Who’s At Risk Of Lyme Disease
The risk of getting Lyme disease is higher:
- for people who spend time in woodland or moorland areas
- from March to October because more people take part in outdoor activities
It’s thought only a small proportion of ticks carry the bacteria that cause Lyme disease. Being bitten doesn’t mean you’ll definitely be infected. However, it’s important to be aware of the risk and speak to a GP if you start to feel unwell.
Moving Forward With Bartonella Research
In 2021, a new Bartonella Research Consortium was formed with a $4.8 million grant from The Steven & Alexandra Cohen Foundation.
The consortium includes Ed Breitschwerdt and Ricardo Maggi of North Carolina State University, Monica Embers of Tulane University, and Timothy Haystead of Duke University, who is continuing the work of the late Dr. Neal Spector.
The team is actively working towards creating a targeted treatment for bartonellosis and quickly getting the drug to the marketplace for use in both animals and humans.
Its time medicine moves beyond the one-pathogen-one-disease model. Lets face it, ticks are full of toxic soup. Because each pathogen interacts with the host in unique ways, extensive research is needed to understand all factors surrounding co-infections and Lyme disease.
Understanding the complex nature of these pathogens, how they impact the immune system, and how other bacterial and viral factors shape illness, will be key in improving public health.
Its time for the CDC, NIH, HHS, the Tick-Borne Disease Working Group and other researchers to start looking deeper into the prevalence of Bartonella infectionsnot just in patients with Lyme disease but in all patients with poorly-defined chronic illnesses.
Diagnosis Of Lyme Disease
Diagnosis is currently based on clinical findings supported by several types of laboratory tests. One type of test seeks to isolate the actual organism from the EM skin lesion, blood, joints, and cerebrospinal fluid. Other types of tests attempt to detect antibodies formed by the patients immune system against the organism. Currently, serology tests are poorly standardized and physicians must interpret them with caution. They are insensitive during the first several weeks of infection and may remain negative in people treated early with antibiotics. Test sensitivity increases when patients progress to later stages of the disease, but a small proportion of Lyme disease patients never develop a positive blood test result. Another complicating factor is that there can be a cross-reaction in the blood test, giving a false positive result for Lyme disease in persons who really have conditions such as syphilis, Rocky Mountain spotted fever, human immunodeficiency virus infection, infectious mononucleosis, lupus or rheumatoid arthritis. Although present diagnostics are not perfect, great strides have been made in the past twenty years. More sensitive and specific tests for Lyme disease are being developed.
Also Check: Can Lyme Disease Cause Spinal Stenosis
How Is Lyme Disease In Dogs Treated
Treatment for Lyme disease consists of at least 4 weeks of antibiotics. Your vet will prescribe these if your dog shows signs of Lyme disease or has a high level of antibodies, even without any symptoms.
A second round of antibiotics might be required if the infection persists, Richardson says.
In severe cases, further medical treatment of the kidneys, heart, or nerves may be needed, along with supportive care like intravenous fluids. To manage your pets pain, a veterinarian may prescribe NSAID pain relievers or steroids and restrict exercise.
Treatment For Lyme Disease Symptoms
Doctors say the sooner you notice symptoms, the better your outcome. People treated in the early stages of Lyme generally make a full, rapid recovery, the CDC notes.
Antibiotics are recommended for most people with Lyme disease, but what that regimen looks like varies widely from person to person. The National Institute of Allergy and Infectious Diseases says a short course of an oral antibiotic, such as doxycycline or amoxicillin, can clear up Lyme infection in most cases. However, the particular drug, dosage, and duration your doctor recommends may depend on factors such as:
- Whether you are pregnant
- Allergies to medications
Even after treatment, some people report lingering symptoms. They may have persistent pain, muscle and joint aches, unexplained numbness, and fatigue, for example. Brain fog and sleep disruption are also common, says Dr. Flanagan. These sputtering symptoms can stretch over a few months, he says, “but they will get better graduallyit can take time: two steps forward, one step back.”
Symptoms that persist for more than six months may lead to what the CDC calls post-treatment Lyme disease syndrome . The CDC says people with PTLDS can get better in time, but it can take months. Some doctors recommend prolonged antibiotic treatment. However, CDC cautions that long-term courses of antibiotics can actually be dangerous.
