Can Lyme Disease Cause Fasciculations
4.6/5Lyme canwillcomplete answer
Chronic Lyme disease symptoms: Headaches, extreme fatigue, facial paralysis, tingling sensations, stuff neck, swollen glands, sore throat, twitching of muscles, eye floaters, extreme menstrual symptoms, buzzing in ears, nausea, vomiting, night sweats, costochondritis, shortness of breath, mood swings, depression,
Similarly, what diseases cause Fasciculations? Fasciculations in motor neuron diseasesNumerous motor neuron diseases occur with fasciculations,38 such as Progressive Spinal Muscular Atrophies, Amyotrophic Lateral Sclerosis, Benign Monomelic Amyotrophy, Post-Polio Syndrome, Kennedy’s disease, among others.
Just so, can Lyme cause Parkinson’s?
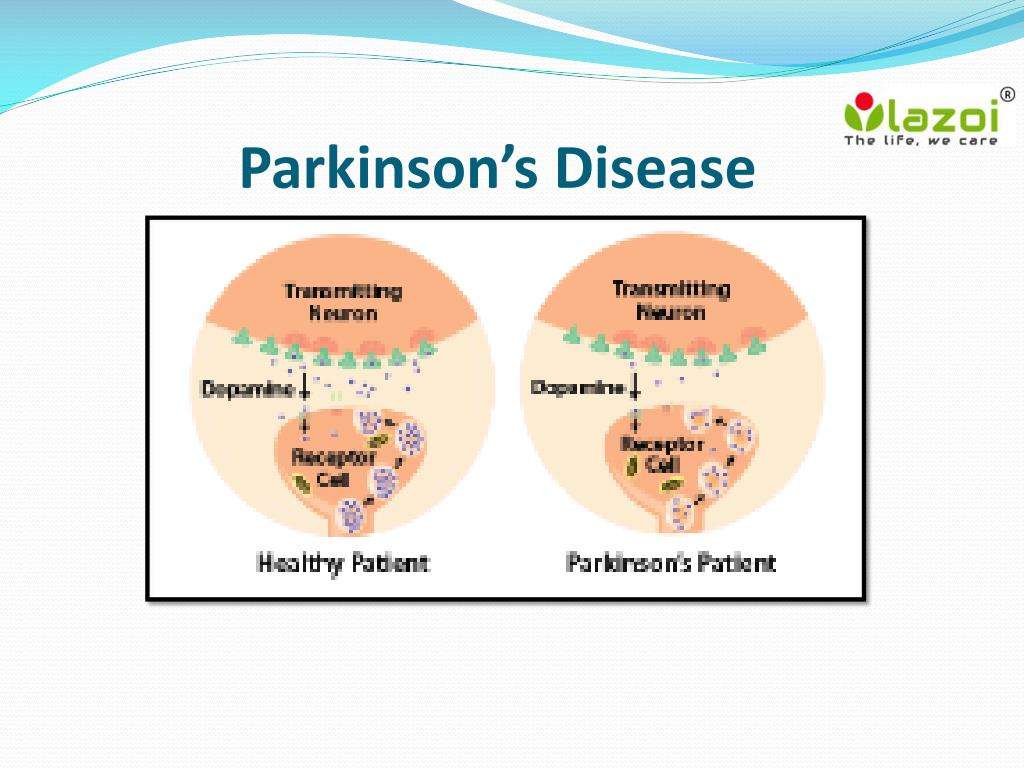
Lyme can cause Parkinson’s in a person with the right genetic and environmental risks and exposures. Parkinson’s is probably a result of inflammation in the brain resulting in destruction of dopamine producing cells. Treating the Lyme will help reduce inflammation.
What are the neurological symptoms of Lyme disease?
Lyme associated neurological symptoms may include:
- Facial palsy/weakness .
- Headache/neckache.
- Double vision .
