Can Nerve Damage From Lyme Disease Be Reversed
This type of neuropathy presents with intermittent paresthesias, does not show significant clinical deficits, and can be treated with antibiotics.
There is no way to prevent Lyme disease from occurring if you only get a tick bite. As a result of being exposed to Lyme, your immune system and brain function are compromised. If left untreated, Lyme can cause long-term symptoms, including nerve damage, as well as long-term chronic illness. Can the nerve damage caused by Lyme Disease be reversed? NutriNerve is a nutritional supplement designed to support nerve health by providing all of the nutrients required to recover from nerve damage. This natural formula has the potential to help you with a variety of health issues, including pain relief. It can help to improve your immunity, boost energy, and reduce inflammation in the body.
Although there is currently no cure for PTLDS, there are medications that can be used to alleviate some of its symptoms. Doxycycline and amoxicillin, for example, have the potential to alleviate pain and fatigue while also improving cognitive function. It is not guaranteed that these treatments will work for everyone, but they are worth trying if you are experiencing any problems after finishing your antibiotic treatment.
What Happens If Lyme Disease Goes Untreated For Years
If Lymedisease is not diagnosed and treated early, the spirochetes can spread and may go into hiding in different parts of the body. Weeks, months or even years later, patients may develop problems with the brain and nervous system, muscles and joints, heart and circulation, digestion, reproductive system, and skin.
Diagnosing Neurological Lyme Disease
The first step in the diagnosis of Lyme disease and associated infections is to order blood tests through a Lyme specific laboratory. It is well-established the traditional two-tiered test has low sensitivity for diagnosing Lyme disease.
The diagnosis of acute central nervous system involvement of Lyme disease requires a lumbar puncture to analyze cerebral spinal fluid . The analysis of the CSF should include IgM and IgG antibodies to Borrelia bacteria and a test looking for the bacteria DNA . If either of these markers is elevated, it is diagnostic of Lyme neuroborreliosis.
An increased level of white blood cells in the CSF known as pleocytosis also aids in the diagnosis. However, some people with neuroborreliosis do not have elevated antibodies in the CSF, and since pleocytosis can be present in other central nervous system infections, Lyme disease may not be considered.
The chemical attractant something known to call the immune system to fight an infection CXCL13 in the CSF has become an important marker to help diagnose Lyme neuroborreliosis. In a 2018 study of Lyme neuroborreliosis patients with elevated white blood cells but no detectable Lyme antibodies in their CSF, 73% had raised levels of CXCL13. The authors of the study have proposed a CXCL13 result greater than 160 pg/mL is consistent with Lyme neuroborreliosis.
Also Check: How To Test For Lyme Disease In Adults
Not Removing Ticks Properly And Immediately
Not removing ticks immediately and correctly can increase your risk of Lyme disease.
To remove a tick properly:
- Use fine-tipped tweezers to grasp the tick as close to the skins surface as possible.
- Pull the ticks body away from the skin using a slow and steady motion. Do not twist or jerk the tick, as this can cause the mouthparts to break off and stay in the skin. If this happens, remove the mouthparts with tweezers.
- Clean the bite area and your hands with rubbing alcohol or soap and water.
How Do Lyme & Tick
- A 37 year old man with a constant headache so intense any sound, light, or movement is intolerable.
- A 26 year old with Multiple Sclerosis but with no family history of the disease.
- A 12 year old girl with chronic muscle spasms so severe she requires a walker.
- A 51 year old woman unable to retrieve words when she speaks.
- A 10 year old boy with a sudden onset of an obsessive-compulsive disorder.
- A 4 year old with intense rages that occur almost all day.
- A 27 year old man with crippling anxiety that over 30 physicians and mental health providers were unable to treat effectively
All these cases are people with Lyme and Tick-Borne Disease. It seems inconceivable that a little tick can cause such extremes and incapacitation. Yet these diseases and autoimmune disease, in general, are on the rise.
**Dr. Roseann is hosting a professional training on the Neurocognitive and Neuropsychiatric impact of Lyme, Tick-Borne, and PANS/PANDAS with BCIA on June 29th. Learn More.**
You May Like: Treating Lyme Disease After Years
Lyme Disease Leg Pain At Night
There are many possible causes of leg pain at night, and Lyme disease is one of them. Lyme disease is a bacterial infection that is transmitted by ticks. Lyme disease can cause a wide range of symptoms, including leg pain. Leg pain from Lyme disease is often worse at night, and it can be accompanied by other symptoms such as fatigue, fever, and headache. If you think you may have Lyme disease, it is important to see a doctor for diagnosis and treatment.