Recommended Reading: Can I Get Lyme Disease Twice
How Is Lyme Disease Diagnosed
Your doctor will examine you and ask you if youve been in an area where you may have been bitten by a tick before making a diagnosis.
You may have a blood test to confirm the diagnosis.
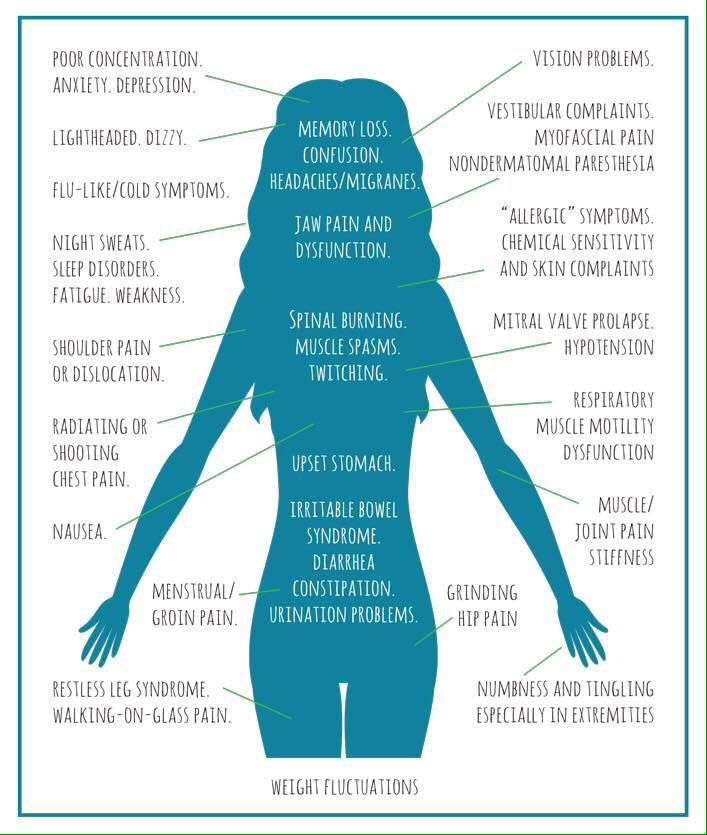
Stages Of Lyme Disease And Their Common Symptoms
If you have already been diagnosed with Lyme disease, learning about Lyme stages can help you know what symptoms you might experience. Youll also be able to watch for signs that could mean that your Lyme disease has progressed. Lyme disease symptoms are more likely to progress if you have not been appropriately treated.
If you dont have a Lyme disease diagnosis, its helpful to know that Lyme disease can cause a variety of seemingly unrelated symptoms throughout your body. If you develop symptoms listed below, especially after youve gotten a tick bite or spent time in an area where Lyme disease is common, you can ask your doctor whether you might have Lyme disease and if you should be tested for it. .
There are three stages of Lyme disease. Early localized, or Stage 1, Lyme disease occurs soon after being infected, when Lyme bacteria are still close to the site of the tick bite. Common symptoms of early localized Lyme disease include a rash or mild, flulike symptoms. Over time the Lyme bacteria can spread, or disseminate, to other parts of the body, causing more serious symptoms associated with early disseminated or late disseminated Lyme disease. This is more likely if you are not diagnosed and treated early.
Recommended Reading: Lyme Disease Joint Pain Symptoms
Can Lyme Disease Be Prevented
If youre travelling to an area where ticks are common, especially in spring or summer:
- wear long sleeves, long pants and long socks
- use insect repellent containing DEET
- check your body carefully and regularly
Remove ticks as soon as possible.
It is important to kill the tick first to prevent more saliva from being forced into the wound. Kill the tick with a product that quickly freezes it, such as a spray used to treat warts. Then gently remove it with tweezers when it is dead. This method will also lower your chances of developing an allergy to ticks. If you are allergic to ticks, you need the tick to be removed by a doctor.
Read more about preventing and treating insect bites.
Should Your Dog Get The Lyme Disease Vaccine
The goal of Lyme disease vaccination is to prevent the infection in dogs before any exposure to Borrelia burgdorferi. The vaccine includes a series of two shots, given 2 to 4 weeks apart, followed by annual boosters.
Consult with your veterinarian to determine if your dog needs the Lyme disease vaccination. Your vet may recommend the vaccine if you live in an area that is high risk or your dog is frequently involved in outdoor activities. Vaccination is often considered additional protection for dogs living in Lyme areas.