New Possible Correlation Between Lyme Disease And Lewy Body Dementia
Lyme disease, also known as Lyme borreliosis, is an infectious disease caused by Borrelia burgdorferi bacterium, which is spread by ticks. The most common sign of infection is a red rash that appears at the site of the tick bite. Other signals of Lyme include flu-like symptoms, joint pain and weakness in the limbs.
After a 69-year-old woman was diagnosed and repeatedly treated for Lyme disease for 15 years before her death, researchers at the Tulane National Primate Research Center who had previously discovered the persistence of B. burgorferi despite antibiotic therapy found that the same bacterium was still intact upon autopsy.
In addition to the typical symptoms of Lyme, she experienced continual neurological decline, including a severe movement disorder and personality changes. The woman eventually passed away after being diagnosed with Lewy body dementia a disease that presents itself with similar declined motor functions of Parkinsons Disease with the added element of significant memory issues.
The Tulane research team found that her central nervous system still harbored intact spirochetes despite aggressive antibiotic therapy for Lyme disease at different times throughout her illness. The findings may lead to a correlation between Lyme disease and Lewy body dementia.
To learn more about research being done by Tulane NPRC, please visithere.
What Are The Symptoms Of Chronic Lyme Disease
An extensive list of symptoms of chronic Lyme disease was developed by Dr. Joseph Burrascano, a pioneer in treating chronic Lyme disease. Many Lyme symptoms, such as fatigue, cognitive impairment, joint pain, poor sleep, mood problems, muscle pain, and neurological presentations also occur in other diseases.
Recommended Reading: Lyme Disease Class Action Lawsuit
Infection And Risk Of Parkinsons Disease
Article type: Review Article
Authors: Smeyne, Richard J.a | Noyce, Alastair J.b c | a | Savica, Rodolfod | e *
Affiliations: Department of Neuroscience, Vickie and Jack Farber Institute of Neuroscience, Thomas Jefferson University, Philadelphia, PA, USA | Preventive Neurology Unit, Wolfson Institute of Preventive Medicine, Queen Mary University of London, London, UK | Department of Clinical and Movement Neurosciences, UCL Institute of Neurology, London, UK | Department of Neurology, Mayo Clinic, Rochester, Minnesota and Division of Epidemiology, Department of Health Sciences Research, Mayo Clinic, Rochester, MN, USA | The Edmond J Safra Program in Parkinsons disease, Toronto Western Hospital and the University of Toronto, Toronto, Canada
Correspondence: Correspondence to: Connie Marras MD, PhD, 7-MCL 399 Bathurst St. Toronto, Ontario, M5T 2S8, Canada. Tel.: +1 416 603 6422 Fax: +1 416 603 5005 E-mail:.
Keywords: Parkinsons disease, infection, viruses, bacteria, etiology
DOI: 10.3233/JPD-202279
Journal: Journal of Parkinson’s Disease, vol. 11, no. 1, pp. 31-43, 2021
Abstract
Thanks For Signing Up
We are proud to have you as a part of our community. To ensure you receive the latest Parkinsons news, research updates and more, please check your email for a message from us. If you do not see our email, it may be in your spam folder. Just mark as not spam and you should receive our emails as expected.
Don’t Miss: Common Signs Of Lyme Disease
Bacterial Infections And Pd Risk
The ample spectrum of bacteria that may acutely or permanently infect the tissues of humans has been associated with the development and, to a lesser extent, with the progression of PD. Bacterial production of pro-inflammatory and neurotoxic factors might play a major role in the development and/or in the cascade of neurotoxic events leading to degeneration. One key player in such events is the bacterial endotoxin lipopolysaccharide . LPS stimulates production of several inflammatory factors that may contribute to neurodegeneration. Tumor necrosis factor- is released from microglia nitric oxide is released by microglia and astrocytes in and there is hyperproduction of prostagladins. All of these phenomena may lead to neurodegeneration and gliosis . Given that LPS is the endotoxin of Gram-negative bacteria, theoretically, every Gram-negative infection can induce a cascade that could trigger PD however, the evidence on bacteria is limited to a number of specific organisms.
