Posttreatment Lyme Disease Syndrome
Posttreatment Lyme disease syndrome has been defined as the presence of any of: widespread musculoskeletal pain, cognitive complaints, radicular pain, paresthesias, or dysesthesias interfering with function within 6 months after initial diagnosis and treatment and persist for at least 6 months . The symptoms overlap extensively with those of Lyme encephalopathy, differing primarily by the requirement that encephalopathy occur in patients with active extraneurologic infection, whereas PTLDS patients have already been appropriately diagnosed with and treated for Lyme disease. Such symptoms are often present immediately after treatmentas they may be following treatment of other infectionsand usually resolve over time. PTLDS is diagnosed when symptoms persist for 6 or more months.
A Differential Diagnosis May Be Needed To Pinpoint The Actual Cause
If you are experiencing neurological symptoms, do not necessarily assume you have multiple sclerosis , especially considering there are a number of other conditions that can mimic it. Seeing a healthcare provider for an evaluation is critical before jumping to any conclusions.
Depending on your symptoms, a proper diagnosis may be a fairly rapid process involving simple blood tests, or it may be more invasive, like requiring a biopsy.
Here are several medical conditions your healthcare provider may consider as alternative diagnoses to MS.
What Are The Symptoms Of Lyme Disease
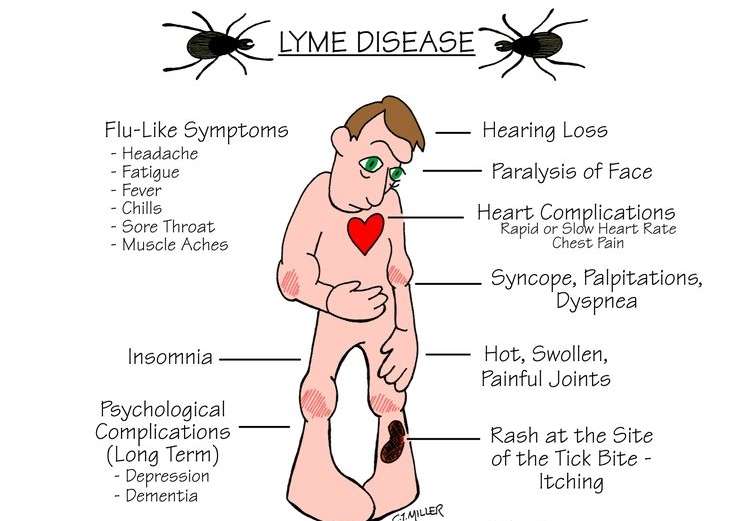
The list of possible symptoms is long, and symptoms can affect every part of the body. The following are the most common symptoms of Lyme disease. But symptoms are slightly different for each person.
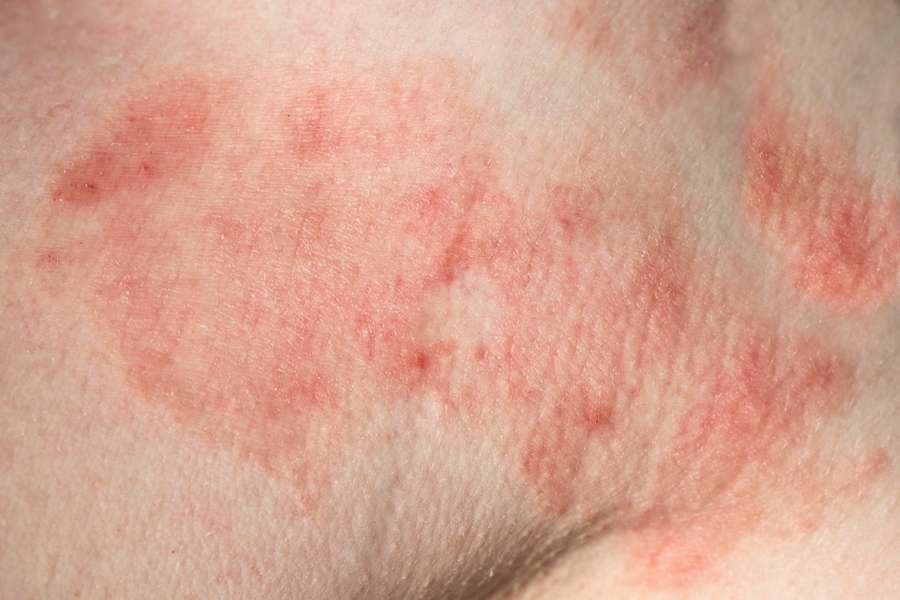
The primary symptom is a red rash that:
-
Can appear several days after infection, or not at all
-
Can last up to several weeks
-
Can be very small or grow very large , and may resemble a âbulls-eyeâ
-
Can mimic such skin problems as hives, eczema, sunburn, poison ivy, and flea bites
-
Can itch or feel hot, or may not be felt at all
-
Can disappear and return several weeks later
Several days or weeks after a bite from an infected tick, you may have flu-like symptoms such as the following:
-
Headache
-
Swollen glands
Weeks to months after the bite, the following symptoms may develop:
-
Neurological symptoms, including inflammation of the nervous system and weakness and paralysis of the facial muscles
-
Heart problems, including inflammation of the heart and problems with heart rate
-
Eye problems, including inflammation
Months to a few years after a bite, the following symptoms may include:
-
Inflammation of the joints
-
Neurological symptoms including numbness in the extremities, tingling and pain, and difficulties with speech, memory, and concentration
Don’t Miss: Vitality Spa Old Lyme Ct
Medical Studies That Show Antibiotics Help Against Multiple Sclerosis
