Western Blot Test Interpretation Of The Results
There are several techniques for performing a test, and each laboratory uses different performance criteria. The Western Blot test should not be interpreted without referring to the symptoms of the disease being diagnosed. It is therefore important that the result is determined by a physician who specializes in treating the disease in question.
Simply interpreting the results of the Western Blot test is based on the observation of bands. The more there are, the greater the certainty of the diagnosis of the disease. Already 3 bands in the Western Blot test prove the presence of pathogens in the body, and 6 give absolute certainty.
In the case of Lyme disease, the IgM bands in the Western Blot test carry much more information. They are most active shortly after infection and also in chronic disease. They usually mean active Lyme disease. On the other hand, the detected IgG antibodies inform about a past infection or active, chronic Lyme disease.
We Implement Proven Measures To Keep Your Data Safe
At HealthMatters, were committed to maintaining the security and confidentiality of your personal information. Weve put industry-leading security standards in place to help protect against the loss, misuse, or alteration of the information under our control. We use procedural, physical, and electronic security methods designed to prevent unauthorized people from getting access to this information. Our internal code of conduct adds additional privacy protection. All data is backed up multiple times a day and encrypted using SSL certificates. See our Privacy Policy for more details.
Popular search
What Does It Mean If Your Lyme Disease Ab Blot Result Is Too High
Two types of antibodies are detected in the Western blot test.
IgM antibodies reflect a relatively recent infection. IgG antibodies in contrast are a sign of an older infection.
IgM antibodies usually disappear after eight weeks post-exposure. IgG remains in the serum for a very long time.
In the Western blot test there are three bands for IgM and 10 bands for IgG.
Here is the important part:
– You need to have 2 out of 3 for the positive IgM result
– Or you need to have 5 out of 10 for the positive IgG result.
This marker is called Lyme Disease AB , Blot and is an aggregate marker for the three IgM results. So if this marker is positive you have at least 2 out of 3 of the IgM markers positive.
Here is the 2nd important part when it comes to a diagnosis:
If a person doesn’t have signs or symptoms of Lyme disease, then the person does not have Lyme disease as the definition of disease requires symptoms.
What could some of those symptoms be?
What are the symptoms of Lyme disease?
Lyme disease symptoms are wide-ranging, with more than a hundred different symptoms recorded. Symptoms can also change over time, as the bacteria spreads throughout the body. To make things more confusing, Lyme disease symptoms will also vary from patient-to-patient. Lyme disease can mimic hundreds of other conditions since its symptoms mirror many medical problems such as multiple sclerosis, arthritis, chronic fatigue syndrome or lupus, and is sometimes known as The Great Imitator because of this.
Read Also: Cottages For Sale In Old Lyme Ct
Traditional Lyme Disease Tests Are Not Specific Enough
Lyme disease is caused by the spiral-shaped bacteria Borrelia. There are multiple species and strains of Lyme borreliae . Therefore, tests must be targeted to these multiple species and strains in order to be able to detect them. If a patient is infected with a species or strain of Lyme borreliae that their test cant detect, they will get a false-negative test result and thus risk missing their diagnosis. This can be costly and dangerous.
Many ELISA and Western blot Lyme disease tests are only equipped to detect one strain of one species of Borrelia: Borrelia burgdorferi B31 . This means that those tests are missing infections caused by other strains and/or species of Lyme borreliae.
In one internal study designed to test the validity of the IGeneX ImmunoBlot against traditional Western blot tests, a total of 132 patients were tested by both Lyme Western blots and Lyme IB. 43 patients were seropositive on the ImmunoBlot, and 14 were positive on standard Western blots prepared from a mixture of two species for Bb ss B31 and 297. Thus 29 of the 43 patients tested negative on Western blots i.e., the Western blot totally missed their infections with strains other than Bb ss B31 and 297.
With such limited tests, patients infected with non-B31 species and strains e.g., B. mayonii, B. californiensis, or European species are at risk of receiving false negatives and missing the chance to treat their diseases.
