What Is Lyme Arthritis
Lyme arthritis occurs when Lyme disease bacteria enter joint tissue and cause inflammation. If left untreated, permanent damage to the joint can occur. Lyme arthritis accounts for approximately one out of every four Lyme disease cases reported to CDC. Because of reporting practices, this statistic may overstate the frequency of arthritis among patients seen in routine clinical practice.
What Are The Signs And Symptoms Of Lyme Disease
Early symptoms usually appear within 3 to 30 days after the bite of an infected tick. In 60-80 percent of cases, a circular bull’s eye rash about two inches in diameter, called erythema migrans, appears and expands around or near the site of the tick bite. Sometimes, multiple rash sites appear. One or more of the following symptoms usually mark the early stage of Lyme disease: chills and fever, headache, fatigue, stiff neck, muscle and/or joint pain, and swollen glands. If Lyme disease is unrecognized or untreated in the early stage, more severe symptoms may occur. As the disease progresses, severe fatigue, a stiff aching neck, and tingling or numbness in the arms and legs, or facial paralysis can occur. The most severe symptoms of Lyme disease may not appear until weeks, months or years after the tick bite. These can include severe headaches, painful arthritis, swelling of the joints, and heart and central nervous system problems.
Health’citizen Scientists’ Take On Tick
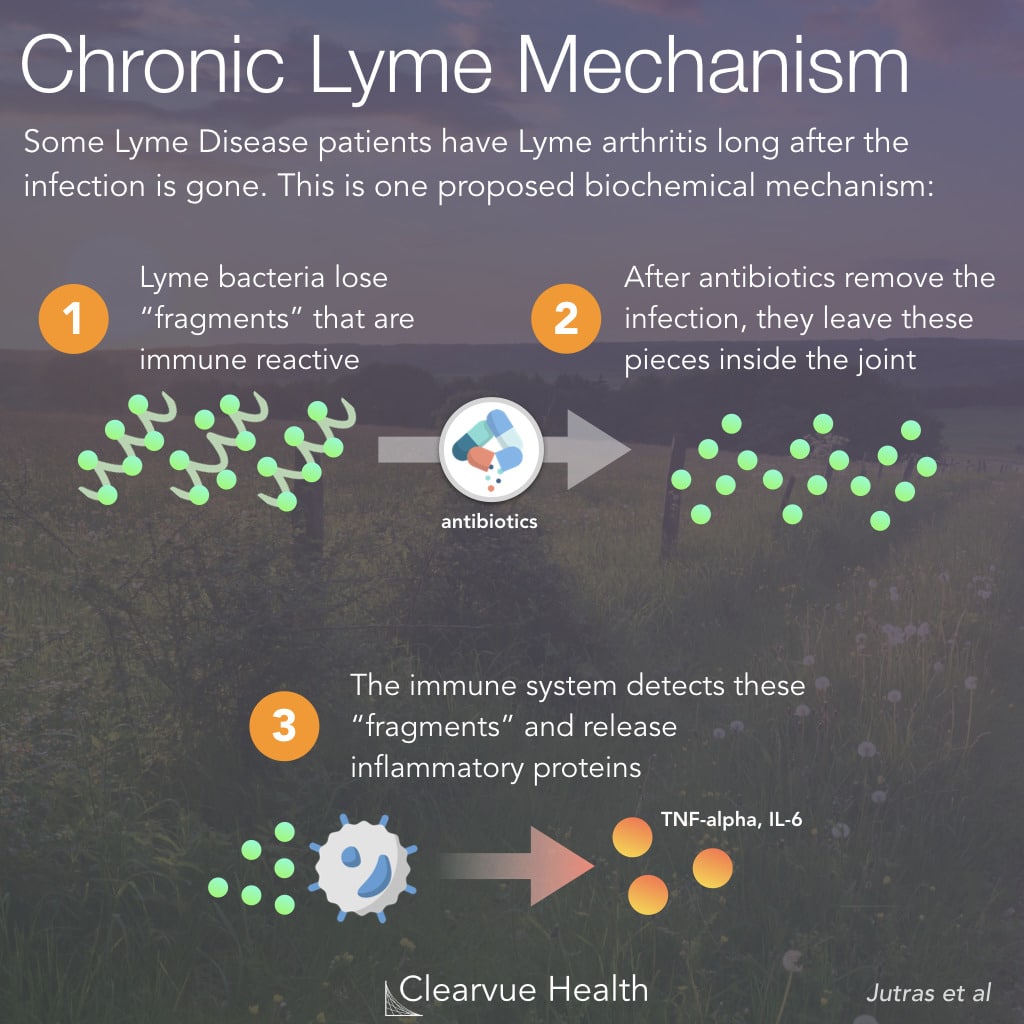
As for the new study, it leaves open the question of whether there are still bacteria in the joints of patients with Lyme arthritis, Lewis said. The authors think that the peptidoglycan remains in synovial fluid after the pathogen is gone. My guess is that the pathogen remains in the joints and sheds the antigen. It would be good to know how things really are.
