British Columbia Specific Information
Ticks are tiny bugs which feed on blood. For information on ticks, removing ticks, and how to avoid being bitten, see HealthLinkBC File #01 Tick Bites and Disease. You may also be interested in the HealthLinkBC File #96 Insect Repellent and DEET.
While most tick bites do not result in diseases, some can. Some of the diseases passed on by ticks include relapsing fever, tularemia, Rocky Mountain Spotted Fever , Q Fever and anaplasmosis. The most well-known is Lyme disease. For more information on Lyme Disease, visit BC Centre for Disease Control – Lyme Disease .
The Best Test For Lyme Disease
Lyme disease is a tick-borne illness spread by Lyme borreliaebacteria which includes, but is not limited to, Borrelia burgdorferi sensu stricto. The Centers for Disease Control and Prevention estimate that there are 400,000 cases of Lyme disease annually, making Lyme a serious public health concern that only stands to grow as the spread of ticks affects disease endemicity and seasonality.
One of the biggest challenges of fighting Lyme disease is providing patients with accurate diagnostic tests. Without access to the best tests for Lyme disease, its impossible to diagnose this treatable disease in a timely manner. When the disease isnt caught in time, it can spread throughout the body and cause chronic health problems that could otherwise be avoided with earlier detection and treatment.
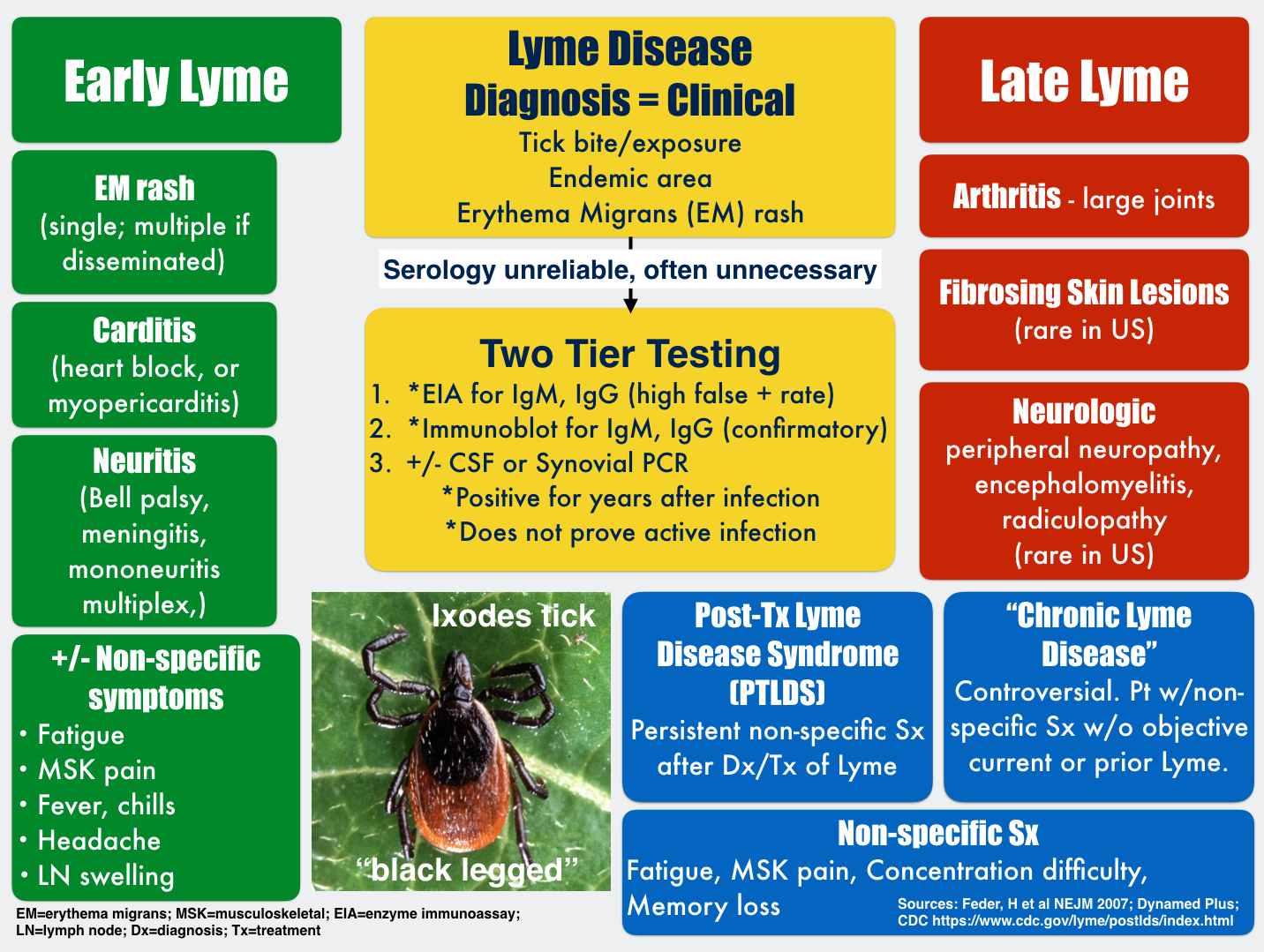
Early Localized Lyme Disease
Early localized Lyme disease usually presents as an acute illness characterized by:
- fever
- headache
- the presence of a single, localized skin lesion known as erythema migrans
Not all patients will present with an EM. Therefore, diagnosis should not be based solely on the presence of EM.
