What To Do If You Have A Blacklegged Tick Bite
Remove the tick by pulling it directly out with fine-tipped tweezers. Lift upward with slow and even pressure. Dont twist when removing it. Dont crush it or put soap or other substances on it. Dont apply heat to it.
Place the tick in a resealable container. See if you can identify what kind of a tick it is.
Immediately after removing the tick, wash your skin well with soap and water or with rubbing alcohol.
Not all ticks carry Lyme. The Lyme bacteria is transmitted only by blacklegged ticks in their nymph or adult stage.
Save the tick to show your doctor. The doctor will want to determine if its a blacklegged tick and if theres evidence of feeding. Ticks enlarge as they feed. Your risk of getting Lyme from an infected tick increases with the length of time that the tick fed on your blood.
Summary:
Pull the tick out with tweezers and save it in a resealable container for identification.
Stage : Early Localized Disease
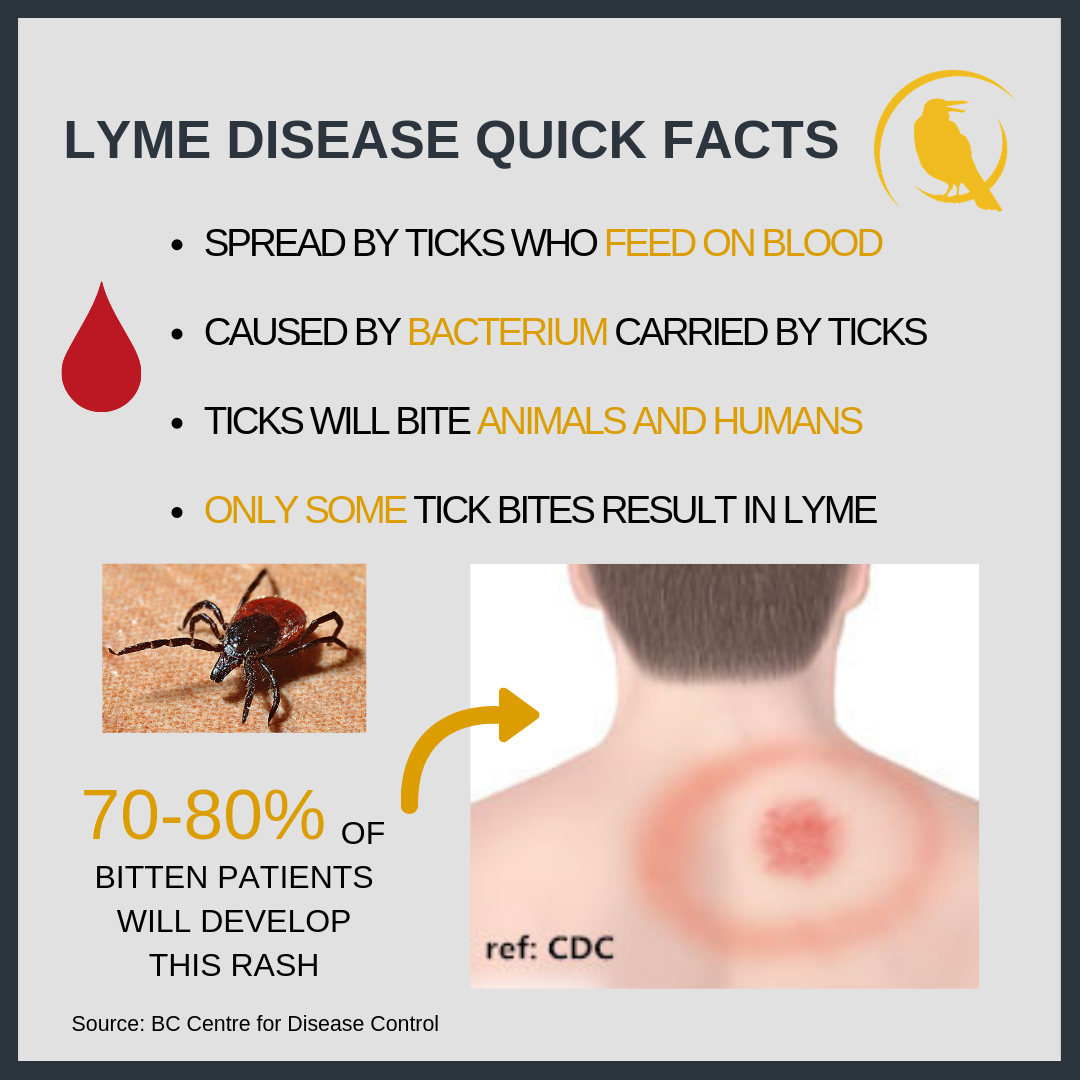
Symptoms of Lyme disease usually start 3 to 30 days after the tick bite. One of the earliest signs of the disease is a bulls-eye rash.
