitis may be accompanied by cranial or peripheral radiculoneuropathy. Neck stiffness can occur early, with or without frank meningitis.
Chronic radicular paresthesias are usually not associated with motor or sensory deficits. The physical examination results are normal.
References
Feder HM Jr. Lyme disease in children. Infect Dis Clin North Am. 2008 Jun. 22:315-26, vii. .
Edlow JA. Bull’s Eye – Unraveling the Medical Mystery of Lyme Disease. 2nd ed. New Haven: Yale University Press 2004.
Read Also: Antibiotics Used For Lyme Disease
What You Can Do
When you make the appointment, ask if there’s anything you need to do in advance, such as fasting for a specific test. Make a list of:
- Your symptoms, including any that may seem unrelated to your reason for scheduling the appointment
- Key personal information, including recent stresses or major life changes, family medical history and alcohol use
- All medications, vitamins or other supplements you take, including doses
- Questions to ask your doctor
Take a family member or friend along, if possible, to help you remember the information you’re given.
For peripheral neuropathy, basic questions to ask your doctor include:
- What’s the most likely cause of my symptoms?
- Are there other possible causes?
- What tests do I need?
- Is this condition temporary or long lasting?
- What treatments are available, and which do you recommend?
- What side effects can I expect from treatment?
- Are there alternatives to the primary approach you’re suggesting?
- I have other health conditions. How can I best manage them together?
- Do I need to restrict activities?
- Are there brochures or other printed material I can take? What websites do you recommend?
Don’t hesitate to ask other questions.
Lyme Disease Treatment & Therapy
- Antibiotics
For Bells palsy
- Eye drops for affected eye
- Medications such as steroids to reduce inflammation of nerve and decrease pain
- Surgery
- Treatment of underlying inflammatory condition, if present
If experiencing weakness, pain, or inflammation
- Ask your doctor about special therapeutic shoes or a knee brace
- Take safety measures to compensate for loss of sensation
- Lyme disease is curable, if treated early
Read Also: Can Lyme Disease Cause Leg Pain
Incubation Of Dorsal Root Ganglia Explant Slices With Live Spirochetes
DRG tissue was obtained immediately after euthanasia from three normal rhesus macaques and placed in PBS pH 7.2 at room temperature. The tissue was sliced using sterile number 21 scalpels . The slices were placed in separate wells of 12-well plates , each containing 2 ml of RPMI 1640 medium supplemented with 10% fetal bovine serum . Live B. burgdorferi spirochetes at a final density of 1 × 107/mL were added to some wells. Some wells received, in addition, brefeldin A , a fungal metabolite that blocks protein transport at a final concentration of 10 g/mL. Corresponding control slices were also held in medium plus brefeldin A without spirochetes. The DRG slices were then incubated at 37°C for four hours in a humidified 5%-CO2 incubator. At the end of the four-hour incubation, tissue slices were fixed in 2% paraformaldehyde in PBS pH 7.0 and cryopreserved as described earlier .
Femoral Neuropathy And Lyme Disease
It is well-recognized that Lyme disease can cause neurologic symptoms, such as peripheral neuropathy when the infection goes untreated. Patients can experience muscle weakness and/or twitching, loss of sensation in parts of the body, numbness, tingling sensations, problems with balance and bladder control, and a feeling of dizziness or faintness. But now, new research indicates that femoral neuropathy may also be due to Lyme disease.
A case report by Lazaro and Butt, published in the International Medical Case Reports Journal, describes a 67-year-old patient with Lyme disease and femoral neuropathy.¹ This is believed to be the first reported case of isolated femoral neuropathy triggered by Lyme disease.
The patient, who lived in central New York, a region endemic for Lyme disease, developed a large erythema migrans rash on his chest, which lasted for 3 weeks, along with swelling of his left knee.
An IgG Western blot test was positive, and he was treated with a 4-week course of doxycycline.
