Lyme Disease Test Two
Two-tiered Lyme disease testing uses two tests. The first is a screening test that should detect anyone who might have the disease. Tests that do this well have are regarded as having high sensitivity. This test is followed by a second test that is intended to make sure that only people with the disease are diagnosed. Tests that do this well have high specificity.
HIV/AIDS is diagnosed with tests that are both highly sensitive and highly specific. They are accurate more than 99% of the time. In Lyme disease, the second test is highly specific. So there are few false positives. Unfortunately, the screening test is highly insensitive and fails to accurately identify patients who have Lyme disease. The two-tiered test system misses roughly 54% of patients.
Because of this, LDo recommends the patients and physicians skip the ELISA and go straight to the Western blot.
Access To Lyme Disease Testing Services
This guidance on the laboratory diagnosis of Lyme disease is intended for healthcare professionals in the UK. Patients concerned about possible Lyme infection should consult an appropriate healthcare professional, for example their GP, in the first instance.
Health professionals wishing to discuss a possible case or ascertain local arrangements for testing should contact a local Infection specialist .
NHS testing for Lyme disease is available through local service providers and the Rare and Imported Pathogens Laboratory at PHE Porton where ISO15189 accredited confirmatory testing is also provided. RIPL is also introducing a testing service for neurological Lyme disease.
RIPL provides medical and laboratory specialist services to the NHS and other healthcare providers, covering advice and diagnosis of a wide range of unusual bacterial and viral infections, including Lyme disease.
RIPL continuously updates its methods and will make further information on Lyme disease diagnostic testing available as it arises.
What Abnormal Results Mean
A positive ELISA result is abnormal. This means antibodies were seen in your blood sample. But, this does not confirm a diagnosis of Lyme disease. A positive ELISA result must be followed up with a Western blot test. Only a positive Western blot test can confirm the diagnosis of Lyme disease.
For many people, the ELISA test remains positive, even after they have been treated for Lyme disease and no longer have symptoms.
A positive ELISA test may also occur with certain diseases not related to Lyme disease, such as rheumatoid arthritis.
Read Also: Can Lyme Disease Cause Leg Pain
How To Test For Lyme Disease
Wondering how to get tested for Lyme disease? The Centers for Disease Control and Prevention suggests a two-step testing process to check for a Lyme disease infection, both of which involve antibody testing , typically done on the same blood sample.
If the first step in the process returns a negative test result, then the second step is not necessary. However, if the first step yields a positive result, the second test is recommended as confirmation of a Lyme disease diagnosis. The Everlywell Lyme Disease Test follows this recommended protocol from the CDC, so it includes the two-step testing process.
Should You Get A Test For Lyme Disease
If Lyme disease is treated soon after a tick bite, the outlook is great. Most cases of Lyme disease respond to a 2- to 4-week round of antibiotics.
If Lyme disease goes untreated, it can be more difficult to eliminate. For some, it can lead to inflammation of the joints, heart, and nervous system. Progression of the disease, and its severity, can vary from person to person.
Lyme disease is staged in categories: acute, early disseminated, and late disseminated. Later stages of Lyme disease may involve multiple systems in the body.
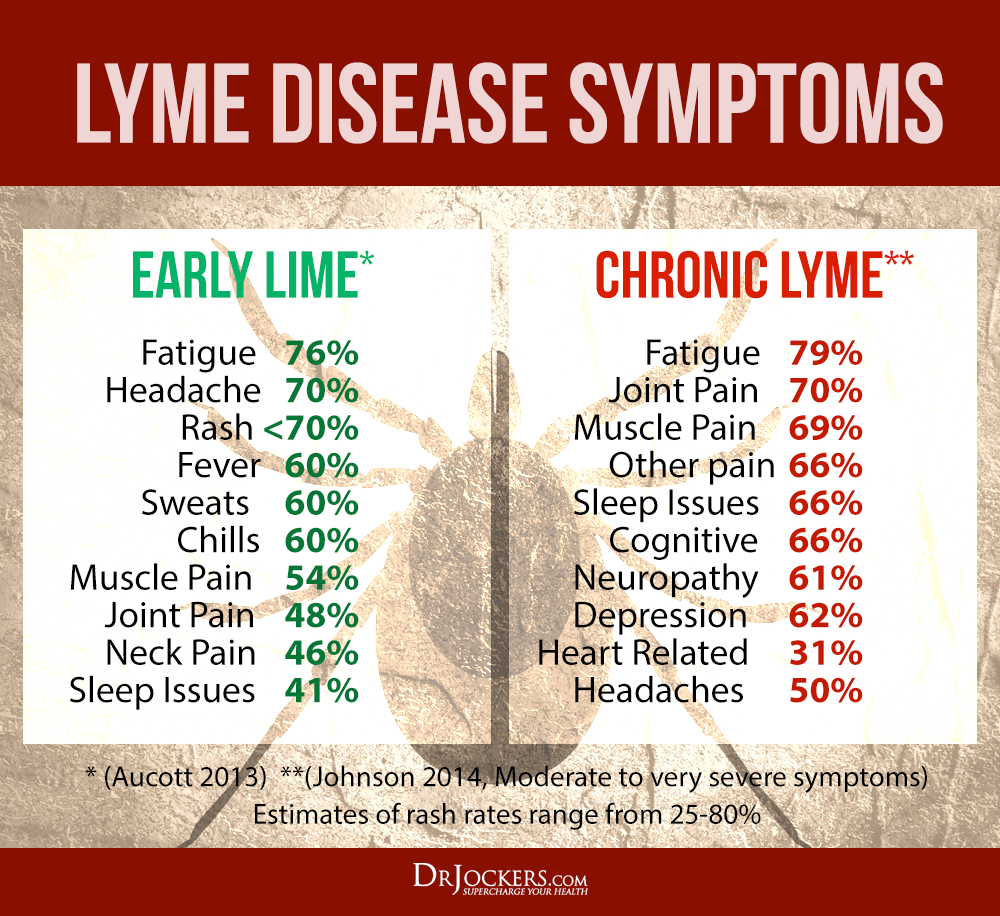