Most patients will present with EMs within 7 days of the initial tick bite. However, the incubation period can vary between 3 and 30 days.
The skin lesion is characteristically an annular erythematous lesion greater than 5 cm in diameter that:
- slowly increases in size
- is usually painless and non-pruritic
The lesion sometimes develops central clearing, but it can be more homogenously erythematous. In dark-skinned patients, the rash may appear more as a bruise.
Variations of an EM are highly suggestive of Lyme disease and can take the following forms:
- blistering
- blue-purple hues
- a bull’s-eye appearance
A skin lesion called erythema migrans can develop into a bull’s-eye at the site of a tick bite. It is shown here on a patient’s upper arm.Footnote 1
A typical sign of early non-disseminated Lyme disease is an expanding rash called erythema migrans. This can take on the appearance of a bull’s eye.Footnote 1
Some Lyme disease skin lesions are uniformly red and do not appear with the classic ring.Footnote 1
Some patients present with a central blistering lesion, commonly mistaken as a spider bite. This is likely due to an inflammatory reaction to the pathogen induced by the tick.Footnote 1
- fatigue
Don’t Miss: How Does Lyme Disease Affect You
Notice To Readersrecommendations For Test Performance And Interpretation From Thesecond National Conference On Serologic Diagnosis Of Lyme Disease
The Association of State and Territorial Public HealthLaboratory Directors, CDC, the Food and Drug Administration, theNational Institutes of Health, the Council of State and TerritorialEpidemiologists, and the National Committee for Clinical LaboratoryStandards cosponsored the Second National Conference on SerologicDiagnosis of Lyme Disease held October 27-29, 1994. Conferencerecommendations were grouped into four categories: 1) serologictest performance and interpretation, 2) quality-assurancepractices, 3) new test evaluation and clearance, and 4)communication of developments in Lyme disease testing. Thisreport presents recommendations for serologic test performance andinterpretation, which included substantial changes in therecommended tests and their interpretation for the serodiagnosis ofLD.
It was recommended that an IgM immunoblot be consideredpositive if two of the following three bands are present: 24 kDa * , 39 kDa , and 41 kDa . It was furtherrecommended that an that IgG immunoblot be considered positive iffive of the following 10 bands are present: 18 kDa, 21 kDa *,28 kDa, 30 kDa, 39 kDa , 41 kDa , 45 kDa, 58 kDa , 66 kDa, and 93 kDa .
The details of both plenary sessions and the work groupdeliberations are included in the publication of the proceedings,which is available from the Association of State and TerritorialPublic Health Laboratory Directors telephone 822-5227.
Searching For A Diagnosis
The next few months brought an onslaught of additional symptoms and medical appointments with various specialists. First, a rheumatologist told me that the chest pain I was experiencing was costochondritis, or inflammation of the cartilage of the rib cage.
A spine specialist did X-rays and MRIs of my spine, as my neck had become increasingly stiff with very limited mobility, along with nonstop cracking and popping. A neurologist concluded that I had carpal tunnel syndrome, which would explain the onset of increasing numbness and tingling in my hands. But why was I having these issues I when hadn’t done any of the repetitive wrist motions known to cause carpal tunnel inflammation?
