Lyme Neuroborreliosis And Dementia
Lyme disease caused by B. burgdorferi sensu lato is transmitted by the bite of an infected tick of the species Ixodes. Specific associations exist in some areas between Borrelia species and vertebrate hosts . In Europe all the three genospecies, Borrelia burgdorferi sensu stricto , Borrelia garinii, and Borrelia afzelii, were isolated from humans. However, in the USA only B. burgdorferi s.s. has been identified. B. garinii and B. burgdorferi s.s. frequently cause
Lyme Disease Patients With Memory Problems
| The safety and scientific validity of this study is the responsibility of the study sponsor and investigators. Listing a study does not mean it has been evaluated by the U.S. Federal Government. Read our disclaimer for details. |
| Recruitment Status : Suspended First Posted : April 18, 2018Last Update Posted : April 18, 2018 |
| Device: Transcranial Direct Current Stimulator | Not Applicable |
Lyme disease is a tick-borne illness caused by Borrellia Bugdorferi after tick bite. This disease mostly presents with a skin rash which looks like bulls eye and therefore known as bulls-eye skin rash or Erythema Migrans. The standard of care of Lyme disease is a few weeks of antibiotics. Most of the patients do well after antibiotics treatment. However 10-20% of patients go on to develop persistent symptoms such as memory problems, fatigue and pain several months after the antibiotics treatment. Such symptoms are collectively known as Post Treatment Lyme Disease Syndrome. In this study we want to see if a device known as Transcranial Direct Current Stimulator is helpful in reducing these symptoms after Lyme disease treatment.
| No |
Fifteen subjects will be selected to take part in this study. All subjects must meet the following criteria:
Can Lyme Disease Cause Cognitive Dysfunction Or Dementia
The question of whether Lyme disease could cause dementia was addressed by Wormser and colleagues in an article entitled Lack of Convincing Evidence That Borrelia burgdorferi Infection Causes Either Alzheimer Disease or Lewy Body Dementia, published in the journal Clinical Infectious Diseases.¹
The authors reviewed a paper by Gadila et al.² which concluded that a Lyme disease infection might cause Lewy body dementia. The case described a 69-year-old woman who died 15 years after her initial infection with Lyme disease with a clinical diagnosis of Lewy body dementia.
The woman had initially presented with an erythema migrans rash, headache, joint pain, and fever. Her symptoms resolved with 10 days of doxycycline.
Over time, she developed a sleep behavior disorder, cognitive problems , photophobia, paresthesias, fasciculations, and myoclonic jerks. She initially improved with IV followed by oral antibiotics. But her condition later worsened.
The extensive workup at that time led to the diagnoses of both a REM behavioral disorder with verbalizations and movements and a neurodegenerative dementia characterized by expressive aphasia, visual agnosia, anomia, deficits in executive function and calculation, and mild memory problems.
She passed away 15 years after the onset of her illness.²
An autopsy revealed the presence of Borrelia burgdorferi in the brain and spinal cord tissue of the patient.
Can Lyme disease cause dementia?
Inside Lyme Podcast Series
References:
Read Also: Does Lyme Disease Last Forever
Long Covid Could Reveal Clues To Alzheimers Lyme Disease
Last week, the U.S. Congress failed to approve $15 billion needed to continue Covid-19 precautions, even though todays low case counts are likely to rise, as they are in Europe, with the sub-variant called BA.2. Weve learned that some expensive mitigation measures, such as deep cleaning, are a waste of money, and could be scrapped, but funding for studying Covid should increase not just for prevention measures and vaccines, but for research into the long-term consequences of infection.
Some people who got Covid-19 early in the pandemic still havent recovered, and what looked like long Covid might, for some people, be a permanent condition if no treatment is found. The lingering symptoms are often different from those associated with acute infection. Patients report changes in memory, trouble thinking clearly or concentrating, mood disorders, sleep disturbances, changes in balance and gastrointestinal problems. Some have a form of fatigue that can get much worse with physical or mental exertion.
The good news is that some of the countrys top medical researchers have jumped on this problem and are gaining momentum. What they learn is likely to apply to other medical problems. Take the work of Mark Albers, a neurologist at Massachusetts General Hospital who had been uncovering the weird relationship between loss of sense of smell and Alzheimers Disease. Now hes expanded his research to learn about similar changes in Covid-19 patients.
Investigating Connections Between Lyme Disease And Dementia

Recently, the National Institute on Aging, as part of the National Institutes of Health , approved the acceptance of research to study the role of microbes in causing dementia.
This announcement came right on the heels of a recent UK study detecting bacteria in the brains of Alzheimers patients.
This announcement was also the first step in allowing the NIH and Centers for Disease Control to grant research money to study the role of diseases like Lyme disease and tick-borne relapsing fever in facilitating the process and progression of various dementias, including Lewy body dementia and Alzheimers dementia.
