Late Stage Lyme Disease: Symptoms And Treatment
by Lyme Mexico | Mar 17, 2021 | News |
There are three stages of Lyme disease. If you are experiencing the symptoms in the late stage, that means you have already passed through the first two stages of early localized and early disseminated Lyme disease.
During the early localized phase, you may have had a rash associated with the bite given by the infected tick. Symptoms following the bite may have included chills, fever, headaches, fatigue, stiff neck, muscle soreness, and possibly swollen lymph nodes.
If you did not receive the right treatment at the onset, you quickly moved into the next stage. During the early disseminated phase, the Lyme infection started spreading through your body.
Symptoms in the second stage include all of the signs from the early localized stage, only worse. You may also experience vision problems, pain or weakness in your limbs, heart palpitations, and facial paralysis such as bells palsy.
If left untreated, stage two will turn into late stage Lyme disease.
If you are in stage three, or the late disseminated stage, you have been struggling with symptoms for a long while and without treatment specific to Lyme disease.
The symptoms of late stage Lyme disease are genuine and can interfere with daily functioning.
Where Am I At Now In The Process
Im still struggling, but mostly physically, which I prefer over the mental issues I used to deal with. Fortunately, I no longer experience brain fog or seizures, but constantly deal with migrating pain. I go through weeks at a time feeling great and then weeks of a flare up where no medicine seems to help. I jump around trying to figure out the best treatment for this disease. Ive been through everything from antibiotics, stem cells and homeopathic treatments.
We are at the point where my husband can work from home and stay with me during my flare ups. Five years in and were learning to not panic when Im stuck in a wheelchair. I spend Sunday mornings loading up my pill case, which is now down to one instead of two!
This is not the life I had planned, but its what Ive been dealt. In the past two years, Ive been determined to make the best of it.
False Negatives And Positives
Since early treatment is crucial to prevent complications, accurate diagnosis is essential. Those who have a history of tick bites and a bullseye rash do not need to be tested and should be treated as if they have Lyme disease. However, when the picture is less clear but Lyme disease is suspected, laboratory testing is recommended. False negative results are common in early Lyme disease because the standard test detects antibodies to the Borrelia bacteria and these take several weeks to develop. In addition, some people who receive antibiotics within the first few weeks of a tick bite may not develop antibodies or may only develop them at levels too low to be detected by the test.
In line with this, the NHS Highland National Lyme Borreliosis Testing Laboratory advises that patients with a clinical history consistent with early Lyme disease who have a negative test should be retested six to eight weeks after symptom onset. It is also possible for the antibody test to give a false positive result, so positive tests are confirmed using a second test, called a Western Blot.
Don’t Miss: When Do Symptoms Of Lyme Disease Start
Lyme Disease And The Cdc
In order for the Centers for Disease Control to recognize a Lyme case for surveillance purposes, there must be objective findings, such as positive blood tests, Bells palsy or joint swelling . The chart below reflects the CDC-reviewed surveillance case manifestations from 2001 to 2010.
This situation contributes to what many experts view as severe undercounting of Lyme disease by the CDC.
Where Is Lyme Disease Prevalent
LD is spreading slowly along and inland from the upper east coast, as well as in the upper midwest. The mode of spread is not entirely clear and is probably due to a number of factors such as bird migration, mobility of deer and other large mammals, and infected ticks dropping off of pets as people travel around the country. It is also prevalent in northern California and Oregon coast, but there is little evidence of spread.
In order to assess LD risk you should know whether infected deer ticks are active in your area or in places you may visit. The population density and percentage of infected ticks that may transmit LD vary markedly from one region of the country to another. There is even great variation from county to county within a state and from area to area within a county. For example, less than 5% of adult ticks south of Maryland are infected with B. burgdorferi, while up to 50% are infected in hyperendemic areas of the northeast. The tick infection rate in Pacific coastal states is between 2% and 4%.
You May Like: Town Of East Lyme Jobs
Early Detection Is Key
Lyme disease is easiest to treat at the early or acute stage, within the first 30 days of exposure. This is why its so important to take precautions to prevent tick bites, both during and outside of tick season. Protect yourself when near potential tick habitats, always perform tick checks after outdoor activity , and dont delay seeking medical attention if you notice any symptoms that might be related to tick-borne illness. Its important to get tested as soon as possible for the best chances of recovery.
