Lyme Disease In Dogs: What You Need To Know Now
Lyme disease is an infectious, tick-borne disease that is prevalent in the Northeast, as well as common throughout the United States. In Sussex county specifically, its incredibly common due to the high tick population in our area. Ticks that transmit Lyme disease are carried by deer, and with the number of deer in New Jersey both growing and expanding their terrain, the instances of Lyme disease in dogs continue to grow as well.
Protecting your dog from this dangerous disease is always a better option than waiting until your pet has become infected. Treatment can be costly, and depending on how the dog responds, in some cases, it can become a long term issue. Chronic Lyme is often harder to treat, with symptoms that can remain with your pet for their lifetime. If your pet does become infected, early diagnosis and a specific treatment plan designed by your vet is the best chance at beating the disease for good. In rare cases, it can cause kidney damage and failure that can be fatal, so tick control is important.
Even walking dogs along a road can be enough opportunity for ticks to latch on.
And stay tuned for more blogs on what to do if you think your dog has lyme to learn about diagnosis and treatment options, and an upcoming series about treating Lyme disease in horses, which is also high risk in our area.
Dengue And Dengue Hemorrhagic Fever
Dengue is an acute, usually self-limited febrile zoonotic illness commonly referred to as âbreakbone fever.â Dengue virus is a flavivirus with 4 antigenically similar types however, human infection with one type does not consistently or completely confer immunity to the other types. The World Health Organization estimates that Dengue virus infects 50 million people annually. The virus is spread by the mosquito, Aedes aegypti, and the disease distribution generally occurs within the vectorâs distribution. The incubation period ranges from several days to 1â2 weeks. The symptoms and severity of disease vary with age. Infections are often asymptomatic in children. Classic Dengue presents with fever, severe myalgias, arthralgias, headache, retro-orbital pain, gastrointestinal symptoms and rash. Minor bleeding from mucosal surfaces, hemoptysis and gastrointestinal hemorrhage can occur. In contrast, Dengue hemorrhagic Fever and Dengue Shock syndrome are characterized by increased vascular permeability, spontaneous hemorrhage, and hypotension.
The differential diagnosis of dengue is very similar to that of yellow fever. There is no effective antiviral treatment at this time and treatment is supportive. Although there are vaccine candidates in development, there are currently no approved vaccines for dengue.
High T Cell Chemokine Levels Are Associated With Seroconversion
In this patient cohort, 35.7% of Lyme patients fail to test positive either at diagnosis or through seroconversion following antibiotic treatment . This is consistent with previous studies that demonstrated that a significant fraction of Lyme patients that exhibit EM along with other symptoms of infection do not seroconvert when assayed by the current two-tiered testing , . When we examined whether various elevated mediator levels could be correlated with seroconversion status, a significant association was observed with elevated CXCL9 and CXCL10 but not CCL19 levels . When other clinical parameters such as duration of illness or size/dissemination of EM lesions were analyzed, there was no association with seroconversion status.
Don’t Miss: How Would I Know If I Had Lyme Disease
Liver Enzymes 500 And Newly Diagnosed With Lyme Disease Can They Be Related
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
HealthTap doctors are based in the U.S., board certified, and available by text or video.
Diagnosis Of Monocytic Ehrlichiosis Bacterialinfection

Lab tests are used to diagnose this type of lyme disease.Testing often shows a decrease in your dog’s platelet count, the bloodcells that cause clotting , low red blood cell counts and lower white blood cell count . Yourveterinarian may also find enlarged lymph nodes and higher than normalliver enzyme counts.
Treatment of Ehrlichiosis Bacterial Infection
Antibiotics are used to treat this type of lymedisease for 3 weeks. If your dog has asevere case then treatment can last 1 year. If your dog has a severecase then your veterinarian may recommend a blood transfusion. Dogswith this problem are expected to make a full recovery. In some casesthe prognosis is not as good if all parts of the blood are affected.Similar concerns exist if your dog has a heart deformity or bone marrow disease .
