Persistent Symptoms After Treatment For Lyme Disease
It is well-recognized that some patients experience prolonged symptoms during convalescence from Lyme disease, and a subset suffer significant functional impairment., The most common complaints among such patients are arthralgias, myalgias, headache, neck and backache, fatigue, irritability, and cognitive dysfunction .
A working definition was developed to categorize patients with post-Lyme disease symptoms , those patients with persistent clinical symptoms after treatment for Lyme disease, but who lack objective evidence of treatment failure, reinfection, or relapse . PLDS is not strictly speaking a coherent clinical diagnosis its primary value has been to define a patient cohort for further study. Nonetheless, it is worth considering how it conceptually differs from CLD. To meet criteria for PLDS, patients must have unequivocal documentation of appropriately treated Lyme disease, lack objective manifestations of Lyme disease, and have persistent symptoms that cannot be explained by other medical illnesses. Thus, of patients with chronic symptoms that have been attributed to Lyme disease, those meeting criteria for PLDS are those for whom infection with B burgdorferi is most plausible. This makes the studies of PLDS paradigmatic for the understanding of CLD.
Getting Diagnosed Isn’t Always Straightforward
Lyme disease, a tick-borne bacterial infection, is pretty uncommon in London , so I was sure there was some kind of mistake.
The Independent reports that there are around 1,000 diagnosed cases in the UK every year, most commonly in rural areas, compared to the 300,000 annual reported cases in the US. If it’s not diagnosed early, it can lead to neurological problems like Bell’s palsy , as well as memory and heart problems, according to Mayo Clinic.
It turns out the rash on my inner left thigh was actually where I’d been bitten while sitting on the grass in St James’s Park in central London that June, a month before my hospital visit.
A rash with a red ring around the site of a tick bite, known as erythema migrans , which appears three to 30 days after being bitten, is one of the main telltale signs of Lyme disease.
What Is The History Of Lyme Disease
Interestingly, the disease only became apparent in 1975 when mothers of a group of children who lived near each other in Lyme, Conn., made researchers aware that their children had all been diagnosed with joint pain from rheumatoid arthritis. This unusual grouping of illnesses that appeared “rheumatoid” eventually led researchers to the identification of the bacterial cause of the children’s condition, which was then named “Lyme disease” in 1982.
The only vector for Lyme disease in the U.S. is the black-legged tick, or deer tick, known as Ixodes scapularis. These ticks are carriers of the Lyme disease spirochete in their stomachs Ixodes ticks may also transmit the Powassan virus. The ticks are vectors that can transmit the bacterium to humans with a tick bite. The number of cases of tick-borne illness in an area depends on the number of ticks present and how often the ticks are infected with the bacteria. In certain areas of New York, where Lyme disease is common, over half of the ticks are infected. Lyme disease has been reported most often in the northeastern United States, but it has been reported in all 50 states, as well as China, Europe, Japan, Australia, and parts of the former Soviet Union. In the United States, it is primarily contracted in the Northeast in the states from Maine to Maryland, in the Midwest in Minnesota and Wisconsin, and in the West in Oregon and Northern California. What those children actually had was Lyme arthritis.
Recommended Reading: Do Antibiotics Get Rid Of Lyme Disease
What Is Chronic Lyme
According to the CDC and IDSA, most people who test positive for Lyme respond well to antibiotics, even if they arent diagnosed or treated until months or years after the initial infection. But some patients continue to suffer long after the standard antibiotic course.
Researchers have some ideas about the causes of this more difficult condition. Its possible that the bacteria or some of the toxins they produce are sometimes able to survive the treatment. Its also possible that the body suffers some sort of autoimmune response to the bacteria or the treatment itself. Or it could be that these illnesses are the result of multiple simultaneous infectionsnot just with Borrelia burgdorferi but with several other pathogens that the blacklegged tick is known to transmit.
But ultimately, doctors are divided over several basic questions: How common is this condition? Can it be treated with antibiotics? And what should it be called?
The CDC and IDSA refer to this as post-treatment-Lyme-disease syndrome, a condition for which no proven cause or treatment options exist. According to both, theres no evidence that prolonged antibiotic therapy works against Lyme disease.