Recommending specific efforts to look for Lyme bacteria in Alzheimers brains was a very important first step.
Don’t Miss: Medicine Used For Lyme Disease
Detecting Borrelia Spirochetes: A Case Study With Validation Among Autopsy Specimens
- 1Division of Immunology, Tulane National Primate Research Center, Tulane University Health Sciences, Covington, LA, United States
- 2Department of Psychiatry, Columbia University, New York, NY, United States
- 3Division of Molecular Imaging and Neuropathology, New York State Psychiatric Institute, New York, NY, United States
- 4Macedonian Academy of Sciences and Arts, Skopje, Macedonia
- 5Department of Pathology and Cell Biology, Columbia University, New York, NY, United States
Does Alzheimer’s Make The Brain More Susceptible To Infection
The blood-brain barrier protects the brain by controlling what substances can pass from the blood into brain tissue. In Alzheimer’s disease, the blood-brain barrier is damaged, particularly in the brain region affected by Alzheimer’s.
Evidence suggests that inflammation, the Alzheimer’s hallmark amyloid protein and the ApoE4 gene, which are all linked to Alzheimer’s disease, can contribute to the breakdown of the blood-brain barrier. Once it has been weakened, bacteria, viruses, and other harmful substances can get through into the brain more easily. This may explain why certain viruses and bacteria, such as herpes and spirochetes, are more common in the brains of people with Alzheimer’s.
Read Also: Lyme Disease And Back Pain
Kris Kristofferson’s Lyme Disease Misdiagnosed As Alzheimer’s
Actor and songwriter Kris Kristofferson and some of those closest to him are speaking out about his health problems and their surprising cause.
Kristoffferson struggled with memory problems in recent years and was told he had Alzheimer’s disease, but it appears he was misdiagnosed and all along has actually been suffering from the tick-borne illness Lyme disease.
Articles in Rolling Stone and the entertainment magazine Closer Weekly reveal that the 80-year-old — whose songs have been covered by the likes of Johnny Cash, Janis Joplin and Elvis Presley — has struggled through a years-long medical odyssey.
Kristofferson and his wife Lisa told Rolling Stone that for years, doctors had been telling him that his increasingly debilitating memory loss was due to either Alzheimer’s or to dementia brought on by blows to the head from boxing and playing football and rugby in his teens and early twenties.
“Some days, Kristofferson couldn’t even remember what he was doing from one moment to the next,” the site said of the actor who starred alongside Barbra Streisand in the 1976 film “A Star is Born,” and who’s known for his roles in the Blade movies and other films.
Earlier this year, though, a doctor decided to test Kristofferson for Lyme disease, which can cause neurological problems, including memory issues and what some describe as “brain fog,” as well as a broad range of other symptoms. The test came back positive.
> > > 1tsp Of This Powder Stops Brain Fog And Rejuvenates Brain Cells
Eating a healthy diet is an excellent memory loss remedy. It should consist of fruits and vegetables, as well as whole grains and low-fat proteins. Avoid alcohol and drugs, which can also cause confusion and memory loss. Its important to follow your doctors recommendations, and review your medications regularly. If you suspect a medical condition, you may want to consult a medical professional for a diagnosis and treatment. This way, a physician can prescribe the right medication. Can Lyme Disease Cause Dementia
Eating a healthy diet is an effective memory loss remedy. A diet rich in fruits and vegetables can improve your memory. A balanced diet can also help you to retain information longer. Try to consume at least five servings of these foods a day. The berries contain anthocyanins and flavonoids, which can be very helpful in fighting memory loss. A study of 16,000 women found that those who ate more berries were less likely to suffer from cognitive decline. Turmeric root contains a substance called curcumin, which is found in high concentrations. This compound is a powerful antioxidant that has anti-inflammatory effects.
You May Like: Cost Of Western Blot Test For Lyme
Rnascope Is A Sensitive Technique For Finding Viable Pathogen But Requires Freshly Prepared Tissue
Figure 8. Validation of RNA integrity on Fresh frozen NHP frontal cortex brain tissue using RNAscope assay. NHP tissue was stained with a 3-plex positive control probe POLR2A targeting DNA-directed RNA polymerase II RPB1, PPIB targeting cyclophilin B, and UBC that targets Ubiquitin C. In terms of relative expression levels, UBC is highest, PPIB is considered a moderate-high, POLR2A is moderate-to low expressor target. Successful staining has 49 dots per cell of PPIB/POLR2A and UBC of 1015 dots per cell. PPIB is considered a standard to determine the RNA quality of brain samples. Represents red fluorescence, indicating the specificity of PPIB, whereas, displays a far-red puncta targeting UBC gene. Absence of POLR2A signal in represents, quality of RNA being partially compromised. A merge image of all the channels can be seen in . White arrows were pointing toward the fluorescence puncta and orange arrows toward autofluorescence of the tissue.