The most common sign of Lyme disease is an erythema migrans, or bulls-eye rash. The rash often appears after a delay of 3 to 30 days after the tick bite, according to the
Research from 2014 suggests that the bulls-eye rash may last for 3 to 4 weeks. About 80 percent of people with Lyme disease have a single erythema migrans rash. But the bacteria can spread and lead to multiple rashes, indicating disseminated Lyme disease.
While a rash is the most common symptom of Lyme disease, it isnt the only one.
With disseminated Lyme disease, symptoms can also include neurologic conditions, such as cranial nerve palsy and meningitis that mimics aseptic meningitis. Heart inflammation can also be a sign of Lyme disease.
If youre experiencing any of these signs or symptoms, an at-home test may help you identify Lyme disease. With the click of a button, a test can be shipped to your front door.
To select the best tests, we look at studies and user reviews.
Also Check: Hotels Near Old Lyme Ct
How Do You Test For Lyme Disease With An At
Hereâs how to check for Lyme disease with the Everlywell test.
To take our at-home Lyme Disease Test, collect a small sample of blood with a simple finger prick. Youâll then send the sample to a lab for analysis , and youâll be able to view your results on our secure, online platform.
Consider taking this Lyme test if:
- You have traveled to areas infested with ticks that can transmit Lyme bacteria , found ticks on your body, and are now experiencing symptoms of Lyme disease.
- If you believe you have been exposed to a tick and are experiencing symptoms , taking this antibody test can help assess for Lyme disease. If you have been tested previously, but are now having new symptoms, this Lyme disease test kit can also help.
How To Avoid Tick Bites
To reduce the chance of being bitten:
- cover your skin while walking outdoors and tuck your trousers into your socks
- use insect repellent on your clothes and skin products containing DEET are best
- stay on clear paths whenever possible
- wear light-coloured clothing so ticks are easier to see and brush off
Also Check: Do You Get A Rash With Lyme Disease
How Do You Diagnose The Later Stages Of Lyme Disease
Disseminated Lyme disease, due to unsuccessful or delayed treatment, can become disabling. The bacteria can leave the skin where it was initially inoculated by the tick and travel through the bloodstream to numerous systems of the body, primarily joints, heart, brain, muscles and the nervous system.
Late disseminated Lyme disease has a wide range of presentations including joint pain, extreme fatigue, neuromuscular pain, cardiac problems, headaches, and other central nervous system dysfunction. There are some distinguishable signs of later stage Lyme disease including facial palsy in the second stage, and swollen knees in the third stage that are somewhat specific for Lyme disease, but not absolutely, because there are other causes of Bells Palsy and swollen knees.
Diagnosis can be confirmed by serology blood tests which measure the antibodies that are formed by the immune system in response to the Lyme disease bacterial infection. Collection of cerebrospinal fluid by lumbar puncture may be indicated in neurologic cases that may involve the central nervous system.
If I Am Worried About Lyme Disease Who Can I Talk To
Lyme disease is being increasingly recognised as causing illness and hardship, if the diagnosis is missed. Over the last number of years, there has been a marked increase in awareness of the condition among GPs and hospital doctors in Ireland. Each of the HSEs Hospital Groups have a number of Infectious Disease Consultants who are expert in the diagnosis and management of Lyme disease. If you have been bitten by a tick or have other reasons to strongly suspect you may have Lyme disease, you should visit your GP for advice.