Notably, there is minimal evidence for associations between more severe infection such as sepsis and the future risk of PD. A recently published case-control study reported that there was no association between severe infections that required hospitalization and sepsis and the risk of PD later in life . However, it is not yet clear whether an infectious condition proximate to the onset of PD or before the onset of PD can trigger or lower the threshold for the upcoming neurodegenerative process.
A Case Of Lyme Disease And Parkinsons Disease
Some people with LD will have symptoms of brain problems after their diagnosis. These problems can include memory loss and shaking of the hands and feet. Most of these problems go away after the person takes medications to treat LD.3 There is one time that a person had symptoms of Parkinsons disease after his treatment for LD. These symptoms continued to get worse until the person eventually passed away.1 This is the only case that doctors know of someone who developed Parkinsons disease from LD. This case of Parkinsons disease was verified by an autopsy. This person had no brain symptoms before his LD diagnosis. Researchers dont know if the LD caused the Parkinsons disease symptoms, or if this person would have developed Parkinsons disease without having LD.
Recommended Reading: Getting Tested For Lyme Disease
Myths And Facts About Parkinsons Disease
For those living with Parkinsons, separating the myths from the facts can be a big challenge. So, from causes to treatment to quality of life, weve answered some of your common questions.
18,000 people a year are diagnosed with Parkinsons, however theres still a lot that people dont know about the disease. Weve separated the fact from the fiction.
Fact: Exercise Can Help Parkinsons Disease
Yes, doing at least 2.5 hours of exercise a week can slow the progression of Parkinsons disease symptoms.
Those living with Parkinsons should choose exercises which are safe, easy to stick with and, most importantly, enjoyable. Walking, dancing, and light aerobics are popular and can help increase balance and agility.
Most popular with our readers
Parkinsons can be a lonely experience. Whether with family, friends, or a local group, exercise is a great way to stay social and can boost your mood too.
Exercises for Parkinsons
All exercise is good for you, however certain activities are better suited to the different stages of Parkinsons.
For mild symptoms, focus on exercises that really build up a sweat and get the whole body moving, such as running, cycling or swimming.
For more progressed symptoms, exercises that improve balance and flexibility are ideal. Yoga or a fast paced walk can target specific areas of the body to improve strength.
For complex symptoms, gentle home workouts and chair exercises can help make everyday tasks easier.
Always get advice from a nurse or physiotherapist before starting a new exercise. They may also provide information on Parkinsons exercise classes. If youre looking for inspiration you can also try Parkinsons UKs exercise toolkit.
You May Like: Can You Get Lyme Disease From Eating Deer Meat
Those With Experience Issue Warning: Be Lyme Aware
Nymphal deer ticks, which cause most of the Lyme disease cases, are tiny about the size of a sesame seed. Adult deer ticks can also cause infection.
- Submitted
A Hugo resident who loves the outdoors, Brenda Peltier said she now avoids the woods like the plague for fear of ticks.
- Submitted
Nymphal deer ticks, which cause most of the Lyme disease cases, are tiny about the size of a poppy seed. Adult deer ticks can also cause infection.
- Submitted
The month of May doesnt just bring flowers. It also brings that nemesis of the great outdoors: the blacklegged tick that causes Lyme disease.
May is Lyme Disease Awareness Month. Talk to people who attend a local Lyme support group, and it becomes obvious the disease is endemic here, despite myriad efforts to preach prevention.
Preventing a tick bite remains the primary goal of the Minnesota Lyme Association , a 15-year-old advocacy group that holds monthly support meetings at the White Bear School District Center , in addition to hosting speakers with expertise on researching, diagnosing and treating tick-borne diseases.
Founded by Anne Myre of Scandia in 2006, MLA helps those afflicted by Lyme or tick-borne disease lead a healthy, vibrant life. She started the support group out of desperation as she was suffering from chronic fatigue and joint pain that was traced to a tick bite.
Myres goal with the nonprofit she started is prevention, prevention, prevention.