The vaccine is not 100% effective, however, and preventative measures are still important such as avoiding areas where ticks commonly live and checking your dog after walks, advises Richardson.
Read Also: Houses For Sale In Lyme Ct
Including Clinical Symptoms For The Diagnosis Of Lyme Disease
Laboratory testing for Lyme disease is known to have low sensitivity. Lyme specialty laboratories have improved testing methodologies to increase test sensitivity, but they still produce false-negative results. Furthermore, lab tests only provide objective information. Including subjective clinical symptoms improves the accuracy of diagnosis. For example, is there another significant lab result that explains the patients symptom picture?
An individualized approach is particularly significant when dealing with complex and poorly understood multisystem diseases. In opposition to this conservative and traditional approach , some have attempted to oversimplify the diagnosis of Lyme disease by reducing the diagnosis to reliance upon the U.S. CDC surveillance definition. However, the surveillance definition has never been intended to be a sole diagnostic criterion, particularly in late-stage disease.
Donât Miss: Medication For Lyme Disease In Dogs
Resources For Maine Residents
Public Law, Chapter 340, LD 597, 126th Maine State Legislature: An Act to Inform Persons of the Options for the Treatment of Lyme Disease
- Acknowledges difficulty in diagnosing and treating Lyme disease
- Information on risks of long term antibiotic therapy
Public Law, Chapter 235, LD 422, 127th Maine State Legislature: An Act to Improve Access to Treatments for Lyme Disease
- Allows licensed physicians to prescribe long-term antibiotic therapy to eliminate infection or to control a patients symptoms
You May Like: How To Test A Tick For Lyme
Signs And Symptoms Of Lyme Disease
We include products we think are useful for our readers. If you buy through links on this page, we may earn a small commission. Heres our process.
Overview
Lyme disease is an underreported, under-researched, and often debilitating disease transmitted by spirochete bacteria. The spiral-shaped bacteria, Borrelia burgdorferi, are transmitted by blacklegged deer ticks. Lymes wide range of symptoms mimic those of many other ailments, making it difficult to diagnose .
The blacklegged ticks can also transmit other disease-causing bacteria, viruses, and parasites. These are known as coinfections . These ticks that transmit Lyme are increasing their geographical spread. As of 2016, they were found in about half the counties in 43 of 50 states in the United States .
Lyme is the fifth most reported of notifiable diseases in the United States, with an estimated 329,000 new cases found annually . Some studies estimate that there are as many as 1 million cases of Lyme in the United States every year .