Also Check: Google What Is Lyme Disease
If The C6 Test Is Positive What Is The Next Step
A positive C6 test means antibodies to C6 were found. The next step is to do a QC6 test, which determines if the levels of antibody are high enough to justify treatment. If the value of the QC6 is higher than 30 IU/mL and signs of illness are present, then antibiotic treatment should be considered. If the QC6 is less than 30 IU/mL and there are no signs of illness, then treatment may not be necessary.
In addition to doing the QC6 test, your veterinarian may want to take samples of blood and urine to assess kidney function and to look for protein in the urine. A positive test for protein in the urine could signal serious underlying kidney disease.
How Is Lyme Disease Treated
Common antibiotics are effective at clearing the infection and early symptoms and in helping to prevent the development of complications. If untreated, the disease will progress to a longer-term form in about half of patients. Antibiotics are generally given for up to three weeks. If complications develop, intravenous antibiotics may need to be used to treat the infection. The bacteria can survive for long periods in the body even if no symptoms develop. If untreated, the bacteria can cause chronic irritation in in a number of the bodys organs. That is why early diagnosis and treatment with antibiotics is important.
Also Check: How To Confirm Lyme Disease
Cdc Supports The Development Of New Tests
New tests may be developed as alternatives to one or both steps of the two-step process. Before CDC will recommend new tests, they must be cleared by the Food and Drug Administration . For more details, see: Recommendations for Test Performance and Interpretation from the Second National Conference on Serologic Diagnosis of Lyme Disease.
Question 3 Is There A Molecular Test For Lyme Disease

One example of a molecular test for Lyme disease at Quest is the Lyme Disease DNA, Qualitative Real-Time PCR, Blood . Amplification of Borrelia genomic DNA from blood, fluids or tissues can support the diagnosis of Lyme disease. Click here for a list of this and other molecular tests for Lyme disease at Quest.
Don’t Miss: Doxycycline Monohydrate For Lyme Disease
Current Research On New Approaches
NIAID actively supports research on Lyme disease diagnostics. Small businesses and public/private partnerships often submit applications for new research projects. NIAID grantees also work directly with CDC scientists to evaluate and compare the effectiveness of currently used diagnostic methods.
Working with CDC, NIAID plays a major role in encouraging the development of new approaches to improve Lyme disease diagnosis in people with tick-borne co-infections such as anaplasmosis or babesiosis. New diagnostic tests are also needed to distinguish between people with B. burgdorferi infection and those whose immune responses stemming solely from past Lyme disease vaccination. Although Lyme disease vaccines for humans are no longer available in the United States, the discontinued LYMErix vaccine used between 1998 and 2002 was based on a specific part of B. burgdorferi called outer surface protein A . In response to the vaccines, immunized individuals developed antibodies for OspA. Because the conventional ELISA measures OspA antibodies to determine if someone has Lyme disease, the test does not provide accurate results for immunized individuals. People who received the vaccination will test positive whether or not they are actually infected with B. burgdorferi.
NIAID is supporting research on a variety of approaches to improve the diagnosis of Lyme disease:
Current Problems With Lyme Disease Diagnosis & Patient Care
- Diagnostic tests cannot yet accurately identify the earliest stage of Lyme disease when making the diagnosis is crucial.
- The rash is not always present or easily recognized
- Misdiagnosis and delayed diagnosis can make Lyme disease more difficult to treat and lead to prolonged and debilitating illness
- Early symptoms can be mistaken for a summer flu
- Lyme disease can involve several parts of the body, including joints, connective tissue, heart, brain, and nerves, and produce different symptoms at different times.
- Antibody testing done after early treatment may be negative and never turn positive for some cases
- Borrelia burgdorferi can evade our protective immune system and trigger immune system dysfunction.
- No reliable blood test is presently available to measure treatment success, necessitating close clinical follow up and improved physician education.
- Presently there is no vaccine to prevent Lyme disease available to humans.
Also Check: Lyme Disease And Massage Therapy
How Is Lyme Disease Diagnosed How Reliable Are These Lab Tests
There are several tests available to diagnose Lyme disease. The CDC recommends using a two-part process. If the first step, called an EIA , yields a positive result or is difficult to interpret, a second step, called a Western Blot test, is used for confirmation.