When it comes to finding physical explanations for patient symptoms, its not necessary to determine whether PTLDS is caused by lingering bacteria or to a malfunctioning immune system, said Dr. Peter Novak, an assistant professor of neurology at Harvard Medical School and director of the autonomic laboratory at Brigham and Womens Hospital. Novak, who also was not involved in the new study, and his colleagues have discovered patients end up with damage to their small nerves and also diminished blood flow to certain areas of the brain.
He suspects that damage is due to changes in the immune system that were kicked off by the Lyme infection and remain after the bacteria have been obliterated. As for patients who experience improvement when treated with long courses of antibiotics, Novak believes this is because many antibiotics also have an anti-inflammatory effect.
So, while others look for ways to test for the presence or absence of the bacteria, Novaks strategy is to try to make patients feel better by treating their symptoms.
FOLLOW NBC HEALTH ON &
Also Check: Lyme Disease Head Pressure Treatment
Incidence Of Autoimmune Disease Development After Lyme Disease
Patients may develop new-onset systemic autoimmune joint diseasesincluding rheumatoid arthritis , psoriatic arthritis , or spondyloarthritis following Lyme infection, according to research published in Arthritis & Rheumatology.
Shelia L. Arvikar, MD, of the division of rheumatology, allergy, and immunology at the Center for Immunology and Inflammatory Diseases at Massachusetts General Hospital and Harvard Medical School, Boston, MA, and colleagues conducted a medical record review of all adult patients seen at a single specialty rheumatology clinic between 2003 and 2015. The researchers also analyzed records of patients enrolled in the Lyme arthritis cohort over a 2 year period for comparison.
Dr Arvikar and colleagues identified 30 patients who had developed new-onset systemic autoimmune joint disease a median of 4 months after Lyme disease 15 patients with RA, 13 with PsA, and 2 with peripheral SpA. Patients diagnosed with PsA or SpA were found to have had a past medical history significant for psoriasis, axial involvement, or enthesitis.
The number of patients that we have evaluated has steadily increased over the past 13 years, Dr Arvikar and colleagues wrote. Moreover, during the most recent 3-year period, the proportion of patients in whom we diagnosed a systemic autoimmune joint disease following Lyme infection increased even more.
How Is Lyme Disease Spread
Not all deer ticks are infected with the bacteria that cause Lyme disease. Ticks can become infected if they feed on animals such as mice and other mammals that are infected. The disease can be spread when an infected tick bites a person and stays attached for a period of time. In general, the tick must be attached for 36 to 48 hours or more. Lyme disease does not spread from one person to another. Transfer of the bacteria from an infected pregnant woman to her fetus is extremely rare.