Don’t Miss: How To Kill Lyme Disease Naturally
Acute Lyme Disease Patient Defined Subgroups Have Distinct Clinical Features
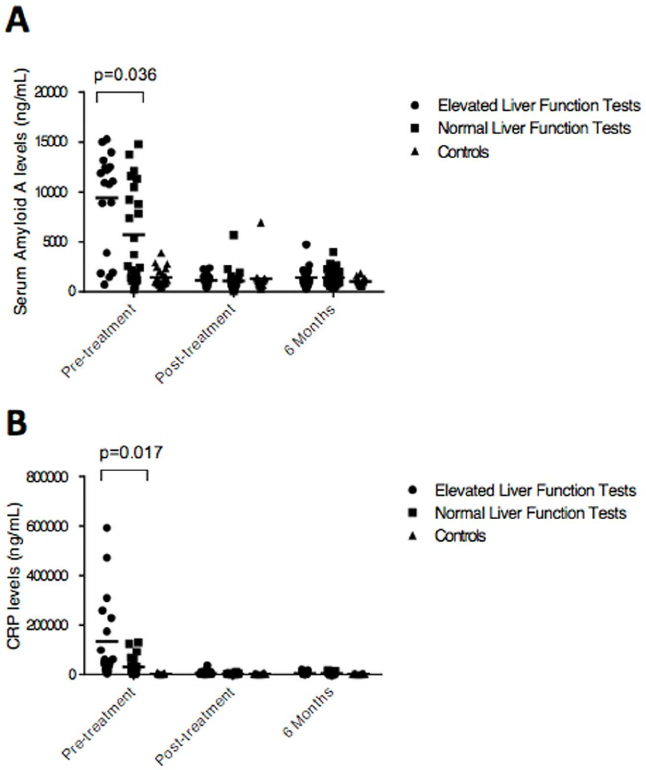
Based on immune mediator levels during acute infection, two subgroups of Lyme patients could be distinguished. presents a comparison of these two groups for a range of clinical outcomes. No differences in demographics, duration of illness or the distribution of single versus multiple erythema migrans lesions were noted between the two groups. However, significant differences were noted in the number of symptoms , absolute lymphocyte levels , liver enzyme tests and the presence of detectable anti-Borrelia antibodies . Lyme disease patients displaying high mediator levels at the initial pre-treatment visit had higher rates of seroconversion, but also had greater rates of lymphopenia and elevated liver enzyme.
Are Test Results Accurate
ALP test results are usually regarded as accurate, but, like any medical test, an ALP blood test is not perfect. There are potential sources of error in the processing and analysis of your blood sample, so laboratories must take care to follow best practices to ensure dependable results.
Testing for ALP isoenzymes is more technically demanding. Different methods exist for determining the part of the body that is the source of increased ALP, but special techniques that are not available at all laboratories can make this testing much more reliable.
Read Also: What Kind Of Ticks Give You Lyme Disease
Blacklegged Tick Risk Areas
Although it is possible to be bitten by blacklegged tick anywhere in New Brunswick, the risk is highest in areas where blacklegged tick populations are established or could become established. Blacklegged Tick Risk Areas are based on provincial tick surveillance data and are identified on a county level because it is difficult to exactly define the geographic limits of tick populations. Although blacklegged ticks are more likely to be found within risk areas than in other parts of the province, the distribution of ticks within Blacklegged Tick Risk Areas is not uniform because suitable habitat is not found everywhere.
Lyme Disease Risk areas
General Diseases: Lyme Disease Symptoms
Dog General Diseases and Symptoms QuickLinks
Lyme disease is a term that applies to severaldifferent types of bacteria transmitted by ticks. Symptoms of caninelyme disease are dependent on the type of bacteria that has beentransferred by a deer tick to your dog . Humanscannot be infected by a dog or a cat.
The group of bacteria that causes infection iscalled Ehrlchiosis. Each form of ehrlchiosis bacteria tends to infect aspecific type of white blood cell or the platelets.
- White Blood Cells: which are the way they body fights infection.
- Red Blood Cells: transportoxygen
- Platelets: helpthe blood to clot
Recommended Reading: Lyme Disease And Chronic Fatigue
Herpes Simplex Virus And Other Herpes Viruses
The pathogenesis of HSV hepatitis remains speculative and proposed mechanisms include a large inoculum of HSV, an impaired immune response including possible hypersensitivity reactions, enhanced virulence of certain HSV strains and directly viral cytopathy.
Early treatment with acyclovir appears to be associated with improved survival, reinforcing the need to establish the diagnosis promptly. In one review of treated cases, 13 of 21 patients survived. Given the severity of this syndrome, some authors recommend treatment with acyclovir at a dose of 10mg/kg IV every 8 hours.
Identification Of A Cytokine/chemokine Signature Associated With Acute Lyme Disease
We have conducted a prospective cohort study of acute Lyme disease and post-treatment events . All patients enrolled in the study have untreated early Lyme disease that meets the Infectious Disease Society of America criteria for diagnosis , , . Using samples collected from this cohort we employed a bead-based multiplex cytokine assay to measure the levels of 58 immune mediators and 7 acute phase proteins in the serum of patients with untreated early Lyme and matched controls. Displayed in is a heat map of those mediators significantly elevated in early acute Lyme disease at the initial pre-treatment visit compared to controls. Most notable are elevated levels of several T cell chemokines , acute phase inflammatory markers , several IL-1 cytokine family members , inflammatory cytokines TNF-α and IL-6 and the T cell cytokine IL-2. Collectively, these cytokines and chemokines generate a novel signature that clearly distinguishes acute Lyme patients from normal controls.