Chronic aching muscles can be caused by Lyme disease. Aside from fatigue, headaches, dizziness, light and sound sensitivity, memory and concentration issues, stiff neck, tingling, and joint and muscle pain, a few other symptoms may occur. Before you begin to investigate the source of your muscle pain, you should first figure out what is causing it. Understanding why you feel sore when you have Lyme will help you understand how the immune system functions in this context. Musculoskeletal issues, particularly arthritis, are common in people who have this disease. The increased sensitivity to Lyme that occurs when you take medication for it is caused by the elimination of Lyme bacteria. For several years prior to Lyme, there is a marked cellular and humoral immune response that starts to affect the large joints, particularly the knee.
Visualizing Brain Fog In Post
More than one in 10 people successfully treated with antibiotics for Lyme disease go on to develop chronic, sometimes debilitating and poorly understood symptoms of fatigue and brain fog that may last for years after their initial infection has cleared up.
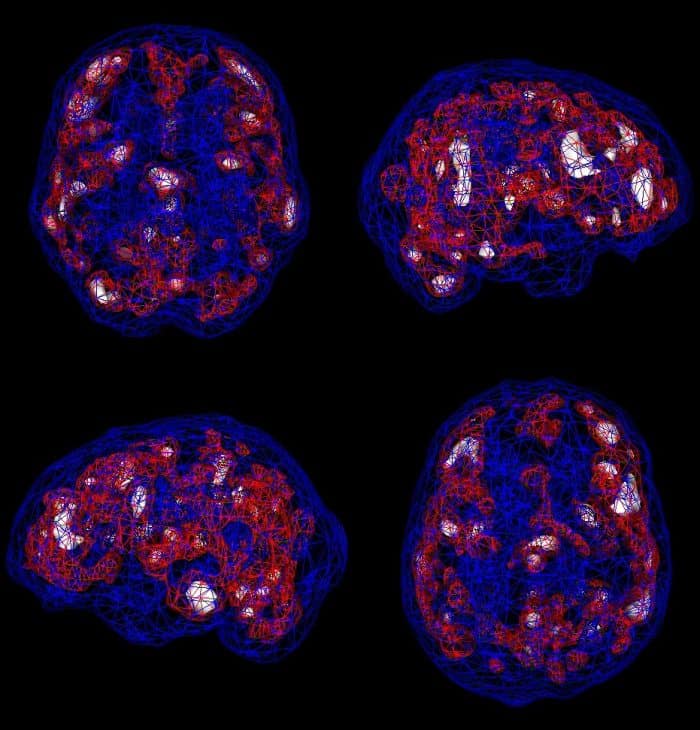
Now, a Johns Hopkins team has used an advanced form of brain scan to show that 12 people with documented post-treatment Lyme disease syndrome all show elevation of a chemical marker of widespread brain inflammation, compared with 19 healthy controls.
Results of the study, published in Journal of Neuroinflammation, suggest new avenues for treating the long-term fatigue, pain, sleep disruption and brain fog associated with PTLDS. Theres been literature suggesting that patients with PTLDS have some chronic inflammation somewhere, but until now we werent able to safely probe the brain itself to verify it, says Jennifer Coughlin, a senior author and associate professor of psychiatry and behavioral sciences.
What this study does is provide evidence that the brain fog in patients with post-treatment Lyme disease syndrome has a physiological basis and isnt just psychosomatic or related to depression or anxiety, says John Aucott, director of the Johns Hopkins Lyme Disease Research Center.
In addition, the results suggest that drugs designed to curb neuroinflammation may be able to treat PTLDS, although clinical trials are needed first to determine the safety and benefit of such therapy, Aucott says.
Also Check: Lyme Ab W Reflex Western Blot
Cause #: Untreated Infections
Lyme disease and Lyme coinfections like babesia, bartonella, and mycoplasmacontribute to metabolic and immune changes in the body because the microbes can be low-grade and persist for long periods of time. While no system of the body is off-limits, the central nervous system and the endocrine system are particularly vulnerable.
When pathogens invade the nervous system, white blood cells immune cells like lymphocytes and plasmocytes flood into the white matter of the brain and the spinal cord, says Dr. Bill Rawls, Medical Director of RawlsMD and Vital Plan. This causes a cascade of inflammatory immune messengers, called cytokines, in cerebrospinal fluid.