You May Like: What Is Lyme Disease In Dogs
Lyme Disease And Rheumatoid Arthritis: Similarities Differences And Why A Misdiagnosis Can Be Deadly
Because its symptoms mimic those of so many other diseases both tick-borne and otherwise Lyme disease is often misdiagnosed. One of the most common Lyme disease misdiagnoses is Rheumatoid Arthritis , a chronic condition with less clear causes than Lyme disease.
Though there are many fundamental differences between these two conditions, its true that arthritic pain stemming from Lyme disease can often look like RA. In fact, Lyme was first discovered and documented in part because of a group of children presenting with arthritis symptoms in Lyme, Connecticut.
So, if youre experiencing joint pain, how can you tell the difference? If youve been bitten by a tick or think youre at risk for a tick-borne disease, its extremely important not to delay seeking medical attention or ignore any arthritic pain that might be associated with Lyme disease. Continue reading to better understand the differences and similarities between Lyme disease and arthritis.
Lyme Disease: Causes and Risk Factors
Lyme disease is a tick-borne infectious disease caused by the spiral-shaped bacteria Borrelia burgdorferi sensu lato. Though Lyme is treatable with antibiotics, it can worsen, change symptoms, spread to the neurological system, become a chronic condition, and even become life-threatening if not diagnosed and treated right away.
Common Symptoms of Lyme Disease
Early Lyme Disease Symptoms
- Bulls eye rash, or Erythema Migrans
Late Stage Lyme Disease Symptoms
- Facial drooping
Signs Of Arthritis After Lyme Disease
Joints are complex structures that connect bones to each other. These structures also make it possible to twist, bend and move your body. Arthritis happens when inflammation affects joint functioning.
The symptoms of arthritis after Lyme disease often come on suddenly and may include:
- Brief periods of joint pain, swelling and stiffness
- Pain that occurs in just one joint, typically a large one like your knee
- Difficulty performing once simple activities, like standing from a seated position or climbing stairs
- A popping sensation when you use the joint. Find out more about crepitus .
You May Like: How Long Does It Take To Get Lyme Disease
Lyme Disease: Why Does Joint Pain Persist
Researchers have found clues that might lead to a treatment for Lyme arthritis. The secret may lie in the walls of the bacterium that causes the condition.
Lyme disease occurs when a person becomes infected with a tick-borne bacterium called Borrelia burgdorferi.
Initial symptoms typically include general fatigue, fever, skin rashes, and headaches.
Although doctors can often treat Lyme disease with antibiotics, if they do not catch it early, the bacteria can cause long-term issues with the individuals joints.
In fact, following infection with B. burgdorferi, about 60% of people develop a condition called Lyme arthritis, the hallmarks of which are inflamed and painful joints.
Lyme arthritis can persist for months or even years in some cases.
Researchers are still unsure why joint symptoms can continue long after antibiotics have destroyed the bacteria.
30,000 cases of Lyme disease among the United States population.
However, the true number of cases is likely to be much higher. In fact, the CDC estimate that there might be up to 300,000 cases each year.
According to the CDC, reports of Lyme disease have tripled since the late 1990s, and overall, tick-borne diseases are becoming more prevalent. This increase is due, at least in part, to rising global temperatures.
Due to the steady growth in the number of cases, scientists are keen to uncover more effective ways of treating the long-term symptoms.
Read Also: Can Lyme Disease Cause Jaw Pain
Prevention Of Lyme Arthritis
Preventive measures to avoid or minimize tick bites are important and may include landscaping measures, removal of deer from specific areas, wearing appropriate clothing such as pants tucked into socks, and tick repellants. In areas where ticks are common, its important to check your child frequently and remove any ticks. Ticks may remain on your childs skin for hours before attaching themselves, so checking for ticks after coming inside may help remove them before they attach.
Read Also: What Are The Lasting Effects Of Lyme Disease
Lyme Disease: A Cause Of Fibromyalgia Chronic Fatigue And Arthritis
Lyme Disease: a cause of fibromyalgia, chronic fatigue and arthritisBy Nicola McFadzean, N.D.