Learn The Stages Of Lyme Disease
Lyme disease occurs in three stages: early localized, early disseminated and late disseminated. However the stages can overlap and not all patients go through all three. A bulls-eye rash is usually considered one of the first signs of infection, but many people develop a different kind of rash or none at all. In most cases, Lyme symptoms can start with a flu-like illness. If untreated, the symptoms can continue to worsen and turn into a long-lived debilitating illness.
Stage 1: Early Localized Disease
Symptoms with early localized Lyme disease may begin hours, a few days or even weeks after a tick bite. At this point, the
infection has not yet spread throughout the body. Lyme is the easiest to cure at this stage.
Symptoms may include:
- skin rash, which may or may not look like a bulls eye
- flu-like illness, including chills and fever
- fatigue
- muscle soreness and joint pain
- swollen lymph nodes
- sore throat
Stage 2: Early Disseminated Lyme
Early disseminated Lyme may occur several weeks or months after the tick bite. Bacteria are beginning to spread throughout the body. In addition to flu-like symptoms, this stage is often characterized by increase in symptoms such as:
- chills
- pain, weakness or numbness in the arms, legs
- vision changes
- heart problems, such as palpitations, chest pain
- rash may appear on body
- facial paralysis
Stage 3: Late Disseminated Lyme Disease
Related Content
Find a LLMD
Lyme Symptom Tracker App
Get started with your diary
Don’t Miss: What To Do If You Have Lyme Disease
When To See A Doctor
A person should see a doctor if they have recently received a tick bite. It is not possible to know whether a tick is carrying Lyme disease, and the symptoms may take weeks to appear.
The earlier a person receives a diagnosis and treatment, the higher the likelihood of a quick and complete recovery.
It is not always possible for a person to tell if a tick has bitten them. As such, people should also see a doctor if they experience any Lyme disease symptoms. A doctor will ask about the persons symptoms and duration and whether the person has spent time in tick-infested areas.
Treatment For Chronic Lyme Disease
Sometimes, people go through treatment for Lyme disease but their symptoms donât go away. If this lasts over 6 months, itâs known as chronic Lyme disease or âpost-treatment Lyme disease syndromeâ .
Doctors still arenât sure why some people get PTLDS. Some believe that getting Lyme disease may cause damage to your tissues or immune system. Others believe itâs because the bacteria that causes Lyme hasnât completely gone away.
There is little evidence that taking more antibiotics at this stage will help. They may actually be harmful. Instead, your doctor will focus on treating the symptoms youâre still having. This will be different for everyone. Some people could benefit from a medicine that relieves fatigue, while others may need a drug that can help with headaches or very sensitive skin.
Your doctor could also have you try a treatment that helps people with chronic fatigue syndrome or fibromyalgia.
More research is needed to figure out how best to treat PTLDS. Itâs something that can be frustrating. Just remember: Many people who have this condition do start feeling like their old selves after a few months.
Recommended Reading: What Is Lyme Disease And What Are The Symptoms
May Is Lyme Awareness Month
May is Lyme Awareness Month and honestly, Id rather skip this entire part of my story. However, Ive been reminded that once upon a time, I told myself that when I got better, I would do what I could to help others in my situation.
Lyme is a tricky thing. Most people know what Lyme Disease is: you get a tick bite, theres a bulls-eye rash, you take antibiotics, and youre better. Thats acute Lyme.
Then theres something much more complicated, scary and controversial called Chronic Lyme . Most doctors dont believe there is such a thing. Late Stage Lyme occurs when youve been bitten and either the disease lies dormant and presents itself later after a big event or you never fully recover from your initial treatment from acute Lyme. Many doctors say that Chronic Lyme is not really Lyme. They claim its some other disease you havent figured out yet, like MS, Lupus, Rheumatoid Arthritis, etc.
So when I was diagnosed, not only did I have to figure out this complicated disease , I had to fight for my right to even treat it. The Chronic Lyme world is often secretive and hidden, uncovered by insurance, and doctors are continually losing their licenses over prescribing unnecessary treatments such as long term antibiotics.