There are a few studies that show that antibiotics work, so that’s not too controversial any more. What remains controversial is why antibiotics work. People, including medical doctors, like to interpret facts in such a way that their world view doesn’t get demolished. Doctors like to believe that infections are not the cause of neurological problems. That simply is too disturbing a thought. So when antibiotics are proven to stop and even reverse the symptoms of MS, they are quick to deny any relation to bacteria, but claim: “It must be some antiinflammatory effect of the antibiotics”. The first study shows that antibiotics as a treatment for MS work:
Renal System Dysfunction Caused By Lyme Disease
The renal system is a vital part of the overall functioning of the body. Without the ability to filter the blood, it can lead to the aforementioned symptoms and conditions.
The damage done to the renal system following a Lyme disease infection can:
- Cause the kidney filtration system to cease functioning, or function at a lower level.
- Aid in the formation of lesions on the kidneys.
- Cause the build-up of waste in the bloodstream.
- Lead to the leakage of proteins and red blood cells out of the system.
- Eventually cause kidney disease or kidney failure.
You May Like: Arizona Lyme Disease Treatment Center
Lyme Is Not The Only Threat
As mentioned earlier in this article, there is another group of borrelia that causes a disease that is similar to, but biologically distinct from, Lyme. This disease, called Tick-Borne Relapsing Fever or TBRF, is often characterized by fevers that wax and wane every few days. However, many patients never experience relapsing fevers or any fevers at all. Like those of Lyme and other tick-borne diseases, TBRF symptoms can often go undetected or be mistaken for other conditions, which can give the disease time to develop into neurological symptoms.
So, as with Lyme, it is crucial to get an early and accurate diagnosis of TBRF. Be aware that TBRF will not show up on a Lyme test the test must be designed to test for TBRF borrelia in order to show accurate results. If symptoms are Lyme-like but test results are negative, doctors should consider the possibility of TBRF.
Invite More Calm Into Your Life
Since stress is a powerful immune system disruptor, finding more calm is key to restoring immune health and resolving symptoms of neurological Lyme. One of the best tools to fight stress is getting optimal sleep. Without it, your immune functions are disrupted, and healing is compromised.
Sleep is especially important for recovery from neuroinflammatory illnesses. Studies have shown that even one night of compromised sleep in healthy people is associated with accumulation of beta amyloid in the brain, a hallmark of Alzheimers disease.
Your goal: At least 8 hours of good sleep a night, including 4 hours of deep sleep. Practicing good sleep hygiene can help you hit the mark that includes keeping a regular bedtime, and limiting light, computer screens, and stimulation in the evening.