Lyme disease was once thought of as an obscure disease that only affected people living in the northeast. Increasingly, however, Lyme disease is showing itself to be more prevalent than ever, and more widespread throughout the country, and indeed the world.
The number of Lyme disease cases is difficult to estimate because of both unreported and undiagnosed cases. The number of reported cases exceeds 20,000 per year, and climbing sharply, while the estimate of actual cases is approximately 100,000 per year.
The primary organism behind Lyme disease is a spirochete called Borrelia burgdorferi. A spirochete is a type of bacteria that is long, slender, and assumes a spiral shape. Tick bites are one of the more common routes of transmission however, more recent research has shown that mosquitoes can transmit the Borrelia spirochetes. Lyme frequently appears in multiple members of the family but can present differently. For example, a child has autism, while his mother has fibromyalgia. Both may test positive for Lyme disease.
Many individuals with chronic Lyme disease have other health issues that must be addressed alongside treating the spirochete itself. Among these issues are mold toxicity, parasite infections in the gut, heavy metal toxicity and hormone imbalance. Natural remedies can be used effectively to address the majority of those issues.
Submitted by:
When To Consider Testing For Lyme
You might be wondering if your joint pain could be related to Lyme disease, especially if youve had a blacklegged tick bite in the past.
The CDC estimates that a staggering 90% of cases of Lyme disease may go undiagnosed in the US each year. So while approximately 30,000 reported cases of Lyme reported annually, as noted, the actual number of cases may be closer to 300,000.
Lyme disease is often called the great imitator, because it mirrors many other diseases. These include, but are not limited to, osteoarthritis, rheumatoid arthritis, and multiple sclerosis. Unfortunately, unless you live in an area considered Lyme endemic, such as the northeastern United States, most conventional doctors may not think to test you for Lyme.
If your symptoms include waxing and waning flu-like symptoms, brain fog, fatigue, or joint pain, and if you think you may have had a tick bite in the past, consider asking your doctor for a test for Lyme disease. Remember that some people with Lyme experience have all of the above symptoms and more, while some experience just one. Also be aware that the ELISA test commonly given by conventional doctors is not always accurate, as it tests for antibodies that may or may not be present at the time of testing. My initial ELISA test came back negative it had been a year since my initial tick bite but my symptoms were in full force.
Arthritis.
Lucky for us, researchers may have just discovered a way
Also Check: The Side Effects Of Lyme Disease
Lyme Arthritis: A Small Piece Of The Larger Autoimmunity Puzzle
View IssueArth Rheum.Arth Rheum. Nature Rev Rheum.J Am Acad Orthop Surg.Curr Opin Rheumatol. J Clin Invest.Ann Intern Med. Disclosures: We were unable to process your request. Please try again later. If you continue to have this issue please contact .
Spotting and managing early Lyme disease can be easy: Just look for the bullseye. But when the rash goes away and the infection remains untreated for a prolonged period, Lyme arthritis can develop. That is when the real challenges begin.
To be fair, even Lyme arthritis can be easily recognizable, according to Robert Kalish, MD, rheumatologist and director of rheumatology education at Tufts Medical Center. Lyme arthritis is generally going to be a swollen knee in around 90% of patients, he told Healio Rheumatology.
Clinically, the knee or knees have a large effusion even after joint aspiration,Cassandra Calabrese, DO, of the department of rheumatologic and immunologic disease at the Cleveland Clinic, added.
Calabrese noted that the remainder of cases can manifest as persistent or intermittent pain and swelling in other larger joints, such as the shoulders, ankles or elbows. It can go on for years, generally being more persistent than intermittent, she said.
Beyond the Bullseye
Rheumatologists have played a pivotal role in the story of Lyme disease since it was first discovered by Steere in 1976, following an outbreak of juvenile arthritis or arthritis of unknown cause in Lyme, Connecticut.
