How Do I Remove A Tick From My Dog
Check your pet immediately after it has been in a tick-infected area. The deer tick is a small tick and only about pinhead size in juvenile stage, but is a little more obvious in the adult phase and after feeding. If you find a tick moving on your pet, the tick has not fed. Remove the tick promptly and place it in rubbing alcohol or crush it between two solid surfaces. If you find a tick attached to your pet, grasp the tick with fine tweezers or your finger nails near the dogs skin and firmly pull it straight out. There are also tools available called Tick Twister® or Tick Key® which can be useful. However, take care to use them cautiously as twisting or jerking the tick may cause the mouth parts to break off and remain in the skin. See your veterinarian if you are unsure or unable to remove the tick from your dog.
Make sure you protect your fingers from exposure by using a tissue or a disposable glove.You may need another person to help restrain your dog. Removing the tick quickly is important since the disease does not appear to be transmitted until the tick has fed for approximately 12 hours. If you crush the tick, do not get the ticks contents, including blood, on your skin.
Note: The bacterium that causes Lyme disease can pass through a wound or cut in your skin.
Hunting For Alternative Drug
Frustrated by the lack of treatment options for Lyme disease patients with lingering symptoms, Rajadas and his team began hunting for a better alternative in 2011. In 2016, they published a study in Drug Design, Development and Therapy that listed 20 chemical compounds, from about 4,000, that were most effective at killing the infection in mice. All 20 had been approved by the Food and Drug Administration for various uses. One, for instance, is used to treat alcohol abuse disorder.
Jayakumar Rajadas
In this most recent study, azlocillin, one of the top-20 contenders, was shown to eclipse a total of 7,450 compounds because it is more effective in killing B. burgdorferi and causes fewer side effects. Lyme disease affects more than 300,000 people annually, according to the Centers for Disease Control and Prevention. It can affect various organs, including the brain, skin, heart, joints and nervous system, and cause heart problems and arthritis if untreated. Symptoms include fever, headaches, chills, and muscle and joint pain.
Traditional antibiotics, such as doxycycline, are effective as an early course of treatment for the infection in the majority of patients, but it remains unclear why these drugs fail to treat 10% to 20% of patients, Rajadas said.
Type Of Clinician Overseeing Care
We asked patients to tell us the type of clinician overseeing their care. Choices included: family physicians, internists, rheumatologists, infectious disease specialists, and clinicians whose practice focused on tick-borne diseases . Very few patients selected an infectious disease specialist. Seventy-five percent of high responders and well patients report having their care overseen by an LLMD.
Physicians who treat Lyme disease as their primary focus might be expected to have better results than physicians who dont simply because volume of cases handled means a greater experience level. It is commonly recognized in medicine that volume of cases is associated with better treatment outcomes . Just as patients with cancer commonly seek out physicians who specialize in that area, perhaps patients with chronic Lyme disease should also.
Read Also: Bell’s Palsy Lyme Disease Treatment
Stage : Late Disseminated Lyme Disease
Stage 3 or late disseminated Lyme disease is the final stage of the disease. A person may enter this stage if they did not receive treatment for Lyme disease in the early stages, or if their symptoms persisted despite treatment. As such, doctors sometimes refer to this stage as chronic or post-treatment Lyme disease .
Stage 3 Lyme disease can occur after an infected tick bites a person.
A person with stage 3 Lyme disease may experience additional symptoms, including:
- severe joint pain and swelling, known as chronic Lyme arthritis
- heart palpitations or irregular heartbeat, due to Lyme carditis
- inflammation of the brain and spinal cord
- mental fogginess
How Is Lyme Disease Diagnosed And Treated

Lyme disease is usually diagnosed when a person develops a bulls-eye rash, flu-like symptoms , or both. These symptoms usually start a few days or weeks after the person is bitten by an infected tick.
A two-step blood test can verify the presence of Lyme disease antibodies, although it does take a few weeks for those antibodies to develop. And despite what some physicians and advocacy groups claim, a blood test is the only way Lyme disease can be confirmed, Larry Zemel, MD, head of rheumatology at Connecticut Childrens Medical Center, tells Health. Some doctors say they can diagnose Lyme even when patients test negative repeatedly, but that has not been borne out by any scientific study, he says.