Is There Anything Else I Need To Know About Lyme Disease Tests

At-home test kits for Lyme disease are available. To do these tests, you usually collect a drop of blood from your finger and send it to a lab for testing. If you want to do an at-home test, it’s important to talk with your provider first. Some at-home tests may use lab methods that aren’t proven to work, so your results may not be accurate.
Recommended Reading: How Long Does Lyme Disease Last In Humans
Western Blot Test Lyme Co
Western Blot is not suitable for identifying Lyme co-infections. It gives a vague answer, exposing the patient to costs. In this case, it is better to use the reimbursable ELISA test, which will also be more precise.
We also recommend Shipping PCR test for Lyme disease and co-infections , which you can conveniently and safely buy at Medonet Market to send the tick to the laboratory.
What Is The Best Way To Remove A Tick And What If I Did Not Get The Entire Tick Out
The Centers for Disease Control provides this information about removing a tick: Remove a tick from your skin as soon as you notice it. Use fine-tipped tweezers to firmly grasp the tick very close to your skin. With a steady motion, pull the ticks body away from your skin. Then clean your skin with soap and warm water. Throw the dead tick away with your household trash. Avoid crushing the ticks body. Do not be alarmed if the ticks mouthparts remain in the skin. Once the mouthparts are removed from the rest of the tick, it can no longer transmit the Lyme disease bacteria. If you accidentally crush the tick, clean your skin with soap and warm water or alcohol. Dont use petroleum jelly, a hot match, nail polish, or other products to remove a tick. View a diagram of how to remove a tick.
Read Also: What Type Of Doctor Treats Lyme Disease
Testing For Lyme Disease
Although there are several testing strategies that can assist in making a diagnosis of Lyme disease , serology is currently the only standardized laboratory testing available. The following describes the different test platforms used for the laboratory diagnosis of Lyme disease. The advantages and limitations of each are presented in Table 2.
Antibody Test Quick Facts
- The timing of the test is crucial. It takes 4-6 weeks for the body to develop enough antibodies to show up on a test, so if you test too early, you could get a false negative.
- Most antibody tests are blood tests. Also known as serological tests, they require that a patient have a small sample of blood taken, and they detect antibodies in the patients serum or plasma.
- Not every test is able to detect every type of Lyme Borrelia. In fact, most tests like those recommended by the CDC are only designed to detect one or two species of Borrelia, even though at least 18 distinct types of Lyme-causing Borrelia are active in North America. This is a major cause of mis- and missed diagnoses.
You May Like: Old Lyme Beach Cottage Rentals
Western Blot Test When To Do It
Antibodies do not appear in the body immediately after infection. During this time, the so-called serological window where Western Blot testing is not reliable. In the case of Lyme disease, the serological window is 4 weeks. Only after this time can the ELISA test be performed, followed by the Western Blot test.
Long after this time, the Western Blot test result may be false-negative as the amount of antibodies fluctuates from time to time. Therefore, in the case of serious suspicions of the disease, it should be repeated every few weeks so as to find the right time for the appearance of antibodies. The reliable result of the Western Blot test may appear even in the fifth time.
Sometimes antibiotic therapy helps to achieve realistic results and confirm the infection by the Western Blot test. Taken by antibiotics, they modify the immune system, while increasing the number of produced antibodies. However, performing the Western Blot test during antibiotic therapy will not give the desired results yet. This may happen several weeks after your treatment has finished.
Common Antibody Tests And How They Work
ELISA
The Enzyme-Linked Immunosorbent Assay is the first-tier test, or screening test, recommended by the CDCs two-tier testing strategy. This plate-based test works by taking a sample of the patients blood and then placing it in a petri dish containing a specific Lyme antigen. If the patients sample contains Lyme antibodies, they will bind to the antigens in the petri dish. This process is revealed when the lab technician adds an enzyme to the dish and observes the reaction.
The ELISA has been heavily criticized in the Lyme community for its limitations as a screening test. In two-tier testing, screening tests should be as sensitive as possible. If the test isnt sensitive enough, it can fail to detect infections. Since the CDC only recommends performing a Western Blot if the first test was positive, someone who has Lyme that was not detected in their screening test can be left with an infection that will worsen and become much harder to treat.