Assessment Total Clinical Assessment Or Laboratory Assessment
A tradition in mainstream medicine is to first perform a thorough clinical exam, to then consider lab tests when they might help with the diagnosis, and to use clinical judgment to develop an individualized diagnosis and treatment plan. We treat patients, not diseases . An individualized approach is particularly significant when dealing with complex and poorly understood multisystem diseases. In opposition to this conservative and traditional approach, some have attempted to oversimplify the diagnosis of Lyme disease by reducing the diagnosis to reliance upon the United States Centers for Disease Control and Prevention surveillance definition . However, the surveillance definition has never been intended to be a sole diagnostic criterion, particularly in late-stage disease. Although meeting the surveillance definition for Lyme disease may confirm the diagnosis, not meeting the surveillance definition does not rule out the diagnosis of the disease. This has been emphasized by the Centers for Disease Control and Prevention and has been supported by studies performed by them . In spite of this warning, many physicians fail to perform adequate clinical examinations when suspecting Lyme disease, and by default place excessive reliance upon laboratory testing that can be highly flawed .
Don’t Miss: Lyme Disease Symptoms And Treatment In Humans
Late Stage Lyme Disease Treatment
May present with various neurological or musculoskeletal symptoms, and lacks truly pathogenic features. Late in the infection, significant levels of IgG specific antibodies are easily detectable by both antibody capture EIA and immunoblotting . IgM and IgA are variably present in late untreated patients. The serologic characteristics are usually different for most patients with late stage infection. In addition to serologic testing, bacterial DNA may be detected, especially in the bodily fluids of patients with Lyme, and rarely if ever in whole blood late in the infection.
Heart Failure
Probable Late Lyme Disease

Table presents demographic and clinical characteristics of the 13 patients with probable late Lyme disease in comparison to patients with other Lyme disease and non-Lyme disease related diagnoses. The median age at illness onset was 61 in patients with probable late Lyme disease. The majority of the patients in the overall sample, with exception of those with confirmed late Lyme arthritis, presented with some combination of fatigue, generalized musculoskeletal pain, and cognitive complaints. By definition, patients with probable late Lyme disease had no history of physician documented or treated EM rash and no objective clinical signs associated with late Lyme disease. However, 38% recalled a rash consistent with EM at illness onset not documented or diagnosed by a physician. In some cases the rash was felt by the patient or physician to be atypical for Lyme disease because of the lack of the classic bulls eye appearance or because the rash did not meet the minimum 5cm size in the CDC surveillance criteria . This proportion of prior patient-documented rash in the absence of physician diagnosed erythema migrans was higher in the probable late Lyme disease group when compared to the other four disease groups .
Read Also: Lyme Disease And Red Meat
Stage : Early Disseminated Lyme Disease
If stage 1 Lyme disease remains undiagnosed and untreated, it can progress to stage 2, or early disseminated, Lyme disease. This stage occurs 312 weeks after the initial tick bite.
The term disseminated indicates that the bacteria have spread throughout the body. At this stage, the infection may affect the following tissues:
- the skin
- nervous system
- heart
A person who has progressed to stage 2 Lyme disease may develop new symptoms alongside those from stage 1. These new symptoms may include:
- new rashes across the body
- conjunctivitis or vision problems
- poor memory and concentration
Complementary And Alternative Therapies
You should never treat Lyme disease with complementary therapies alone. Only proper antibiotic treatment can cure the disease and avoid complications.
Newsletters and Internet sites have cropped up in recent years advertising untested treatments to people with symptoms of post-Lyme disease syndrome or so-called “chronic Lyme disease” who are frustrated with standard medical treatment. Some remedies may be dangerous and ineffective. Always tell all of your doctors about the herbs and supplements you are using or considering using.
Don’t Miss: Lyme Literate Doctors In Nh
Chronic Lyme Disease Patients Profoundly Debilitated
Many patients with chronic Lyme disease are profoundly debilitated. Investigators of the four NIH-sponsored retreatment trials documented that the patients quality of life was consistently worse than that of control populations and equivalent to that of patients with congestive heart failure. Pain levels were similar to those of post-surgical patients, and fatigue was on par with that seen in multiple sclerosis.