When people are diagnosed with Lyme disease in its early stages, a 10- to 20-day course of oral antibioticsusually with a drug called doxycyclinewill clear the infection and help them feel better fairly quickly. This cures the vast majority of people, and they have a 100% recovery with no lasting effects, says Dr. Zemel.
If Lyme disease isnt diagnosed right away, it can cause more serious symptoms like arthritis and memory problems. These people may need a full month of oral antibiotics, says Dr. Zemel. About 20% of these patients will need IV antibiotics , and they may also need other medications to treat symptoms like pain and muscle stiffness.
Also Check: How Lyme Disease Affects The Brain
What To Expect At Home
Home care for dogs with Lyme disease is relatively straightforward. Doxycycline is usually given by mouth twice daily for at least 30 days. Improvement in the dogs symptoms should be noted within 24-48 hours. If the dogs condition fails to improve in 72 hours or worsens at any time, call your veterinarian.
What Are The Side Effects Of Lyme Disease Treatments
Antibiotics, like all medications, have the potential for side effects. Any antibiotic can cause skin rashes, and if an itchy red rash develops while on antibiotics, a patient should see their physician. Sometimes symptoms worsen for the first few days on an antibiotic. This is called a Herxheimer reaction and occurs when the antibiotics start to kill the bacteria. In the first 24 to 48 hours, dead bacterial products stimulate the immune system to release inflammatory cytokines and chemokines that can cause increased fever and achiness. This should be transient and last no more than a day or two after the initiation of antibiotics.
The most common side effect of the penicillin antibiotics is diarrhea, and occasionally even serious cases caused by the bacteria Clostridium difficile. This bacterial overgrowth condition occurs because antibiotics kill the good bacteria in our gut. It can be helpful to use probiotics to restore the good bacteria and microbiome balance.
Recommended Reading: How To Cope With Lyme Disease
Why This Is Important
The use and duration of antibiotics for chronic Lyme disease treatment is controversial because there is no biomarker that can determine whether the Lyme bacteria has been eradicated in CLD patients. Patients are often told that either chronic Lyme disease does not exist or that it is incurable. If this were true, we would not expect more well and substantially improved patients to be taking antibiotics. Instead, we might have expected the percentage of people using antibiotics to be roughly the same among the patient subgroups.
Do Antibiotics Help Patients With Lyme Disease Who Are Also Diagnosed With Ms
Periodically, I post information about some of the findings from our big data project, MyLymeData. We call these Quick Bytes. In April, my Quick Byte on neurologic Lyme disease focused on how often Lyme patients are misdiagnosed with a neurologic condition including MS . The blog included a brief survey for those whose neurologic Lyme had been misdiagnosed. The survey asked about any antibiotic treatment they may have received. I report on the results of that survey here today.
Our MyLymeData registry asks patients if they were initially misdiagnosed with another illness, and if so, what the illness was. About 20% of respondents were told they had a neurological disease. 14% were misdiagnosed with MS, and 2% with other neurological diseases like ALS, Parkinsons and multiple system atrophy. When looking at this data, it is important to recognize that geography may play a big role in both the prevalence of neurologic conditions and Lyme disease in a particular area.
In my previous blog, I pointed out the dangers of misdiagnosis, particularly when patients are given steroids or other immune suppressants that may allow the infection to run rampant. I also pointed out that patients with Lyme disease can become terribly ill on steroids. These are the points to bear in mind:
Don’t Miss: Samento And Banderol For Lyme Disease
Stage : Early Localized Lyme Disease
Stage 1 or early localized Lyme disease occurs 128 days following a tick bite.
Some people with stage one Lyme disease do not experience any symptoms. If symptoms do occur, they may include the following:
- a skin rash that may or may not resemble a bulls-eye
- flu-like illness, including chills and a fever
- swollen lymph nodes
What Are The Most Common Risk Factors For Lyme Disease
The most common risk factors for Lyme disease include: Spending time in wooded or grassy areas. In the United States, deer ticks are found mostly in the heavily wooded areas of the Northeast and Midwest. Having exposed skin. Ticks attach easily to bare flesh. Not removing ticks promptly or properly.
Read Also: What Are The Symptoms Of Lyme Disease In A Person
You May Like: What Does Lyme Disease Do To The Brain
Achy Stiff Or Swollen Joints
Joint pain and stiffness, often intermittent, are early Lyme symptoms. Your joints may be inflamed, warm to the touch, painful, and swollen. You may have stiffness and limited range of motion in some joints .