What happens during the day is also key to drifting off at night. Finding additional ways to de-stress, getting regular low-intensity exercise, and practicing meditation a couple of times during the day promotes good sleep onset and better quality sleep at night.
Early on, when neuroinflammation is pronounced and the nervous system is very agitated, sleep medications may be indicated. But use them intermittently, and stick to the lowest dose possible.
Acupuncture can be beneficial for reducing pain and restoring normal energy pathways in the body. It is also helpful for restoring normal sleep.
Read Also: Signs Of Lyme Disease In People
Don’t Miss: Does Lyme Disease Cause Back Pain
Why Accurate Ms Diagnoses Are Challenging
There is no single test for MS, so an accurate MS diagnosis can be challenging. Results of a recently study published in the Journal Multiple Sclerosis and Related Disorders suggested that nearly 1 in 5 people with other neurologic conditions are mistakenly diagnosed with MS.1 The confusion also means that many people also live with symptoms for months or years before an official MS diagnosis can be confirmed.
Who Diagnoses Multiple Sclerosis
Many conditions could cause similar neurological symptoms. Getting an accurate diagnosis is sometimes difficult. Some people see multiple providers over years before receiving a diagnosis. While the search can be frustrating, its important to keep looking for answers. Identifying and treating MS as soon as possible can help slow the diseases progression.
If your primary care provider suspects you may have MS, you will need to see a neurologist. A neurologist is a doctor who specializes in treating conditions that affect the nervous system, which includes your brain and spinal cord.
You May Like: Antibiotics Used For Lyme Disease
Recommended Reading: How To Get Rid Of Lyme Disease In Humans
Does Lyme Disease Cause Peripheral Neuropathy
Yes, patients with Lyme disease may develop âperipheral neuropathyâ a dysfunction of the nerves that transmit electrical signals between the bodyâs periphery and the spinal cord and brain. Common symptoms of Lyme-related neuropathy include multi-site âneuropathic painâ , spinal or radicular pain, distal paresthesias , sensory loss, weakness and hyporeflexia. . These symptoms are often caused by malfunctioning of small âA-delta fibersâ and âC fibersâ that carry pain and temperature signals. Pathology of the small nerve fibers can also disrupt autonomic functions such as heart rate, blood pressure, and gastrointestinal functions. Involvement of the cranial nerves can lead to blurry vision, double vision, facial droop, loss of balance, or tinnitus .
The precise mechanisms by which these nerve fibers are damaged in Lyme disease remains a subject of active investigation. Some possibilities include: direct assault on the nerve fibers by spirochetes during periods of active infection immune-mediated damage to the nerve fibers or their protective myelin sheaths by the hostâs own innate or adaptive immune system or production of antibodies with accumulation of immune-complexes that disrupt the small vessels that supply oxygen and nutrients to the metabolically-active peripheral nerves.
Is Multiple Sclerosis A Symptom Of Lyme Disease
. and why is there no current ongoing aggressive human pathology being done in Canada specific to looking for Lyme in patients diagnosed with MS considering that Canada has some of the highest per capita rates of MS in the world?
Lyme on the Brain Lecture Notes of Tom Grier
MS and SpirochetesIn every Lyme disease support group in this country , there have always been at least one multiple sclerosis, MS, patient who turned out to have Lyme disease, and was recovering on antibiotics. But if this is true why is there is no documented connection between spirochetes and M.S.? As it turns out there are more than 50 such MS-spirochete references prior to World War II and going back to as far as 1911, and published in such prestigious journals as the Lancet.
