What Are The Risk Factors For Post Treatment Lyme Disease
Risk factors for Post Treatment Lyme Disease include:
- Delay in diagnosis
- Increased severity of initial illness
- Presence of neurologic symptoms
Increased severity of initial illness, the presence of neurologic symptoms, and initial misdiagnosis increase the risk of Post Treatment Lyme Disease. PTLD is especially common in people that have had neurologic involvement. The rates of Post Treatment Lyme Disease after neurologic involvement may be as high as 20% or even higher. Other risk factors being investigated are genetic predispositions and immunologic variables.
In addition to Borrelia burgdorferi, the bacteria that causes Lyme disease, there are several other tick-borne co-infections that may also contribute to more prolonged and complicated illness.
Treatment For Other Forms Of Lyme Disease
People with other forms of disseminated Lyme disease may require longer courses of antibiotics or intravenous treatment with antibiotics such as ceftriaxone. For more information about treating other forms of Lyme disease, see:
The National Institutes of Health has funded several studies on the treatment of Lyme disease that show most people recover within a few weeks of completing a course of oral antibiotics when treated soon after symptom onset. In a small percentage of cases, symptoms such as fatigue and myalgia can last for more than 6 months. This condition is known as post-treatment Lyme disease syndrome , although it is also sometimes called chronic Lyme disease. For details on research into chronic Lyme disease and long-term treatment trials sponsored by NIH, visit the visit the National Institutes of Health Lyme Disease web siteexternal icon.
Lyme Disease In Humans Facts
- Lyme disease is an illness that is spread by bites from ticks infected by the bacterium Borrelia burgdorferi, Borrelia mayonii, Borrelia afzelii, or Borrelia garinii.
- Lyme disease can affect the skin, joints, heart, and nervous system.
- Lyme disease occurs in phases, with the early phase beginning at the site of the tick bite with an expanding ring of redness.
- Lyme disease is diagnosed based on the patient’s clinical signs of illness and the detection of antibodies to the causative bacteria in the blood.
- Lyme disease is treated with antibiotics.
Also Check: Symptoms Of Lyme Flare Up
Learn The Stages Of Lyme Disease
Lyme disease occurs in three stages: early localized, early disseminated and late disseminated. However the stages can overlap and not all patients go through all three. A bulls-eye rash is usually considered one of the first signs of infection, but many people develop a different kind of rash or none at all. In most cases, Lyme symptoms can start with a flu-like illness. If untreated, the symptoms can continue to worsen and turn into a long-lived debilitating illness.
Stage 1: Early Localized Disease
Symptoms with early localized Lyme disease may begin hours, a few days or even weeks after a tick bite. At this point, the
infection has not yet spread throughout the body. Lyme is the easiest to cure at this stage.
Symptoms may include:
- skin rash, which may or may not look like a bulls eye
- flu-like illness, including chills and fever
- fatigue
- muscle soreness and joint pain
- swollen lymph nodes
- sore throat
Stage 2: Early Disseminated Lyme
Early disseminated Lyme may occur several weeks or months after the tick bite. Bacteria are beginning to spread throughout the body. In addition to flu-like symptoms, this stage is often characterized by increase in symptoms such as:
- chills
- pain, weakness or numbness in the arms, legs
- vision changes
- heart problems, such as palpitations, chest pain
- rash may appear on body
- facial paralysis
Stage 3: Late Disseminated Lyme Disease
Related Content
Find a LLMD
Lyme Symptom Tracker App
Get started with your diary
What Is Late Lyme Disease
Lyme disease, also known as Lyme borreliosis, is caused by an infection with the bacteria Borrelia burgdorferi. This bacteria is disseminated through tick bites. Infected ticks usually bite small mammals, who do not develop any kind of infection from the bacteria. When humans are exposed to B. Burgdorferi from a tick bite, however, they can develop Lyme disease.
People who work outside or spend time in woodland areas, where there is greater potential for exposure to tick bites, are most at risk of infection.
Lyme disease is a condition which progresses in stages:
Read Also: What Type Of Doctor Treats Lyme Disease
Do All Ticks Transmit Lyme Disease
No. In the northeastern and north-central U.S., the black-legged tick carries Lyme disease. In the Pacific coastal U.S., the western black-legged tick spreads the disease.
Other major tick species in the U.S., like the lone star tick and the dog tick, do NOT transmit the Lyme disease bacterium. But beware: All 50 states have reported Lyme disease, as well as Canada, Europe, Asia, Australia, and South America.