Pain may move around. Sometimes your knees may hurt, whereas other times its your neck or your heels. You may also have bursitis . Bursae are the thin cushions between bone and surrounding tissue.
The pain may be severe, and it may be transitory. More than one joint may be affected. Most often the large joints are involved .
People often attribute joint problems to age, genetics, or sports. Lyme should be added to that list, as these statistics indicate:
- One study estimates that 80 percent of people with untreated Lyme have muscle and joint symptoms .
- Fifty percent of people with untreated Lyme have intermittent episodes of arthritis .
- Two-thirds of people have their first episode of joint pain within six months of the infection .
- Use of anti-inflammatory drugs may mask the actual number of people with joint swelling .
Summary:
Joint pain that comes and goes, or moves from joint to joint, could be a sign of Lyme.
Read Also: How Do You Contract Lyme Disease
Stage : Quickly Expanding Rash
After being bitten by a black-legged tick, a quickly growing rash can appear. This is the earliest stage of Lyme disease, known as stage 1.
Most people who develop a rash, get it within days or weeks of being bitten by a tick.
Where you see the rash: If you develop a rash, it appears near the tick bit you. For most people, that means the back, groin, armpit, or a lower leg. However, a tick can bite you anywhere.
What the rash can look like: You may see a spot or bump on the skin, which is the bite mark. Around or near the bite mark, a rash develops. Some people see the bulls-eye rash . You can also have one of the other rashes shown here.
Early rash caused by Lyme disease
Notice the bite mark in the center of this early rash, which will expand quickly.
Bulls-eye rash on womans upper arm
This is another early sign of Lyme disease.
Lyme disease rash with lighter color on the outside
This rash has expanded, but you can still see the bite mark in the center.
Rash from Lyme disease has begun to clear
As the rash begins to clear, the redness fades.
If you develop a rash during this stage, you may notice that it:
-
Feels smooth and warm to the touch
-
Causes a burning sensation
-
Itches or feels painful
-
Has an outer edge that feels scaly or crusty
When the rash and symptoms begin: According to the Centers for Disease Control and Prevention , the rash begins 3 to 30 days after the tick bites you.
About 50% of people who have Lyme disease develop flu-like symptoms , which include:
Read Also: Best Herbs For Lyme Disease
Lyme Disease Antibiotic Treatment Research
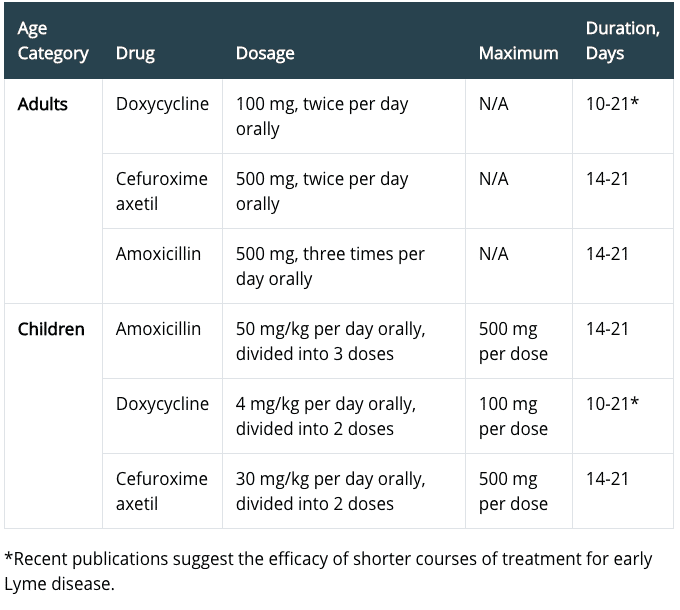
For early Lyme disease, a short course of oral antibiotics, such as doxycycline or amoxicillin, cures the majority of cases. In more complicated cases, Lyme disease can usually be successfully treated with three to four weeks of antibiotic therapy.
After being treated for Lyme disease, a minority of patients may still report non-specific symptoms, including persistent pain, joint and muscle aches, fatigue, impaired cognitive function, or unexplained numbness. These patients often show no evidence of active infection and may be diagnosed with post-treatment Lyme disease syndrome .
Multiple clinical trials, funded by NIH and others, have shown no benefit to additional IV antibiotic treatment in patients with Lyme disease, although the interpretation of those results have been challenged by some.