Robert Kalish, MD,
Early Symptoms And Signs Of Lyme Disease
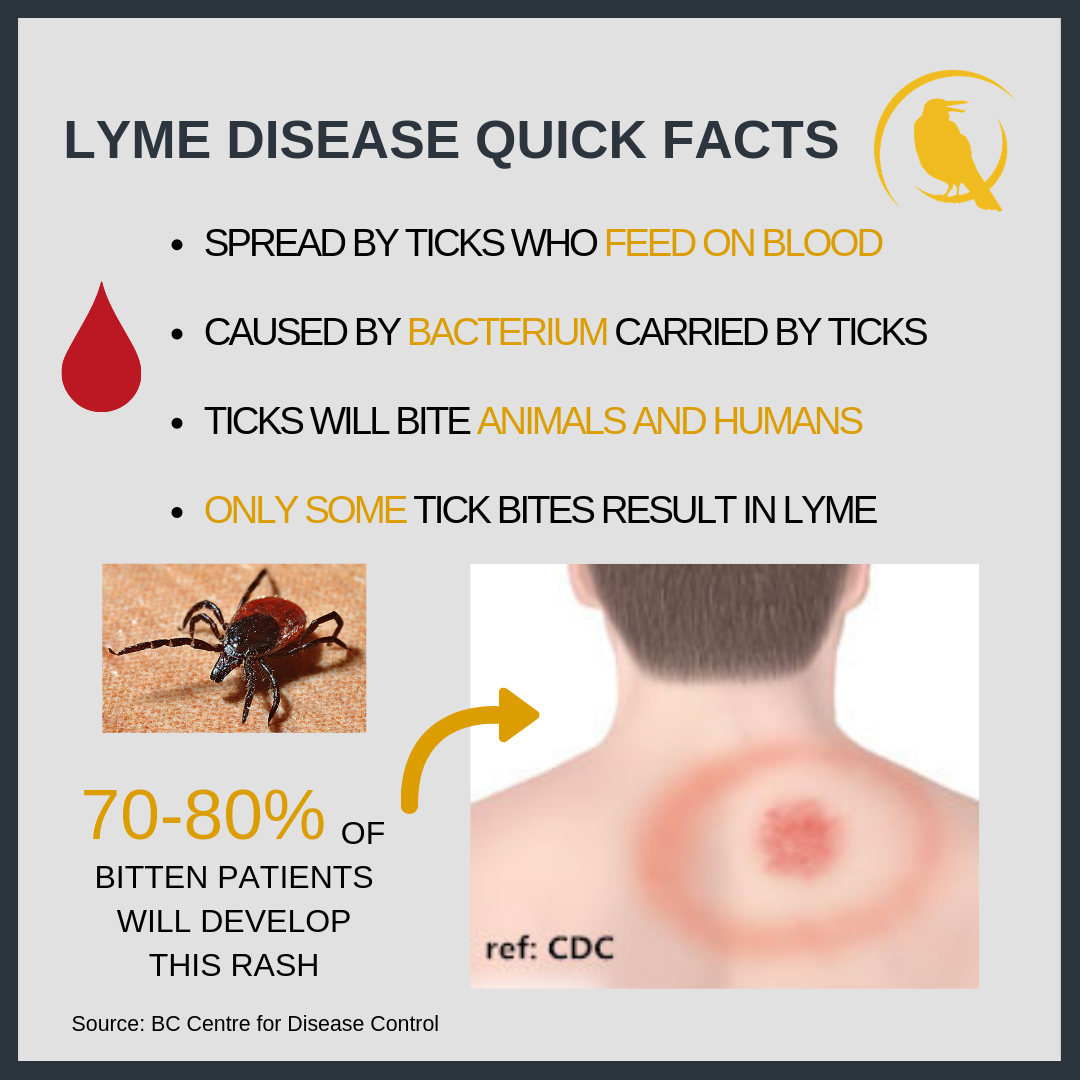
You can expect a small, red bump on the site of your bite, or where you removed the tick from, and this will resolve within a day or two. This is to be expected after being bitten by any insect, and it in itself is not an indicator that you have Lyme disease.