The rash occurs at the site of the tick bite, usually, but not always, as a central red spot surrounded by a clear spot with an area of redness at the edge. It may be warm to the touch, but its not painful and doesnt itch. This rash will gradually fade in most people.
The formal name for this rash is erythema migrans.
Some people with lighter skin have a rash thats solid red. Some people with darker skin may have a rash that resembles a bruise.
The rash can occur with or without systemic viral or flu-like symptoms.
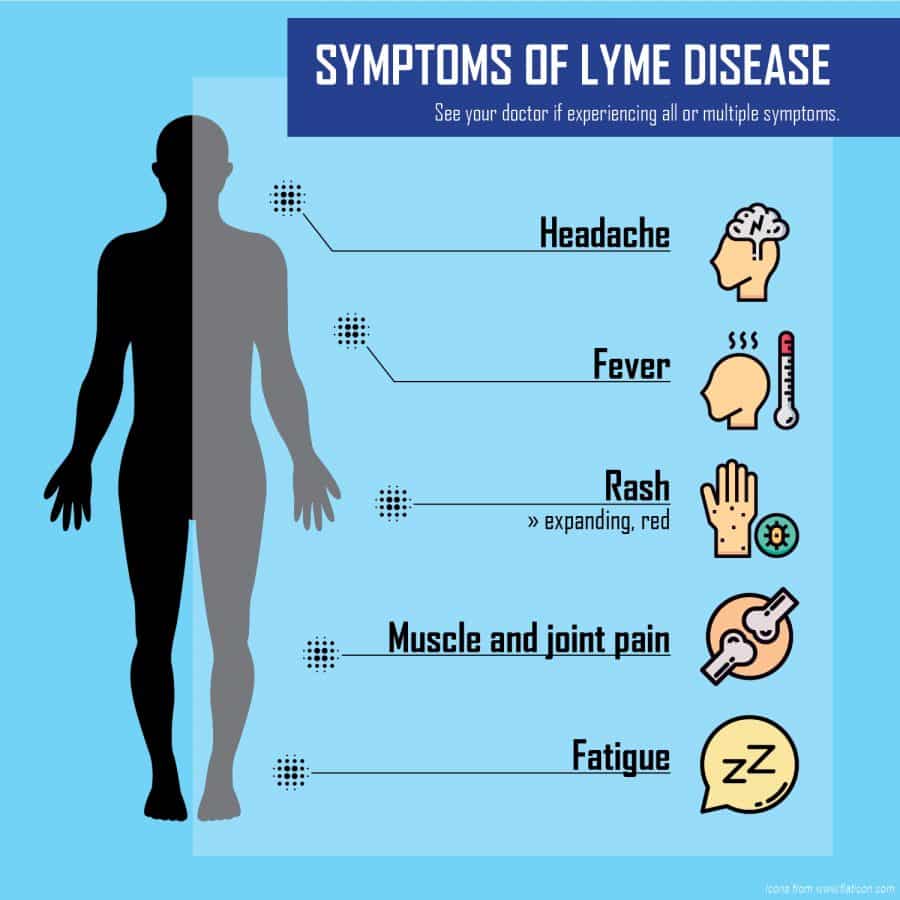
Other symptoms commonly seen in this stage of Lyme disease include:
Youll have a general feeling of being unwell. A rash may appear in areas other than the tick bite.
This stage of the disease is primarily characterized by evidence of systemic infection, which means infection has spread throughout the body, including to other organs.
Symptoms can include:
- disturbances in heart rhythm, which can be caused by Lyme carditis
- neurologic conditions, such as numbness, tingling, facial and cranial nerve palsies, and meningitis
The symptoms of stages 1 and 2 can overlap.
How To Remove Ticks
Tick bites aren’t always painful. You may not notice a tick unless you see it on your skin. Check your skin and your children’s or pets’ skin after being outdoors.