Because I continued to struggle with shortness of breath, a pulmonologist assessed my lungs. Those tests came back normal. Once again, I was told that most likely costochondritis was the cause of my breathing issues. How desperately I wanted all of these pains to go away, yet the diagnoses seemed almost like guesses, and the symptoms were not fading.
I explained that I had been bitten by a tick, but that my tests were negative. He encouraged me to ask for additional testing.
RELATED: How Do You Get Lyme Disease?
Read Also: Can Lyme Disease Cause Psoriasis
The Most Common Lyme Disease Blood Tests
The two most common diagnostic tests for Lyme disease are the enzyme-linked immunosorbent assay and the Western blot. These Lyme disease tests allow physicians to visualize the reaction between antibodies in an infected persons blood to specific antigens or parts of the bacteria that cause Lyme disease.
In the case of the Western blot, for example, antigens are separated by size and then transferred onto a membrane strip. When an antibody reacts with an antigen on the strip, that band will turn dark purple. For test results to be positive, a specific combination of bands on the membrane strip must be present.
When Are Specialized Lyme Units
This is one of the requests posted on the petition for a better management of Lyme disease: “The creation of Lyme specialized hospital units with, eventually, certified institutes, for both basic research and research clinical. Doctors are also asking for the recognition of Lyme disease as a long-term condition that entitles patients to 100% coverage of their treatments.
The Ministry of Health plans to announce a major national action plan against Lyme disease in September 2016 .
Also Check: Treatment For Lyme Disease Years Later
The Igenex Lyme Immunoblot Solves These Problems
IGeneX has developed a serological test that increases specificity without sacrificing sensitivity that has changed how to test for Lyme disease. It uses specifically created recombinant proteins from multiple species and strains of Lyme borreliae and reduces inconsistencies in reading and interpreting the test bands.
More species detected The Lyme ImmunoBlot tests for more species of Lyme borreliae than the traditional ELISA and Western blot tests, reducing the risks of false negatives due to the inability to detect antibodies to a certain strain or species of Lb. The test includes all Borrelia-specific antigens relevant in North America and Europe, not just B. burgdorferi B31 or 297.
The result is a single test that replaces at least 8 Western blots.
More accurate testing The ImmunoBlot uses specific recombinant proteins that are sprayed in precise amounts onto specific locations on the membrane strip, allowing for greater control of the quantity and location of the antigens. This makes reading the bands much more accurate and consistent.
Earlier detection The ImmunoBlot can detect infections at multiple stages of illness, letting you catch infections earlier.
The IgM and IgG ImmunoBlots superior specificity and sensitivity make them the best Lyme disease test available.
Persistent Symptoms Following Treatment
In most cases, timely treatment according to the appropriate regimen described in the chart above is effective. However, some Lyme disease patients have persistent symptoms following treatment. Research continues into the causes and methods of treatment.
There is no definitive evidence that persistent symptoms represent ongoing infection. Post-infectious inflammation due to damage from the infectious process may respond to anti-inflammatory drugs.
Don’t Miss: What Are The Effects Of Lyme Disease In Humans
Improve Diagnostic Tests For Lyme Disease
In an interview with the Obs, Professor Christian Perronne recalls that the bacteria that causes Lyme disease is not alone. There are nearly twenty Borrelia or the Elisa test that currently allows to diagnose the disease only identifies 3. In other words: the test can be negative but the disease be there. Another test, the Western-Blot, is more precise but can only be prescribed when the Elisa Test is positive, as confirmation. The doctors, denounces Pr Perronne, do not have the right to prescribe it under pain of prosecution by the Health Insurance.
Does The Time Of Year Matter In The Diagnosis Of Lyme Disease
Since Lyme disease is a tick-borne infection, the seasonality of the disease is linked tightly to the life cycle and behavior of ticks. May, June, July, and early August are the biggest risk months for acquiring first stage Lyme disease in the US. This is the feeding time for nymph and adolescent ticks which are difficult to see. A viral-like illness in those early summer months might be Lyme disease. There is also some transmission of Lyme disease via adult ticks in the fall and winter and throughout the year anytime the temperature is above 40 degrees, but to a lesser degree.
The risk of acute Lyme disease is more of a year-round risk in more temperate regions such as northern California and the pacific northwest. Later stage Lyme disease, however, can manifest at any time.