Most people with Lyme who are treated right away with three weeks of antibiotics have a good prognosis.
But if youre not treated for weeks, months, or even years after infection, Lyme becomes more difficult to treat. Within days of the bite, the bacteria can move to your central nervous system, muscles and joints, eyes, and heart .
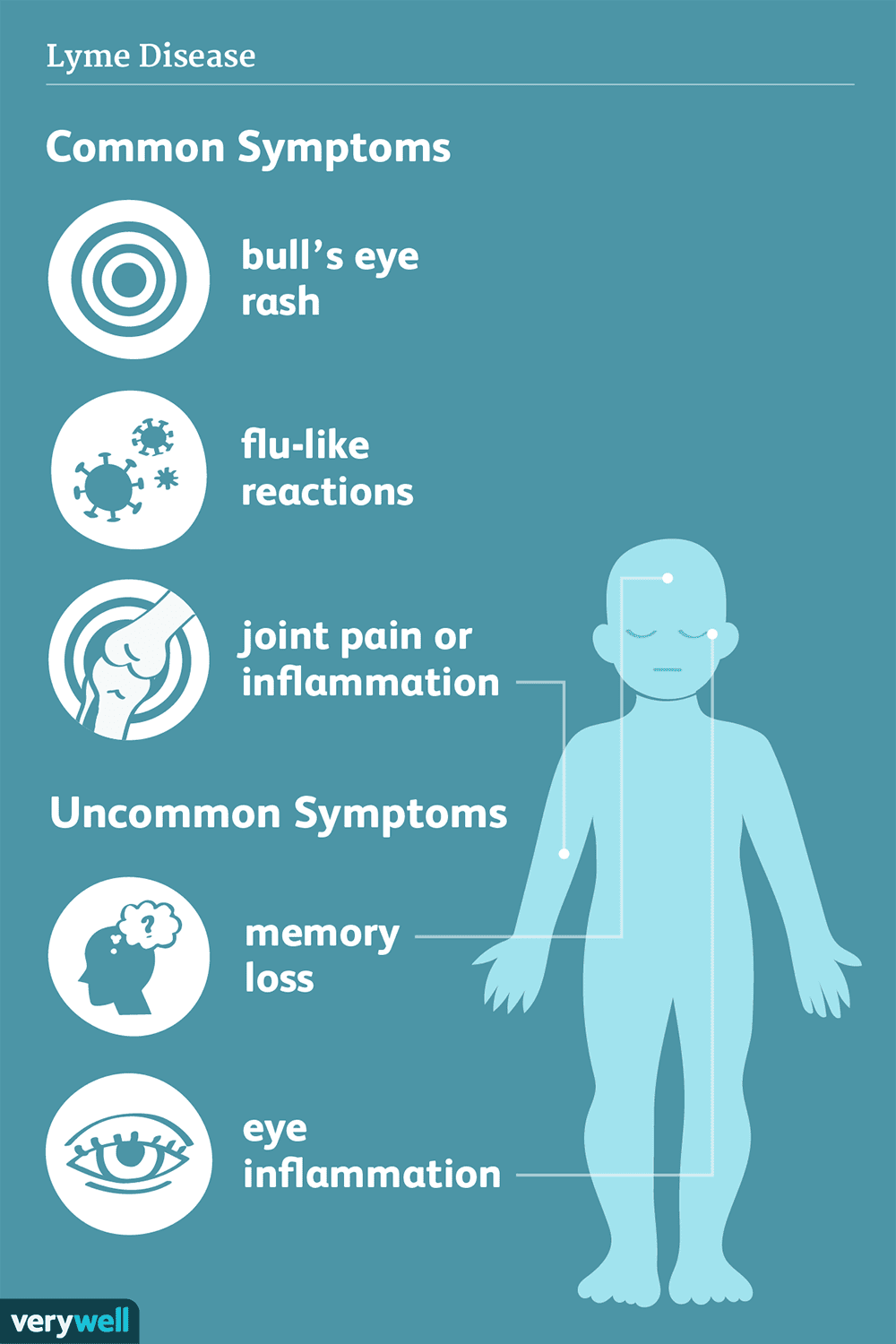
Here is a list of 13 common signs and symptoms of Lyme disease.
How Do Dogs Get Lyme Disease
Lyme disease is caused by the transmission of the bacterium Borrelia burgdorferi through a tick bite. The most common tick in the United States to transmit the disease is the deer tick, also known as the black-legged deer tick.
The deer tick that carry Lyme disease are most common in the following regions of the country:
-
Southern New England states, which include Massachusetts, Connecticut, and Rhode Island
-
Eastern mid-Atlantic states, which include New York, New Jersey, Pennsylvania, Delaware, Maryland, Virginia, West Virginia, and Washington, D.C.
-
Upper Midwest states, specifically in Wisconsin and Minnesota
-
West-coast areas, particularly northern California
The CDC provides a map of cases of Lyme disease throughout the years. You can look at cases in your state to better understand your dogs risk.
You May Like: What Is A Treatment For Lyme Disease
What You Need To Know About Lyme Disease
-
Lyme disease is an infection caused by the spiral-shaped bacteria Borrelia burgdorferi, which is most commonly transmitted by a tick bite.
-
There are over 300,000 estimated new cases of Lyme disease in the United States each year.
-
The symptoms of Lyme disease depend on the how long the infection has been present in the body. The first sign of Lyme disease is often an expanding round or oval red “bullseye” rash.
-
If left untreated, people may develop neurological symptoms and heart problems, and have an approximately 60 percent chance of developing Lyme arthritis.
How Prevalent Is Bartonella In People Who Have Lyme Disease
At a meeting of the federal Tick-Borne Disease Working Group on March 1, Ben Beard, PhD of the CDC made a highly significant statement that passed without remark at the time.
Beards statement was in reply to a comment by Monica Embers, PhD, also a member of the working group. Embers noted that several slides from Beards Clinical Presentation and Pathogenesis subcommittee mentioned neuropsychiatric illness and neuropathic manifestations of Lyme disease.
Were seeing a lot more neuropsychiatric disease associated with Bartonella, said Embers. Im wanting to hear more about your thought process and your recommendation with respect to bartonellosis?