1911 Buzzard Spirochetes in MS Lancet
1913 Bullock MS Agent in Rabbits Lancet
1917 Steiner Spirochetes The Cause of MS Med Kiln
1918 Simmering Spirochetes in MS by Darkfield Micro
1918 Steiner G. Guinea Pig Inoculation with MS infectious agent from Human
1919 Steiner MS Agent Inoculation into Monkeys
1921 Gye F. MS Agent In Rabbits Brain 14:213
1922 Kaberlah MS Agent In Rabbits Deutch Med Works
1922 Sicard MS Spirochetes in Animal Model Rev Neurol
1922 Stepanopoulo Spirochetes in the CSF of MS Patients
1923 Shhlossman MS Agent in Animal Model Rev Neuro
1924 Blacklock MS Agent in Animals J. of Path and Bac
1927 Wilson The Rat as A Carrier of MS British Med Journal
1927 Steiner G Understanding the Pathogenesis of MS
Also Check: Herbal Remedies For Lyme Disease
Misdiagnosing Lyme Diseasethe Great Imitator
The Borrelia burgdorferi spirochete is an evasive organism which can penetrate virtually any organ or system in the body, including the brain and central nervous system, joints, muscles and heart. Lyme disease symptoms may be similar to other medical conditions, making diagnosing a challenge. For this reason, Lyme disease and syphilis have both been coined the great imitator.
Lyme disease and syphilis have both been coined the great imitator.
Patients with Lyme disease have been incorrectly diagnosed with: multiple sclerosis , fibromyalgia, chronic fatigue syndrome, autoimmune diseases including lupus and rheumatoid arthritis , polymyalgia rheumatica, thyroid disease, and psychiatric disorders, among others.
Fatigue, insomnia, and myalgias are seen in both Fibromyalgia and Lyme disease. Chronic Fatigue Syndrome symptoms are often seen in Lyme disease patients and include severe fatigue, impaired memory and concentration, sleep disturbance, myalgias, and arthralgias.
Steere et al. described Lyme disease cases that were misdiagnosed as Juvenile Rheumatoid Arthritis .
Nowakowski and Feder reported cases misdiagnosed as cellulitis.
Plotkin described a 39-year-old male with a retropopliteal rash that progressed, within three weeks to Lyme disease, with a loss of consciousness and a complete heart block that required insertion of a transvenous cardiac pacemaker.
For Chronic Cases Of Lyme Does Iv Igg Hold Hope For Remitting Symptoms And Improving The Quality Of Life
To our knowledge, IV Ig has never been studied in a controlled fashion as a treatment for chronic Lyme disease, although some physicians are using this treatment for patients who are thought to have autoimmune-mediated neurologic sequelae from Lyme disease that persist after antibiotic treatment. There is insufficient data at this point to say whether IVIg treatment will have acute or sustained benefit for patients with persistent symptoms after being treated with antibiotics for Lyme disease. This is an area of research which is worth pursuing. Certainly, given that there is evidence that IV Ig may be beneficial for a variety of inflammatory and autoimmune diseases such as relapsing and remitting multiple sclerosis , myasthenia gravis, pemphigus, polymyositis , dermatomyositis , Wegenerâs granulomatosis , and chronic inflammatory demyelinating polyneuropathy, it is reasonable to consider that this treatment may also be beneficial for patients with post-treatment Lyme disease if there is evidence of immunologic dysfunction. This treatment may be especially helpful if there is evidence of autoimmune-mediated neuropathic pain. IV Ig treatment is expensive and not without risks, so such treatment should only be initiated if the potential for benefits significantly outweigh the risks.
Donât Miss: Long Term Antibiotic Use For Lyme Disease
You May Like: Cost Of Western Blot Test For Lyme
Symptoms Of Lyme Disease And Ms
Both Lyme disease and multiple sclerosis can cause a variety of neurologic symptoms, including:
- Weakness
- Fatigue
- Pins and needles sensations
Lyme and MS also may both cause optic neuritis inflammation in the optic nerve responsible for transmitting visual information from the eye to the brain. This can result in problems such as blurred or double vision.
Neurological symptoms are not the initial symptom of Lyme disease. Those are often delayed, developing anywhere from several days or weeks to months after a person has been infected with B. burgdorferi bacteria. Lyme disease can affect other body parts as well, such as the joints.
In some cases, Lyme disease may also cause symptoms that relapse and remit . The same is true of the form of multiple sclerosis known as relapsing-remitting MS. Lyme disease has even been known to trigger multiple sclerosis attacks , which may complicate differentiating between the two conditions.