You May Like: Lyme Disease Immune System Weakened
How Lyme Disease Is Diagnosed
Your doctor or other healthcare provider may have difficulty diagnosing Lyme disease because many of its symptoms are similar to those of other disorders and illnesses. The only distinctive sign unique to Lyme disease is absent in at least a quarter of the people who become infected. Although a tick bite is an important clue for diagnosis, many people can’t recall having been recently bitten by a tick. This isn’t surprising because the deer tick is tiny, and a tick bite is usually painless.
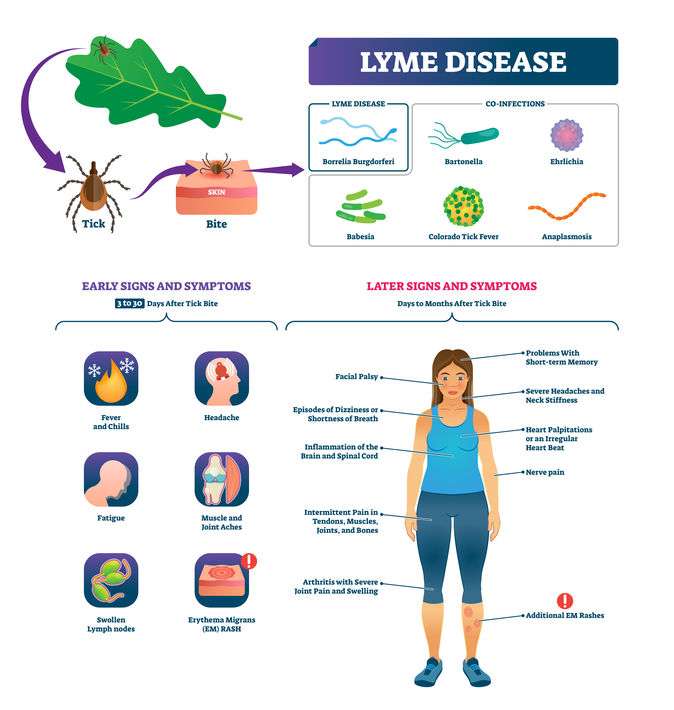
What Is Lyme Disease
Lyme disease is a bacterial infection. You get it when the blacklegged tick, also known as a deer tick, bites you and stays attached for 36 to 48 hours. If you remove the tick within 48 hours, you probably wonât get infected.
When you do get infected, the bacteria travel through your bloodstream and affect various tissues in your body. If you donât treat Lyme disease early on, it can turn into an inflammatory condition that affects multiple systems, starting with your skin, joints, and nervous system and moving to organs later on.
The chances you might get Lyme disease from a tick bite depend on the kind of tick, where you were when it bit you, and how long the tick was attached to you. Youâre most likely to get Lyme disease if you live in the Northeastern United States. The upper Midwest is also a hot spot. But the disease now affects people in all 50 states and the District of Columbia.
You May Like: How To Control Lyme Disease
How Is Lyme Disease Treated
With early-stage Lyme disease, youâll take antibiotics for about 10 days to 3 weeks. The most common ones are amoxicillin, cefuroxime, and doxycycline. The antibiotics will almost always cure your infection. If they donât, you might get other antibiotics either by mouth or as a shot.
If you donât treat your Lyme infection, you might need oral antibiotics for symptoms like weakened face muscles and irregular heartbeat. You may need antibiotics if you have meningitis, inflammation in your brain and spinal cord, or more severe heart problems.
If your Lyme is late stage, the doctor might give you antibiotics either by mouth or as a shot. If it causes arthritis, youâll get arthritis treatment.
Thereâs no therapy for post-treatment Lyme disease syndrome.
What Causes Lyme Disease
Lyme disease is caused by bacteria. In the United States, this is usually a bacterium called Borrelia burgdorferi. It spreads to humans through the bite of an infected tick. The ticks that spread it are blacklegged ticks . They are usually found in the:
- Northeast
- Upper Midwest
- Pacific coast, especially northern California
These ticks can attach to any part your body. But they are often found in hard-to-see areas such as your groin, armpits, and scalp. Usually the tick must be attached to you for 36 to 48 hours or more to spread the bacterium to you.
