Diagnosing Neurological Lyme Disease
The first step in the diagnosis of Lyme disease and associated infections is to order blood tests through a Lyme specific laboratory. It is well-established the traditional two-tiered test has low sensitivity for diagnosing Lyme disease.
The diagnosis of acute central nervous system involvement of Lyme disease requires a lumbar puncture to analyze cerebral spinal fluid . The analysis of the CSF should include IgM and IgG antibodies to Borrelia bacteria and a test looking for the bacteria DNA . If either of these markers is elevated, it is diagnostic of Lyme neuroborreliosis.
An increased level of white blood cells in the CSF known as pleocytosis also aids in the diagnosis. However, some people with neuroborreliosis do not have elevated antibodies in the CSF, and since pleocytosis can be present in other central nervous system infections, Lyme disease may not be considered.
The chemical attractant something known to call the immune system to fight an infection CXCL13 in the CSF has become an important marker to help diagnose Lyme neuroborreliosis. In a 2018 study of Lyme neuroborreliosis patients with elevated white blood cells but no detectable Lyme antibodies in their CSF, 73% had raised levels of CXCL13. The authors of the study have proposed a CXCL13 result greater than 160 pg/mL is consistent with Lyme neuroborreliosis.
The Pain Changes And Moves Around The Body
Another classic trait of Lyme disease is the migratory nature of the pain. The muscle and joint pain, as well as the tingling, numbness and burning sensations often tend to come and go and move around the body. For example, one day the joint pain might be in the knees and a few days later it may be affecting another nerve. Especially when untreated, research says Lyme disease can spread to the joints, heart, and nervous system.
What Complications Can Lyme Disease Cause
Neurological complications can begin to develop in early disseminated Lyme disease. These complications may include:
- Vision disturbances
- Sleep and memory disorders
- Nerve damage in the legs and arms
Other non-neurological complications can also develop, such as severe arthritis, persistent fatigue, mood disturbances, and life-threatening disorders of the heart, lungs, and nervous system.
Also Check: Rheumatologist Specializing In Lyme Disease
Regression And Other Symptoms In Children
Children are the largest population of Lyme patients.
The CDC study of reported Lyme cases from 19922006 found that the incidence of new cases was highest among 5- to 14-year-olds . About one quarter of reported Lyme cases in the United States involve children under 14 years old .
Children can have all the signs and symptoms of Lyme that adults have, but they may have trouble telling you exactly what they feel or where it hurts.
You may notice a decline in school performance, or your childs mood swings may become problematic.
Your childs social and speech skills or motor coordination may regress. Or your child may lose their appetite.
Children are more likely than adults to have arthritis as an initial symptom 01267-2/fulltext#sec0040″ rel=”nofollow”> 25).
In a 2012 Nova Scotian study of children with Lyme, 65 percent developed Lyme arthritis . The knee was the most commonly affected joint.
Summary:
Neck Pain From Lyme Disease
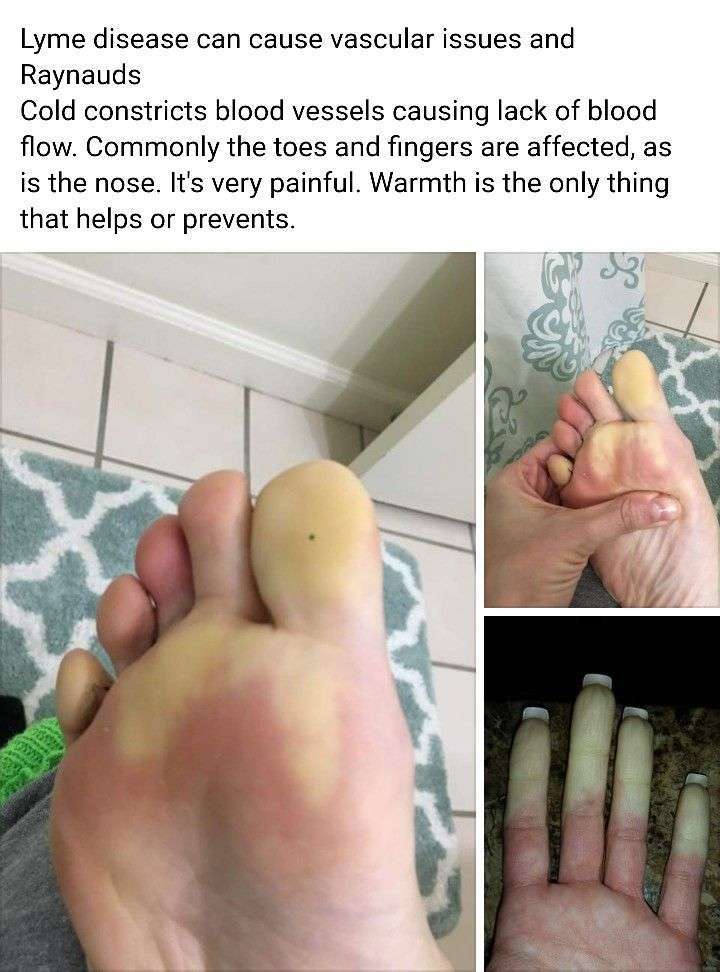
Lyme disease is commonly associated with tick bites and a big circular rash. However, a tick bite does not hurt and many people do not recall being bit or seeing the rash. Further complicating matters, Lyme disease symptoms may start out minor and not become problematic for months or longer.
