Why Choose Hope Brain & Body Recovery Center For Treatment
When seeking treatment for neurological conditions, you shouldnt settle for anything but the most premium treatment. Dr. Joseph Schneider has over 30 years of clinical experience and has attended to over 11,000 patients with a wide array of neurological conditions.
Dr. Schneider has firsthand experience with neurological treatment, having suffered a stroke in 2017. Thanks to his incredibly talented associates and personal knowledge of treatment methods, has made a miraculous recovery. He has devoted his life to the neurological health of his patients and uses his firsthand experience of the recovery process to improve the treatment methods used at Hope Brain & Body Recovery Center.
Choosing Hope Brain & Body Recovery Center gives you access to some of the most modern technical treatment equipment available. We utilize a wide range of modern diagnostic equipment that helps our specialists build some of the most comprehensive neurological profiles for our patients. This means we are able to offer more accurate diagnoses, discover underlying conditions, as well as use the information to create therapy plans that are uniquely designed for each patient.
Who Is At Risk For Lyme Disease
Anyone can get a tick bite. But people who spend lots of time outdoors in wooded, grassy areas are at a higher risk. This includes campers, hikers, and people who work in gardens and parks.
Most tick bites happen in the summer months when ticks are most active and people spend more time outdoors. But you can get bitten in the warmer months of early fall, or even late winter if temperatures are unusually high. And if there is a mild winter, ticks may come out earlier than usual.
Understanding Neurologic Lyme Disease
Lyme disease is a condition that is carried by infected black-legged deer ticks. These ticks are usually found in wooded areas with tall grass. Ticks intended targets are deer and other woodland animals, but will just as easily attach themselves to hikers, hunters, and unsuspecting adventurers. Lyme disease cases are consistently on the rise and the CDC estimates that the current numbers, around 300,000 cases every year, are dramatically underreported.
Dr. Joseph Schneider, DC, DACNB head neurologist at the Hope Brain and Body Recovery Center utilizes state-of-the-art treatment methods and expertise to help patients suffering from Neurologic Lyme Disease. Our team understands how much of a burden Lyme Disease can be and want to help you manage your symptoms and restore your quality of life.
You May Like: How Soon Should You Treat Lyme Disease
Making Connections To Clarify Diagnosis
Chronic Lyme disease shares many symptoms with other chronic illnesses. This is especially true of LNB and chronic neuroinflammatory illnesses such as multiple sclerosis, Alzheimers disease, amyotrophic lateral sclerosis , Parkinsons disease, and traumatic brain injury .
Not surprisingly, new sophisticated methods of microbial detection are showing potential links between these neuroinflammatory illnesses and many of the microbes associated with chronic Lyme disease.
For instance, both Mycoplasma and Chlamydia have been closely linked to multiple sclerosis. Mycoplasma, Borrelia, and Chlamydia have been associated with demyelination. Parkinsons and ALS have been linked to Borrelia and other microbes commonly associated with Lyme disease. Borrelia and other stealth pathogens have been found in the brains of patients who died of Alzheimers disease.
But the connections go well beyond Lyme disease microbes. Two studies shed some light on how closely disruptions in the microbiome are linked to neuroinflammation. One, published in Frontiers of Aging Neuroscience, evaluated the presence of microbes in the autopsied brains of deceased Alzheimers patients. The other, published in Scientific Reports, evaluated the presence of microbes in the autopsied brains of people who had died of multiple sclerosis.
Ultimately, the type of illness a person might end up with depends on three key things:
What Is Chronic Neurological Lyme Disease
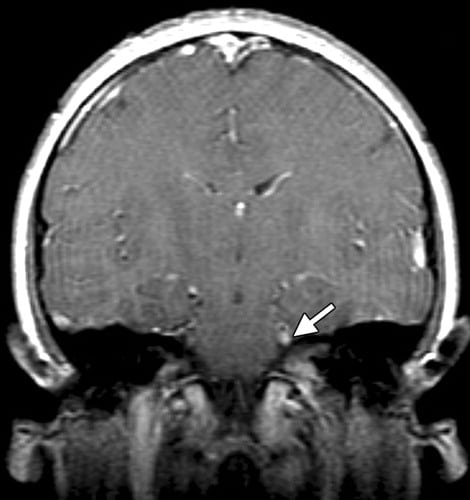
3.4.1 Overview
In most patients with Lyme neuroborreliosis the suspected clinical diagnosis can be confirmed by detecting Borrelia-specific intrathecal antibody synthesis related to inflammatory changes in their cerebrospinal fluid , , , . The production of specific intrathecal antibodies is detected by determining the Borrelia-specific CSF/serum antibody index , , .