But other groups, including the International Lyme and Associated Diseases Society , call it chronic Lyme disease. They say it may stem from a failure to diagnose Lyme disease early on . They also say that long-term antibiotic therapy can work, though they say relapses are common and the road to recovery is bumpy.
Als Mimicked Lyme Disease A Case Report

I first read about this case by Wirsching and colleagues in the journal Clinical Case Reports.
Amyotrophic Lateral Sclerosis , also known as Lou Gehrigs disease, is a progressive motor neuron disease.
The 63-year-old man developed bilateral atrophic arm paresis with preserved reflexes and met the criteria for probable ALS. However, he also tested positive for Lyme disease by spinal tap.
In the year prior to developing ALS symptoms, the patient reportedly had a tick bite without a rash.
In July 2018, that is, within six months, he developed paraparesis of both arms and also suffered from cramps in the shoulder girdle and hand muscles, wrote the authors. By August 2018, the patient was severely impaired in everyday life activities.
His spinal tap revealed pleocytosis and elevated protein. The spinal fluid was positive for IgM and IgG titers for Lyme disease. His blood test was positive by ELISA and IgG Western blot tests. The antibody index was higher in the spinal tap than the blood by IgM but not IgG.
AS ALS mimicked lyme disease, he was prescribed a three-week course of intravenous ceftriaxone but his symptoms did not improve.
Hence, it is unlikely that neuroborreliosis was the main cause of symptoms in our patient, wrote the authors.
Instead, the authors concluded that the patients ALS mimicked Lyme disease.
Considering Lyme disease in differential diagnosis
The following questions are addressed this podcast:
You May Like: What Is Lyme Disease And What Are The Symptoms
Is Lyme Disease Curable What Is The Prognosis Of Lyme Disease
Lyme disease is usually curable with antibiotics. This is so true that some authors of Lyme disease research have stated that the most common cause of lack of response of Lyme disease to antibiotic therapy is a lack of Lyme disease, to begin with! The type of antibiotic depends on the stage of the disease and what areas of the body are affected. Early illness is usually effectively treated with medications taken by mouth, for example, doxycycline , amoxicillin , or cefuroxime axetil . This antibiotic therapy generally results in a rapid cure of Lyme disease. Of note, doxycycline should not be used in pregnancy or children under 8 years of age.
Therefore, if a person finds a typical bulls-eye skin rash developing in an area of a tick bite, they should seek medical attention as soon as possible. Generally, antibiotic treatment resolves the rash within one or two weeks with no long-term consequences. Later illnesses such as nervous-system disease might require intravenous drugs examples are ceftriaxone and penicillin G. There are no home remedies to treat Lyme disease.
In those people with two or more episodes of erythema migrans rash, even years apart, it is felt that the episodes represent different infections or reinfection rather than persistence of the original infection.
What To Do If You Have A Blacklegged Tick Bite
Remove the tick by pulling it directly out with fine-tipped tweezers. Lift upward with slow and even pressure. Dont twist when removing it. Dont crush it or put soap or other substances on it. Dont apply heat to it.
Place the tick in a resealable container. See if you can identify what kind of a tick it is.
Immediately after removing the tick, wash your skin well with soap and water or with rubbing alcohol.
Not all ticks carry Lyme. The Lyme bacteria is transmitted only by blacklegged ticks in their nymph or adult stage.
Save the tick to show your doctor. The doctor will want to determine if its a blacklegged tick and if theres evidence of feeding. Ticks enlarge as they feed. Your risk of getting Lyme from an infected tick increases with the length of time that the tick fed on your blood.
Summary:
Pull the tick out with tweezers and save it in a resealable container for identification.
Read Also: What Happens If You Have Lyme Disease
Stopping The Saliva Preventing The Disease
Researchers explain that the black-legged tick species Ixodes scapularis transmits the Lyme disease pathogen Borrelia burgdorferi. This disease contains several proteins and the team focused their research on 19 different types.