Lyme disease causes neck pain in more than 30% of cases. Watch:Neck Pain Causes Video
Media reports rarely focus on neck pain with Lyme disease, but some estimates note that it occurs in more than 30% of the cases and is typically one of the earlier symptoms.1 Recognizing Lyme disease early and seeking treatment can make a big difference in the outcome.
Read Also: Can Any Tick Carry Lyme Disease
Lyme Disease: Numbness In Feet
Lyme disease can cause numbness and tingling in the feet and limbs as a result of peripheral neuropathy, a neurological disorder which can result from untreated Lyme disease.
Numbness and tingling in the feet can also be a symptom of many other conditions or injuries. Its important to discuss any discomfort in your feet with an experienced podiatrist to get an accurate diagnosis. Back to top
Can Lyme Disease Be Prevented
Not all cases of Lyme disease can be prevented. But you can help protect your family from tick bites. If you go into an area where ticks live, be sure to:
- Stay in the middle of the trail, instead of going through high grass or the woods.
- Wear closed shoes or boots, long-sleeved shirts, and long pants. Tuck pant legs into shoes or boots to prevent ticks from crawling up legs.
- Use an insect repellent.
- Consider treating clothing and gear with permethrin to repel ticks. When used properly, permethrin is safe for all ages. But don’t use it on clothing or other material a child may suck on or chew.
- Wear light-colored clothing to help you see ticks more easily.
- Shower and wash hair after being outside to remove ticks before they attach.
You May Like: How To Cure Lyme Disease Naturally
Ways To Identify Lyme Disease In Time And Take The Proper Treatment:
1) If you live in a wooded area or plan to go camping or spend anytime outdoors where ticks are often present, come prepared with tick sprays and wear clothing that covers your body to reduce the chances of being bit.
2) Often times a tick bite can go unnoticed like it did in my case, so make sure that during and post trip, that you look at your body to see if there have been any tick bites. If you notice them, seek a doctor immediately to test yourself and start treatment if necessary. The earlier you spot this, the better.
3) Sometimes, you may find that a tick may actually be on you when you spot the bite, in which case you should also get rid of it and see if a bite mark is left. Whether or not it is, still seek a doctor and repeat the same things.
Risk Factors For Acquiring Lyme Disease
Where you vacation or live, as well as what outdoor activities you participate in, affects your likelihood of being exposed to Lyme disease. Common factors that put you at risk of contracting Lyme disease include:
- Spending time in grassy or wooded areas. Deer ticks are very prevalent in the Central PA area due to its heavily wooded countryside. Deer ticks thrive in these types of places. Children here are particularly at risk as well as adults who work outdoors.
- Having exposed skin. Ticks find it easy to attach themselves to exposed skin, so if youre in an area thats known for ticks, always wear long sleeves and long pants and never allow your pets to run through long grasses.
- Removing ticks incorrectly or not quickly enough. As you already know, bacteria from a tick bite has the potential to enter your bloodstream if the tick has been attached to you for between 36 to 48 hours or longer. If you spot and correctly remove the tick within 48 hours, your risk of acquiring Lyme disease is low, so always check your skin after being outdoors.
The Centers for Disease Control and Prevention notes that older adults and children are most susceptible to the disease, along with others, like park rangers and firefighters, who spend time outside. Its estimated that 300,000 people nationwide are diagnosed with Lyme disease each year.
Also Check: Doctors Who Specialize In Lyme Disease
What Are The First Signs And Symptoms Of Lyme Disease
In the first early localized stage of Lyme disease the skin at the site of the tick bite becomes infected with Borrelia burgdorferi bacteria which can cause an expanding round or oval red skin lesion called erythema migrans. This may or may not be associated with flu-like symptoms within days to a month after the tick bite such as achiness, chills, fever, sweats, fatigue, malaise, headache, stiff neck, muscle soreness, joint pain, swollen lymph nodes, and sore throat. The combination of the skin lesion and flu-like symptoms are the primary manifestations of acute stage Lyme disease. Acute Lyme disease is not associated with typical cold-like symptoms of runny nose, prominent cough, or prominent diarrhea.