3.4.2 Determination method
Methods used to determine the AI should take into account the blood/CSF barrier function, as otherwise false negative results may be produced . The determination of the antibody index according to Reiber is a proven method that is recommended , , , . The following formula is used to calculate the Borrelia-specific AI : Antibody index =
If intrathecal immunoglobulin synthesis is present in the Reiber diagram , the total IgG ratio must be replaced by the Q-Lim ratio . In this case: Antibody index =
A value of =1.5 is recommended as the cut-off for a positive AI, unless otherwise evaluated , , , previously recommended higher limit values of 2.0 are considered less sensitive when a reliable test performance can be ensured . Quantitative measuring methods are usually used to determine the AI and are implemented in commercial, EDP-supported systems .
It is important to note that there can be considerable fluctuations in the determination of AI . Hence antibody testing and AI determination should be conducted in accredited microbiology laboratories.
Summary
Read Also: Symptoms Of Lyme Flare Up
Get Tested And Treated Early
Studies acknowledge that up to 30% of patients go on to suffer further Lyme symptoms even after treatment, sometimes called Post-Treatment Lyme Disease Syndrome . One of the biggest risk factors for this condition is delayed treatment.
Research is finally, if slowly, catching up to the reality that letting Lyme disease slip through the cracks of insufficient diagnostic testing causes real suffering for patients. IGeneX is at the forefront of solving this problem, offering more sensitive and accurate testing for Lyme disease and other tick-borne diseases that can cause mental health problems when left untreated. Learn more today.
Pots Constipation And Lyme Disease
POTS stands for postural orthostatic tachycardia syndrome which means the heart rate will increase when someone changes position, from laying or sitting to standing. POTS is very common in late-stage Lyme disease since the autonomic nervous system does not maintain tone in blood vessels causing a drop in blood pressure. When the blood pressure drops, the heart rate has to increase to stabilize blood pressure. Mast cell activation syndrome is another common cause of POTS and MCAS is frequently seen as a consequence of Lyme disease.
Another common symptom associated with autonomic nervous system dysfunction is constipation. Termed gastroparesis, constipation can happen when the nerve that signals intestinal muscular contraction become damaged by the bacteria and the resulting immune response.
Read Also: Bpc 157 For Lyme Disease
The Effects Of Lyme Disease On The Nervous System
A limping dancer, a student forced to the bench.
According to Dr. Erik Kolbenheyer, an internist, gastroenterologist, family doctor, occupational health specialist, doctor of traditional Chinese medicine, there are some particularly interesting cases of Lyme borreliosis, where the disease causes bizarre symptoms in the nervous system. The doctor, who, being personally affected by the disease, turns to his patients with excellent diagnostic sense and great empathy, presents two shocking cases from his own practice when young people became ill but fortunately, their quality of life essentially returned to its previous level.
In cases where the bacteria attack the nervous system, anxiety, depression, panic attacks, and strange movement disorders may appear. It is a very complex set of symptoms, so in these cases, the help of a neurologist is needed to examine the patient in other directions. As the symptoms of the nervous system can take on quite unusual forms, patients and relatives might panic.
You May Like: Where Can I Get Lyme Disease Test
Neurological And Psychiatric Issues Associated With Lyme Disease And Tbrf
Chronic illness often has significant impacts on mental health, and Lyme disease is no different. With the accuracy and sensitivity of todays recommended Lyme testing still so lacking, many Lyme patients have to wait too long to get accurate diagnoses and treatment. To compound this problem, many patients with Lyme-like symptoms are not even tested for the similar, but biologically distinct, Tick-Borne Relapsing Fever . That gives infections time to spread throughout the body and cause neurological and psychiatric symptoms.
This article will outline the direct and indirect effects that Borreliosis both Lyme disease and TBRF can have on mental health, including how and why untreated Lyme can develop into neurological Lyme disease.
Don’t Miss: Best Diet For Lyme Disease Patients
Texas A& m Research Aims To Improve Lyme Disease Diagnostics
Research by two Texas A& M University scientists is focused on improving Lyme disease treatment outcomes by developing a test that’s both more accurate and more efficient than the current test for the infection.
Lyme disease, the fastest growing vector-borne illness in the U.S., according to the Bay Area Lyme Foundation, is challenging to diagnose and can only be treated in the early stages of infection. Once the infection spreads to the nervous and muscular systems, it is both harder to detect and less susceptible to antibiotics.