Working with the University of Pennsylvania, they analyzed pieces of mRNA which produce all 19 of these tick saliva proteins. Scientists who created the COVID-19 vaccine used the same strategy to develop a formula that protects against the SARS-Cov-2 virus.
Using guinea pigs, the team discovered that vaccinated animals quickly developed redness at the bite site after encountering a disease-carrying tick. As long as researchers removed the ticks right after the redness started, none of the guinea pigs developed Lyme disease. Conversely, around half of the unvaccinated group of guinea pigs were infected with B. burgdorferi bacteria despite researchers removing the ticks.
Interestingly, the vaccine successfully protected immunized guinea pigs from a single tick bite, even if researchers left the tick on the animals skin. On the other hand, a single tick bite led to Lyme disease in 60 percent of the unvaccinated guinea pigs. The vaccine also prevented ticks from feeding aggressively on their hosts and caused them to dislodge from their skin quicker.
The vaccine does have its limits. Results show protection against Lyme disease dropped off when leaving three ticks attached to the vaccinated guinea pigs.
Also Check: Type Of Doctor For Lyme Disease
What Are The Symptoms Of Lyme Disease
Symptoms can start anywhere from 3 to 30 days after the bite. They may look different depending on the stage of your infection. In some cases, you wonât notice any symptoms until months after the bite.
Early symptoms include:
All of those symptoms are also common in the flu. In most Lyme infections, one of the first symptoms youâll notice is a rash.
Without treatment, symptoms can get worse. They might include:
- Severe headache or neck stiffness
- Rashes on other areas of your body
- Arthritis with joint pain and swelling, particularly in your knees
- âDroopingâ on one or both sides of your face
- Inflammation in your brain and spinal cord
- Shooting pains, numbness, or tingling in your hands or feet
What does the rash look like?
Some Lyme rashes look like a bull’s-eye with circles around the middle. But most are round, red, and at least 2 inches across.
The rash slowly gets bigger over several days. It can grow to about 12 inches across. It may feel warm to the touch, but itâs usually not itchy or painful. It can show up on any part of your body.
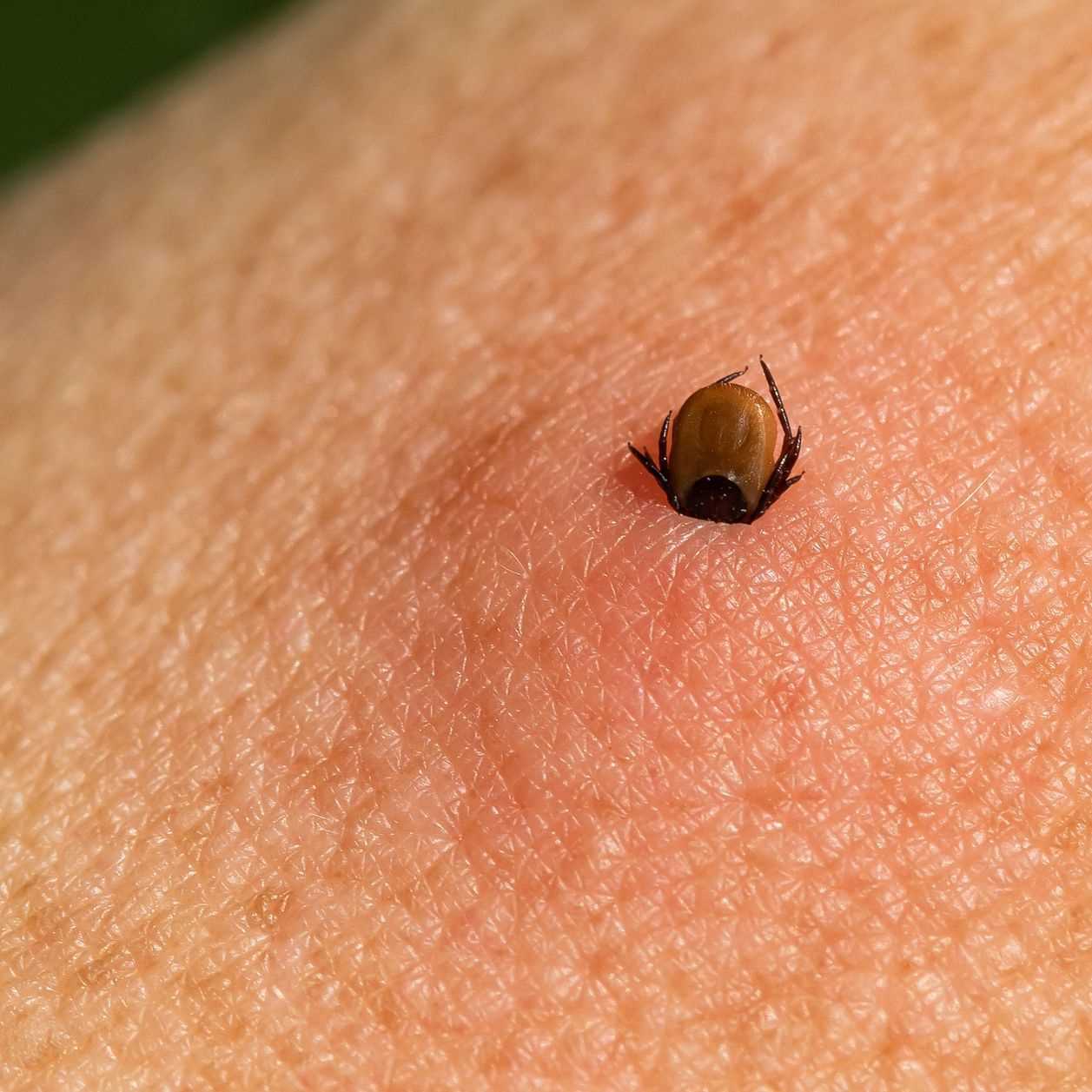
How small are ticks?