Types Of Peripheral Neuropathy
Compression | Other Types of PN
Lyme disease is an inflammatory disease that rapidly progresses. Transmitted by the bite of an infected deer tick, Lyme disease is most common in the Northeast section of the United States. However, the disease has also appeared in the upper East coast, in the upper Midwest, and along the coasts of northern California and Oregon.
Signs of Lyme disease include skin rash and painful inflammation of joints , accompanied by flu-like symptoms. The symptoms of Lyme disease increase in severity as the disease spreads though the body.
Early diagnosis and treatment are important to stop the progression of the disease. If untreated, the disease can result in neurological disorders such as peripheral neuropathy, including Bell’s palsy, as well as pain, numbness or weakness in the limbs. The onset of peripheral neuropathy typically develops weeks, months or years later, if the disease is left untreated.
While potentially serious, Lyme disease can be treated, especially in the early stages. It is important to take preventive measures when outdoors in areas known to have infected deer ticks. Some helpful steps include: wearing enclosed shoes and light colored clothing checking clothing and exposed skin frequently for ticks and using insect repellant containing DEET on skin or clothes.
You May Like: How Does A Human Get Lyme Disease
Older Adults Vulnerable To Lyme Disease
For most people, Lyme disease will result in no lasting illness after some initial flu-like symptoms. But for others, it can become debilitating if left untreated. Older adults can be particularly vulnerable, and they may brush off the effects. Symptoms of Lyme disease that has progressed include short-term memory loss, joint pain or swelling, and fatigue signs often attributed to aging.
You might start thinking, I’m just beginning to lose my memory a bit. And everybody does that as they get older, said Dr. Brian Fallon, a psychiatrist and director of the Lyme and Tick-Borne Diseases Research Center at Columbia University.
Other long-term effects include chronic pain, irregular heartbeat, brain fog, shooting pains or numbness in the arms or legs, and severe headaches.
Fragments From Lyme Bacteria Persist In Joints Even After The Bacteria Are Killed Off
A new study published in Proceedings of the National Academy of Sciences sheds light on this medical mystery. To keep from spilling open, bacteria have rigid cell walls made of a matrix of protein and sugars, called peptidoglycan. Most bacteria recycle their peptidoglycan when they grow and divide, but the peptidoglycan of B. burgdorferi has a peculiar structure, and the bacteria is unable to reuse it. Instead, it dumps it into its immediate surroundings, like a microbial litterbug.
This peptidoglycan collects in the joints where B. burgdorferi is found. Almost all patients in the PNAS study with Lyme arthritis had peptidoglycan in their joint fluid. Most of them also had specific antibodies to peptidoglycan in the joint fluid, suggesting that the peptidoglycan was driving the inflammatory process. These antibodies were not found in fluid from people with other joint conditions, such as rheumatoid arthritis, osteoarthritis, or gout.
Patients with Lyme arthritis who did not get better with antibiotics still had peptidoglycan in their joint fluid. However, their joint fluid did not contain detectable B. burgdorferi DNA. This suggests that even after the bacteria were killed off, the peptidoglycan stayed behind, and stimulated further inflammation. This may explain why people with Lyme arthritis who do not respond to antibiotics may improve with medications that damp down the immune system, such as methotrexate or TNF inhibitors.
You May Like: How To Avoid Lyme Disease
Lyme Disease Vs Rheumatoid Arthritis
Lyme disease can sometimes be confused for other conditions, and its not uncommon for patients presenting with Lyme disease-related joint pain to be misdiagnosed with rheumatoid arthritis . Both Lyme and RA cause joint pain and can be debilitating when left untreated, but there are differences.
- Lyme arthritis tends to manifest in larger joints , on one side of the body. Lyme joint pain tends to come and go.
- Rheumatoid arthritis occurs more often in the hands, feet, fingers, and toes, and shows up on both sides of the body. RA joint pain and stiffness occurs every day, and is usually chronic.
- Lyme disease usually goes away when treated, and most patients make a full recovery.
- Rheumatoid arthritis treatment can manage symptoms and show the progression of the disease, but there is no cure.
Lyme pain can often migrate throughout the body, and patients may have pain in their knee one week, and in their wrists the following week, says Chicago-based integrative medicine specialist Casey Kelley, MD. With rheumatoid arthritis, the pain often stays where it begins and does not migrate.