To remove a tick:
The risk of getting ill is low. You don’t need to do anything else unless you become unwell.
Don’t Miss: Can Dogs Get Rid Of Lyme Disease
Knowing Important Lyme Disease Facts
Treatment For Lyme Disease
Treatment for Lyme disease is usually done with a 2-3 week course of antibiotics and is generally very effective, especially when treatment is done early in the course of the illness. If you think you have symptoms caused by a deer tick bite you can get care quickly and virtually by contacting your doctor or through Everyday Online.
A short, one-day antibiotic treatment might be called for to prevent Lyme disease after a deer tick bite if several criteria are met:
- The tick is identified as a blacklegged tick
- The tick was attached for at least 36 hours. If the tick you pulled off is engorged or puffed up with blood, then it was probably on this length of time.
- The treatment is started less than 72 hours after finding the attached tick.
- The treatment is only for adults and children 8 years or older.
Find more information about Lyme disease and other illnesses caused by deer ticks by visiting the Minnesota Department of Health website or the CDC website.
Also Check: Treating Lyme Disease With Essential Oils
How Are Dogs Tested For Lyme Disease
Diagnosis is made by a combination of history, physical signs, and diagnostics. For dogs, the two blood tests for diagnosing Lyme disease are called the C6 Test and Quant C6 test. Veterinarians perform both.
The C6 test detects antibodies against a protein called C6. Presence of the antibodies suggests an active Lyme infection. The C6 antibodies can be detected three to five weeks after an infected tick bites a dog and may be found in the bloodstream even before the dog shows signs of illness.
The next step is to do a Quant C6 test. This, along with urinalysis will help determine if antibiotic treatment is necessary.
Who’s At Risk Of Lyme Disease
The risk of getting Lyme disease is higher:
- for people who spend time in woodland or moorland areas
- from March to October because more people take part in outdoor activities
It’s thought only a small proportion of ticks carry the bacteria that cause Lyme disease. Being bitten doesn’t mean you’ll definitely be infected. However, it’s important to be aware of the risk and speak to a GP if you start to feel unwell.
Recommended Reading: The Side Effects Of Lyme Disease
Who Gets Lyme Disease
Anyone bitten by an infected deer tick can get Lyme disease. Most U.S. cases of Lyme disease happen in Connecticut, Delaware, Maine, Maryland, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, and Wisconsin. But Lyme disease is also found in other parts of the U.S., Europe, and Asia.
Other things that might increase a person’s risk include:
- spending a lot of time outdoors in tall grass, brush, shrubs, or wooded areas
- having pets that may carry ticks indoors
- activities such as yardwork, hiking, camping, fishing, or hunting in tick-infested areas
Later Signs And Symptoms
- Severe headaches and neck stiffness
- Additional EM rashes on other areas of the body
- Arthritis with severe joint pain and swelling, particularly the knees and other large joints.
- Intermittent pain in tendons, muscles, joints, and bones
- Heart palpitations or an irregular heart beat
- Episodes of dizziness or shortness of breath
- Inflammation of the brain and spinal cord
You May Like: First Signs Of Lyme Disease In Dogs
Lyme Disease Rashes And Look
Circular, expanding rash with target-like appearance.
Expanding rash with central crust
Expanding lesion with central crust on chest.
Expanding erythema migrans
Photo Credit: Reprinted from Bhate C, Schwartz RA. Lyme disease: Part I. Advances and perspectivesexternal icon. J Am Acad Dermatol 2011 64:619-36, with permission from Elsevier.
Description:Early, expanding erythema migrans with nodule.
Multiple rashes, disseminated infection
Early disseminated Lyme disease multiple lesions with dusky centers.
Red, oval plaque
Red, expanding oval-shaped plaque on trunk.
Expanding rash with central clearing
Circular, expanding rash with central clearing.
Bluish hued rash, no central clearing
Bluish hued without central clearing.
Expanding lesion, no central clearing
Expanding lesion without central clearing on back of knee.
Red-blue lesion with central clearing
Red-blue lesion with some central clearing on back of knee.
Insect bite hyper-sensitivity
Large itchy rash caused by an allergic reaction to an insect bite.
Fixed drug reaction
Description:A skin condition that occurs up to two weeks after a person takes a medication. The skin condition reappears at the same location every time a person takes that particular medication.