However, if you have been infected, you can expect the following within a month or so:
- Flu-like symptoms. Early-stage Lyme disease can present as chills, fever, fatigue body aches, stiff neck, headache and other flu-like symptoms.
- Rash development. Between three and 30 days after an infected tick bites you, you may see a rash that looks like a bulls eye. This will expand over days, and it can grow to as many as 11 to 12 inches across. It is usually not painful or itchy.
Don’t Miss: Deer Tick Lyme Disease Symptoms
Key Points For Healthcare Providers
What Can Be Done To Prevent Lyme Disease
The best prevention of Lyme disease is through awareness. Generally, ticks cannot jump or fly onto a person. They wait in vegetation and cling to animals and humans when they brush by. When in a potentially tick-infested habitat take special care to prevent tick bites, such as wearing light-colored clothing and tucking pants into socks and shirt into pants. Check after every 2 to 3 hours of outdoor activity for ticks on clothing or skin. Brush off any ticks on clothing or skin before skin attachment occurs. A thorough check of body surfaces for attached ticks should be done at the end of the day. If removal of attached ticks occurs within 36 hours, the risk of tick-borne infection is minimal. For proper tick removal, please watch the video at Tick removal. A vaccine for Lyme disease is not currently available.
Insect repellents can be effective at reducing bites from ticks that can spread disease. If you decide to use a repellent, use only what and how much you need for your situation. More information on repellents can be found at Environmental Protection Agency – insect-repellents.
In addition:
Domestic animals can carry ticks into areas where you live so it is important to check pets for ticks before they enter the home.
Read Also: Blood Test For Lyme Disease In Humans
Who Gets Lyme Disease
Lyme disease can affect people of any age. People who spend time outdoors in activities such as camping, hiking, golfing, or working or playing in grassy and wooded environments are at increased risk of exposure. The chances of being bitten by a deer tick are greater during times of the year when ticks are most active. Ticks can be active any time the temperature is above 45° F. Young deer ticks, called nymphs, are active from mid-May to mid-August and are about the size of poppy seeds. Adult ticks are most active from March to mid-May and from mid-August to November and are about the size of sesame seeds. Both nymphs and adults can spread Lyme disease. Infected deer ticks can be found throughout New York State.
Synovial Fluid Analysis Imaging And Other Tests
On presentation, joint aspiration is usually done for diagnostic purposes to rule out the presence of other arthritides such as crystalline arthropathy or staphylococcal septic arthritis. Joint fluid white cell counts are usually inflammatory in the range , but cell counts as low as 500 or as high as 100,000 cells/mm3 have been reported.3 Although tests for rheumatoid factor or antinuclear antibodies typically yield negative results, antinuclear antibodies in low titer may be detected. Peripheral white blood cell counts are usually within the normal range, but inflammatory markers, such as ESR and CRP, may be elevated. Imaging studies are not required for diagnosis or are not typically performed. The major reason for imaging studies in Lyme arthritis is when there are concerns for alternative diagnoses.
In patients with Lyme arthritis, plain films, MRI scanning or ultrasound typically show non-specific joint effusions, while MRI studies utilizing contrast dye, may display synovial thickening or enhancement. In adult patients, imaging studies may show co-incidental degenerative changes or chronic mechanical injuries, but these abnormalities would not be expected to cause significant synovitis or inflammation. Lyme arthritis is not rapidly erosive, but with longer arthritis durations, joint damage can be seen on radiographic studies.32 Finally, MRI scanning may be useful in the planning of synovectomies by determining the extent of synovitis within the joint.
Also Check: What Is It Like To Have Lyme Disease