Getting Lyme puts you at greater risk for later developing RA and other types of inflammatory arthritis. One study found that nearly one-third of participants who had Lyme-arthritis later developed an inflammatory arthritis.
Lyme disease symptoms typically begin 3-30 days after youve been bitten by a tick. Early symptoms of Lyme disease include:
- Bulls eye rash
How To Avoid Getting Lyme Disease
Of course, the best way to conquer Lyme disease is to avoid it in the first place, said Thomas Mather, a professor of public health entomology at the University of Rhode Island and director of the Tick Encounter Resource Center.
That has become harder to do. The dramatic increase in cases of Lyme disease is likely due to the movement of white-tailed deer into semi-urban settings, Mather said. The ticks need those deer to reproduce.
Mather urges these precautions:
- Be aware of which ticks are present in your geographical area. Also, what time of year theyre most active.
- Use tick repellent. The CDC says it should contain 20 percent or more DEET, picaridin or IR3535 on exposed skin.
- Use a permethrin spray on clothing, including shoes, socks and pants. You can also buy clothing that has been pre-treated with permethrin.
- Do a daily tick check, even if youre just out in your yard or garden. Ticks can attach to your shoes and crawl up the inside of your pants leg.
- Keep an eye on your pets. They can bring into your house ticks that may simply fall off and land on your rug or furniture.
Don’t Miss: What Are The First Symptoms Of Lyme Disease
Lyme Disease Joint Pain And Arthritis
Lyme disease and joint pain unfortunately go hand in hand, as Lyme-related arthritis is commonly found in Lyme disease sufferers. If you have Lyme arthritis, you have swollen, painful joints that cause stiffness and pain. It is found in people who are in the late stages of Lyme disease. According to an article in Science Daily, approximately 60 percent of patients with untreated Lyme disease will develop related arthritis.
Lyme arthritis is caused by the bacteria that causes Lyme disease getting into your joints and causing inflammation of your tissues. Over time, this can cause damage to your cartilage. Most cases of Lyme arthritis are short-lasting and affect only one large joint.
Lyme arthritis can affect your:
- Knees
- Elbows
- Shoulders
In the U.S., its estimated that about 60 percent of untreated Lyme disease patients will experience intermittent episodes of swelling and lyme disease joint pain for months to years after they are infected by a tick bite.
Thankfully, most Lyme arthritis cases can be treated with antibiotics and NSAIDs, although some people may require surgery to remove some diseased tissue. Around ten percent of untreated patients may go on to develop chronic arthritis, reports Johns Hopkins Arthritis Center.
Lyme Disease & Plantar Fasciitis
A Lyme co-infection called Bartonella can cause the same foot and heel pain symptoms as plantar fasciitis:
- Painful inflammation along the bottom of your foot
- Pain is worst first thing in the morning
- Long periods of standing or sitting cause pain to flare up
Statistically, Americans are more likely to suffer from plantar fasciitis than Bartonella. No matter the cause of your foot pain, its important to learn the root cause for effective treatment. Our experienced surgical podiatrists will evaluate your foot and heel pain with a view to creating an effective and lasting treatment plan. Back to top
Milwaukee podiatrists treating all types of foot, heel & ankle pain
Our team of elite surgical podiatrists are committed to providing the highest level of care for every patient. Well take the time to listen as you describe your symptoms, and provide solutions for fast pain relief and long-term results.
Recommended Reading: Lyme Disease Specialists In Maryland
Chronic Lyme Disease Vs Acute And Late Stage Lyme
One reason chronic Lyme disease is harder to detect and treat than Lyme at earlier stages is that chronic Lyme disease symptoms are more wide-ranging and varied. Chronic Lyme disease can cause symptoms of early Lyme disease such as fatigue and muscle aches to recur, but it can also cause new symptoms that affect different parts of the body.
Mitochondria Dysfunction And Chronic Pain
Mitochondria are the energy factories found in every cell. By some estimates there are 300 to 400 mitochondria in a cell. Chronic infection can damage the mitochondria. There is a growing body of science showing damaged mitochondria leads to chronic pain.
Lyme Disease Pain Strategy
It is possible to repair mitochondria. See How to Fix Mitochondria & Get Energy in Lyme Disease for steps to repair the injured mitochondria.
One other strategy is to eat low inflammatory foods which support mitochondria. See The Best Brain, Inflammation, Pain, Energy, and Detox Diet Ever for more information about an effective paleo diet.
Read Also: How To Get Rid Of Lyme Disease In Humans