Elevated Immune Mediators in Lyme Disease.
Don’t Miss: Alternative To Doxycycline For Lyme
Severe Hyperbilirubinemia: A Rare Complication Of Lyme Disease
Lin Zheng
1Internal Medicine Residency Program, Inspira Medical Center in Vineland, Vineland, NJ 08360, USA
2Division of Hospital Medicine, Department of Medicine, Cooper Medical School of Rowan University, Camden, NJ 08103, USA
Abstract
Gastrointestinal signs and symptoms are common in the early stages of Lyme disease. However, hyperbilirubinemia from Lyme disease is extremely uncommon. There are only two case reports in literature attributing Lyme disease to hyperbilirubinemia. Here we report a case of severe hyperbilirubinemia as the presenting symptom of Lyme disease. Other plausible etiologies have been ruled out after extensive workups, including liver biopsy. His hyperbilirubinemia gradually resolved after being started on doxycycline. With high incidence of Lyme disease, it should be considered for patients who present with hyperbilirubinemia in endemic areas with possible tick exposure.
1. Introduction
Lyme disease is a multisystemic infection caused by the tick-borne spirochete, Borrelia burgdorferi. Gastrointestinal involvement, such as acute hepatitis, could present in the early stages of Lyme disease . However, hyperbilirubinemia secondary to Lyme disease is extremely uncommon. There are only two case reports in literature attributing Lyme disease to hyperbilirubinemia one of which was in a pediatric patient . Here we present a rare case of hyperbilirubinemia secondary to Lyme disease.
2. Case Presentation
3. Discussion
Conflicts of Interest
What Every Dog Owner Should Know About Preventing Diagnosing And Treating This Tricky Tick
Most people think of Lyme disease being caused by ticks and thats partly true. The organism that actually causes Lyme disease is a spirochete bacteria called Borrelia burgdorferi ticks just pick up, carry around, and transmit the bacteria into the creatures they feed upon. The best way to prevent your dog from getting Lyme disease, then, is to prevent his exposure to ticks. Sound easy? Anyone whose dog has ever had Lyme disease can tell you that it aint necessarily so.
Lyme disease is named for Lyme, Connecticut, the town where it was first discovered. While most common in the northeastern United States, Lyme exposure has been recorded in all 48 of the continental United States. Lyme is most common in the northeast, upper Midwest, and parts of California, but can be present anywhere that Ixodes ticks are found which is just about everywhere. The Companion Animal Parasite Councils website has an interactive map that shows how many Lyme disease tests were performed and how many animals tested positive in each state.
Read Also: Lyme Disease And Massage Therapy
Nerve And Brain Repair
Glutathione is found in every cell of our body. By lowering oxidizing agents and free radicals, it allows for normal cell repair functions to occur. In this way it is the master repair agent of a cell. Excess cell damage and decreased cell function can occur from Lyme germs and other stressors. Under assault there is greater cell production of oxidizing agents and free radicals. Ultimately these damage the cell power factories called mitochondria. Without power cells can not heal. And without adequate glutathione, mitochondria cannot heal as free radicals and oxidizing agents continue to bombard these cell power plants.
The problem in chronic infection states like Lyme is the cell glutathione levels eventually become too low trying to keep up with mitochondria and cell injury caused by Lyme germs and the coinfections. This is particularly a problem in nerve cells.
Filling up a cell’s glutathione gas tank can help nerve cells repair and recover. In my experience I have seen marked improvements in thinking and neuropathy when I used glutathione with my patients. For more information on this see My Brain Isn’t Working …. I Think.
Lyme Disease Treatment For Dogs
According to Justine A. Lee, DVM, DACVECC, DABT, of St. Paul, Minnesota, the decision to treat should be based on the presence of clinical signs, breeds at risk for developing life-threatening chronic effects , and presence of proteinuria or microalbuminuria. Dogs with clinical signs should be treated to provide relief, and breeds at higher risk of developing Lyme nephritis should be treated as a preventative measure.
Proteinuria and microalbuminuria are signs of kidney damage, and so suggest the potential for Lyme nephritis. Proteinuria is considered significant only in the absence of a urinary tract infection , so a UTI must be ruled out before proceeding.