Better diagnostics, treatment strategies
What Happened To The Classic Bull’s
An initial bite from a tick can cause a rash that will appear in three months to a year. While the characteristic “bull’s-eye” rash is associated with Lyme disease, the rash only appears in an estimated 50% of infected individuals, or it may appear in a different form. If this rash does appear, it will generally wane over a two to a four-week period. 70 percent of all patients who do present with Lyme disease complex never recall such a rash.
Read Also: What’s The Cure For Lyme Disease
Lyme Disease Could Be The Real Cause Of Arthritic Symptoms In Children And Adults
The misdiagnosis of arthritic symptoms is actually what first catapulted Lyme disease into the public spotlight more than 40 years ago. A group of adults and children in Lyme, Connecticut, were experiencing various symptoms initially attributed to rheumatoid a
rthritis and juvenile rheumatoid arthritis , respectively. The cause of the symptoms was later linked to tick bites and ultimately Borrelia burgdorferi, the bacterium that causes Lyme disease.
Today, arthritis is still one of the most common misdiagnoses of Lyme disease, especially if patients dont recall being bitten by a tick or dont alert doctors to the fact that they or their children have been in regions where Lyme disease is prevalent. Similar to symptoms of both RA and JRA, Lyme disease can cause joint pain, fatigue, and fever. Patients with Lyme disease, however, may also have additional symptomssuch as headache, chills, sore muscles, and swollen lymph nodes. The presence of a rash can also help distinguish Lyme disease from RA or JRA, but, again, the absence of a rash should not rule out a Lyme disease diagnosis.
Fact: Stem Cells Are A Possible Treatment For Parkinsons Disease

Stem cells have the potential to lead to better treatments for Parkinsons disease, but were not there yet.
These special cells are grown in a lab and can be turned into almost any type of cell. Researchers have been able to turn them into dopamine producing cells to replace those lost to Parkinsons.
However, before becoming an available treatment doctors need to provide more proof stem cells are safe and effective.
Recommended Reading: Foods That Kill Lyme Disease
The Cdc Reveals The Truth About Lyme Disease
Lyme disease is a bacterial infection caused by the bite of an infected black-legged tick, also known as a deer tick. Lyme and its numerous co-infections can mimic or cause virtually any medical, neurological, or psychiatric condition. It is called the great imitator and has been vastly underdiagnosed in the U.S. due to inadequate testing methods and general lack of acknowledgment by the medical community. A nasty relative of the STD syphilis, Lyme causes a multitude of medical, neurological, and psychiatric impairment issues, yet is much harder to cure.
Lymepolicywonk: Misdiagnosis Of Lyme Disease As Ms Mylymedata Quick Bytes
This is the first in what I hope will be a series of quick bytes of some of the preliminary results we are getting from MyLymeData. You can choose to watch the video or read the blog. Today I am going to talk about what we are finding with misdiagnosis. Most of us know that Lyme disease is commonly misdiagnosed as chronic fatigue, fibromyalgia, or depression. But did you know that 20% are misdiagnosed with uncurable progressive neurologic diseases?
MyLymeData is the patient registry launched by LymeDisease.org in November 2015. We currently have 4000 people enrolled in MyLymeData. Our goal is to reach 10,000 enrolled so were well on our way. One of the things we are using MyLymeData for is to find out what is going on with chronic Lyme disease and we do this by asking the patients directly. This blog is based on data from MyLymeData.
We asked patients in the MyLymeData registry if they were initially misdiagnosed with another illness. Unfortunately, most of these patients report that they were initially misdiagnosed and roughly 20% of those with chronic Lyme disease were initially misdiagnosed with a neurologic disease. 14% of chronic Lyme patients report being initially misdiagnosed with MS and roughly 2% are misdiagnosed with other neurologic diseases, like ALS, Parkinsons and Multiple systems atrophy.
Now you might think no harm/no foulso long as they eventually correctly diagnose and treat the Lyme disease.
But thats not true.
Let us know your experience.