However, Shortly after the completion of the doxycycline therapy, this patient began complaining of gait difficulties and frequent falls, as well as intermittent painful cramps in his right thigh, writes Lazaro.
An electromyography test, which measures muscle response or electrical activity when a nerve muscle is stimulated, indicated the patient had a femoral neuropathy.
Related Articles:
Read Also: How Does A Person Get Lyme Disease
Lyme Neuroborreliosis: Preliminary Results From An Urban Referral Center Employing Strict Cdc Criteria For Case Selection
David S. Younger
1Lyme Neuroborreliosis Research Program, NYU School of Medicine, 333 East 34th Street, Suite 1J, NY 10016, USA
2Department of Medicine, Lenox Hill Hospital, New York, NY 10021, USA
Academic Editor:
Abstract
Lyme neuroborreliosis or neurological Lyme disease was evidenced in 2 of 23 patients submitted to strict criteria for case selection of the Centers for Disease Control and Prevention employing a two-tier test to detect antibodies to Borrelia burgdorferi at a single institution. One patient had symptomatic polyradiculoneuritis, dysautonomia, and serological evidence of early infection and another had symptomatic small fiber sensory neuropathy, distal polyneuropathy, dysautonomia, and serological evidence of late infection. In the remaining patients symptoms initially ascribed to Lyme disease were probably unrelated to B. burgdorferi infection. Our findings suggest early susceptibility and protracted involvement of the nervous system most likely due to the immunological effects of B. burgdorferi infection, although the exact mechanisms remain uncertain.
1. Introduction
2. Methods
Noncontrast magnetic resonance imaging and nuclear medicine cerebral perfusion imaging with single-photon emission spectroscopy screened for brain dysfunction, the main symptoms of which were typically neurocognitive.
3. Patient Descriptions
3.1. Patient 1
3.2. Patient 2
4. Discussion
References
Copyright
More related articles
Lyme And Neuropathy: How To Ease Nerve Pain Tingling And Weakness
Lyme disease can affect several systems of the body the brain, nervous system, joints, heart, and more.
The list of symptoms infected individuals can experience is expansive and varies from person to person.
Its one of the reasons a Lyme disease diagnosis may be controversial.
Yet, one thing everyone seems to agree on about the tick-borne disease is that it can significantly impact the nervous system, especially without prompt treatment in the early stages of the infection.
Unfortunately, Lyme often goes missed early on. The telltale sign of a Lyme infection an erythema migrans rash, or the classic bulls-eye rash doesnt occur in every case. .
And the initial symptoms of infection may be nothing more than fever, chills, headache, fatigue, or muscle aches, making them easy to miss or brush off as a case of the flu.
But as the disease advances, the bacteria associated with Lyme, Borrelia burgdorferi, spreads via the bloodstream to other parts of the body, a process known as dissemination. This occurs in the days and weeks following infection, referred to as early disseminated Lyme disease.
If an infection goes untreated for months to years, however, theres a good chance the infection will proceed to late stage or late disseminated Lyme disease, sometimes called chronic Lyme disease. Thats when the nervous system can become involved, and symptoms ratchet up to a whole new level.
Read Also: Treating Dogs For Lyme Disease
Lifestyle And Home Remedies
To help you manage peripheral neuropathy:
- Take care of your feet, especially if you have diabetes. Check daily for blisters, cuts or calluses. Wear soft, loose cotton socks and padded shoes. You can use a semicircular hoop, which is available in medical supply stores, to keep bedcovers off hot or sensitive feet.
- Exercise. Regular exercise, such as walking three times a week, can reduce neuropathy pain, improve muscle strength and help control blood sugar levels. Gentle routines such as yoga and tai chi might also help.
- Quit smoking. Cigarette smoking can affect circulation, increasing the risk of foot problems and other neuropathy complications.
- Eat healthy meals. Good nutrition is especially important to ensure that you get essential vitamins and minerals. Include fruits, vegetables, whole grains and lean protein in your diet.
