Lyme Disease Frequently Asked Questions
If you have not done so already, remove the tick with fine-tipped tweezers.
The chances that you might get Lyme disease from a single tick bite depend on the type of tick, where you acquired it, and how long it was attached to you. Many types of ticks bite people in the U.S., but only blacklegged ticks transmit the bacteria that cause Lyme disease. Furthermore, only blacklegged ticks in the highly endemic areas of the northeastern and north central U.S. are commonly infected. Finally, blacklegged ticks need to be attached for at least 24 hours before they can transmit Lyme disease. This is why its so important to remove them promptly and to check your body daily for ticks if you live in an endemic area.
If you develop illness within a few weeks of a tick bite, see your health care provider right away. Common symptoms of Lyme disease include a rash, fever, body aches, facial paralysis, and arthritis. Ticks can also transmit other diseases, so its important to be alert for any illness that follows a tick bite.
References:
Moody KD, Barthold SW, 1991. Relative infectivity of Borrelia burgdorferi in Lewis rats by various routes of inoculation.external iconAm J Trop Med Hyg 44: 135-9.
There are no reports of Lyme disease being spread to infants through breast milk. If you are diagnosed with Lyme disease and are also breastfeeding, make sure that your doctor knows this so that he or she can prescribe an antibiotic thats safe for use when breastfeeding.
The Swiss Agent: Long
Lyme disease is a serious problem here in the United States and we really need to find solutions to some of the limitations that we have, particularly in diagnosing this infection, said Claudia Molins, a microbiologist at the CDC. We want a test that can be used within the first two weeks of infection and that does not rely on antibody production.
So Molins and her colleagues are focusing on metabolomics an approach that, rather than testing directly for the immune response to the infection, instead looks for a wide spectrum of collateral damage.
Specifically theyre looking for so-called metabolite biosignatures: the litany of sugars, peptides, lipids, amino acids, fatty acids, and nucleotides normally present in the blood.
Infections like Lyme, the thinking goes, change the levels of these things and they do so in a predictable, measurable way.
Molins and her team tested that hypothesis by tapping a unique CDC resource freezers filled with well-characterized blood serum samples. They used serum from 89 early Lyme patients, within the first month of infection, and 50 healthy controls to develop an algorithm to detect Lyme blood signatures.
The researchers then tested that algorithm on a larger sample of serums and found that they could diagnose 88 percent of early Lyme cases, and could differentiate Lyme from other diseases 93 percent of the time. The results were published in a 2015 study in Clinical Infectious Diseases.
Lyme Disease Is Remarkably Difficult To Diagnose
The problem with Lyme disease is that the bacteria can create a hard shell around themselves when inactive so that the blood tests are unable to detect them. This is especially true when the disease has reached the chronic stage. The timing of the symptoms is often used by a medical provider to establish a time line to a tick bite or exposure to a high-risk region where the disease is commonly transmitted.
Because the ticks that can spread Lyme disease are often the size of a pinhead, the ticks might not even be notice. A bulls-eye rash at the bite location is a trademark symptom of Lyme disease, but only about half of the people who are infected with the bacteria develop the rash. Once the disease reaches the chronic stage, chronic arthritis, joint pain, and neurological symptoms begin to appear, sometimes several months after the infection.
You May Like: What Are The Symptoms Of Lyme Disease In A Person
Lyme Disease Antibody Test Procedure
The Lyme disease antibody test requires no advance preparation. A lab technician will swab the inside of your elbow with an antiseptic before drawing your blood. Your blood will be drawn from a vein in your arm using a small needle.
The blood draw should not be painful, though you might feel a slight prick when the needle is inserted into your vein.
The blood sample will be collected in a vial. The puncture site will be bandaged, if needed, after the needle is removed. After the blood draw, you are free to go home.
There are very few risks associated with the Lyme disease antibody test. Excessive bleeding is possible, but there may be an increased risk if you take blood thinning medications or certain anti-inflammatory drugs like:
- heparin
The Elisa And Western Blot Are Not Sensitive Enough
Another major limiting factor of the traditional ELISA and Western blot is the quality. These tests tend to use lysed BB cultures, and therefore, depending on the culture conditions, some antigens are over-expressed, and some are under-expressed. This, in turn, can affect the ability to detect antibodies from patients blood.
Whats more, if a patient tests too early after a tick bite, his or her body may not have produced enough antibodies to show up on a test with suboptimal sensitivity.