Dr. Artem Rogovskyy, an associate professor at the Texas A& M School of Veterinary Medicine & Biomedical Sciences , and Dr. Dmitry Kurouski, an assistant professor in the Texas A& M Department of Biochemistry & Biophysics and the Department of Biomedical Engineering, are testing Raman spectroscopy, a technique used to detect vibrations at the molecular level, as a diagnostic tool for Lyme disease.
The results of Rogovskyy and Kurouski’s second paper on Raman spectroscopy as a diagnostic tool for Lyme disease demonstrate that blood samples from mice and humans infected with the Lyme pathogen were more accurately identified with the Raman spectroscopy test than with the two-tiered serology, the only diagnostic method currently approved to diagnose Lyme disease in humans in the United States.
More information:Frontiers in Cellular and Infection Microbiology
What Is Lyme Disease
Lyme disease is a bacterial infection you get from the bite of an infected tick. At first, Lyme disease usually causes symptoms such as a rash, fever, headache, and fatigue. But if it is not treated early, the infection can spread to your joints, heart, and nervous system. Prompt treatment can help you recover quickly.
Recommended Reading: Is There A Home Test For Lyme Disease
Treatment For Neurological Lyme Disease
After defining the problem, she moves on to solutions. The next section deals with pharmaceutical approaches to Lyme disease in the brain, including an explanation of the blood-brain barrier and what drugs can effectively penetrate it. She discusses medications that reduce inflammation, as well as those to stabilize neurological function, balance mood and help people think more clearly.
Section 3 discusses natural approaches to Lyme disease in the brain: antimicrobials, such as Cats Claw and teasel root anti-inflammatories, such as curcumin and stephania root antioxidants, such as glutathione neurotransmitter support and essential oils such as peppermint and frankincense.
Section 4 deals with nutrition. Readers of her earlier book, The Lyme Diet, will find familiar themes: avoid gluten, dairy, sugar, caffeine, alcohol and additives such as MSG.
Ducharme explains about therapies to help the brain, including neurofeedback, Brainwave Entrainment, and hyperbaric oxygen. She covers sleep and exercise. She reviews different kinds of psychotherapy for patients with Lyme brain.
Understanding Symptoms Of Neurological Lyme
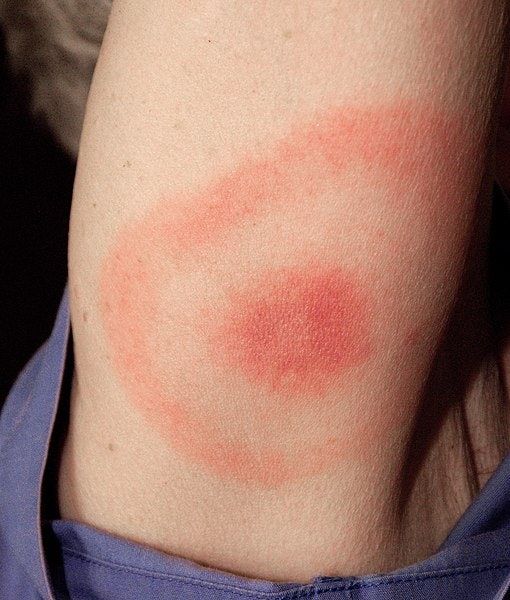
LNB is thought to occur in about 15% of Lyme disease cases, according to research in Frontiers in Neurology but a definite percentage is impossible to pin down. The majority of people with Lyme disease experience some form of neurological symptoms, but a specific composite of symptoms that constitute neurological Lyme is not well defined. Making matters worse, the Centers for Disease Control and Prevention , does not recognize LNB as a separate entity, and it doesnt acknowledge the existence of a chronic or persistent form of Lyme disease.
Studies suggest that the most common symptom of LNB is facial nerve palsy , which is characterized by temporary paralysis on one side of the face. Some people also experience sound sensitivity and discomfort in the ear on the paralyzed side, and if youre unable to close that eye, dry eye can occur. Most people eventually recover fully from Bells palsy, with improvement in the first few weeks and continuing for three to six months, but a subset of people may develop lifelong symptoms.
Another common symptom of LNB is neurogenic pain that starts in the back and radiates down the legs. With that comes weakness, numbness, and tingling in the lower extremities. For most people, symptoms begin resolving within the first few weeks after starting treatment, however, others may have pain that lasts for months or years.
Read Also: Lyme Disease What Is It
How To Recover From Neurological Lyme
When youre suffering from debilitating symptoms of neurological Lyme, its tempting to seek out medications that promise fast relief. But the place for drug therapy in chronic, neuroinflammatory illnesses isnt clear-cut. In fact, because neuroinflammation is so complex, targeted synthetic drug therapy may hinder the healing process.