The Patient Harbored Borrelia in the Amygdala and Spinal Cord
Tissue slices adjacent to the autopsy tissue specimens that were positive for DNA were stained for the presence of persisters. For this, slides were stained with the primary rabbit polyclonal antiB. burgdorferi antibody and a goat anti-rabbit IgG-Alexa Fluor 488 secondary antibody. An intact Borrelia spirochete with the expected morphology was identified within fixed tissue of the spinal cord . The spirochete appeared to be adjacent to vasculature.
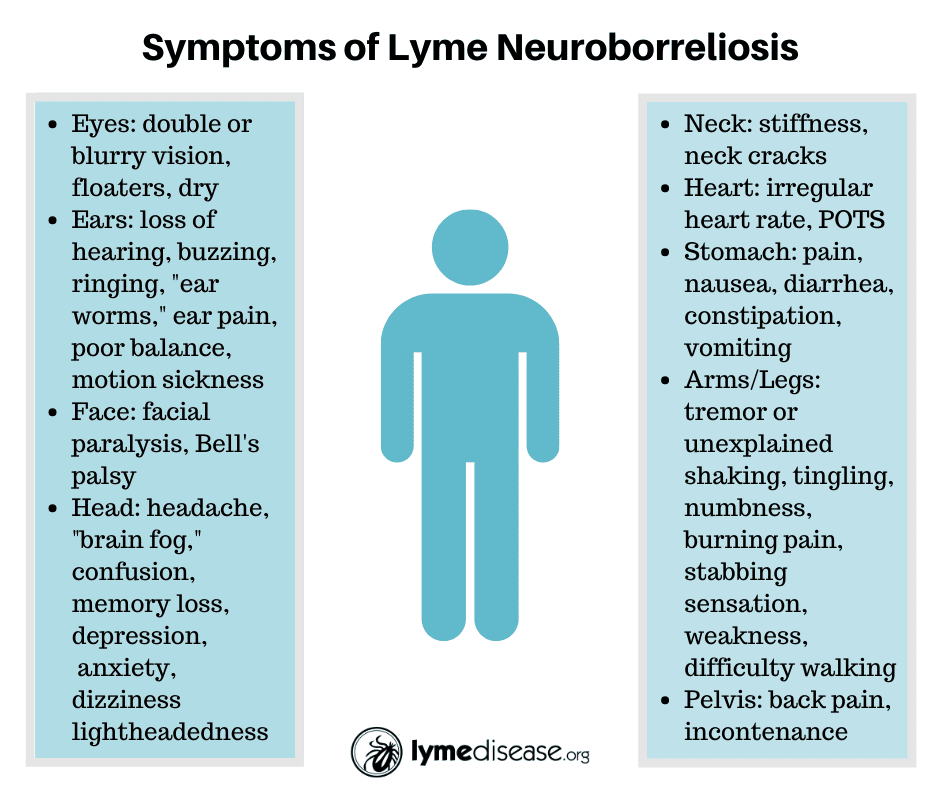
What Lyme Disease Does To Your Brain
Lyme disease is a bacterial infection that you catch when an infected deer tick bites you. The first symptoms can appear within a few days or weeks. They include a target-shaped rash, fatigue, fever, swollen lymph nodes, muscle aches, and headache. Often, doctors promptly recognize and treat Lyme disease with antibiotics. But when treatment is delayed, the infection can spread to other areas, including the nerves, liver and eyes. It can also spread to the central nervous systemthe brain and spinal cordand cause the following problems.
Recommended Reading: How To Relieve Pain From Lyme Disease
The Case Of A Retired Defence Intelligence Agency
The Washington Post also reported a case from an officer who has worked at the Defense Intelligence Agency.
After surviving Leukaemia, the 81-year man was told that he had dementia. Sandra Boodman, the reporter, wrote that doctors were convinced that the retired agent was battling a fatal type of dementia that was rapidly progressive.
This led him to become delusional, moody, childish, and confused, something that he was not when he was a competent man.
This was a wrong diagnosis.
Later on, doctors discovered that he had Lyme meningoencephalitis when he started having challenges with walking, had tremors in his arms, and was also suffering from incontinence.
After a positive diagnosis for Lyme disease, he immediately started antibiotics for treatment and went on to make a full recovery.
Study Finds Evidence Of Persistent Lyme Infection In Brain Despite Aggressive Antibiotic Therapy
Tulane University researchers found the bacterium that causes Lyme disease in the brain tissue of a woman who had long suffered neurocognitive impairment after her diagnosis and treatment for the tick-borne disease. The presence of the corkscrew-shaped Borrelia burgdorferi spirochetes in the former Lyme disease patients brain and spinal cord were evidence of a persistent infection.