Who Gets Lyme Disease
Anyone bitten by an infected deer tick can get Lyme disease. Most U.S. cases of Lyme disease happen in Connecticut, Delaware, Maine, Maryland, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, and Wisconsin. But Lyme disease is found in other parts of the U.S., Europe, Asia, and Australia too.
Recommended Reading: Lyme Disease Prevention In Humans
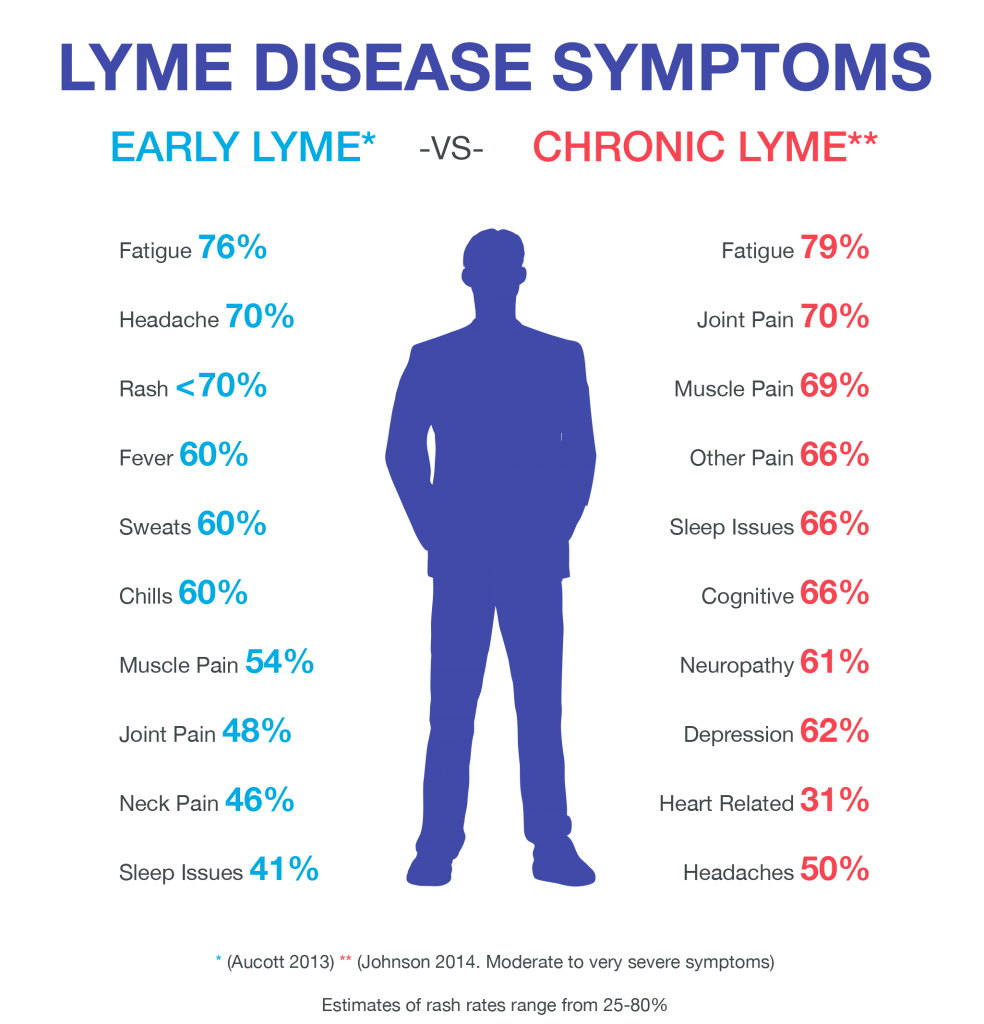
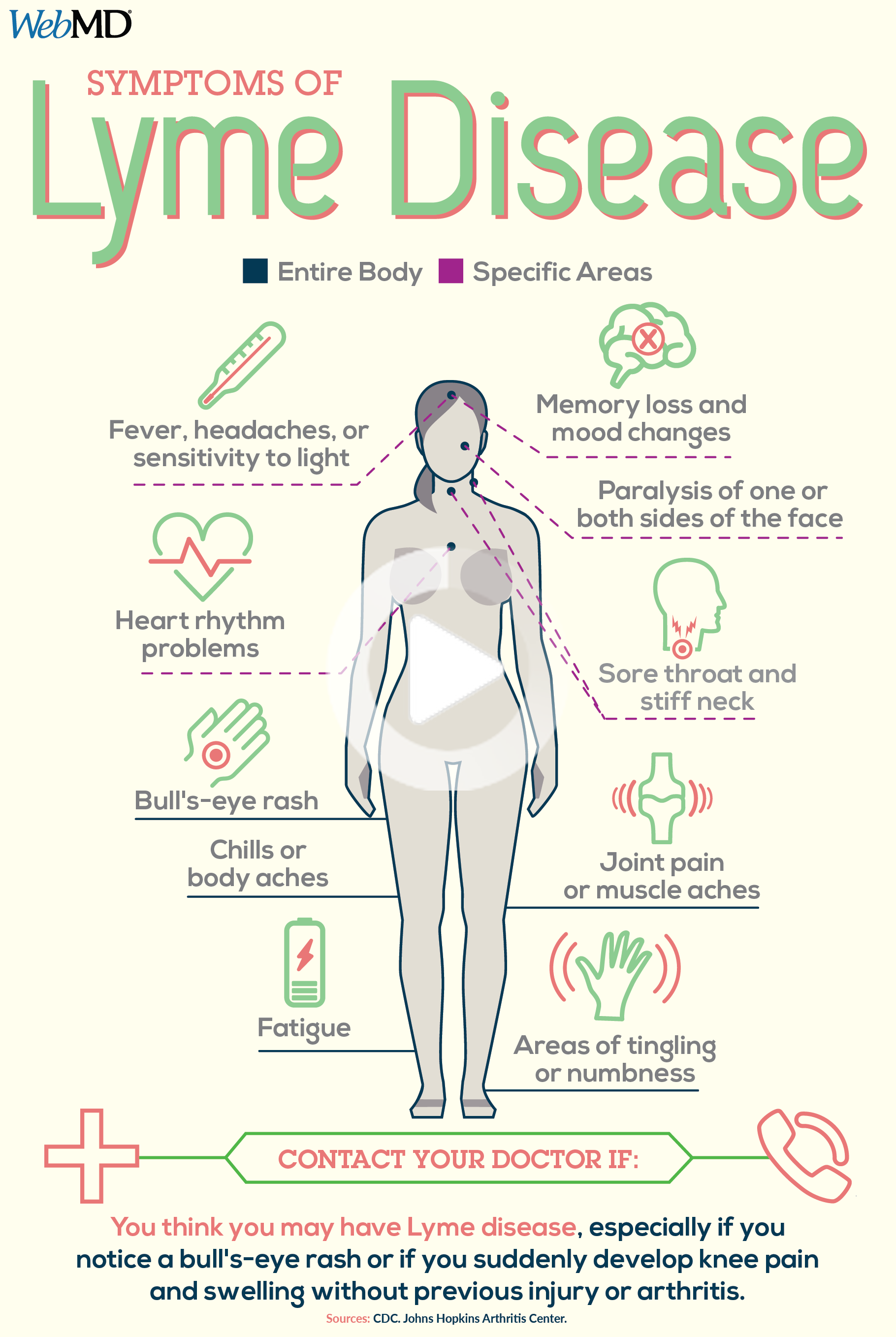
Symptoms: As The Infection Spreads
If the disease goes untreated in its early stages, over several weeks or months it can spread to other areas of the body like your:
- Joints
- Heart
- Nervous system
You could also have more rashes and periods of pain and weakness in your arms or legs. Other symptoms include:
- Facial muscle paralysis
- Headache
- Inflamed brain and spinal cord
What Is The History Of Lyme Disease
Interestingly, the disease only became apparent in 1975 when mothers of a group of children who lived near each other in Lyme, Conn., made researchers aware that their children had all been diagnosed with joint pain from rheumatoid arthritis. This unusual grouping of illnesses that appeared “rheumatoid” eventually led researchers to the identification of the bacterial cause of the children’s condition, which was then named “Lyme disease” in 1982.
The only vector for Lyme disease in the U.S. is the black-legged tick, or deer tick, known as Ixodes scapularis. These ticks are carriers of the Lyme disease spirochete in their stomachs Ixodes ticks may also transmit the Powassan virus. The ticks are vectors that can transmit the bacterium to humans with a tick bite. The number of cases of tick-borne illness in an area depends on the number of ticks present and how often the ticks are infected with the bacteria. In certain areas of New York, where Lyme disease is common, over half of the ticks are infected. Lyme disease has been reported most often in the northeastern United States, but it has been reported in all 50 states, as well as China, Europe, Japan, Australia, and parts of the former Soviet Union. In the United States, it is primarily contracted in the Northeast in the states from Maine to Maryland, in the Midwest in Minnesota and Wisconsin, and in the West in Oregon and Northern California. What those children actually had was Lyme arthritis.