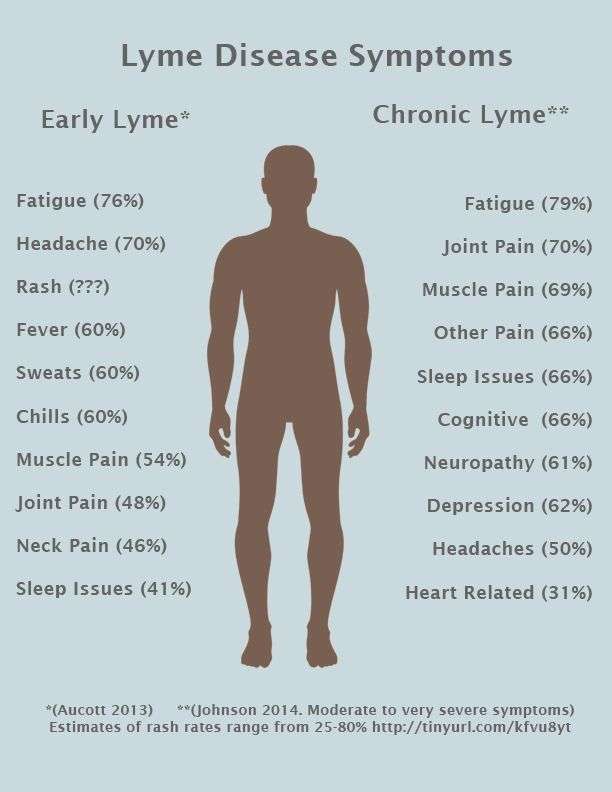
An LDo published survey of over 3,000 patients with chronic Lyme disease found that patients suffer a worse quality of life than most other chronic illnesses, including congestive heart failure, diabetes, multiple sclerosis and arthritis. Over 70% of patients with chronic Lyme disease reported fair or poor health. Similar results have been found in other studies. Many of the symptoms associated with Lyme disease are common in other diseases. The CDC surveillance criteria for confirmed cases specifically exclude most of the symptoms that patients report, including fatigue, sleep impairment, joint pain, muscle aches, other pain, depression, cognitive impairment, neuropathy, and headaches. However, these common symptoms can be severe and may seriously affect quality of life.
Stage : Early Localized Lyme
In this stage of infection, patients might notice a Lyme rash, often in the shape of a very defined bulls eye. This stage occurs within 30 days after a bite from an infected black-legged tick. Other symptoms in this stage might be fever, chills, fatigue, headache, joint pain, and sore throat. Early localized Lyme is treated with a round of strong antibiotics. Most often, early localized Lyme disease can be cured with doxycycline.
You May Like: Dr Frank Noonan Lyme Disease
Early Stages Of Lyme Disease
If presenting with classic features in an endemic area, is diagnosed straightforwardly. Diagnosis is more challenging however if symptoms are not typical, and laboratory testing is indicated. Most patients symptomatic with B. burgdorferi infection are sero-positive , demonstrating an initial IgM response best shown by antibody capture EIA. If a patient is suspected of having early Lyme disease is initially sero-negative, repeat follow-up testing is very useful. The evolution of the host immune response to B. burgdorferi infection is typically very quick. In as short a time as a week or two, an initially seronegative patient can develop robust seropositivity. The IgA response on antibody capture EIA is noted in early infection as well. Unlike the IgM and IgG response , IgA levels usually fall rapidly with effective treatment and infection resolution, often becoming undetectable within the first few months. In that early window of an infection, when a patient is sometimes acutely symptomatic but prior to developing a detectable serologic response, it is possible with PCR technology to detect the DNA of B. burgdorferi in a whole blood specimen. It has been our observation that this window of B. burgdorferi bacteremia is brief, and by the time the patient has developed the characteristic serologic response, whole blood PCR testing for Lyme will have become negative.
When Did This Start
After the birth of my daughter in 2014, I began having back and chest pains so intense that I was unable to continue breastfeeding. My right arm was constantly tingling and throbbing. At times I felt like I was holding a vibrating cellphone when I wasnt. Pain around my collarbone was so excruciating that I had trouble breathing. I got checked out by a hospital, several neurologists and a rheumatologist. I endured endless blood work, medication changes, CT scans, MRIs, EEGs, EMGs, and EKGs. No one had any answers for me. I was diagnosed with fibromyalgia . However, I always had lots of inflammation, which they admitted didnt fit the diagnosis.
Over time, the disease progressed and most of my medications exacerbated my symptoms. I was left bedridden, unable to care for myself or my family. I started experiencing all sorts of neuropathy pain like twitching, tremors, numbness, tingling, migrating pain, and crawling skin. In addition, I had hair loss, rashes, panic attacks, blurred vision, paranoia, nausea, vomiting, fainting, air hunger, seizures and brain fog.
You May Like: What Is The Test For Lyme Disease Called