Recommended Reading: Do Neurologists Treat Lyme Disease
Cdc Supports The Development Of New Tests
New tests may be developed as alternatives to one or both steps of the two-step process. Before CDC will recommend new tests, they must be cleared by the Food and Drug Administration . For more details, see: Recommendations for Test Performance and Interpretation from the Second National Conference on Serologic Diagnosis of Lyme Disease.
Why Lyme Is Tough To Diagnose
- Lyme symptoms are similar to other illnesses, so misdiagnosis is common.
- Many Canadian doctors are unfamiliar with Lyme, so they dont test for it or administer the wrong tests.
- Only a handful of blood tests effectively detect Lyme bacteria, so the infection is often missed.
Dont get discouraged if you get a negative diagnosis. Seek out second, and even third, opinions if you must!
Read Also: Kozlowski Orthodontics East Lyme Ct
The Chronic Lyme Disease Controversy
Chronic Lyme disease is a poorly defined term that describes the attribution of various atypical syndromes to protracted Borrelia burgdorferi infection. These syndromes are atypical for Lyme disease in their lack of the objective clinical abnormalities that are well-recognized in Lyme disease and, in many cases, the absence of serologic evidence of Lyme disease as well as the absence of plausible exposure to the infection. The syndromes usually diagnosed as CLD include chronic pain, fatigue, neurocognitive, and behavioral symptoms, as well as various alternative medical diagnosesmost commonly neurologic and rheumatologic diseases. Perhaps the most recognized and contentious facet of this debate is whether it is effective, appropriate, or even acceptable to treat patients with protracted antibiotic courses based on a clinical diagnosis of CLD.
Traditional Lyme Disease Tests Are Not Specific Enough
Lyme disease is caused by the spiral-shaped bacteria Borrelia. There are multiple species and strains of Lyme borreliae . Therefore, tests must be targeted to these multiple species and strains in order to be able to detect them. If a patient is infected with a species or strain of Lyme borreliae that their test cant detect, they will get a false-negative test result and thus risk missing their diagnosis. This can be costly and dangerous.
Many ELISA and Western blot Lyme disease tests are only equipped to detect one strain of one species of Borrelia: Borrelia burgdorferi B31 . This means that those tests are missing infections caused by other strains and/or species of Lyme borreliae.
In one internal study designed to test the validity of the IGeneX ImmunoBlot against traditional Western blot tests, a total of 132 patients were tested by both Lyme Western blots and Lyme IB. 43 patients were seropositive on the ImmunoBlot, and 14 were positive on standard Western blots prepared from a mixture of two species for Bb ss B31 and 297. Thus 29 of the 43 patients tested negative on Western blots i.e., the Western blot totally missed their infections with strains other than Bb ss B31 and 297.
With such limited tests, patients infected with non-B31 species and strains e.g., B. mayonii, B. californiensis, or European species are at risk of receiving false negatives and missing the chance to treat their diseases.
Read Also: What Is The Best Antibiotic To Treat Lyme Disease
What Happens During Lyme Disease Testing
Lyme disease testing is usually done with your blood or cerebrospinal fluid.
For a Lyme disease blood test:
- A health care professional will take a blood sample from a vein in your arm, using a small needle. After the needle is inserted, a small amount of blood will be collected into a test tube or vial. You may feel a little sting when the needle goes in or out. This usually takes less than five minutes.
If you have symptoms of Lyme disease affecting your nervous system, such as neck stiffness and numbness in hands or feet, you may need a test of cerebrospinal fluid . CSF is a clear liquid found in your brain and spinal cord. During this test, your CSF will be collected through a procedure called a lumbar puncture, also known as a spinal tap. During the procedure:
How To Avoid Tick Bites
To reduce the chance of being bitten:
- cover your skin while walking outdoors and tuck your trousers into your socks
- use insect repellent on your clothes and skin products containing DEET are best
- stay on clear paths whenever possible
- wear light-coloured clothing so ticks are easier to see and brush off
Recommended Reading: Lyme Disease And Massage Therapy
How Is Lyme Disease Diagnosed
Your doctor will diagnose you based on your symptoms and whether youâve been exposed to a tick. They might also run a blood test. In the first few weeks of infection, the test may be negative because antibodies take a few weeks to show up.
Hopefully soon, there will be tests that can diagnose Lyme disease in the first few weeks after youâre exposed. The earlier you get treated, the less likely itâll get worse.