Read Also: Lyme Disease Diagnosis And Treatment
How To Avoid Tick Bites
To reduce the chance of being bitten:
- cover your skin while walking outdoors and tuck your trousers into your socks
- use insect repellent on your clothes and skin products containing DEET are best
- stay on clear paths whenever possible
- wear light-coloured clothing so ticks are easier to see and brush off
What Is Lyme Disease How Does My Dog Get Infected
Lyme disease is an infectious disease caused by bacteria called Borrelia. The bacteria are most commonly carried by the deer tick . Infection occurs when a dog is bitten by an infected tick. It appears that the disease is not transmitted until the tick has fed for approximately 12 hours. The tick itself becomes infected by feeding on infected mice, birds, deer, and other animals.
You May Like: Dr Horowitz Lyme Disease Treatment Protocol
Positive Elisa On Serum
RIPL will automatically proceed to do IgM and IgG immunoblot tests after a positive or indeterminate ELISA test and will provide an overall interpretation of the ELISA and immunoblot in the light of the clinical details provided on the request form.
Please provide clinical details to allow the interpretation of serological results. These are needed for interpretation because borrelia-specific antibodies may persist for several years in patients who have had Lyme disease in the past, long after the bacteria have been cleared from the body. Therefore, detection of borrelia specific antibodies in someone with no evidence of current clinical symptoms or recent tick exposure argues against active Lyme disease infection. After successful treatment of Lyme disease antibody concentrations may slowly fall over time.
Borrelia species are notifiable organisms. The numbers of positive results from laboratory confirmed cases in RIPL are reported to UKHSA and analysed for inclusion in UKHSA Health Protection Reports as part of Lyme disease epidemiology and surveillance.
What Are The Symptoms Of Lyme Disease
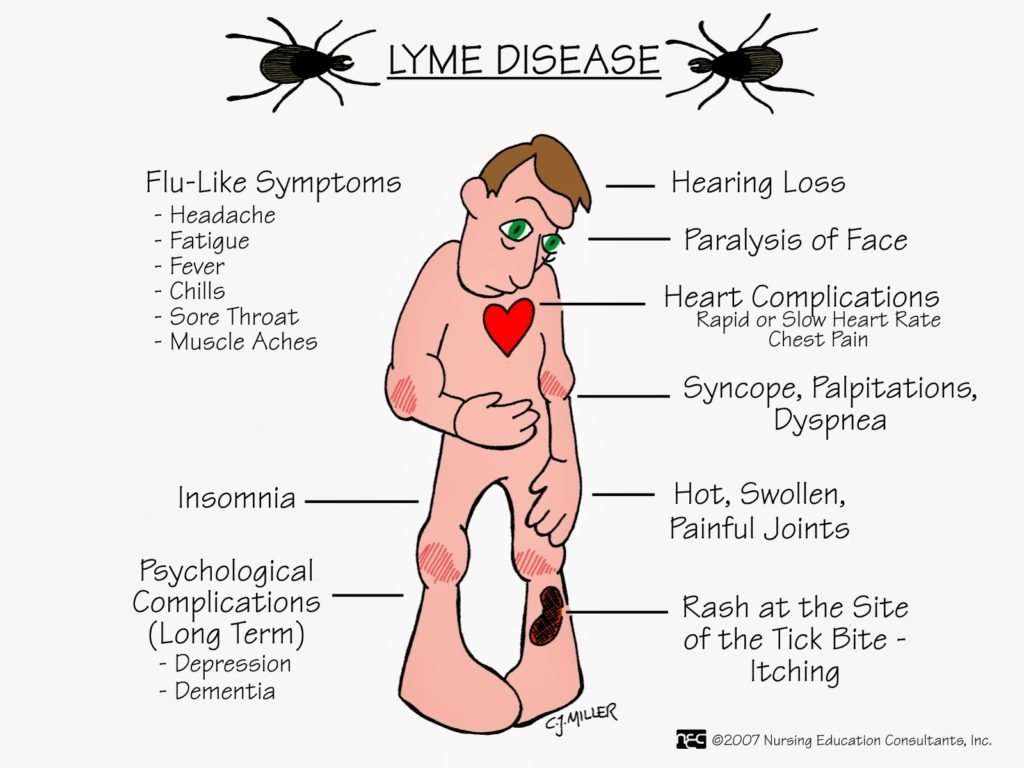
Lyme Disease is a bacterial infection that results from a tick bite. The symptoms vary, and you can feel sick for months because of it. Some of the most common symptoms of Lyme disease are flu-like symptoms such as fever, chills, and headache. A rash can also occur in 70 to 80 percent of infections. If left untreated, the symptoms can worsen into facial palsy, dizziness, heart palpitations, and more.