Unfortunately, these and other diagnostic methods are beset by shortcomings, particularly methods which rely upon blood samples. According to the Lyme Research Alliance, Lyme disease blood testing is fraught with problems and, at best, should only be an adjunct to the clinical diagnosis of the disease a statement which appears to align with observations by medical researchers. For example, consider this excerpt from a 2012 study published in Open Neurology Journal :
In considering the diagnosis of Lyme disease, a major problem is the inability of documenting the existence and location of the bacteria. After the initial transfer of the bacteria from the Ixodes tick into the person, the spirochetes spread locally, but after an initial bacteremic phase, the organisms can no longer be reliably found in body fluids Currently, the use of circulating antibodies directed against specific antigens of the Lyme borrelia are the standard means to diagnose the disease, but specific antibodies are not an adequate means to assess the presence or absence of the organism.
- ADD
Other Diagnostic Tests For Lyme Disease
Some laboratories offer Lyme disease testing using urine or other body fluids. These tests are not approved by FDA because they have not been proven to be accurate. For example, one study of urine-based polymerase chain reaction assays for Lyme disease diagnosis showed that with currently available tools, urine cannot be used to accurately diagnose Lyme disease. Another study by NIAID-supported scientists showed that the Lyme Urinary Antigen Test was unreliable and resulted in excessive numbers of false positives. In the same study, researchers confirmed that an ELISA followed by a Western blot test was nearly 100 percent reliable in diagnosing Lyme disease. With the availability of so many Lyme disease tests, including non-commercial tests developed by individual facilities, it is impossible to address the accuracy of each one. The development of new, rapid, clearly validated diagnostic tests continues to be a need.
You May Like: Amoxicillin Vs Doxycycline For Lyme
How Much Does A Lyme Disease Test Cost
The cost of a Lyme disease test depends on what type of test is performed an ELISA test or a combination of ELISA and western blot tests.
Averagely, the cost for an ELISA test for Lyme disease is in the vicinity of $120 or more. If you include a confirmation western blot test, it can attract an additional $130 or more. More details on pricing can be referenced on our website.
Although an ELISA test might come back negative, it is best to combine it with a western blot test because not everyone shows the rash or bulls eye symptoms of Lyme disease.
After a successful diagnosis and treatment, it is equally important to do a follow-up test for Lyme disease years later to be sure that any similar flu-like symptoms are something else and not the same disease reoccurring.
Types Of Lyme Disease Tests
Antibody titer tests for Lyme disease measure antibodies that are specific to the bacteria that can trigger the condition. Antibodies are part of the bodys immune response. Tests look for two types of antibodies, known as immunoglobulin M and immunoglobulin G .
IgM antibodies usually peak within a few weeks after an infection with Borrelia bacteria and start to collapse 4-6 months after infection. IgG antibodies are slower to develop, beginning to show 4-6 weeks after exposure and may peak 4-6 months after exposure. While IgM tends to be associated with an active infection, both IgM and IgG can persist in the blood for many years.
The Centers for Disease Control and Prevention recommends a two-stage or two-tiered test for these antibodies. If the initial blood test is positive for IgM or IgG antibodies associated with the Borrelia bacteria, a second test is done, often using different laboratory methods.
Testing for IgM and IgG can support the finding that you have been exposed to Borrelia, but this on its own does not prove whether or not you have Lyme disease.
Follow-up testing may be necessary if testing is inconclusive. This could involve repeat blood tests or the use of different types of medical tests to rule out other health conditions. In people suspected of bacterial reinfection, imaging tests may be used to detect joint inflammation.
You May Like: Is Diarrhea A Symptom Of Lyme Disease
Borrelia Species Pcr Results
Borrelia species DNA may occasionally be detected in the blood by PCR, but a negative PCR test is of no value in excluding localised Lyme disease.
The overall sensitivity of PCR on a skin biopsy of an EM or ACA rash is around 50% and is limited by the chance of a single biopsy hitting a site with a significant number of organisms.
In neurological Lyme disease involving the CNS, up to 10% of cases may be PCR positive on a CSF sample a negative PCR result does not exclude the diagnosis.
Synovial fluid may be positive by PCR in up to 50% of cases. A negative result does not exclude the diagnosis.
Lyme Disease Antibody Test Procedure
The Lyme disease antibody test requires no advance preparation. A lab technician will swab the inside of your elbow with an antiseptic before drawing your blood. Your blood will be drawn from a vein in your arm using a small needle.
The blood draw should not be painful, though you might feel a slight prick when the needle is inserted into your vein.
The blood sample will be collected in a vial. The puncture site will be bandaged, if needed, after the needle is removed. After the blood draw, you are free to go home.
There are very few risks associated with the Lyme disease antibody test. Excessive bleeding is possible, but there may be an increased risk if you take blood thinning medications or certain anti-inflammatory drugs like:
- heparin
Also Check: Bitten By A Tick Lyme Disease