The findings were published in Frontiers in Neurology.
The 69-year-old woman, who experienced progressively debilitating neurological symptoms throughout her illness, decided to donate her brain to Columbia University for the study of the disease as her condition worsened. While she had first experienced the classic symptoms of Lyme disease 15 years prior and was treated accordingly after her diagnosis, she experienced continual neurological decline including a severe movement disorder and personality changes, and eventually succumbed to Lewy body dementia. Lewy body dementia is associated with abnormal protein deposits in the nerve cells of the brain which can cause impairment in thinking, movement and mood, leading to a severe form of dementia.
These findings underscore how persistent these spirochetes can be in spite of multiple rounds of antibiotics targeting them,
Monica Embers
This is the first time researchers have identified a possible correlation between Lyme disease infection and Lewy body dementia.
Also Check: How Does Lyme Disease Start
Pathological Manifestations Of Neurosyphilis
The clinical and pathological manifestations of neurosyphilis occur in three stages .
Following an incubation period of about 3 weeks , the typical primary chancre usually begins as a single painless papule which rapidly becomes eroded and indurated with a characteristic cartilaginous consistency on palpation. The histology shows inflammatory infiltrates consisting chiefly of lymphocytes , plasma cells, and histiocytes. Obliterative
Tulane Researcher Asks Could Chronic Lyme Contribute To Alzheimers Dementia
In 2019, the late-great-science-writer Sharon Begley wrote an insightful article, The maddening saga of how an Alzheimers cabal thwarted progress toward a cure for decades.
Begleys reporting described how a powerful group of researchers became fixated on one theory of Alzheimers causation at the expense of all others.
Their hypothesis: that Alzheimers cognitive decline was caused by neuron-killing, beta-amyloid protein clumps in the brain, and that if you dissolved the clumps, the disease process would stop.
As this theory hit a brick wall, Begley showed how the actions of the cabal harmed patients: for decades, believers in the dominant hypothesis suppressed research on alternative ideas: They influenced what studies got published in top journals, which scientists got funded, who got tenure, and who got speaking slots at reputation-buffing scientific conferences.
One of these researchers is Monica Embers, PhD, an associate professor of microbiology and immunology at the Tulane National Primate Research Center. Shes also the leading expert in identifying treatments that can eradicate Lyme bacteria infections in nonhuman primates, our closest mammalian relatives.
Read Also: Do Neurologists Treat Lyme Disease
Dementia & Alzheimer’s Disease
There has been a lot of interest in the topic of Lyme disease and dementia in the medical world.
This is after several high-profile cases in the media pointed out to experts that there is a need to consider Lyme disease as one of the possible causes of dementia.
We can describe Lyme disease as a bacterial infection that comes about when an infected black-legged tick bites a person.
This tick is also referred to as a deer tick.
Early detection of the disease is vital because taking antibiotics cures the illness.
Regrettably, when it is not detected early enough, the infection grows worse, weakening the immune system and resulting in an array of inflammatory responses.
> > > Breaking: Scientist Finds 1 Way To Fix Alzheimer And Memory Loss
A doctor will perform a physical exam to evaluate your mental processes. He or she will also ask you about any medications youre currently taking and any stressful situations youre facing. Your memory loss provider may also ask you about your symptoms and ask you to take notes on how youre feeling. The doctor may recommend that you get an appointment with a neuropsychologist. A neuropsychologist can help you figure out the best way to treat your memory loss.
A doctor will conduct a physical exam to determine the exact cause of your memory loss. He or she will also ask you about your medical history and whether youve experienced other forms of memory loss. After your medical history, your provider will discuss your options for treatment. If youre experiencing severe symptoms of memory loss, you should seek out a professional. It will help you get the right kind of care for your specific situation. So, take action today.
A healthcare provider will perform a physical exam to assess the condition of your memory. He or she will ask you about your family and friends and any medications youre taking. Once he or she has established the root cause, a proper treatment will be given. If you have a mild form of memory loss, you can still function independently and perform everyday tasks. If your symptoms are more severe, you may need to see a medical professional.
You May Like: Can Lyme Disease Cause Low Platelet Count
Dementia Doesn’t Always Mean Alzheimer’s
Dementia is any memory loss or thinking problem caused by changes in your brain. Alzheimer’s is just one type. Your memory also can be harmed by many other health issues, such as a stroke, Parkinson’s disease, or a buildup of fluid on your brain.
If you notice symptoms that have you concerned, see a doctor right away. They’ll give you a thorough exam that may include taking a sample of your blood for testing, brain imaging, and neurological testing to figure out what’s going on with your health and get you help.