Many medications suppress or disrupt immune system functions and inhibit deep sleep, which is absolutely essential for recovery. Anti-inflammatory drugs, including steroids and nonsteroidal anti-inflammatory agents like ibuprofen and naproxen, are examples of medications with the capacity to dampen the immune system and impede healing.
These drugs have also been shown to impede clearance of beta amyloid, a proteinaceous substance associated with neuroinflammatory disorders that is the hallmark identifying factor of Alzheimers disease. Though short-term use of antibiotic therapy has shown benefit in some cases of dementia and MS, tolerance to therapy and relapse are likely with long-term use of synthetic antibiotics.
This makes sense when you consider that LNB and other neuroinflammatory conditions are primarily associated with chronic immune dysfunction as opposed to infection with specific pathogens.
So while antibiotics initially suppress microbes, with extended use, pathogens arise in the gut and skin. The gut and brain barriers become more compromised, and immune functions are further depressed, thus enhancing neurological symptoms.
Neurological Complications Of Rheumatologic Conditions
Systemic lupus erythematosis , rheumatoid arthritis, Sjogren syndrome, and mixed connective tissue disease are a few of the rheumatologic conditions that can affect the nervous system, and they can do so in a variety of ways. Additionally, many parts of the nervous system can be involved, from the muscle to the peripheral nerve all the way to the cerebral cortex. For instance, some patients can have abnormal blood clotting as a complication of SLE, which can affect the brain. Additionally, these conditions may place patients at risk for opportunistic infections, as mentioned above, usually due to the longstanding immune therapy required to treat these diseases.
Read Also: Justin Bieber Lyme Disease Treatment
Cerebrospinal Fluid Analyses And Antibody Response
CSF analysis was performed in all patients . All but one patient showed elevated CSF cell counts. Total protein was increased in 58 patients . The albumin CSF-serum concentration quotient is generally considered as the best indicator for a blood-CSF barrier dysfunction . Measurements of QAlb revealed age-corrected increased values in 59 patients . Barrier impairment was severe in 26 patients and mild to moderate in the others. Only 8 patients presented CSF lactate concentrations > 3.5 mmol/l. 17 patients showed values within a range of 2.6-3.5 mmol/l, while the remaining patients presented CSF lactate concentrations < 2.6 mmol/l.
Table 2
Oligoclonal bands restricted to the CSF were found in 61 patients indicating intrathecal IgG synthesis. Five of these patients showed a combination of oligoclonal bands restricted to the CSF and identical oligoclonal IgG bands in CSF and serum .
When oligoclonal bands were included as a sign of intrathecal IgG synthesis a combined three-class reaction of immunoglobulins was then found in 19 patients . Two-class reactions with the combinations of IgM+IgG in 31 patients and IgA+IgG in 3 patients were detected. Isolated IgG synthesis was found in 9 patients . A two-class reaction of IgM+IgA as well as isolated IgM and isolated IgA synthesis did not occur.
Neurological Lyme Disease: What You Need To Know + Natural Solutions For Recovery
Lyme disease can manifest in a seemingly endless number of ways. While the spectrum of symptoms is similar for many people, the worst of the bunch varies from one person to the next. And for those who have a predominance of neurological symptoms, the disease can feel especially debilitating and difficult to overcome.
Thats in large part because neurological Lyme also referred to as Lyme neuroborreliosis is often confused with other serious neurological conditions such as multiple sclerosis and Parkinsons disease, which can be scary and overwhelming. And because most doctors lack an understanding of Lyme disease in general, and especially of Lyme associated with a predominance of neurological symptoms, LNB often goes unrecognized.
So how can you tell if the symptoms youre experiencing do signify LNB? Moreover, where do you go from there to find relief? Keep reading for information that could provide the turning point in your recovery.
Recommended Reading: Heat Treatment For Lyme Disease
Neurological Symptoms From Late
If Lyme disease or associated infections are not adequately treated or go untreated, the persistence of the bacteria, and the inflammation from the immune response, can affect nerve function leading to a myriad of neurological symptoms. One study indicated it took an average of a year and a half following a tick bite for symptoms to manifest in the peripheral nervous system and two years to the onset of symptoms in the central nervous system . The significant length of time from bacterial exposure to onset of symptoms creates a challenge in associating Lyme disease as the cause of chronic neurological symptoms.
Neuropathy is a general term for disease of the nerves.
Polyneuropathy refers to multiple nerves involved in the pathology. In late-stage Lyme disease, polyneuropathy typically manifests as numbness, tingling or burning and can include any nerve but most commonly begins in the hands/arms and feet/legs. Less frequently, chronic neuropathy can lead to radicular pain.
Encephalopathy refers to generalized brain dysfunction