This influx of proinflammatory cytokines causes neuroinflammation in the brain, which can contribute to a range of neurological symptoms, including those associated with Lyme brain. Because most Lyme patients have a compromised immune system, the body struggles to keep the offending pathogens in check.
The outcome? You continue to experience a prolonged inflammatory response and resulting symptoms until youre able to suppress the harmful, stealth infections.
Recommended Reading: Lyme Disease And Chest Pain
What Does Pain From Lyme Disease Feel Like
Early Lyme symptoms include pain and stiffness in the joints, which are frequently intermittent. If your joints are inflamed, irritated, painful, or swollen, you should seek medical attention. You may experience stiffness or a limited range of motion in some joints as a result of this condition. Some people experience chronic pain that travels around them.
Lyme Disease: The Rash, The Symptoms, And The Treatment
It may also resemble a bulls eye if left untreated. It may cause irritation, but it can also cause pain. If you have an extremely severe case of shingles, you may experience itching and blistering. Lyme disease can cause fever, headache, neck stiffness, muscle pain, and fatigue, among other symptoms. Flulike symptoms, such as a mild fever, chills, and body aches, may occur in some people. In some cases, lyme disease may appear without symptoms at all. This condition is especially prevalent in people who have been infected with the disease for a long time and have had multiple tick bites. You should consult a doctor if you suspect you have Lyme disease. Although there is no cure for Lyme disease, treatment may be effective in relieving symptoms.
Recommended Reading: Do You Ever Recover From Lyme Disease
Lyme Disease Brain Fog Is A Serious Thing
When the levels of quinolinic acid are too high in the brain, the may indicate that the infection has crossed the blood-brain barrier. Brain fog is a common occurrence in Lyme patients. Unlike that normal fogginess you might feel when you wake up still drowsy, Lyme brain fog causes ongoing mental conditions that continue to worsen over time.
Some patients may experience psychosis, and many feel like they are going crazy. These mental issues are the direct result of Lyme-causing bacteria-producing toxins that impact the brain. The immune system may not be able to get rid of them on its own.
Lyme patients can’t just “shake offtheir symptoms. Treatments include ways to reduce inflammation and manage brain fog.
Brain Fog Looks Like Cognitive Decline
Brain fog causes problems like:
- lost ability to form words and thoughts easily
- trouble focusing
- personality changes
It can be hard to detect some of the more subtle symptoms. For instance, you might normally love loud music, but after a tick bite, you find it hard to handle the way you once did. Or your fatigue won’t go away, no matter how much you sleep or how restful your slumber is each night.
Infections of any kind can result in symptoms like brain fog and the others listed above. It may seem like asking your doctor for antibiotics can help, but if there is brain inflammation and neurodegeneration, you need further treatment. Antibiotics alone are not the answer for Lyme disease.
Brain Fog In Lyme Disease: What Is It
There are two kinds of brain fog in Lyme disease. Some people have both forms.
- Type 1 Brain Fog. The first kind is a feeling or sensation of cloudiness or fogginess of the head.
- Type 2 Brain Fog. The second type is a problem with brain function where a person cannot think. People with thinking problems usually have problems with short-term memory, confusion, poor attention, organization, word finding, or concentration.
Type 1 brain fog is caused by a buildup of cytokine inflammation chemicals and another chemical made in brain infections called quinolinic acid. It is also due to a buildup of toxins in the blood from mold or yeast overgrowth in the intestines. While the literature does not describe this type of brain fog or its treatment. I have observed great improvement in Type 1 brain fog by lowering cytokine inflammation chemicals with liposomal curcumin 500 mg 3 times a day, eliminating intestinal yeast, or removing mold toxins. See Step One: Treat Infections or Mold Toxins below for links to articles on this site regarding yeast and mold toxins. Note, fixing Type 2 brain fog also fixes Type 1 brain fog.
In this article I focus primarily on the treatment steps for Type 2 brain fog. Type 2 brain fog has three possible causes
Recommended Reading: Best Herbal Treatment For Lyme Disease
Do Remnants Of Lyme Bacteria Cause Ongoing Brain Inflammation
Even after antibiotic treatment, some Lyme disease patients suffer from an array of symptoms including neurological issues that greatly diminish their quality of life.
Brain scans of these patients show persistent neuroinflammation, but the cause has been unclear.