Ticks come in three sizes, depending on their life stage. They can be the size of a grain of sand, a poppy seed, or an apple seed.
Don’t Miss: How Can You Tell If You Have Lyme Disease
What Are The Stages Of Lyme Infection
There are three stages:
- Early localized Lyme: Flu-like symptoms like fever, chills, headache, swollen lymph nodes, sore throat, and a rash that looks like a bull’s-eye or is round and red and at least 2 inches long
- Early disseminated Lyme: Flu-like symptoms like pain, weakness, or numbness in your arms and legs, changes in your vision, heart palpitations and chest pain, a rash , and a type of facial paralysis known as Bellâs palsy
- Late disseminated Lyme: This can happen weeks, months, or years after the tick bite. Symptoms might include arthritis, severe fatigue and headaches, dizziness, trouble sleeping, and confusion.
About 10% of people treated for Lyme infection donât shake the disease. They may go on to have three core symptoms: joint or muscle pain, fatigue, and short-term memory loss or confusion. This is called post-treatment Lyme disease syndrome. It can be hard to diagnose because it has the same symptoms as other diseases. Plus, there isn’t a blood test to confirm it.
Experts arenât sure why Lyme symptoms donât always go away. One theory is that your body keeps fighting the infection even after the bacteria are gone, like an autoimmune disorder.
Who’s At Risk And Where Are Ticks Found
The risk of getting Lyme disease is higher:
- for people who spend time in woodland or moorland areas
- from March to October because more people take part in outdoor activities
Ticks are found throughout the UK and in other parts of Europe and North America. There are a high number of ticks in the Scottish Highlands.
It’s thought only a small proportion of ticks carry the bacteria that cause Lyme disease. Being bitten doesn’t mean you’ll definitely be infected. However, it’s important to be aware of the risk and speak to a GP if you start to feel unwell.
Don’t Miss: How Do I Get A Tick Tested For Lyme Disease
When Should You See A Doctor If You Think You Have Lyme
The rash is a pretty good indication that you may have been bitten. Take a photo of the rash and see your doctor. At this stage, treatment with antibiotics will probably work.
If you don’t have the rash but have symptoms like fatigue, fever, and headache but no respiratory symptoms like a cough, you may want to talk to your doctor.