Recommended Reading: Can Lyme Disease Cause Dementia
Lyme Igg Western Blot
Based on internal validation studies, IGeneX established the following criteria:
Positive If:two or more of the following bands are present: 23-25, 31, 34, 39, 41 and 83-93 kDa.
Exception Indeterminate: If only bands 31 and 41kDa are present.
Note: There are two Borrelia antigens present at 31kDa position on the Western blot strip. One is a very specific marker of Lyme disease whereas the second antigen is a house keeping gene that can also present in some viruses and bacteria, including other spirochetes. It is also present in some viruses and other spirochetes. Therefore, when there a positive signal at position 31 kDa band, there is 50% chance that the positive signal is due to presence of Lyme specific antibody in patient serum. Thus, the following confirmation test of an Indeterminate Western Blot IgG result is recommended: Test # 489 31 kDa Epitope Test IgG.
Negative If: test result does not meet either positive or indeterminate criteria.
CDC/NYS Criteria:
The Lyme IgG Western Blot is considered positive if 5 of the following 10 bands are present: 18, 23-25, 28, 30, 39, and 41, 45, 58, 66 and 83-93kDa.
Western Blot Test Indications
Western Blot is used as the second step in disease diagnosis. The first is the ELISA test. The difference between these diagnostic test methods is in the characteristics of the results the Western Blot shows a qualitative one, and the ELISA gives quantitative results, alerting that there are some antibodies in the patients blood. For this, it uses a certain scale. However, the Western Blot test shows which infection has occurred and at what stage the disease progresses. An indication for its use is a positive ELISA test result. Negative categorically eliminates the patient from further diagnosis.
You May Like: Which Tick Carries Lyme Disease
High Endemicity Screening Of A Child
A healthy child from an area of high endemicity receives an annual physical. The mother notes that the child enjoys playing in the backyard, which is adjacent to a heavily wooded area.
Serologic testing should not be ordered because the child is asymptomatic. A false-positive test result would expose the child unnecessarily to the risks of treatment. In this scenario, the probability that a positive test represents true infection is less than 25 percent.
Recommended Reading: How To Treat Lyme Naturally
The Diagnostic Accuracy Of Tests Compared To Clinical Diagnosis
Two-tier serological test vs. clinical diagnosis
Thirteen studies evaluated the two-tier serological test protocol for diagnosis of LD at different stages of disease and after antibiotic therapy. Table 2 provides the meta-analytic summaries demonstrating low sensitivity, 46.3% , for early LD patients and increasing sensitivity with stage 2, 89.7% , and stage 3, 99.4%H LD. There was relatively high specificity across control groups. Most false positives within the control groups were patients with diseases known to produce antibodies that cross-react in serological tests for B. burgdorferi. Nine studies presented results for two-tier serological testing where at least one of the tests was not FDA licensed , Table 2. Heterogeneity analysis of sensitivity and specificity on the impact of using non-commercial tests was not significant. At the early stage of LD the two-tier testing method was good for ruling in LD if the patient tested positive, but had very poor predictive value for ruling out LD, which is why it is recommended to retest after 30 days . However, for convalescent patients treated at stage 1 LD sensitivity remained low even after 30 days.
Read Also: Is Lyme Disease An Autoimmune Disease
Bartonella Species Igg Western Blot
Bartonellosis is caused by Bartonella species, e.g. B. elizabethae, B. vinsonii, B. henselae, and B. quintana. Bartonellosis is a complex and progressively systemic illness which tends to mimic other diseases and is most likely known to be a co-infection with Lyme disease. Therefore, determination of specific antibodies is helpful in the diagnosis of Bartonellosis. The Bartonella IgG Western Blot panel detects specific antibodies in human serum to B. elizabethae, B. vinsonii, B. henselae, and B. quintana. IGeneX interpretation is based on internal validation studies.
Interpretation:Positive: Presence of 2 or more specific antibodies to Bartonella antigen detected. If positive, species is determined.Indeterminate: Presence of one specific antibody to Bartonella antigen detected.Negative: No specific antibody to Bartonella antigen detected.