Also Check: How To Cure Lyme Disease Naturally
Disease Reporting And Case Definitions
The Centers for Disease Control and Prevention maintains a list of nationally notifiable diseases . RSMo 192.139, Communicable Disease Reporting, Guidelines for Department, stipulates that communicable disease reporting requirements established by the Missouri Department of Health and Senior Services shall be in accordance with guidelines, funding requirements, or recommendations established by CDC. DHSS has incorporated CDC-mandated diseases as well as selected other diseases for which there are established diagnostic tests into 19 CSR 20-20.020, Reporting Communicable, Environmental and Occupational Diseases . Local public health agencies and/or DHSS are notified by physicians, laboratories, and other reporters when diseases/conditions listed in 19 CSR 20-20.020 are confirmed or suspected. DHSS, in turn, reports cases to CDC.
The usefulness of public health surveillance data depends on its uniformity, simplicity, and timeliness. CDCs case definitions establish uniform criteria for disease reporting and should not be used as the sole criteria for establishing clinical diagnoses, determining the standard of care necessary for a particular patient, setting guidelines for quality assurance, or providing standards for reimbursement. Use of additional clinical, epidemiologic, and laboratory data may enable a physician to diagnose a disease even though the formal surveillance case definition may not be met.
Sign Up For Our Newsletter
Disclaimer: The above material is provided for information purposes only. The material is not nor should be considered, or used as a substitute for, medical advice, diagnosis, or treatment, nor does it necessarily represent endorsement by or an official position of Global Lyme Alliance, Inc. or any of its directors, officers, advisors or volunteers. Advice on the testing, treatment or care of an individual patient should be obtained through consultation with a physician who has examined that patient or is familiar with that patients medical history. Global Lyme Alliance, Inc. makes no warranties of any kind regarding this Website, including as to the accuracy, completeness, currency or reliability of any information contained herein, and all such warranties are expressly disclaimed.
Also Check: Can Lyme Disease Cause Psoriasis
What You Need To Know About Lyme Disease
-
Lyme disease is an infection caused by the spiral-shaped bacteria Borrelia burgdorferi, which is most commonly transmitted by a tick bite.
-
There are over 300,000 estimated new cases of Lyme disease in the United States each year.
-
The symptoms of Lyme disease depend on the how long the infection has been present in the body. The first sign of Lyme disease is often an expanding round or oval red “bullseye” rash.
-
If left untreated, people may develop neurological symptoms and heart problems, and have an approximately 60 percent chance of developing Lyme arthritis.
How Are Dogs Tested For Lyme Disease
Diagnosis is made by a combination of history, physical signs, and diagnostics. For dogs, the two blood tests for diagnosing Lyme disease are called the C6 Test and Quant C6 test. Veterinarians perform both.
The C6 test detects antibodies against a protein called C6. Presence of the antibodies suggests an active Lyme infection. The C6 antibodies can be detected three to five weeks after an infected tick bites a dog and may be found in the bloodstream even before the dog shows signs of illness.
The next step is to do a Quant C6 test. This, along with urinalysis will help determine if antibiotic treatment is necessary.
You May Like: How To Cure Lyme Disease
How To Safely Remove A Tick
Not all ticks carry Lyme disease, and some ticks carry other diseases. To avoid infecting yourself, never crush a tick with your fingers. For more information on the safe removal, disposal and identification of ticks visit CDC.gov/ticks.
Late Or Chronic Lyme Disease Treatment
Experts agree that the earlier you are treated the better, since early treatment is often successful. Unfortunately, a substantial portion of patients treated with short-term antibiotics continue to have significant symptoms. The quality of life of patients with chronic Lyme disease is similar to that of patients with congestive heart failure. Doctors dont agree about the cause of these ongoing symptoms. The primary cause of this debate is flawed diagnostic testing. There is currently no test that can determine whether a patient has active infection or whether the infection has been eradicated by treatment.
The IDSA thinks Lyme disease symptoms after treatment represent a possibly autoimmune, post-Lyme syndrome that is not responsive to antibiotics. The IDSA essentially regards Lyme disease as an acute infection like strep throat that can be treated with a short course of antibiotics. The IDSA guidelines are now eight years old and do not reflect recent science.