Also Check: Can Lyme Disease Cause Leg Pain
Viral Infections And Pd Risk
The notion of a viral etiology to PD has been mooted for many years. One early example, and poi-gnant today in light of the recent SARS-CoV-2 pandemic, was the emergence of a parkinsonian disorder, encephalitis lethargica , that has been linked to the 1918 influenza pandemic. Viruses, particularly those that are neurotropic, are plausible causal agents of PD but have been relatively understudied compared to genetic risk factors and other environmental risk factors for PD. In this section we will consider the viruses that have been linked to PD in observational studies and evaluate the strength of evidence to support a causal link.
Hepatitis B and C viruses have also been investigated for their associations with PD in recent epidemiological studies. Understanding such associations are important given the prevalence of these infections. Hepatitis C virus is an RNA virus of the Flavivirus family and is estimated to infect 143 million people worldwide. It primarily involves the liver with chronic infection resulting in cirrhosis and hepatocellular carcinoma . Extrahepatic manifestations include a myriad of inflammatory and immune-mediated disorders .
Symptoms Of Lyme Disease
The symptomology of Lyme disease is varied and diverse, resulting in significant difficulty in diagnosis. Known as “The Great Imitator,” Lyme disease can mimic the symptoms of Fibromyalgia, Chronic Fatigue Syndrome, MS, ALS, Parkinson’s and Alzheimer’s, as well as more than some 350 other diseases. When patients do present with a number of infections and coinfections, including other tick-borne infections, it is this complicated presentation that we call Lyme Disease Complex.
Don’t Miss: Claritin Protocol For Lyme Disease
What Causes Parkinsons Disease
Parkinsons disease is a chronic, progressive neurological disease that currently affects about 1 million Americans. Parkinsons disease involves a small, dark-tinged portion of the brain called the substantia nigra. This is where you produce most of the dopamine your brain uses. Dopamine is the chemical messenger that transmits messages between nerves that control muscle movements as well as those involved in the brains pleasure and reward centers. As we age, its normal for cells in the substantia nigra to die. This process happens in most people at a very slow rate.
But for some people, the loss happens rapidly, which is the start of Parkinsons disease. When 50 to 60 percent of the cells are gone, you begin to see the symptoms of Parkinsons.
What Is Neurologic Lyme Disease
Neurologic symptoms of Lyme disease occur when the Lyme disease bacteria affect the peripheral or central nervous systems.
- Cranial nerve involvement: When the cranial nerves are affected, facial palsy can occur on one or both sides of the face.
- Peripheral nerve involvement: When the peripheral nerves are affected, patients can develop radiculoneuropathy which can cause numbness, tingling, shooting pain, or weakness in the arms or legs.
- Central nervous system involvement: When the central nervous system is affected, Lyme meningitis can cause fever, headache, sensitivity to light, and stiff neck.
Out of every 100 patients whose cases are reported to CDC, 9 have facial palsy, 4 have radiculopathy, and 3 have meningitis or encephalitis. Because of reporting practices, this statistic may overestimate how often these manifestations are seen by clinicians.
Recommended Reading: Can I Get Tested For Lyme Disease
Infection And Pd: An Epidemiologic Perspective
Additional evidence for a role of an infectious trigger or risk factor for PD is found in studies showing a relationship between specific occupational exposures and PD. In some studies, occupations where there is higher interpersonal exposures show an increased risk of developing PD . There is also a significant body of literature on specific infections and subsequent risk of PD, which will be discussed later in this paper. However, there are significant challenges interpreting epidemiological evidence for etiology in PD. The very long prodromal period, spanning decades, makes measurement of initiating factors difficult due to inadequate availability of records or poor recall. In addition, there is undoubtedly a complex interplay of genetic and environmental factors influenced by the neurodegenerative process during the prodromal period that make interpretation difficult. These general challenges are amplified by the complexity of considering the timing and relative impact of multiple short infectious exposures over a lifetime, the widely varying types of infectious agents, variable severity of infections and the inevitable presence of unrecognized infections. For example, a recent epidemiological study tested the multiple microbe hypothesis and reported that PD risk was increased compared to healthy controls in individuals who were seropositive for five or six of the pathogens studied but not less .