Disclaimer: This test was developed and its performance characteristics determined by IGeneX, Inc. It has not been cleared or approved by the FDA. The FDA has determined that such approval is not necessary. The test is used for clinical purposes and should not be regarded as investigational or for research. IGeneX, Inc. is licensed by CMS and NYS to perform high complexity clinical laboratory testing.
Western Blot Test What Does The Test Look Like
The Western Blot test looks for antibodies produced by the body against specific bacteria, viruses or parasites. These antibodies fight against antigens on the surface of microorganisms. Western Blot detects IgM and IgG antibodies. The first are produced by the body as a result of the first contact with the pathogen, and the rapid increase in their number indicates a recent disease process. In turn, IgG antibodies are produced much later, reaching their peak around 6 months after infection. They can stay in the body for several years.
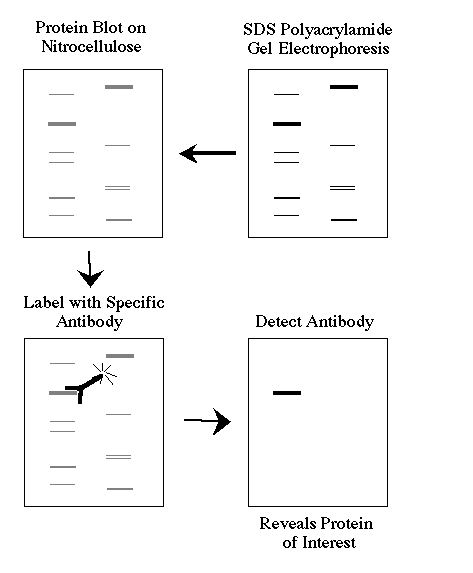
To perform the Western Blot test, the test persons blood serum is needed, as well as comminuted, killed culture bacteria. These, influenced by impulses of electric current, are broken down into fragments, including proteins, i.e. antigens. The next step in the Western Blot test is to transfer the antigens to a nitrocellulose membrane cut into strips and combine them with the patients blood serum. With the help of a special technique, the solution is stained, and the so-called stripes. Thus, the Western Blot test shows infection and the test is positive.
Also Check: Symptoms Of Lyme In Child
More About Western Blot Testing In North America
The IgG Western Blot test is designed to detect antibodies specific to Borrelia burgdorferi, the bacteria that cause Lyme disease. For Lyme disease in North America, a positive IgG Western Blot test requires at least 5 of 10 measured bands to be positive .
The scored IgG bands are 18 kDa, 24 kDa , 28 kDa, 30 kDa, 39 kDa , 41 kDa flagellin , 45 kDa, 58 kDa , 66 kDa, and 93 kDa.
The Lyme IgM Western Blot test measures 3 different types of antibodies. The North American IgM Western Blot is considered positive only if 2 of 3 IgM bands are positive .
The scored IgM bands are 24 kDa , 39 kDa , and 41 kDa .
According to the CDC, Depending upon the assay, OspC could be indicated by a band of 21, 22, 23, 24 or 25 kDA.
What Percent Of Cases Of Reasonably Proven Lyme Disease Present Without Erythema Migrans
According to the Centers for Disease Control , erythema migrans occurs in 60-80% of Confirmed cases. Under careful monitoring of patients who develop new onset symptoms, about 20% have systemic symptoms without a rash or other objective sign of Lyme disease .
To be considered a confirmed case by CDC for epidemiologic surveillance in the absence of a rash, a person has to have laboratory evidence of infection and at least one late manifestation of Lyme disease. Late manifestations of Lyme disease considered diagnostic are: joint swelling, facial palsy or other specific signs of nervous system involvement, or specific cardiac conduction defects. The CDC also has criteria for a probable case, defined as physician-diagnosed Lyme disease that has laboratory evidence of infection. Suspected cases without an EM are those with laboratory evidence of infection but no clinical information available.
Recommended Reading: Dumpster Rental Old Lyme Ct