Microalbuminuria cant be measured with a standard urinalysis it requires special testing, which is unnecessary if proteinuria is seen. It can also be caused by other types of infection or inflammation.
Doxycycline is the antibiotic of choice for most Lyme disease cases. Other options are amoxicillin, minocycline, and Convenia . The dogs clinical symptoms should resolve rapidly after starting treatment, but the full course of medication must be given to ensure that the infection has been completely cleared and all spirochetes killed.
Before doing a biopsy, discuss with your vet how likely the results are to change treatment and prognosis. Kidney biopsies can damage the kidneys and rarely impact treatment or prognosis. Glomerulonephritis can also be diagnosed via urine protein:creatinine ratio.
Also Check: Does Lyme Disease Stay With You Forever
What Is Lyme Disease
Lyme disease is an infectious disease caused by the bacteria Borrelia burgdorferi. B. burgdorferi is transmitted to humans by a bite from an infected black-legged or deer tick. The tick becomes infected after feeding on infected deer, birds, or mice.
A tick has to be present on the skin for at least 36 hours to transmit the infection. Many people with Lyme disease have no memory of a tick bite.
Lyme disease was first recognized in the town of Old Lyme, Connecticut, in 1975. Its the most common tickborne illness in Europe and the United States.
People who live or spend time in wooded areas known for transmission of the disease are more likely to get this illness. People with domesticated animals that visit wooded areas also have a higher risk of getting Lyme disease.
How Much Does The Test Cost
The price for ALP testing can vary based on where you live, the location where you have your blood sample taken, whether ALP is tested alone or with other measurements, and whether you have health insurance. Costs for ALP isoenzyme testing may be different than costs for standard ALP tests.
Technician fees for the blood draw, laboratory fees, and charges for office visits can all be included in the cost of an ALP test. Health insurance often covers most or all of these costs when the test is prescribed by your doctor, but you may need to pay a deductible or copay.
At-home tests are not covered by insurance and may be available for less than $150.
For details about what your out-of-pocket costs would be for alkaline phosphatase tests, check directly with your doctors office and your health insurance provider.
Don’t Miss: Dr Nader Soliman Lyme Disease
News: Persistent Lyme Infection May Cause Hepatitis
The CDC keeps asking for credible scientific evidence that persistent infection may cause problems in these patients. We have delivered that evidence on a silver platter.
Press release from Union Square Medical Associates:
San Francisco, CA June 22, 2014
A new study suggests that persistent infection may cause hepatitis in Lyme disease. The study was published in the online journal Research Open Access.
Lyme disease is a tickborne infection caused by Borrelia burgdorferi, a type of corkscrew-shaped bacteria known as a spirochete . Last summer, the Centers for Disease Control and Prevention announced that Lyme disease is much more common than previously thought, with over 300,000 new cases diagnosed each year in the United States. That makes Lyme disease almost twice as common as breast cancer and six times more common than HIV/AIDS.
Our findings show that persistent infection can cause problems in Lyme disease, said Marianne Middelveen, lead author of the study published online this week. We have used sophisticated diagnostic techniques to show that the Lyme spirochete can attack the liver despite antibiotic therapy.
The presence of the Lyme spirochete in blood and liver tissue supports persistent infection, said Dr. Mayne. It looks like antibiotic treatment failed to eradicate the disease in this patient.
Reference: Research Open Access 2014 1:875. Read the full article: .
Cxcr3 Expressing T Cells Are Decreased In Lyme Disease And Co
The chemokines CXCL9 and CXCL10 bind to a common receptor CXCR3 expressed largely on T cells . We reasoned that high serum levels of these chemokines may drive T cells into inflamed tissues and as a result levels of CXCR3 expressing T cells may be altered during acute Lyme disease. Levels of CXCR3+ CD4 T cells were determined by polychromatic flow cytometry , and found to be significantly lower in the blood of patients with acute Lyme disease versus controls . In addition, serum levels of CXCL10 and CXCL9 were inversely related to the frequency of CXCR3+ CD4+ T cells in the peripheral circulation.
CXCR3 Expressing CD4+ T cell levels correlate with serum CXCL10.
Panel A: CXCR3 expressing CD4+ T cells were detected using polychromatic flow cytometry. Displayed is a representative plot. Panel B: The frequency of CXCR3+CD4+ T cells among total CD4+ PBMCs were determined in Lyme patients prior to treatment and healthy controls . Levels of CXCR3+CD4+ T cells were lower in cases vs. controls at pre-treatment . Panel C. The levels of blood CXCR3+CD4+ T cells were negatively correlated CXCL10 serum levels in pretreatment early Lyme disease cases .
You May Like: Full Recovery From Lyme Disease