- Avoid excessive alcohol. Alcohol can worsen peripheral neuropathy.
- Monitor your blood glucose levels. If you have diabetes, this will help keep your blood glucose under control and might help improve your neuropathy.
Make Healthy Lifestyle Choices
These habits support your nerve health:
- Eat a diet rich in fruits, vegetables, whole grains and lean protein to keep nerves healthy. Protect against vitamin B-12 deficiency by eating meats, fish, eggs, low-fat dairy foods and fortified cereals. If you’re vegetarian or vegan, fortified cereals are a good source of vitamin B-12, but talk to your doctor about B-12 supplements.
- Exercise regularly. With your doctor’s OK, try to get at least 30 minutes to one hour of exercise at least three times a week.
- Avoid factors that may cause nerve damage, including repetitive motions, cramped positions that put pressure on nerves, exposure to toxic chemicals, smoking and overindulging in alcohol.
Don’t Miss: Kozlowski Orthodontics East Lyme Ct
Peripheral Neuropathy In Lyme Disease Patients
Reported cases of Lyme disease have been rising steadily over the past 30 years, but its diagnosis can be challenging. Left untreated, patients with Lyme disease can go on to develop neurological symptoms, including those that are characteristic of peripheral neuropathy.
Francis Bean, DPM, has been experiencing neurological symptoms in his lower extremities for more than six months. When they arise, he feels a tingling in his hallux, his heels go numb, and he develops a hypersensitivity to temperature and touch that leads to a painful burning sensation. On paper, these sound like common symptoms of diabetic peripheral neuropathya condition with which Bean, as a podiatrist, is quite familiar.
But Bean doesnt have diabetes. His peripheral neuropathy developed as a result of Lyme disease, and in the US, hes one of a growing number of people with similar complications.
Lyme borreliosis, or Lyme disease, is a multisystem infectious disease caused in the US by the spirochete Borrelia burgdorferi , which is transmitted almost exclusively through tick bites.1,2 Though cases are concentrated primarily in limited geographic areas where the tick is endemic, Lyme disease is the most commonly reported vector-borne infection in the country, and reported cases of its occurrence have been rising steadily over the past 30 years.3,4
What To Expect From Your Doctor
Your doctor is likely to ask you questions, such as:
- Do you have health conditions, such as diabetes or kidney disease?
- When did your symptoms begin?
- Have your symptoms been continuous or occasional?
- How severe are your symptoms?
- Does anything seem to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
- Does anyone in your family have symptoms similar to yours?
© 1998-2022 Mayo Foundation for Medical Education and Research . All rights reserved.Terms of Use
Recommended Reading: How To Test For Late Stage Lyme Disease
Evaluation Of The Role Of Inflammation In Mediating Neuronal Apoptosis In Dorsal Root Ganglia Cultures Using The Anti
DRG cell cultures were seeded as described above in chamber slides for evaluation of apoptosis or for evaluation of immune mediators and maintained in growth medium for six days. Prior to stimulation with live B. burgdorferi, DRG cultures were incubated with various concentrations of dexamethasone , 5 M, 15 M and 150 M for 24 hours at 37°C, after which they were washed and then incubated in fresh growth medium containing the respective concentrations of dexamethasone and live B. burgdorferi at a MOI of 10:1 at 37°C for 24 hours and devoid of P/S. Similar concentrations of dexamethasone as those mentioned above have been reported to inhibit the production of CCL2 in mice microglia . The dexamethasone that we used in our experiments is supplied as a water-soluble formulation consisting of dexamethasone and a carrier substance –cyclodextrin . The effect of HPC alone, at respective molar concentrations found in the concentrations of dexamethasone that we used in our experiments, was done by incubating DRG cultures as described above in the presence and absence of B. burgdorferi and the above mentioned concentrations of carrier alone at 15 M, 45 M and 450 M, respectively.