Ringworm
Description:Ringworm is a common skin infection that is caused by a fungus. Its called ringworm because it can cause a ring-shaped rash that is usually red and itchy with raised edges.
Pityriasis rosea rash
Granuloma annulare rash
Ongoing Symptoms Of Lyme Disease
A few people who are diagnosed and treated for Lyme disease continue to have symptoms, like tiredness, aches and loss of energy, that can last for years.
These symptoms are often compared to fibromyalgia and chronic fatigue syndrome.
It’s not clear why this happens to some people and not others. This means there’s also no agreed treatment.
Speak to a doctor if your symptoms come back, or do not improve, after treatment with antibiotics.
The doctor may be able to offer you further support if needed, such as:
- referral for a care needs assessment
- telling your employer, school or higher education institution that you require a gradual return to activities
- communicating with children and families’ social care
Page last reviewed: 05 July 2021 Next review due: 05 July 2024
Recommended Reading: Post Treatment Lyme Disease Syndrome Mayo Clinic
Lyme Disease: Signs And Symptoms
This publication is licensed under the terms of the Open Government Licence v3.0 except where otherwise stated. To view this licence, visit nationalarchives.gov.uk/doc/open-government-licence/version/3 or write to the Information Policy Team, The National Archives, Kew, London TW9 4DU, or email: .
Where we have identified any third party copyright information you will need to obtain permission from the copyright holders concerned.
This publication is available at https://www.gov.uk/government/publications/lyme-disease-signs-and-symptoms/lyme-disease-signs-and-symptoms
How You Get Lyme Disease
Lyme disease can be transmitted by the bite of a tick infected with Borrelia burgdorferi bacteria.
Ticks survive in many habitats but prefer moist areas with leaf litter or longer grass, like in woodland, grassland, moorland, heathland and some urban parks and gardens.
Ticks dont jump or fly but climb on to your clothes or skin if you brush past vegetation.
They then bite into the skin and start to feed on your blood. Being bitten doesnt mean youll definitely be infected as not all ticks carry the bacteria that cause Lyme disease.
If bitten by an infected tick, you are more likely to become infected the longer the tick remains attached and feeding.
Ticks are very small and their bites are not painful, so you may not realise you have one attached to your skin. It is important to check yourself for ticks after outdoor activities and remove any ticks promptly and safely.
Recommended Reading: Hyperbaric Chamber Treatment For Lyme Disease
How To Spot A Tick Bite
Every year, I see patients who are diagnosed with Lyme disease and other tick-borne illnesses. Many of them dont recall being bitten by a deer tick as they are quite small, especially in the nymph or juvenile stage. Wood ticks are larger than deer ticks and do not cause Lyme disease or other tick related illnesses. It takes at least 24 hours for an attached deer tick to transmit the Lyme disease bacteria. If you spend time outdoors in tick habitat, my advice is to do a daily, full-body tick check.
Ways You Can Prevent A Tick Bite
If you spend time outdoors its important to know how to spot a tick bite, learn to safely remove a tick, and when to seek medical care for Lyme disease or other tick-borne illnesses. Peak tick season runs from May to October and if you spend any time outdoors, its wise to know how to spot a tick bite, know how to remove a tick safely, and when to seek medical care.
- Treat your clothing and outdoor gear with 0.5 percent permethrin.
- Use a tick repellent with at least 20 percent DEET.
- Walk in the center of marked trails.
- Wear a long-sleeved shirt and pants when outdoors.
To learn more about tick prevention, head to 7 tips to keep you tick-free.
Recommended Reading: Can Lyme Disease Cause Dizziness
Who Is At Risk For Lyme Disease
Anyone can get a tick bite. But people who spend lots of time outdoors in wooded, grassy areas are at a higher risk. This includes campers, hikers, and people who work in gardens and parks.
Most tick bites happen in the summer months when ticks are most active and people spend more time outdoors. But you can get bitten in the warmer months of early fall, or even late winter if temperatures are unusually high. And if there is a mild winter, ticks may come out earlier than usual.
Is There A Blood Test For Lyme Disease
If your doctor suspects that you have Lyme disease, they may order two blood tests. These will look for signs that your body is trying to fight it off. The results are most precise a few weeks after youâve been infected.
These tests are:
ELISA test. This test canât check for the bacteria that causes Lyme disease. It can only look for your immune systemâs response to it.