Tetracycline Plus Macrolide Plus Grapefruit Seed Extract Plus Japanese Knotweed
- doxycycline 100 mg 2 pills 2 times a day
- clarithromycin 500 mg 1 pill 2 times a day
- grapefruit seed extract 250 mg 1 pill 2 times a day.
- Japanese knotweed½ tsp 3 times a day
Key Points:
- Tetracyclines and macrolides both block protein production by binding to the protein production apparatus in germs called ribosomes. But they each bind to a different part of the ribosome improving the blockade of protein production.
- Japanese knotweed is added here to treat persister Lyme. It also may treat growing Lyme and can lower inflammation cytokines.
Also Check: How To Check For Lyme Disease In Dogs
For Depression And Anxiety
Both psychotherapy and pharmacotherapy have proven benefits for improving mood. Psychotherapy has many different types such as supportive, dynamic, cognitive behavioral, dialectical behavior therapy, transference focused psychotherapy each of which offers benefit. Pharmacotherapy also has many different types. For depression the first-line options usually are SSRIs, SNRIs, Tricyclics or other agents with more unique modes of action.
A few noteworthy tips on anti-depressant agents:
- Most anti-depressant agents also help in reducing anxiety. However the opposite isn’t necessarily true. Specific anti-anxiety agents such as clonazepam or diazepam may not necessarily help fight depression.
- Most anti-depressants take three to eight weeks before an effect is seen. Therefore, it is unwise to stop an anti-depressant after only three or four weeks, as staying on it another two to three weeks may lead to a good response.
- Dosage makes a difference. Some anti-depressants work fine at low doses some medications however are effective only at higher doses. Some medications are more effective as the dose is increased. Other antidepressants may have a therapeutic range one has to achieve at least a certain dosage .
What Causes Lyme Disease
People get Lyme disease when they are bitten by an infected tick. Ticks live in areas with a lot of plant life, such as wooded areas or fields. They sit near the top of grassy plants and low bushes. They wait there for people or animals to brush up against them. Ticks can crawl on your clothes or body for up to several hours or more before attaching to the skin.
Ticks can attach to any part of your body. They are usually found in hard-to-see areas, including the armpits, groin, or scalp. An infected tick needs to be attached to your skin for 36 to 48 hours before it passes the bacteria on to you.
People who spend time in outdoor areas where ticks are common are at higher risk of getting tick-borne diseases.
You May Like: Urgent Care East Lyme Ct
How Is Lyme Disease Diagnosed
It can be difficult to diagnose Lyme disease. The ticks that carry it are very small and the bites dont hurt. Many patients dont remember being bitten. In addition, most of the symptoms are common with other illnesses.
If you find a tick in your skin, use tweezers to remove it immediately. Then wait a few days to see if you develop any symptoms. If you do, call your family doctor. Your doctor will ask you about your symptoms. They will look at the bite and check for a rash. They may order a blood test. But those arent always necessary to make the diagnosis. They can often give false results, especially in early-stage Lyme disease.
People who have joint swelling or nervous system problems may need to have special tests. Your doctor may need to take some fluid from the swollen joint or the spine to check for clues to your condition.
If you have been sick for 4 weeks or more, call your doctor. They can give you a blood test at this stage. It will tell you if you have Lyme disease.
Look How Far Ive Come
My initial Lyme test was, in the words of my doctor, lit up like a Christmas tree. Pretty much everything on it was positive: 2 different strains of Lyme, babesia, bartonella, and mycoplasma. I was a mess.
This summer I had a repeat test. Everything came back negative. While this doesnt mean Im definitively negative for Lyme, it certainly indicates weve been able to reduce the load enough that its not showing up on the tests. Ill likely need to continue some level of treatment for quite some time.
There are many Lyme specialist who dont believe its ever possible to be completely cured of Lyme. Its a sneaky bacteria and good at hiding. Many believe, the best you can get is to effectively put yourself in remission and strengthen your immune system. This keeps the Lyme bacterial load low enough that the symptoms are kept at bay.
Another fantastic result of treatment has been a huge decrease in inflammation. My c4a levels were 20,749 when I was first diagnosed. Thats a lot. . At the beginning of this year, after about a year of treatment, they were down at 17,594. This September, I was delighted to see my levels down to 4,090. Im inching closer to being back in the normal levels.
Read Also: Lyme Disease Specialist In Wisconsin