Lyme Disease Vs Ms: Complications
Complications can arise in both Lyme disease and multiple sclerosis if not managed and treated properly. If Lyme disease is caught early, antibiotics can be given immediately to reduce complications, but if treatment is delayed chronic complications can arise including fatigue, arthritis and joint pain, headaches, short-term memory problems, numbness, Bells palsy , heart problems including slow or irregular heartbeat, and depression, which can be set off by living with the complications of Lyme disease.
Complications of multiple sclerosis include an increase in urinary tract infections due to disrupt bladder nerves responsible for opening and closing of the bladder, osteoporosis, pressure sores, aspiration pneumonia which can make swallowing difficult and so food and liquid spills into the lungs, and depression as a result of living with multiple sclerosis. Many multiple sclerosis treatments can help prevent these complications from arising so its important to get proper treatment right away.
You May Like: Best Medication For Lyme Disease
What Triggers Autoimmune Diseases
The most common explanation is that an affected persons immune system, partly due to the genes they inherited, is primed to react abnormally to some trigger, such as an infection, an environmental exposure , or some other factor. For most autoimmune diseases, we cant easily figure out what triggers them. If we could, we might be able to prevent them.
Lyme Disease Vs Ms: Signs And Symptoms
Symptoms of multiple sclerosis include:
- Numbness or weakness in one or more limbs
- Partial or complete vision loss, pain during eye movement
- Prolonged double vision
- Swollen lymph nodes
- Erythema migrans rash, which looks like bulls eye
As the disease progresses, symptoms can worsen into severe headache and neck stiffness, with additional rashes, arthritis accompanied by severe joint pain and swelling, muscle loss in the face, intermittent pain in the tendons, muscle joints, and bones, heart palpitations or irregular heartbeat, dizziness or shortness of breath, nerve pain, shooting pain, numbness or tingling, and problems with short-term memory.
Recommended Reading: Is There A Shot For Lyme Disease
Strategies For Managing Nerve Pain
1. Reduce Your Microbial Burden
When youre dealing with Lyme disease and co-infections, its not always easy to pinpoint which stealth pathogen is affecting your nervous system. In fact, its most reasonable to recognize that all sneaky microbes are capable of disrupting immune function and causing it to go awry.
When your bodys microbial burden becomes too great, your microbiome becomes imbalanced, driving inflammation and aggravating neuropathy. Thus, at the top of the priority list is decreasing the infectious load to normalize and calm the immune system.
When youre looking for natural solutions to lessen the impact of stealth pathogens, herbal therapy can play a critical role. Not only do herbs have antimicrobial properties, but they are anti-inflammatory and contain antioxidants as well.
Moreover, herbs dont disrupt the delicate balance of the microbiome like synthetics medications do. Some of my favorite herbs with antimicrobial and immunomodulating properties to keep in mind include:
2. Use Medications Cautiously
When it comes to neuropathy, the reality is that sometimes you need some extra support to get your pain levels to a tolerable level. There are a variety of over-the-counter and prescription medications that may be useful from time to time.
However, the value of medications is limited to short term management of symptoms because of cumulative side effects. The list of medications commonly recommended by healthcare providers includes:
What Are The Symptoms Of Renal Problems Caused By Lyme Disease
When Lyme disease causes glomerular disease in patients, the symptoms can be serious and debilitating. They include:
- Edema in the face, hands, feet, and other parts of the body
- Muscle and tissue loss caused by low amounts of protein in the blood
- Kidney disease leading to tiredness, insomnia, weight loss, itchy skin
- Blood in the urine
These signs and symptoms need to be addressed immediately as they can lead to permanent damage to kidney function, which can cause seizures, coma, or in the worst cases, death.
Other symptoms to look out for if you suspect the development of chronic kidney disease include:
- Gastrointestinal issues such as nausea, vomiting, and appetite loss
- Insomnia
- Chest pain or shortness of breath from the build-up of fluids
- Skin irritations such as pigmentation changes and unexplainable scratch marks
- Hypertension
- Muscle issues such as twitching and cramping
- Cognitive decline
- Chronic fatigue and widespread weakness
Read Also: What Antibiotics Treat Lyme Disease In Humans