Once Borrelia burgdorferi gets into your blood, your body begins to make special proteins called antibodies to fight it off. The ELISA test checks for those antibodies.
Although itâs the most common way to check for Lyme disease, the ELISA test isnât perfect. It can sometimes give false âpositiveâ results. On the other hand, if you have it done too soon after youâve been infected, your body may not have developed enough antibodies for the test to detect them. This will give you a ânegativeâ result even though you do have Lyme disease.
Western blot test. Whether your ELISA test comes back positive or negative, your doctor will need to do this blood test, too.
A Western blot uses electricity to split certain proteins in your blood into patterns. This is then compared to the pattern of people known to have Lyme disease.
At least five band matches means that you have Lyme disease. Still, not all labs have the same standards. Thereâs a chance that you could get a âpositiveâ result from one and a ânegativeâ result from another.
- Alzheimerâs disease
Read Also: Can You Get Lyme Disease From Mosquitoes
Preventive Antibiotics After A Tick Bite
According to guidelines from the Infectious Diseases Society of America , people bitten by deer ticks should not routinely receive antibiotics to prevent the disease, especially if Lyme disease is not common in that area. In areas where Lyme disease is prevalent, a single dose of an antibiotic is commonly administered after a tick bite.
A single dose of the antibiotic doxycycline may be given if:
- At least 20% of ticks in the geographic area are infected with B. burgdorferi.
- The tick is still attached to the person and is positively identified as a species of Ixodes tick that carries the Lyme disease B. burgdorferi spirochete.
- Doxycycline treatment can be given within 72 hours of the tick bite.
- It is safe for the person to receive doxycycline.
In general, the risk of developing Lyme disease after being bitten by a tick is only 1% to 3%. However, if you have an attached tick or have removed it yourself, be sure to inform your health care provider. Also let your provider know if you develop a bull’s-eye rash or any flu-like symptoms in the first 30 days following a tick bite.
Treating Early Stage Lyme Disease
The early stages of Lyme disease usually include the bull’s-eye rash and flu-like symptoms of chills and fever, fatigue, muscle pain, and headache. In rare cases, people develop an abnormal heartbeat .
All of these conditions are treated with 14 to 28 days antibiotics courses. The exact number of days depends on the drug used and the person’s response to it. Antibiotics for treating Lyme disease generally include:
- Doxycycline. This antibiotic is effective against both Lyme disease and human granulocytic anaplasmosis . It is the standard antibiotic for anyone over 8 years old, except for pregnant women. It is a form of tetracycline and can discolor teeth and inhibit bone growth in young children. It can also cause birth defects if used during pregnancy.
- Amoxicillin. This type of penicillin is probably the best antibiotic for pregnant women. Some people are allergic to penicillin and strains of Lyme bacteria are emerging that are resistant to it.
- Cefuroxime . This cephalosporin antibiotic is an alternative treatment for young children and for adults with penicillin allergy.
- Intravenous ceftriaxone or cefotaxime. Intravenous infusions of one of these cephalosporin antibiotics may be warranted if there are signs of infection in the central nervous system or heart.
Other types of antibiotics, such as macrolides like azithromycin and clarithromycin, are not recommended for first-line therapy.
Antibiotic Side Effects
Don’t Miss: Iv Ozone Therapy For Lyme Disease
Treating Late Stage Lyme Disease
Most cases of Lyme disease involve a rash and flu-like symptoms that resolve within 1 month of antibiotic treatment. However, some people go on to develop late-stage Lyme disease, which includes Lyme arthritis and neurologic Lyme disease.
Untreated, slightly more than half of people infected with B. burgdorferi will develop Lyme arthritis. About 10% to 20 % of people develop neurologic Lyme disease. A very small percentage may develop acrodermatitis chronica atrophicans, a serious type of skin inflammation occurring more frequently in Europe. These conditions are treated for up to 28 days with antibiotic therapy.
If arthritis symptoms persist for several months, a second 2 to 4 week course of antibiotics may be recommended. Oral antibiotics are used for Lyme arthritis and acrodermatitis chronica atrophicans.
In rare cases, people with arthritis may need intravenous antibiotics. A 2 to 4 week course of intravenous ceftriaxone is used for treating severe cases of neurological Lyme disease. For milder cases, 2 to 4 weeks of oral doxycycline is an effective option.