Recommended Reading: Lyme Disease Symptoms Without Rash
Are There Any Diseases That Can Be Misdiagnosed As Lyme Disease
Lots of diseases could be misdiagnosed as Lyme disease. This of course makes sense when you know that Lyme disease itself may manifest as a multisystemic disorder that can mimic other diseases. This means that just as the Lyme disease might be missed in some cases, some individuals may be misdiagnosed as having Lyme disease when in fact they have another disease. Erring on either side of this diagnostic divide can be dangerous. Given that the main symptoms that afflict patients with Lyme disease are fatigue and pain and given that these are non-specific symptoms seen in a wide ranges of diseases, including cancer, hematologic, and endocrine disorders, one has to make sure to rule out other reasonable causes of fatigue and pain before making the diagnosis of Lyme disease. It is also important to realize that a patient can have two independent diseases Lyme disease and another emergent condition. For example, concurrent depression,sleep apnea or hypothyroidism may exacerbate fatigue in a patient with actual Lyme disease.
Is Lyme Disease Curable
While there is no vaccine to prevent us from getting Lyme disease, it can be treated with antibiotics, and most people recover within a few weeks. However, some people can get what is known as Post-Treatment Lyme Disease Syndrome, in which symptoms such as pain, fatigue, or difficulty thinking can last for months.
You May Like: Dr Nader Soliman Lyme Disease
Experts Agree Around The World
A strong scientific consensus is evident about Lyme disease diagnosis and testing.
A 2018 French review of 16 Lyme diagnostic guidelines from 7 countries revealed a global consensus regarding diagnosis at each stage of the infection. The only outlier was the pseudoscience group German Borreliosis Society , a German counterpart to the pseudoscience group ILADS.
Future Possibilities For Diagnostic Tools

NIAID-supported scientists have identified genome sequences for multiple strains of B. burgdorferi. Greater advances in diagnostics are anticipated as genetic information is combined with advances in microarray technology, imaging, and proteomics. These growing fields of science are expected to lead to improved diagnostic tools as well as provide new insights on the pathogenesis of Lyme disease. Examples of tools being developed with NIAID support include use of metabolomics to characterize new biomarkers of infection, next generation T-cell based measurements, and novel antigens for improved measurement of effective treatment.
Read Also: How To Avoid Lyme Disease
What Is An At
An at-home Lyme disease test will typically be a blood finger prick test.
If you have been exposed to the bacteria Borrelia that leads to the infection of Lyme disease, your body will have created two antibodies to fight it off. The test will look for the presence of both types of antibodies, known as immunoglobulin M and immunoglobulin G .
You will receive your test kit along with account information so that you can get your test results as soon as theyre ready. Follow the manufacturers instructions exactly as they are described.
Each test has different instructions, so its very important to read the kits detailed information before getting started.
Interpretation Of Lyme Multiplex Results1213
The Lyme Multiplex Assay is a fully quantitative test. It results in a numeric antibody value for each of the three B. burgdorferi antigens tested. A brief interpretation on each value is submitted with the test report. In addition, the antibody profile gives an advanced interpretation on the infection and vaccination status of the horse. Antibodies to OspA serve as markers for vaccination and those to OspC and OspF as markers for infection . In treated horses, quantitative antibody values are valuable indicators to follow-up on treatment success.
Figure 3:B. burgdorferi
You May Like: How To Prevent Lyme Disease
Are There Any Risks To Lyme Disease Tests
There is very little risk to having a blood test or a lumbar puncture. If you had a blood test, you may have slight pain or bruising at the spot where the needle was put in, but most symptoms go away quickly. If you had a lumbar puncture, you may have pain or tenderness in your back where the needle was inserted. You may also get a headache after the procedure.
How Stephanie Got Answers
About four years ago, Tait started to suspect she had Lyme disease. A family friend had Lyme, and Tait recognized some of her own symptoms appearing in her friend. She asked her doctor for an ELISA, an enzyme-linked immunosorbent assay, or a blood test thats typically the first way doctors test patients who may have Lyme disease. When she learned her insurance wouldnt cover the cost, she paid for the test out of pocket. It came back negative.