What Do I Do If I Find A Tick On My Skin
Dont panic. Use fine-tipped tweezers to grasp the tick as close to the skins surface as possible. Pull up with steady, even pressure. Be careful not to squeeze or twist the tick body. Sometimes parts of the tick remain in the skin. You can leave them alone or carefully remove them the same way you would a splinter. Do not use heat , petroleum jelly, or other methods to try to make the tick back out on its own. These methods are not effective.
Wash the area where the tick was attached thoroughly with soap and water. Keep an eye on the area for a few weeks and note any changes. Call your doctor if you develop a rash around the area where the tick was attached. Be sure to tell your doctor that you were bitten by a tick and when it happened.
Also Check: How Do You Feel When You Have Lyme Disease
Where To Buy Cbd Hemp Oil In Johnstown Pa
- Is It Safe To Give A Toddler Hemp Oil Organic Hemp Oil Supplement
- Cv Sciences Plus Cbd Oil Hemp Spray Thc Content
- Does Hemp Oil Have Natural Parabens In It Cbd Hemp Oil Tincture 500mg
- Nutiva Organic Cold Pressed Unrefined Hemp Oil Omega 6
- Hemp Oil Cell
- Cbd Hemp Oil Uses Oil Uses Sunaroma Organic Indian Hemp Oil
- Danish Oil For Finishing Over Hemp Oil Cbd Vs Hemp Oil For Sleep
- Ananda Full Spectrum Hemp Oil
- Cbd Hemp Oil For Soap Making
- Hemp Oil Es Igual Que Marihuana Hemp Seed Oil In Hindi
Hemp Oil Kidney Stones Compare Hemp Seed Oil To Flaxseed Oil Colorado Hemp Oil Reviews. Cbd Hemp Oil For Dogs Tinctures Bionatrol Cbd Hemp Oil Cbd Hemp Mct Tincture Oil What Is It. Black Label Hemp Oil Nature S Blend Organic Hemp Seed Oil Hemp Seed Oil Essential Fatty Acids.
Other Causes Of Lyme Disease Symptoms
Sometimes people think they have the symptoms of Lyme disease, but it is a different disease caused by ticks. Diseases caused by tick bites that are known in Australia are:
- Queensland tick typhus
- Q fever
- mammalian meat allergy
Sometimes there is no known diagnosis for symptoms such as fatigue, disordered thinking, disturbances of the senses, joint pain and headaches. These symptoms are real and can be very debilitating. In this case, you doctor will work with you to manage the symptoms and improve your quality of life.
Also Check: Lyme Disease Chain Of Infection
What Type Of Illness Does B Mayonii Cause
Based on limited information, illness caused by B. mayonii appears similar to that caused by B. burgdorferi, but with a few differences. Like B. burgdorferi, B. mayonii causes fever, headache, rash, and neck pain in the days after infection and can cause arthritis after a few weeks of illness. Unlike B. burgdorferi, B. mayonii can also cause nausea and vomiting large, widespread rashes and a higher concentration of bacteria in the blood.
The Misdiagnosis Of Chronic Lyme Disease
Many patients referred for Lyme disease are ultimately found to have a rheumatologic or neurologic diagnosis. Rheumatologic diagnoses commonly misdiagnosed as Lyme disease include osteoarthritis, rheumatoid arthritis, degenerative diseases of the spine, and spondyloarthropathies.,, Some patients are found to have neurologic diseases, including multiple sclerosis, demyelinating diseases, amyotrophic lateral sclerosis, neuropathies, and dementia. Some CLD advocates have argued that these various conditions are simply manifestations of Lyme disease,, but these hypotheses are untenable. Lyme disease is transmitted quite focally, and there is no epidemiologic evidence that these alternative diagnoses cluster in regions with high Lyme disease transmission. There has been no association between diagnoses such as multiple sclerosis, amyotrophic lateral sclerosis, or rheumatoid arthritis and antecedent Lyme disease, these diagnoses do not arise concurrently with other recognized manifestations of disseminated Lyme disease , and there is no quality evidence associating any of these diagnoses with seroconversion to B burgdorferi. Although there can certainly be clinical overlap between Lyme disease and other conditions, objective findings and studies will generally allow them to be differentiated.
You May Like: When To Test For Lyme Disease