Also Check: Can Lyme Disease Cause Lower Back Pain
Signs And Symptoms Of Untreated Lyme Disease
Seek medical attention if you observe any of these symptoms and have had a tick bite, live in an area known for Lyme disease, or have recently traveled to an area where Lyme disease occurs.
Untreated Lyme disease can produce a wide range of symptoms, depending on the stage of infection. These include fever, rash, facial paralysis, and arthritis.
The appearance of the erythema migrans rash can vary widely.
- Fever, chills, headache, fatigue, muscle and joint aches, and swollen lymph nodes may occur in the absence of rash
- Erythema migrans rash :
- Occurs in approximately 70 to 80 percent of infected persons
- Begins at the site of a tick bite after a delay of 3 to 30 days
- Expands gradually over several days reaching up to 12 inches or more across
- May feel warm to the touch but is rarely itchy or painful
- Sometimes clears as it enlarges, resulting in a target or bulls-eye appearance
- May appear on any area of the body
- Does not always appear as a classic erythema migrans rash
Swollen Knee
- Severe headaches and neck stiffness
- Additional EM rashes on other areas of the body
- Arthritis with severe joint pain and swelling, particularly the knees and other large joints.
- Intermittent pain in tendons, muscles, joints, and bones
- Heart palpitations or an irregular heart beat
- Episodes of dizziness or shortness of breath
- Inflammation of the brain and spinal cord
Links with this icon indicate that you are leaving the CDC website.
Lyme Disease In Missouri
The first question to ask is, Does Lyme disease occur in Missouri? There have been patients with symptoms similar to those in other areas of the United States, but B. burgdorferi has not yet been isolated from any patients in Missouri. Lyme disease is nationally notifiable and is therefore notifiable in Missouri. Missouri patients who fulfill the strict CDC case definition for Lyme disease are reported as such. Because the EM rashes of Missouri origin are similar to those in other parts of the country, they are referred to as EM-like by the Division of Vector-Borne Infectious Diseases, National Center for Infectious Diseases, CDC. The clinical syndrome associated with the EM-like rash appears similar to Lyme disease and is called Lyme-like disease.
The uncertainty regarding the occurrence of Lyme disease is not unique to Missouri . Determining the geographic distribution and prevalence of a disease-causing agent is always challenging, particularly when the agent is a relatively recently identified one. This problem is compounded many fold, when one realizes that it is not only the distribution and prevalence of the agent that must be considered, but also that of possible reservoirs and vectors that maintain and transmit the agent. All of these factors must come together at the same place and time before disease can be caused in a host.
You May Like: My Dog Tested Positive For Lyme Disease
Stage : Small Oval Rashes Or A Reddish Lump
When a tick that causes Lyme disease bites you, it infects you with bacteria. Without treatment, the bacteria can spread to other areas of your body. Stage 2 begins when the bacteria spread to other parts of your body.
During this stage, you may see small, oval rashes on your skin. Some people develop a bluish-red lump.
Where you see these signs: Because the infection has spread, small rashes can appear anywhere on your skin, except for your palms and soles. Most rashes appear on the arms, legs, and face.
Some people develop a lump, which your doctor may refer to as borrelial lymphocytoma. In children, this lump tends to appear on an earlobe. Adults often see a raised growth form around a nipple.
Borrelial lymphocytoma on a childs ear
This can appear in stage 2 of Lyme disease.
What you may see on your skin: The rashes that appear during stage 2 differ from the rash that can appear in stage 1. In stage 2, the rashes stay the same size rather than grow larger.
When the rashes, lump, and symptoms begin: About 30 to 45 days after the tick bites you, you may notice rashes or a lump. These can also take longer to appear, sometimes six months or more.
Some people develop symptoms, which make them feel ill, including:
-
Shortness of breath and dizzy spells
-
Bells palsy, which causes one half of the face to droop
-
Heart problems, such as chest pains or an irregular heartbeat
Stage : Later Symptoms
- shooting pains, numbness or tingling in the hands or feet
- heart palpitations
These symptoms may go away without treatment within a few weeks or months. However, some people develop chronic Lyme disease and have lasting symptoms.
Around of people who do not receive treatment for the disease develop recurrent episodes of arthritis with severe swelling, especially in the large joints.
Also Check: Late Stage Lyme Disease Symptoms