Tulane University researchers have discovered that remnants of B. burgdorferi, the bacteria that causes Lyme disease, may contribute to inflammation in both the central and peripheral nervous systems.
These remnants are significantly more inflammatory than live, intact bacteria. Their results were published in Scientific Reports.
Lead researcher Geetha Parthasarathy, PhD, assistant professor of immunology at the Tulane National Primate Research Center, explored the effects of B. burgdorferi remnants on nervous system tissue using a nonhuman primate model, investigating the effects on both the frontal cortex and dorsal root ganglion.
How Do You Treat Lyme & Tick
Access to proper tick bite treatment can often be hindered because there the medical community disagrees about how to identify those with Lyme Disease. Moreover, no perfect measures of identification exist. Lacking good measures for Lyme Disease, which has been readily accepted for decades, is compounded by lacking measures for the dozens of co-infections.
Diagnosis guidelines do not require positive blood work, yet many physicians erroneously use the CDC epidemiology study submission guidelines for diagnosis. Thus, patients are often forced to pay out of pocket for the best diagnostic tools available, which are through private lab companies.
Relying on incorrect guidelines means patients are told they must have 5 out of 10 bands to be diagnosed with Lyme. This creates a major barrier to quick and necessary tick bite treatment. Only clinical opinion after a physical exam is required to make a diagnosis of Lyme.
Read Also: Can Lyme Disease Cause Lower Back Pain
What Causes The Symptoms Of Lyme Disease
While the symptoms of Lyme disease can be severe if untreated, they are not thought to be caused by any toxins or detrimental substances produced by B. burgdorferi, as is the case with some other particularly harmful bacteria. Unfortunately, what does cause the symptoms is still not completely clear. It is thought, however, that most of the problems likely are due to side effects of the immune system response to the presence of the bacterium. The primary immune response thought to be at play is inflammation, a general reaction your immune system has to any potentially harmful or foreign substance.
Inflammation involves the accumulation of immune system cells at a site of infection or damage, and the goal of the response is to repair damage and remove potentially dangerous foreign invaders. Inflammation, however, can also lead to secondary symptoms a well-known example of this is when you experience redness, pain, and swelling around the area of an injury. Secondary effects of this sort are thought to contribute to the symptoms of Lyme disease ranging from the initial skin rash to joint problems.
The inflammation that occurs after B. burgdorferi infection seems to be disproportionate to the threat of the bacterium. In other words, the inflammatory response is stronger than it needs to be. Often, it even continues after the immune system has eliminated B. burgdorferi from the body. The reasons for this exaggerated response are unclear.
Should You See A Neurologist For Lyme Disease
A neurologist is a specialized medical professional who deals with all neurological disorders. When a person is suffering from neurological complications of Lyme disease, it may seem as though seeing a neurologist may help. But in truth, any doctor can test and diagnose you with Lyme disease, regardless of your symptoms.
It might be appropriate to see a neurologist for Lyme disease if you are only experiencing neurological symptoms however, if you have any other symptoms of the infection, you should see your general practitioner first.
The neurological symptoms of Lyme disease can be difficult to cope with, but the good news it that Lyme disease can be treated. The best way to address any neurological symptoms is see your doctor so they can direct you to the right specialist or assist in getting you diagnosed with Lyme disease so treatment can begin.
Featured image by Hainguyenrp on Pixabay
You May Like: Can Lyme Disease Spread From Person To Person
Lyme Sci: When Brain Inflammation Persists After Lyme Disease Treatment
In a new study, researchers from the Johns Hopkins School of Medicine have found evidence of chemical changes and widespread inflammation in the brains of patients with chronic symptoms following treatment for Lyme disease.
This Johns Hopkins study, in Journal of Neuroinflammation, supports the experience of hundreds of thousands of patients who have tried for years to have their chronic symptoms of pain, sleep disturbance, fatigue, and cognitive impairment validated.
What this study does is provide evidence that the brain fog in patients with post-treatment Lyme disease syndrome has a physiological basis and isnt just psychosomatic or related to depression or anxiety, says John Aucott, M.D., a senior author of the new paper and director of the Johns Hopkins Lyme Disease Research Center.
The fact is, too many patients with Lyme disease are left with chronic, debilitating symptoms following treatment for Lyme disease. In the nearly 40 years since the discovery of Lyme, no one has been able to determine why some patients get better with treatment and others remain ill.