ILADS physicians believe that ongoing symptoms probably reflect active infection, which should be treated until the symptoms have resolved. These physicians use treatment approaches employed for persistent infections like tuberculosis, including a combination of drugs and longer treatment durations. The ILADS guidelines have just recently been updated using a rigorous review of the medical literature.
Read Also: Is There A Human Vaccine For Lyme Disease
Chronic Lyme Disease Vs Post
Patients typically use the term chronic Lyme disease to describe the cluster of symptoms that started after getting Lyme disease and that persist despite having received a course of antibiotic treatment which has been deemed curative by the Infectious Diseases Society of America. Patients say, “I’m not cured. I have symptoms now that I never had before Lyme disease. I’m fatigued 90% of the day. My muscles ache. My brain is in a fog. I can’t think clearly any more. I’m super sensitive to light and sound. What is going on? Chronic Lyme disease does exist – I’m a living example of it!”
Whatever one calls it, the experience is the same. Most often these patients experience profound fatigue, pain, and/or cognitive impairment. Mild to moderate levels of depression and anxiety may also accompany these symptoms, as the functional limitations can lead to social isolation, inability to work, and loss of sense of one’s identity as a provider, caretaker, or friend. Sometimes patients find themselves identifying with Job – the just and good man in the Bible whose life was wrecked by illness, death of loved ones, and economic disaster he felt tormented by God.
Treatment Following A Tick Bite
- In some circumstances, a single dose of antibiotic given within 72 hours of a tick bite might prevent the development of Lyme disease. Several criteria must be met:
- The tick must be identified as the blacklegged tick .
- The tick must have been attached for at least 36 hours .
- The tick bite occurred in a highly endemic area
Read Also: Symptoms Of Lyme Disease In My Dog
Lyme Disease In Dogs And Other Pets
Household pets can get Lyme disease, too. Typical symptoms in animals include swollen joints and lameness, fever, and loss of appetite. Experts in the FDAs Center for Veterinary Medicine say that dogs with Lyme disease occasionally develop serious kidney disease that can be fatal.
There are ways you can reduce your pets risk for tick bites and Lyme disease. Regularly checking pets for all types of ticks, for instance, reduces the risk of infection for both pet and owner. Avoid allowing your dog to roam in tick-infested areas.
Topical, oral and/or collar products are also very important in preventing Lyme disease in dogs.
There are two basic types of Lyme disease vaccines available for dogs. Talk to your veterinarian to see if vaccination is appropriate for your dog. There is no vaccination for cats, which do not seem susceptible to Lyme disease.
What Is Lyme Disease
Lyme disease is an infectious disease caused by the bacteria Borrelia burgdorferi. B. burgdorferi is transmitted to humans by a bite from an infected black-legged or deer tick. The tick becomes infected after feeding on infected deer, birds, or mice.
A tick has to be present on the skin for at least 36 hours to transmit the infection. Many people with Lyme disease have no memory of a tick bite.
Lyme disease was first recognized in the town of Old Lyme, Connecticut, in 1975. Its the most common tickborne illness in Europe and the United States.
People who live or spend time in wooded areas known for transmission of the disease are more likely to get this illness. People with domesticated animals that visit wooded areas also have a higher risk of getting Lyme disease.
Recommended Reading: Can You Die From Lyme Disease
Two Standards Of Care For Lyme Disease Treatment
There is significant controversy in science, medicine, and public policy regarding Lyme disease. Two medical societies hold widely divergent views on the best approach to diagnosing and treating Lyme disease. The conflict makes it difficult for patients to be properly diagnosed and receive treatment.
One medical society, the Infectious Diseases Society of America , regards Lyme disease as hard to catch and easy to cure with a short course of antibiotics. IDSA claims that spirochetal infection cannot persist in the body after a short course of antibiotics. The group also denies the existence of chronic Lyme disease.
In contrast, the International Lyme and Associated Diseases Society , regards Lyme disease as often difficult to diagnose and treat, resulting in persistent infection in many patients. ILADS recommends individualized treatment based on the severity of symptoms, the presence of tick-borne coinfections and patient response to treatment.
LDo believes that patients and their doctors should make Lyme disease treatment decisions together. This requires that patients be given sufficient information about the risks and benefits of different treatment options. Then, patient and health care provider can collaborate to reach an informed decision, based on the patients circumstances, beliefs and preferences.