Tait, however, wasnt convinced. She asked for another test, but she said the doctor refused. So she turned to a private lab for a second test, this one a Western Blot, which doctors typically turn to next, to verify a positive ELISA result. That test was positive for the Lyme antibodies.
I sobbed, because there it was in my hands that I wasnt just jumping to conclusions, Tait said. I walked back into my doctors office and said, Here it is. They said, Well, we didnt do this test, so how do we know? I said, Youve got to be kidding me. I have a lab test!
Tait started getting treatment at a private clinic in Idaho that specializes in treating Lyme disease, about a six-hour drive from where she lives.
Lyme disease is typically treated with antibiotics, and when treated early, people with Lyme usually recover completely. Taits treatment plan included antibiotics, immunotherapy, various supplements as well as dietary changes. But because she had been sick for so long, some of her health problems were irreversible.
You May Like: Best Lyme Treatment In The World
More About Western Blot Testing In North America
The IgG Western Blot test is designed to detect antibodies specific to Borrelia burgdorferi, the bacteria that cause Lyme disease. For Lyme disease in North America, a positive IgG Western Blot test requires at least 5 of 10 measured bands to be positive .
The scored IgG bands are 18 kDa, 24 kDa , 28 kDa, 30 kDa, 39 kDa , 41 kDa flagellin , 45 kDa, 58 kDa , 66 kDa, and 93 kDa.
The Lyme IgM Western Blot test measures 3 different types of antibodies. The North American IgM Western Blot is considered positive only if 2 of 3 IgM bands are positive .
The scored IgM bands are 24 kDa , 39 kDa , and 41 kDa .
As discussed above, the IgM Western Blot should only be used in the first 30 days of illness.
According to CDC, Depending upon the assay, OspC could be indicated by a band of 21, 22, 23, 24 or 25 kDA.
Most Accurate: Dna Connexions
-
Test looks for Borrelia burgdorferi, in addition to 10 other common vector-borne pathogens
-
Urine Sample
-
Does not accept insurance
-
No assistance after testing results are received
DNA ConneXions is a company known in the scientific community for its detailed analysis of lab results. This at-home Lyme disease test, for example, is superior to the others because it tests for all 10 vector-borne pathogens, while others only test the most common two or three.
DNA ConneXions earned our most accurate distinction because of its detailed Lyme disease test, as well as its impressive laboratory with a biosafety level 2 lab with a CLIA license. This means the company knows its stuff and is able to help people with accurate testing.
After DNA ConneXions receives your urine sample, it will review your sample, and email you your results within two to three weeks. It is unclear how much support the company offers after you receive your results, so it would be wise to schedule an appointment with your primary care doctor. This is to ensure that your body heals entirely if your Lyme disease test is positive.
This is the most expensive kit on this list, costing about $650 for the full Lyme panel. As of now, it will not work with insurance companies or accept HSA. The DNA ConneXions lab, however, is one of the most trusted laboratories worldwide.
Recommended Reading: How To Treat Lyme Disease In Child
Testing For Lyme Disease In Dogs
Lyme disease spread by ticks can be diagnosed with a simple blood tests in your veterinarians clinic. The C6 test is very sensitive and specific at diagnosing cases of Lyme disease and depending on clinical signs and concurrent results, treatment may be started immediately. If treatment has been successful, reductions in the QC6 at six months should be lower than the starting point.
Dont Miss: Beach Houses For Sale In Old Lyme Ct
How Much Do At

Generally, at-home Lyme disease tests cost around $100, while others may cost closer to $500. The difference comes down to how many pathogens you are hoping to test for. On average, the test will look for two or three, but more expensive tests may screen for 10 to 15.
Depending on your insurance and which test you select, it may be covered. Another option is to pay for the Lyme disease test with your HSA/FSA, since some companies will accept that as a payment form.
Don’t Miss: Lyme Disease Blood Test Cost
How Can I Tell If Treatment Is Working
If joint lameness is the presenting sign, improvement may be noted after 3-5 days starting antibiotics. A dog’s response to therapy can be assessed by repeating the QC6 test six months after treatment is complete. Dogs that start with a moderate to high QC6 value typically show a 50% reduction or more in the QC6 at six months, indicating that treatment has been successful. Dogs that have a lower initial QC6 value may not show such dramatic reductions in the QC6 at six months, although the value should still be lower than the starting point if treatment has been successful.
A persistently high QC6 suggests treatment may not have been complete or that the dog became reinfected after treatment was stopped.